Abstract
Background
The Fracture Liaison Service (FLS) care model, a care coordination program for patients experiencing a fragility fracture, is proven to improve management of patients with an osteoporotic fracture, but treatment initiation gaps persist.
Objective
We describe the evolution of a centralized FLS within a university-based healthcare system, including impact of adding clinical pharmacist consultation, and describe circumstances surrounding continued care gaps.
Design
Cohort analysis of osteoporosis medication initiation before FLS, after initial implementation, and after addition of pharmacist consultation.
Patients
Individuals aged 65 and older experiencing any fragility fracture between 7/1/16 and 3/31/22.
Intervention
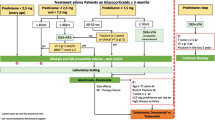
A centralized team outreached eligible patients, ordered dual x-ray absorptiometry and laboratory tests as needed, and scheduled an osteoporosis-focused primary care appointment. Three years after FLS implementation, clinical pharmacist consultative review was added prior to the primary care visit.
Main Measures
Initiation of osteoporosis pharmacologic therapy, completion of DXA, primary care follow-up rate, and description of circumstances where therapy was not initiated.
Key Results
Of 1204 new fractures between 7/1/16 and 3/31/22, 315 patients were enrolled in one of two FLS phases, and 89 eligible historical controls were identified. Medication initiation rates went from 22/89 (25%) pre-FLS to 201/428 (47%) after-FLS phase 1 [POST1] (p<0.001) and to 106/187 (57%) after FLS phase 2 (POST2), when clinical pharmacist consultation was added (p=0.03 versus POST1). DXA was completed in 56/89 (67%) of pre-FLS patients, 364/428 (85%) POST1 patients (p<0.001 versus pre), and 163/187 (87%) POST2 (p< 0.001 versus PRE, p=0.59 versus POST1). Of 375 patients who did not initiate osteoporosis medication, more in the combined post-FLS cohorts attended a follow-up primary care appointment (233/308, 76% attended, versus pre-FLS 41/67, 61%, p=0.016).
Conclusion
An FLS including centralized outreach and care coordination significantly improved patient follow-up, DXA, and medication initiation. Addition of de-centralized pharmacist consultation further improved medication initiation rates.



Similar content being viewed by others
References
LeBoff MS, Greenspan SL, Insogna KL, et al. The clinician's guide to prevention and treatment of osteoporosis. Osteoporos Int. 2022 Oct;33(10):2049-102.
Burge R, Dawson-Hughes B, Solomon DH, Wong JB, King A, Tosteson A. Incidence and economic burden of osteoporosis-related fractures in the United States, 2005-2025. J Bone Miner Res. 2007 Mar;22(3):465-75.
Eastell R, Rosen CJ, Black DM, Cheung AM, Murad MH, Shoback D. Pharmacological Management of Osteoporosis in Postmenopausal Women: An Endocrine Society* Clinical Practice Guideline. J Clin Endocrinol Metab. 2019 May 1;104(5):1595-622.
Desai RJ, Mahesri M, Abdia Y, et al. Association of Osteoporosis Medication Use After Hip Fracture With Prevention of Subsequent Nonvertebral Fractures: An Instrumental Variable Analysis. JAMA Netw Open. 2018 Jul 6;1(3):e180826.
Harvey NC, McCloskey EV, Mitchell PJ, et al. Mind the (treatment) gap: a global perspective on current and future strategies for prevention of fragility fractures. Osteoporos Int. 2017 May;28(5):1507-29.
Hawley S, Javaid MK, Prieto-Alhambra D, et al. Clinical effectiveness of orthogeriatric and fracture liaison service models of care for hip fracture patients: population-based longitudinal study. Age Ageing. 2016 Mar;45(2):236-42.
Wu CH, Tu ST, Chang YF, et al. Fracture liaison services improve outcomes of patients with osteoporosis-related fractures: A systematic literature review and meta-analysis. Bone. 2018 Jun;111:92-100.
Osteoporosis Management in Women Who Had a Fracture (OMW). National Center for Quality Assessment (NCQA); 2022 [updated 2022; cited 2023 9/29/23]; Available from: https://www.ncqa.org/hedis/measures/osteoporosis-management-in-women-who-had-a-fracture/. Accessed December 1, 2023.
Barton DW, Piple AS, Smith CT, Moskal SA, Carmouche JJ. The Clinical Impact of Fracture Liaison Services: A Systematic Review. Geriatr Orthop Surg Rehabil. 2021;12:2151459320979978.
Walters S, Khan T, Ong T, Sahota O. Fracture liaison services: improving outcomes for patients with osteoporosis. Clin Interv Aging. 2017;12:117-27.
Kim M, Brunetti V, Cosman F, Curtis JR, Lewiecki EM, Phelan M, Samai P, McDermott M, Lin TC, Brookhart MA, Hurwitz K. Current trends in the risk of subsequent fracture after initial fracture, and post-fracture treatment among commercially insured postmenopausal women in the United States ASBMR 2023 Annual Meeting; October 13-16, 2023; Vancouver, BC, Canada2023.
Wallace MA, Hammes A, Rothman MS, et al. Fixing a Fragmented System: Impact of a Comprehensive Geriatric Hip Fracture Program on Long-Term Mortality. Perm J. 2019;23.
Wu CH, Chen CH, Chen PH, et al. Identifying characteristics of an effective fracture liaison service: systematic literature review. Osteoporos Int. 2018 May;29(5):1023-47.
Summers KM, Brock TP. Impact of pharmacist-led community bone mineral density screenings. Ann Pharmacother. 2005 Feb;39(2):243-8.
Wopat M, Breslow R, Chesney K, et al. Implementation of a pharmacist and student pharmacist-led primary care service to identify and treat rural veterans at risk for osteoporotic fracture. J Am Pharm Assoc (2003). 2021 Nov-Dec;61(6):e105-e12.
B B. FRI0528 Successful implementation of a pharmacist-led fracture liaison service at a us veteran affairs (VA) hospital. Annals of the Rheumatic Diseases 2017;76:691.
Heilmann RM, Friesleben CR, Billups SJ. Impact of a pharmacist-directed intervention in postmenopausal women after fracture. Am J Health Syst Pharm. 2012 Mar 15;69(6):504-9.
Nakayama A, Major G, Holliday E, Attia J, Bogduk N. Evidence of effectiveness of a fracture liaison service to reduce the re-fracture rate. Osteoporos Int. 2016 Mar;27(3):873-9.
Javaid MK. Efficacy and efficiency of fracture liaison services to reduce the risk of recurrent osteoporotic fractures. Aging Clin Exp Res. 2021 Aug;33(8):2061-7.
Scholten DJ, 2nd, Bray JK, Wang KY, Lake AF, Emory CL. Implementation of a fracture liaison service and its effects on osteoporosis treatment adherence and secondary fracture at a tertiary care academic health system. Arch Osteoporos. 2020 May 28;15(1):80.
Wu CH, Kao IJ, Hung WC, et al. Economic impact and cost-effectiveness of fracture liaison services: a systematic review of the literature. Osteoporos Int. 2018 Jun;29(6):1227-42.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest:
The authors have no conflicts of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Billups, S.J., Fixen, D.R., Schilling, L.M. et al. Lessons Learned: Evaluation of Fracture Liaison Service Quality Improvement Efforts in a Large Academic Healthcare System. J GEN INTERN MED (2023). https://doi.org/10.1007/s11606-023-08568-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11606-023-08568-8