Abstract
Objective
To observe the clinical effectiveness and safety of fire-needle therapy, an external approach of Chinese medicine in treating plaque psoriasis.
Methods
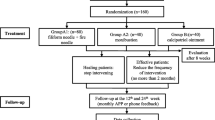
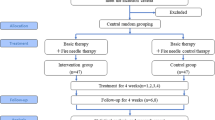
This study was a two-parallel-arm randomized controlled trial. A total of 151 participants with plaque psoriasis were randomly assigned to the fire-needle therapy group (treatment group, 76 cases) or the control group (75 cases) at a 1:1 allocation ratio using SAS software. All participants received Oral Huoxue Jiedu Decoction (活血解毒汤, HXJDD) and applied externally vaseline cream twice a day. Participants in the treatment group received fire-needle therapy once weekly for 4 weeks plus HXJDD and vaseline cream applied the same as the control group. The primary outcome measure was Psoriasis Area and Severity Index (PASI) score, and the secondary outcomes were Dermatology Life Quality Index (DLQL), and Hamilton Anxiety Rating Scale (HAMA), as well as Chinese medicine (CM) syndrome score and photos of target lesions. The indices were evaluated before and after treatment.
Results
Sixty-eight patients in each group completed the study. The treatment group has not yet achieved significant improvement in PASI score (P>0.05) compared to the control group. However, significant differences were found between the two groups in relieving CM syndrome (P<0.05) and improving quality of life (P<0.05).
Conclusion
Fire-needle appears to be safe and may have benefit for psoriasis, the short-term treatment and small sample size limit the conclusions of this study. Further rigorous randomized controlled trials with longer treatment are recommended.
Similar content being viewed by others
References
Sticherling M. Psoriasis and autoimmunity. Autoimmun Rev 2016;15:1167–1170.
Greb JE, Goldminz AM, Elder JT, Lebwohl MG, Gladman DD, Wu JJ, et al. Psoriasis. Nat Rev Dis Primers 2016;2:16082.
Kupetsky EA, Keller M. Psoriasis vulgaris: an evidence–based guide for primary care. J Am Board Fam Med 2013;26:787–801.
Aldredge LM, Young MS. Providing guidance for patients with moderate–to–severe psoriasis who are candidates for biologic therapy: role of the nurse practitioner and physician assistant. J Dermatol Nurses Assoc 2016;8:14–26.
Bhosle MJ, Kulkarni A, Feldman SR, Balkrishnan R. Quality of life in patients with psoriasis. Health Qual Life Outcomes 2006;4:35.
Lee YW, Park EJ, Kwon IH, Kim KH, Kim KJ. Impact of psoriasis on quality of life: relationship between clinical response to therapy and change in health–related quality of life. Ann Dermatol 2010;22:389–396.
Goldenberg G, Lanoue J, Dong J. New oral therapies for psoriasis: a comprehensive review. J Clin Aesthet Dermatol 2016;9:25–28.
Stein Gold LF. Topical therapies for psoriasis: improving management strategies and patient adherence. Semin Cutan Med Surg 2016;35:S36–S44.
Hemne PS, Kunghatkar RG, Dhoble SJ, Moharil SV, Singh V. Phosphor for phototherapy: review on psoriasis. Luminescence 2017;32:260–270.
Griffiths CE, Vender R, Sofen H, Kircik L, Tan H, Rottinghaus ST, et al. Effect of tofacitinib withdrawal and re–treatment on patientreported outcomes: results from a phase 3 study in patients with moderate to severe chronic plaque psoriasis. J Eur Acad Dermatol Venereol 2017;31:323–332.
Czarnecka–Operacz M, Sadowska–Przytocka A. The possibilities and principles of methotrexate treatment of psoriasis–the updated knowledge. Postepy Dermatol Alergol 2014;31:392–400.
Li TT, Wang P, Zhou DM, Jiang X, Jiang CY, Chen WW, et al. Clinical observation of Huoxue Jiedu Decoction for psoriasis vulgaris of blood stasis syndrome. J Pract Dermatol 2016;9:133–135.
Wang Y, Xie X, Zhu X, Chu M, Lu Y, Tian T, et al. Fire–needle moxibustion for the treatment of knee osteoarthritis: a meta–analysis. Evid Based Complement Altern Med 2016;2016:1392627.
Wang N, Li ZF, Wu HH. Clinical observation on therapeutic effect of red–hot needle therapy for spastic hemiplegia in stroke patients. Aupunct Res (Chin) 2015;40:304–308.
Tan EK, Millington GW, Levell NJ. Acupuncture in dermatology: an historical perspective. Int J Dermatol 2009;48:648–652.
Chinese guildlines for the management of psoriasis (2008). Chin J Dermatol (Chin) 2009;42:2.
Feldman SR, Krueger GG. Psoriasis assessment tools in clinical trials. Ann Rheum Dis 2005;64:ii65–ii68.
Finlay AY, Khan GK. Dermatology life quality index (DLQI)— a simple practical measure for routine clinical use. Clin Exp Dermatol 1994;19:210–216.
Fleming P, Bai JW, Pratt M, Sibbald C, Lynde C, Gulliver WP. The prevalence of anxiety in patients with psoriasis: a systematic review of observational studies and clinical trials. J Eur Acad Dermatol Venereol 2017;31:798–807.
Zheng XY, ed. Zheng XY, ed.. Guiding Principle of Clinical Research on New Drugs of Traditional Chinese Medicine. Beijing: China Medical Science Press;2002: 299–302.
Han RX, Yang J, Zhang TS, Zhang WD. Effect of fire–needle intervention on serum IL–1 and TNF–alpha levels of rheumatoid arthritis rats. Aupunct Res (Chin) 2012;37:114–118.
Wu MF, Li S, Qian YM, Li FL. Combination therapy of tacrolimus and Chinese herb medicated bath in children with inverse psoriasis. Chin J Integr Med 2018;24:284–287
Sagi L, Trau H. The Koebner phenomenon. Clin Dermatol 2011;29:231–236.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by the External Treatment Technology Project, Chinese Medicine Science in Beijing, Undertaken by the Beijing Administration of Traditional Chinese Medicine (No. WZF 2012-97)
Rights and permissions
About this article
Cite this article
Pan, Hd., Qi, Xl., Wang, L. et al. Whether Fire-needle Therapy Benefits Plaque Psoriasis: A Multicenter, Randomized, and Controlled Trial. Chin. J. Integr. Med. 25, 259–263 (2019). https://doi.org/10.1007/s11655-018-2940-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11655-018-2940-8