Abstract
Primary care is the foundation of the health care system and the basis for new payment and delivery reforms in the USA. Yet since 2008, primary care visit rates dropped by 6–25% across a range of populations in five sources of national survey and administrative data. We hypothesize three likely mechanisms behind the decline: decreases in patients’ ability, need, or desire to seek primary care; changes in primary care practice such as greater use of teams and non-face-to-face care; and replacement of in-person primary care visits with alternatives such as specialist, retail clinic, and commercial telemedicine visits. These mechanisms require further investigation. In the meantime, the trend prompts us to optimize the primary care visit and embrace the growth of alternatives while preserving the fundamental benefits of primary care.
Similar content being viewed by others
Nobody goes to their primary care office anymore. It’s too crowded. So might say Yogi Berra about a surprising trend in US health care: primary care visit rates are on the decline. Between 2008 and 2016, visits per person to primary care physicians (PCPs) dropped by 6–25% across a range of populations in five sources of national survey and administrative data capturing commercial, Medicare, and nationally representative samples (Fig. 1).
Change in per capita primary care and specialty visit rates between 2008 and 2016. Percentage change in annual per capita visit rates between 2008 and 2015 (nationally representative surveys, Medicare, and commercial data) and between 2012 and 2016 (Health Care Cost Institute data). National survey of office visits analysis was based on National Ambulatory Medical Care Survey (NAMCS; all ages); national panel survey analysis was based on Medical Expenditure Panel Survey (MEPS) data on office and outpatient visits (all ages); Medicare analysis was based on 20% sample of fee-for-service Medicare beneficiaries (18 years and older); commercial analysis was based on 100% sample of claims from large national insurer (18–64 years old); Health Care Cost Institute analysis was based on data obtained from the publicly available 2016 Health Care Cost and Utilization Report (< 65 years old with employer sponsored insurance; available at http://www.healthcostinstitute.org/report/2016-health-care-cost-utilization-report/). Primary care physician was defined as a National Provider Identifier (NPI) with specialty in General Practice, Family Practice, Internal Medicine, or Geriatric Medicine in Medicare; in commercial data, the definition also included Pediatrics; in NAMCS and MEPS, the definition also included Pediatrics and Obstetrics and Gynecology. Nurse practitioners and physician assistants were not included because specialties for these clinicians were not consistently recorded in the data. Visits were identified by Current Procedural Terminology/Healthcare Common Procedure Coding System codes 99201-99215, 99381-99429 (commercial only), and G0402, G0438, and G0439 (Medicare only).
This decline is notable because many believe, and a growing literature supports, that primary care is key to improving health outcomes and stemming unsustainable cost growth in the USA.1,2,3,4 In kind, policy leaders have worked to bolster primary care in a country that has invested less in this foundational specialty than its peers.5, 6 The Affordable Care Act increased PCP reimbursements and encouraged trainees to enter the field.7 Payment and delivery reforms such as the Accountable Care Organization (ACO) and the Patient Centered Medical Home were built upon the primary care relationship.7, 8 To the extent that these investments were meant to shift patient interactions toward primary care (and its main delivery mechanism: the office visit), the decline implies they have fallen short.
And yet, this trend is not necessarily a defeat for primary care and what it was intended to accomplish. In our evolving ambulatory care landscape—shaped by gains in technology and rising patient expectations for convenience and choice—any value assessment or policy reaction must consider the decline within this larger context, as well as its impact on patient outcomes. Here, we untangle potential mechanisms behind the decline (Table 1) and address implications for policy and delivery redesign.
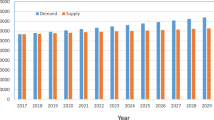
So why are PCP visit rates falling? We hypothesize three overarching mechanisms. The first is Mr. Berra’s: patients may have trouble accessing primary care, or have less need or desire to do so. The aging US population with greater insurance coverage under the Affordable Care Act has overwhelmed our capacity to deliver primary care, exacerbating already long wait times for a new or follow-up visit.9, 10 In particular, the stagnant supply and uneven geographic distribution of PCPs,10 who are also more likely to work part time,11 have only been partially alleviated by the rise in physician assistants and nurse practitioners playing these roles.12 The lack of timely appointments, coupled with growth in high-deductible health plans and out-of-pocket costs as well as heightened patient expectations for timely and accessible care, has unfavorably tipped the perceived (or actual) cost-benefit trade-off for a PCP visit, leading Americans to delay visits, forgo them entirely, or seek alternatives.13
Second, and this may be the good news, primary care clinics may be getting more done at each in-person visit while better meeting their patients’ needs outside of that visit.14 PCPs increasingly interact with their patients through online portals, phone calls, or virtual visits.15 Team members including nurses, care managers, and population health coordinators use chronic disease registries, for example, to track patients between visits. Though primary care clinicians and teams have being doing aspects of this work (unpaid) for decades, it is now explicitly supported through mechanisms like monthly care management fees and virtual visit reimbursements, often in the context of alternative payment and delivery models.16
Third, with more complicated implications, patients are going elsewhere for their care. For instance, we found a rise (or at least a lesser decline) in specialist visit rates (Fig. 1). This could be due to the rising complexity of medical diagnoses and treatments that PCPs may not have the knowledge or time to address17 or to patients’ increasing willingness or ability to self-refer. For patients with conditions like HIV, diabetes, or cancer, specialists may function appropriately as de facto PCPs. In addition, patients accustomed to convenient, on-demand services in other aspects of their lives are opting for care in alternative settings such as retail clinics and urgent care centers, or via direct-to-consumer telemedicine services.18,19,20 Growing access to Internet-based health information,21 symptom checkers, and virtual patient communities may preclude seeking formal medical care altogether.
Alternative payment and delivery models—designed in part to strengthen primary care—have likely played a hand in these mechanisms. For example, the increased attention to primary care in reform efforts may have the unintended consequence of worsening inefficiencies in primary care delivery (thereby reducing capacity), since PCPs bear the brunt of data documentation and reporting requirements in these models. ACOs, charged with lowering costs and improving quality across a PCP-attributed patient population, have tried to shift care from specialty or higher cost settings to primary care by expanding primary care clinic hours, for example. Yet, other ACO strategies—such as care coordination and panel-based primary care compensation—encourage decreased use of in-person primary care visits while specialists, still largely paid through paid fee-for-service,22 continue to be rewarded for seeing patients more often.
Of course, each of these mechanisms require further investigation, and judgment of the PCP visit decline should rest on which mechanisms dominate, why there are differences in the rate of decline across different populations (Fig. 1), how visit rates correlate with other measures of health care delivery (e.g., number of PCPs per capita), and most importantly, the impact on outcomes and spending. The USA already has lower physician visit rates than most other developed countries,6 and we have more to learn about the “right” visit frequency.3, 23
But in the meantime, the trend prompts us to rethink the role of primary care within the evolving ambulatory care landscape while preserving the fundamentals that led policymakers to bet on this field in the first place. For instance, one core function of primary care is to provide patients with care continuity—traditionally measured by in-person physician visits.1, 2 But if the underlying goal of continuity is to establish a trusting, longitudinal relationship with one’s primary clinician, we should consider the full spectrum of in-person and virtual interactions that might contribute to this goal.
So how can primary care work better in the current environment? First, for the clinical scenarios in which in-person primary care is still best, we need to make these visits worthwhile for patients. For instance, offer point-of-care laboratory testing to check and act on diabetes markers in the course of a visit24 or use decision aids to facilitate more productive conversations.25 We should make it easier for patients to schedule and attend these visits—for example, through online self-scheduling and text-based visit reminders—with the added benefit of improving capacity via lower “no-show” rates.26
Second, we should embrace the inevitability of care shifting outside of the primary care office visit. All primary care clinics should offer non-face-to-face care for their patients, investing in technology and restructuring clinicians’ schedules to incorporate this work sustainably as Kaiser Permanente and others have done.14 At the same time, we ought to pursue strategic partnerships between traditional primary care and alternative sources of care. For example, CVS Minute Clinic offers blood pressure management visits with nurse practitioners through a commonly used electronic health record (EHR), so visit notes are visible to PCPs who use a linked EHR. The key will be preserving continuity and managing hand-offs without introducing errors or disrupting PCP workflows, thereby contributing to burnout. Because the array of care-seeking options is dizzying,18 we should make it easier for patients to consult a human being in their primary care office, or a care navigator mobile application, for a quick answer on where to go based on their needs and preferences. Finally, we should better leverage value-based delivery and payment models like ACOs and Comprehensive Primary Care to accomplish these goals—in short, to provide the right care in the right modality for our patients.23
To put all of this in economic terms, in-person primary care visits are losing market share at a time when we may need primary care more than ever. Rather than mourn this as a loss, we should understand and prepare for the future this trend suggests. As Yogi Berra also reminded us, “When you come to a fork in the road, take it.”
References
Friedberg MW, Hussey PS, Schneider EC. Primary Care: A Critical Review Of The Evidence On Quality And Costs Of Health Care. Health Aff. 2010;29(5):766–772. doi:https://doi.org/10.1377/hlthaff.2010.0025.
Starfield B, Shi L, Macinko J. Contribution of Primary Care to Health Systems and Health. Milbank Q. 2005;83(3):457–502. doi:https://doi.org/10.1111/j.1468-0009.2005.00409.x
Rose AJ, Timbie JW, Setodji C, Friedberg MW, Malsberger R, Kahn KL. Primary Care Visit Regularity and Patient Outcomes: an Observational Study. J Gen Intern Med. 2018;1–8. doi:https://doi.org/10.1007/s11606-018-4718-x.
Basu S, Berkowitz SA, Phillips RL, Bitton A, Landon BE, Phillips RS. Association of Primary Care Physician Supply With Population Mortality in the United States, 2005-2015. JAMA Intern Med. 2019. doi:https://doi.org/10.1001/jamainternmed.2018.7624
Schneider EC, Squires D. From Last to First — Could the U.S. Health Care System Become the Best in the World? N Engl J Med. 2017;377(10):901–904. doi:https://doi.org/10.1056/NEJMp1708704.
Koller CF, Khullar D. Primary Care Spending Rate — A Lever for Encouraging Investment in Primary Care. N Engl J Med. 2017;377(18):1709–1711. doi:https://doi.org/10.1056/NEJMp1709538.
Davis K, Abrams M, Stremikis K. How the Affordable Care Act will strengthen the nation’s primary care foundation. J Gen Intern Med. 2011;26(10):1201–1203. doi:https://doi.org/10.1007/s11606-011-1720-y.
Rittenhouse DR, Shortell SM, Fisher ES. Primary Care and Accountable Care — Two Essential Elements of Delivery-System Reform. N Engl J Med. 2009;361(24):2301–2303. doi:https://doi.org/10.1056/NEJMp0909327.
Merritt Hawkins. 2017 Survey of Physician Appointment Wait Times. 2017. https://www.merritthawkins.com/uploadedFiles/MerrittHawkins/Content/Pdf/mha2017waittimesurveyPDF.pdf. Accessed 9 May 2019.
Dall T, West T, Chakrabarti R, Reynolds R, Iacobucci W. 2018 Update The Complexities of Physician Supply and Demand: Projections from 2016 to 2030 Final Report Association of American Medical Colleges. 2018. https://aamc-black.global.ssl.fastly.net/production/media/filer_public/bc/a9/bca9725e-3507-4e35-87e3-d71a68717d06/aamc_2018_workforce_projections_update_april_11_2018.pdf. Accessed 9 May 2019.
Hedden L, Barer ML, McGrail K, Law M, Bourgeault IL. In British Columbia, the supply of primary care physicians grew, but their rate of clinical activity declined. Health Aff. 2017;36(11):1904–1911. doi:https://doi.org/10.1377/hlthaff.2017.0014.
Barnes H, Richards MR, McHugh MD, Martsolf G. Rural And Nonrural Primary Care Physician Practices Increasingly Rely On Nurse Practitioners. Health Aff. 2018;37(6):908–914. doi:https://doi.org/10.1377/hlthaff.2017.1158.
Claxton G, Rae M, Long M, Damico A, Whitmore H. Employer Health Benefits 2018 Annual Survey. Henry J Kaiser Family Foundation. doi:https://doi.org/10.1007/978-1-349-95810-8_714.
Chen C, Garrido T, Chock D, Okawa G, Liang L. The Kaiser Permanente Electronic Health Record: Transforming And Streamlining Modalities Of Care. Health Aff. 2009;28(2):323–333. doi:https://doi.org/10.1377/hlthaff.28.2.323.
Dorsey ER, Topol EJ. State of Telehealth. Campion EW, ed. N Engl J Med. 2016;375(2):154–161. doi:https://doi.org/10.1056/NEJMra1601705.
Peikes D, Dale S, Ghosh A, et al. The Comprehensive Primary Care Initiative: Effects on spending, quality, patients, and physicians. Health Aff. 2018;37(6):890–899. doi:https://doi.org/10.1377/hlthaff.2017.1678.
Østbye T, Yarnall KSH, Krause KM, Pollak KI, Gradison M, Michener JL. Is there time for management of patients with chronic diseases in primary care? Ann Fam Med. 2005;3(3):209–214. doi:https://doi.org/10.1370/afm.310.
Chang JE, Brundage SC, Chokshi DA. Convenient Ambulatory Care — Promise, Pitfalls, and Policy. N Engl J Med. 2015;373(4):382–388. doi:https://doi.org/10.1056/NEJMhpr1503336.
Pitts SR, Carrier ER, Rich EC, Kellermann AL. Where Americans Get Acute Care: Increasingly, It’s Not At Their Doctor’s Office. Health Aff. 2010;29(9):1620–1629. doi:https://doi.org/10.1377/hlthaff.2009.1026.
Poon SJ, Schuur JD, Mehrotra A. Trends in Visits to Acute Care Venues for Treatment of Low-Acuity Conditions in the United States From 2008 to 2015. JAMA Intern Med. 2018;178(10):1342. doi:https://doi.org/10.1001/jamainternmed.2018.3205.
Fox S, Duggan M. Health Online 2013. 2013. http://pewinternet.org/Reports/2013/Health-online.aspx. Accessed 9 May 2019.
Peiris D, Phipps-Taylor MC, Stachowski CA, et al. ACOs Holding Commercial Contracts Are Larger And More Efficient Than Noncommercial ACOs. 2016;35(10):1849–1856. doi:https://doi.org/10.1377/hlthaff.2016.0387.
Ganguli I, Wasfy JH, Ferris TG. What is the right number of clinic appointments?: Visit frequency and the accountable care organization. JAMA. 2015;313(19):1905–1906. doi:https://doi.org/10.1001/jama.2015.3356.
Sohn AJ, Hickner JM, Alem F. Use of Point-of-Care Tests (POCTs) by US Primary Care Physicians. J Am Board Fam Med. 2016;29(3):371–376. doi:https://doi.org/10.3122/jabfm.2016.03.150249.
Friedberg MW, Van Busum K, Wexler R, Bowen M, Schneider EC. A Demonstration Of Shared Decision Making In Primary Care Highlights Barriers To Adoption And Potential Remedies. Health Aff. 2013;32(2):268–275. doi:https://doi.org/10.1377/hlthaff.2012.1084.
Robotham D, Satkunanathan S, Reynolds J, Stahl D, Wykes T. Using digital notifications to improve attendance in clinic: systematic review and meta-analysis. BMJ Open. 2016;6(10):e012116. doi:https://doi.org/10.1136/bmjopen-2016-012116.
Acknowledgments
The authors acknowledge Thomas D. Sequist, MD, MPH.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they do not have a conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ganguli, I., Lee, T.H. & Mehrotra, A. Evidence and Implications Behind a National Decline in Primary Care Visits. J GEN INTERN MED 34, 2260–2263 (2019). https://doi.org/10.1007/s11606-019-05104-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-019-05104-5