Abstract
Background
Rectal bleeding is the most common presenting symptom of colorectal cancer, and guidelines recommend timely follow-up, usually with colonoscopy to ensure timely diagnoses of colorectal cancer.
Objective
Identify loop closure rates and vulnerable process points for patients with rectal bleeding.
Design
Retrospective cohort study, using medical record review of patients aged ≥ 40 with index diagnosis of rectal bleeding at 2 primary practices—an urban academic practice and affiliated community health center, between January 1, 2018, and December 31, 2020. Patients were classified as having completed recommended follow-up workup (“closed loop”) vs. not (“open loop”). Open loop patient cases were categorized into six types of process failures.
Participants
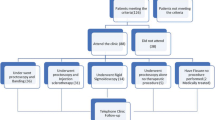
A total of 837 patients had coded diagnoses of rectal bleeding within study window. Sixty-seven were excluded based on prior colectomy, clinical presentation more consistent with upper GI bleed, no rectal bleeding documented on chart review, or expired during the follow-up period, leaving 770 patients included.
Main Measures
Primary outcomes were percentages of patient cases classified as “open loops” and distribution of these cases into six categories of process failure that were identified.
Key Results
22.3% of patients (N = 172) failed to undergo timely recommended workup for rectal bleeding. Largest failure categories were patients for whom no procedure was ordered (N = 62, 36%), followed by patients with procedures ordered but never scheduled (N = 44, 26%) or scheduled but subsequently cancelled or not kept (N = 31, 18%). While open loops increased after the onset of the COVID-19 pandemic, this difference was not significant within our study period.
Conclusions
Significant numbers of patients presenting to primary care with rectal bleeding fail to undergo recommended workup. The majority either have no procedure ordered, or procedure ordered but never scheduled or cancelled and not kept, suggesting these are important failure modes to target in future interventions. Ensuring reliable ordering and processes for timely scheduling and completion of procedures represent critical areas for improving the diagnostic process for patients with rectal bleeding in primary care.

Similar content being viewed by others
References
Crosland A, Jones R. Rectal bleeding: prevalence and consultation behaviour. BMJ. 1995;311(7003):486-488.
Astin M, Griffin T, Neal RD, Rose P, Hamilton W. The diagnostic value of symptoms for colorectal cancer in primary care: a systematic review. Br J Gen Pract. 2011;61(586):e231-243.
Shields HM, Stoffel EM, Chung DC, et al. Disparities in evaluation of patients with rectal bleeding 40 years and older. Clin Gastroenterol Hepatol. 2014;12(4):669-675; quiz e633.
Weingart SN, Stoffel EM, Chung DC, et al. Delayed Workup of Rectal Bleeding in Adult Primary Care: Examining Process-of-Care Failures. Jt Comm J Qual Patient Saf. 2017;43(1):32-40.
Ellis BG, Thompson MR. Factors identifying higher risk rectal bleeding in general practice. Br J Gen Pract. 2005;55(521):949-955.
du Toit J, Hamilton W, Barraclough K. Risk in primary care of colorectal cancer from new onset rectal bleeding: 10 year prospective study. BMJ. 2006;333(7558):69-70.
Cancer Stat Facts: Colorectal Cancer. 2019. https://seer.cancer.gov/statfacts/html/colorect.html. Accessed 3 Nov 2023.
Percac-Lima S, Pace LE, Nguyen KH, et al. Diagnostic Evaluation of Patients Presenting to Primary Care with Rectal Bleeding. J Gen Intern Med. 2018;33(4):415-422.
Committee ASoP, Pasha SF, Shergill A, et al. The role of endoscopy in the patient with lower GI bleeding. Gastrointest Endosc. 2014;79(6):875-885.
Atlas SJ, Feuerstein JD, Lim R, Mishkin D, Percac-Lima S, Roseto J, Ryou M, Sields HM. Prevention and Early Detection of Colorectal Cancer: A CRICO Decision Support Tool. 2019. https://www.rmf.harvard.edu/Risk-Prevention-and-Education/Guidelines-and-Algorithms-Catalog-Page/Guidelines-Algorithms/2019/CRC-Decision-Support-Tool. Accessed 3 Nov 2023.
Nehls N, Yap TS, Salant T, et al. Systems engineering analysis of diagnostic referral closed-loop processes. BMJ Open Qual. 2021;10(4):e001603.
Schiff GD, Bearden T, Hunt LS, et al. Primary Care Collaboration to Improve Diagnosis and Screening for Colorectal Cancer. Jt Comm J Qual Patient Saf. 2017;43(7):338-350.
Ricciardiello L, Ferrari C, Cameletti M, et al. Impace of SARS-CoV-2 Pandemic on Colorectal Cancer Screening Delay: Effect on Stage Shift and Increased Mortality. Clin Gastroenterol Hepatol. 2021 Jul; 19 (7):1410-1417
Phillips RS, Benneyan J, Bargal B et al. Closing the Loop: Re-engineering the Assessment and Tracking of Symptoms in Primary Care. J Gen Intern Med. 2023; 38(4), pp.1054-1058
Imley T, Kanter MH, Timmins R, et al. Creating a Safety net Process to Improve Colon Cancer DIagnosis in Patients with Rectal Bleeding. Perm J 2022; 26:22.034
Ali MK, McKeever Bullard K, Gregg EW, Del Rio C. A cascade of care for diabetes in the United States: visualizing the gaps. Ann Intern Med. 2014;161(10): 681-689.
Siegel RL, Wagle NS, Cercek A, et al. Colorectal cancer statistics, 2023. CA Cancer J Clin 73(3):233-254
Funding
This work was supported in part by the Agency for Healthcare Research and Quality (AHRQ) grant 1R18HS027282.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they do not have a conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Mark D. Aronson and Gordon D. Schiff share senior authorship.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Campbell, K.A., Sternberg, S.B., Benneyan, J. et al. Completion Rates and Timeliness of Diagnostic Colonoscopies for Rectal Bleeding in Primary Care. J GEN INTERN MED 39, 985–991 (2024). https://doi.org/10.1007/s11606-023-08513-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-023-08513-9