Abstract
Objective
To compare the possible effects of wet-cupping therapy with conventional therapy on persistent nonspecific low back pain (PNSLBP).
Methods
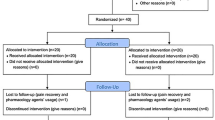
In this randomized clinical trial, 180 participants with the mean age of 45±10 years old, who had been suffering from PNSLBP were randomly assigned to wet-cupping and conventional groups. The wet-cupping group was treated with two separate sessions (4 weeks in total) on the inter-scapular and sacrum area. In the conventional group, patients were conservatively treated using rest (6 weeks) and oral medications (3 weeks). The primary and the secondary outcome were the quantity of disability using Oswestry Disability Index (ODI), and pain intensity using Visual Analogue Scale (VAS), respectively.
Results
There was no significant difference in demographic characteristics (age, gender, and body mass index) between the two groups (P>0.05). Therapeutic effect of wet-cupping therapy was comparable to conventional treatment in the 1st month follow-up visits (P<0.05). The functional outcomes of wet-cupping at the 3rd and 6th month visits were significantly increased compared to the conventional group. Final ODI scores in the wet-cupping and conventional groups were 16.7 ± 5.7 and 22.3 ± 4.5, respectively (P<0.01).
Conclusion
Wet-cupping may be a proper method to decrease PNSLBP without any conventional treatment. The therapeutic effects of wet-cupping can be longer lasting than conventional therapy. (Registration No. IRCT2013021672741))
Similar content being viewed by others
References
Manchikanti L, Singh V, Falco FJ, Benyamin RM, Hirsch JA. Epidemiology of low back pain in adults. Neuromodulation 2014;17 Suppl 2:3–10.
Arslan M, Gokgoz N, Dane S. The effect of traditional wetcupping on shoulder pain and neck pain: a pilot study. Complement Ther Clin Pract 2016;23:30–33.
Kim JI, Lee MS, Lee DH, Boddy K, Ernst E. Cupping for treating pain: a systematic review. Evid Based Complement Alternat Med 2011;2011:467014.
Kim JI, Kim TH, Lee MS, Kang JW, Kim KH, Choi JY, et al. Evaluation of wet-cupping therapy for persistent nonspecific low back pain: a randomised, waiting-list controlled, open-label, parallel-group pilot trial. Trials 2011;12:146.
Lauche R, Cramer H, Hohmann C, Choi KE, Rampp T, Saha FJ, et al. The effect of traditional cupping on pain and mechanical thresholds in patients with chronic nonspecific neck pain: a randomised controlled pilot study. Evid Based Complement Alternat Med 2012;2012:429718.
AlBedah A, Khalil M, Elolemy A, Hussein AA, AlQaed M, Al Mudaiheem A, et al. The use of wet-cupping for persistent nonspecific low back pain: randomized controlled clinical trial. J Altern Complement Med 2015;21:504–508.
Farhadi K, Schwebel DC, Saeb M, Choubsaz M, Mohammadi R, Ahmadi A. The effectiveness of wetcupping for nonspecific low back pain in Iran: a randomized controlled trial. Complement Ther Med 2009;17:9–15.
Lin CW, Haas M, Maher CG, Machado LA, van Tulder MW. Cost-effectiveness of guideline-endorsed treatments for low back pain: a systematic review. Eur Spine J 2011;20:1024–1038.
Rubinstein SM, van Middelkoop M, Kuijpers T, Ostelo R, Verhagen AP, de Boer MR, et al. A systematic review on the effectiveness of complementary and alternative medicine for chronic non-specific low-back pain. Eur Spine J 2010;19:1213–1228.
van Middelkoop M, Rubinstein SM, Kuijpers T, Verhagen AP, Ostelo R, Koes BW, et al. A systematic review on the effectiveness of physical and rehabilitation interventions for chronic non-specific low back pain. Eur Spine J 2011;20:19–39.
Anwar F, Abdelaal M. From leeches to lancets: the lost donors. Transfusion 2008;48:2490–2491.
Cao H, Han M, Zhu X, Liu J. An overview of systematic reviews of clinical evidence for cupping therapy. J Tradit Chin Med 2015;2:3–10.
Cao H, Li X, Liu J. An updated review of the efficacy of cupping therapy. PLoS One 2012;7:e31793.
Cao H, Li X, Yan X, Wang NS, Bensoussan A, Liu J. Cupping therapy for acute and chronic pain management: a systematic review of randomized clinical trials. J Tradit Chin Med 2014;1:49–61.
Rozenfeld E, Kalichman L. New is the well-forgotten old: the use of dry cupping in musculoskeletal medicine. J Bodyw Mov Ther 2016;20:173–178.
Fairbank JC, Pynsent PB. The Oswestry Disability Index. Spine (Phila Pa 1976) 2000;25:2940–2952; discussion52.
Kim TH, Kim KH, Choi JY, Lee MS. Adverse events related to cupping therapy in studies conducted in Korea: a systematic review. Eur J Integr Med 2014;6:434–440.
Kravetz RE. Cupping glass. Am J Gastroenterol 2004;99:1418.
Meng XW, Wang Y, Piao SA, Lu WT, Zhu CH, Mu MY, et al. Wet cupping therapy improves local blood perfusion and analgesic effects in patients with nerve-root type cervical spondylosis. Chin J Integr Med 2018;24:830–834.
Tagil SM, Celik HT, Ciftci S, Kazanci FH, Arslan M, Erdamar N, et al. Wet-cupping removes oxidants and decreases oxidative stress. Complement Ther Med 2014;22:1032–1036.
Bishop FL, Yardley L, Prescott P, Cooper C, Little P, Lewith GT. Psychological covariates of longitudinal changes in back-related disability in patients undergoing acupuncture. Clin J Pain 2015;31:254–264.
Lee MS, Kim JI, Kong JC, Lee DH, Shin BC. Developing and validating a sham cupping device. Acupunct Med 2010;28:200–204.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mardani-Kivi, M., Montazar, R., Azizkhani, M. et al. Wet-Cupping Is Effective on Persistent Nonspecific Low Back Pain: A Randomized Clinical Trial. Chin. J. Integr. Med. 25, 502–506 (2019). https://doi.org/10.1007/s11655-018-2996-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11655-018-2996-0