Abstract
Objective
To observe the effect of Chinese medicine therapy combined with psychological intervention (combined therapy) on the clinical symptoms and levels of blood lipids and sex hormones of patients of peri-menopausal syndrome complicated with hyperlipidemia.
Methods
With the use of a randomizing digital table method, 185 patients that fit the registration standard were randomly assigned to three groups. The 59 cases in Group A were treated with two Chinese patents, Kunbao Pill (坤宝丸) and Modified Xiaoyao Pill (加味逍遥丸); the 63 in Group B received psychological intervention alone; and the 63 in Group C were treated with both (the combined therapy), with the treatment course for all six months. The items of observation included: (1) scoring by SCL-90 on eight factors and seven symptoms; (2) scoring on Chinese medicine symptoms by Kupermann scale, including anxiety and bad temper, scorching sense ation with sweating, dizziness, tinnitus, soreness and weakness of the loin and knees, palpitation, insomnia, lassitude, weakness, and hyposexuality; (3) blood contents of total cholesterol (TC), triglyceride (TG), high-density lipoprotein cholesterol (HDL-C), low-density lipoprotein cholesterol (LDL-C), apoprotein AI (ApoAI) and B (ApoB); (4) levels of sex hormones, including estradiol (E2), progesterone (P), pituitary prolactin (PRL), follicular stimulating hormone (FSH), and), luteinzing hormone (LH) in some randomly selected patients; (5) adverse reaction; and (6) one-year follow-up study on long-term effect.
Results
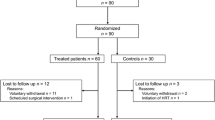
A total of 21 patients (6, 8, and 7 cases in Groups A, B, and C, respectively) dropped out; the drop-out rate was insignificant among groups. (1) The markedly effective rates in Group A, B, and C were 26.42% (14/53), 18.18% (10/55), and 53.57% (30/56), respectively, and the total effective rates in them were 64.15% (34/53), 50.91% (28/55), and 87.50% (49/56), respectively, suggesting the therapeutic efficacy in Group C was significantly better than that in Groups A and B (P<0.01). (2) SCL-90 scoring showed that the total scores decreased significantly after treatment in Group C (P<0.01), but remained unchanged in Groups A and B (P>0.05). (3) Scoring on Chinese medicine symptoms showed the same results as shown by SCL-90 scoring in terms of total scores and individual symptoms, except that menstrual disorder and amenorrhea were unchanged in all three groups (P>0.05). (4) Levels of HDL-C, ApoAI, and E2 increased and those of TG, TC, LDL-C, ApoB, FSH, and LH decreased after treatment in Group C, reaching near normal levels; similar trends of blood lipids were shown in Group A, but the level of sex hormones was unchanged. In Group B all the above-mentioned indices were unchanged (P>0.05). (5) A one-year follow-up study showed the markedly effective rate and the total effective rate in Group C were higher than those in the other two groups respectively (P<0.01). (6) No adverse reaction was found.
Conclusion
Chinese medicine therapy combined with psychological intervention could not only improve the nervous symptoms, but also regulate the blood levels of lipids and sex hormones in patients of peri-menopausal syndrome complicated with hyperlipidemia.
Similar content being viewed by others
References
Yu Q, Chen X. Progress on research of traditional Chinese medicine treatment for menopausal syndrome. J Liaoning Coll Tradit Med (Chin) 2009;11(2):47–48.
Chen XL, AN SX. Changes of hormone and lipoprotein in postmenopausal women with coronary heart disease and the effects of nursing intervention on it. Matern Child Health Care China (Chin) 2007;22:4442–4443.
Anderson HV. Estrogen therapy, atherosclerosis, and clinical cardiovascular events. Circulation 1996;94:1809–1811.
Jin XL. Exploration on formula principles of TCM in treating menopausal syndrome. Chin J Basic Med Tradit Chin Med (Chin) 2008;14:292–293.
Li L, Ren J, Du CF, Xin Y, Wang TF. Literature analyses on distribution characteristics of TCM syndromes and syndrome elements of menopausal syndrome. China J Tradit Chin Med Pharm (Chin) 2008;23:194–197.
Foster SL, Mash EJ. Assessing social validity in clinical treatment research: issues and procedures. J Consul Clin Psychol 1999;67:309–319.
Kazdin AE. Assessing the clinical or applied importance of behavior change through social validation. Behav Modificat, 1977;1:427–452.
Zhang XY, ed. Practical obstetrics and gynecology. 2 nd. Beijng: People’s Medical Publishing House, 2003:845–850.
Focus Group of Prevention and Treatment of Dyslipidemia. Suggestion on prevention and treatment of dyslipidemia. Chin J Cardiol (Chin) 1997;25:169–172.
State Administration of Traditional Chinese Medicine, P. R. China. Standard for diagnosis and efficacy evaluation of traditional Chinese medicine diseases and syndromes. Nanjing: Nanjing University Press; 1994:66
Zheng XY, ed. Ministry of Health, P. R. China. Guiding principle of clinical research on new drugs of traditional Chinese medicine. 1993:16, 96.
Wang XD, Wang XL, Ma H, eds. Rating scale for mental health. Beijing: Press of Chinese Mental Health Journal, 1999:31–35.
Hu LL. Survey on psychohygiene of peri-menopausal women and its influential factors. Chin Gen Prac (Chin) 2001;4:469–470.
He Y, Li LR. Exploration on the mental health and the influential factors in women with menopausal syndrome. J Pract Obstet Gynecol (Chin) 1997;12(2):79.
Cao ZY, ed. Chinese obstetrics and gynecology. 1st ed. Beijing: People’s Medical Publishing House, 1999:2537.
Xu LW, Zhang SJ, Sun ZJ. Thinking on the genesis and pathogenesis of menopausal syndrome. J Tradit Chin Med (Chin) 2008;49:1031–1033.
Song SJ, Li FF, Yin ZW, Yue H, Hou YJ. Research on function of Heshouwu on experimental hyperlipidemia. J Hebei Tradit Chin Med Pharmacol (Chin) 2007;18(4):27–28.
Zhu CP, Zhang SH. Effects of Lycium barbarum Polysaccharides on serum lipids and lipid peroxidation in hyperlipidemic mice. Acta Nutr Sin (Chin) 2005;7:79–80.
Wang CY, Jiang GR, Liang GQ, Wu HJ. Effect of Lycium barbarum polysaccharides on rats’ sexual organ indexes and serum sexual hormone levels. J Jiangsu Univ (Med Edition, Chin) 2007;17:118–120.
Zhang HX, Liu JG, Ma LB, Shi DZ, Li XL, Liang XM. Experimental study of effects of drug couples of bupleurum root and red peony root, vinegar-baked bupleurum root and white peony root on hyperlipidemia in rats. Chin J Exp Med Form (Chin) 2003;9(2):21–23.
XM, Liu QY. Pharmacodynamic study of Xiaoyao Oral Liquid. J Anhui Tradit Chin Med (Chin) 2000;19(6):39.
Dong XF, Deng HQ, Wang L, Huang GH, Liao WM. Effects of psychological intervention on perimenopause women with chief complaints of chest distress. Matern Child Health Care China (Chin) 2008;23:1970–1972.
Wang XX. Effects of psychological intervention on efficacy in patients with menopausal syndrome. Modern Prevent Med (Chin) 2008;35:4163–4164.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Qian, Lq., Wang, B., Niu, Jy. et al. Assessment of the clinical effect of Chinese medicine therapy combined with psychological intervention for treatment of patients of peri-menopausal syndrome complicated with hyperlipidemia. Chin. J. Integr. Med. 16, 124–130 (2010). https://doi.org/10.1007/s11655-010-0124-x
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11655-010-0124-x