ABSTRACT
BACKGROUND
Despite new treatment therapies and the emphasis on patient activation, nearly 50 % of diabetes patients have hemoglobin A1c levels above target. Understanding the impact of unmet treatment goals on the physician-patient relationship is important for maintaining quality care in clinical practice.
OBJECTIVE
To explore physicians’ and type 2 diabetes patients’ views of patients’ difficulty achieving diabetes treatment goals.
DESIGN
Qualitative study using in-depth interviews with a semi-structured interview guide.
PARTICIPANTS
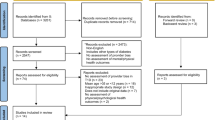
Nineteen endocrinologists and primary care physicians and 34 patients diagnosed with type 2 diabetes at least two years prior.
MAIN MEASURES
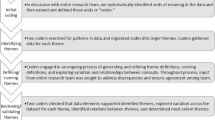
In-depth interviews with physicians and patients. A multidisciplinary research team performed content and thematic analyses.
KEY RESULTS
Qualitative analysis revealed two main findings, organized by physician and patient perspectives. Physician Perspective: Physicians’ Perceived Responsibility for Patients’ Difficulty Achieving Treatment Goals: Physicians assumed responsibility for their patients not achieving goals and expressed concern that they may not be doing enough to help their patients achieve treatment goals. Physicians’ Perceptions of Patients’ Reactions: Most speculated that their patients may feel guilt, frustration, or disappointment when not reaching goals. Physicians also felt that many patients did not fully understand the consequences of diabetes. Patient Perspective: Patients’ Self-Blame for Difficulty Achieving Treatment Goals: Patients attributed unmet treatment goals to their inability to carry out self-care recommendations. Most patients blamed themselves for their lack of progress and directed their frustration and disappointment inwardly through self-deprecating comments. Patients’ Perceptions of Physicians’ Reactions: Several patients did not know how their physician felt, while others speculated that their physicians might feel disappointed or frustrated.
CONCLUSIONS
Physicians’ perceived responsibility and patients’ self-blame for difficulty achieving treatment goals may serve as barriers to an effective relationship. Physicians and patients may benefit from a greater understanding of each other’s frustrations and challenges in diabetes management.
Similar content being viewed by others
REFERENCES
American Diabetes Association. Economic costs of diabetes in the U.S. In 2007. Diabetes Care. 2008;31(3):596-615.
Wang YC, McPherson K, Marsh T, Gortmaker SL, Brown M. Health and economic burden of the projected obesity trends in the USA and the UK. Lancet. 2011;378(9793):815–25.
Yach D, Stuckler D, Brownell KD. Epidemiologic and economic consequences of the global epidemics of obesity and diabetes. Nat Med. 2006;12(1):62–6.
Campbell C, McGauley G. Doctor-patient relationships in chronic illness: insights from forensic psychiatry. BMJ. 2005;330(7492):667–70.
Piette JD, Schillinger D, Potter MB, Heisler M. Dimensions of patient-provider communication and diabetes self-care in an ethnically diverse population. J Gen Intern Med. 2003;18(8):624–33.
Heisler M, Vijan S, Anderson RM, Ubel PA, Bernstein SJ, Hofer TP. When do patients and their physicians agree on diabetes treatment goals and strategies, and what difference does it make? J Gen Intern Med. 2003;18(11):893–902.
Kaplan SH, Greenfield S, Ware JE Jr. Assessing the effects of physician-patient interactions on the outcomes of chronic disease. Med Care. 1989;27(3 Suppl):S110–27.
Von Korff M, Gruman J, Schaefer J, Curry SJ, Wagner EH. Collaborative management of chronic illness. Ann Intern Med. 1997;127(12):1097–102.
Heisler M, Bouknight RR, Hayward RA, Smith DM, Kerr EA. The relative importance of physician communication, participatory decision making, and patient understanding in diabetes self-management. J Gen Intern Med. 2002;17(4):243–52.
Street RL Jr, Krupat E, Bell RA, Kravitz RL, Haidet P. Beliefs about control in the physician-patient relationship: effect on communication in medical encounters. J Gen Intern Med. 2003;18(8):609–16.
Bordin ES. The generalizability of the psychoanalytic concept of the working alliance. Psychotherapy: Theory, Research & Practice. 1979;26(3):252–60.
Ciechanowski PS, Katon WJ, Russo JE, Walker EA. The patient-provider relationship: attachment theory and adherence to treatment in diabetes. Am J Psychiatry. 2001;158(1):29–35.
Ciechanowski P, Russo J, Katon W, et al. Influence of patient attachment style on self-care and outcomes in diabetes. Psychosom Med. 2004;66(5):720–8.
Jahng KH, Martin LR, Golin CE, DiMatteo MR. Preferences for medical collaboration: patient-physician congruence and patient outcomes. Patient Educ Couns. 2005;57(3):308–14.
Glasgow RE, Anderson RM. In diabetes care, moving from compliance to adherence is not enough. Something entirely different is needed. Diabetes Care. 1999;22(12):2090–2.
Anderson RM, Funnell MM. Compliance and adherence are dysfunctional concepts in diabetes care. Diabetes Educ. 2000;26(4):597–604.
Clark NM, Gong M. Management of chronic disease by practitioners and patients: are we teaching the wrong things? BMJ. 2000;320(7234):572–5.
Fuertes JN, Mislowack A, Bennett J, et al. The physician-patient working alliance. Patient Educ Couns. 2007;66(1):29–36.
Escudero-Carretero MJ, Prieto-Rodriguez MA, Fernandez-Fernandez I, March-Cerda JC. Physician/patient relationship in diabetes mellitus type 1 treatment. A qualitative study. Aten Primaria. 2006;38(1):8–15.
Gavin LA, Wamboldt MZ, Sorokin N, Levy SY, Wamboldt FS. Treatment alliance and its association with family functioning, adherence, and medical outcome in adolescents with severe, chronic asthma. J Pediatr Psychol. 1999;24(4):355–65.
Williams GC, Freedman ZR, Deci EL. Supporting autonomy to motivate patients with diabetes for glucose control. Diabetes Care. 1998;21(10):1644–51.
Anderson RM, Funnell MM, Butler PM, Arnold MS, Fitzgerald JT, Feste CC. Patient empowerment. Results of a randomized controlled trial. Diabetes Care. 1995;18(7):943–9.
Greenfield S, Kaplan SH, Ware JE Jr, Yano EM, Frank HJ. Patients' participation in medical care: effects on blood sugar control and quality of life in diabetes. J Gen Intern Med. 1988;3(5):448–57.
Conn VS, Hafdahl AR, Mehr DR, Lemaster JW, Brown SA, Nielsen PJ. Metabolic effects of interventions to increase exercise in adults with type 2 diabetes. Diabetologia. 2007;50(5):913–21.
Karter AJ, Ackerson LM, Darbinian JA, et al. Self-monitoring of blood glucose levels and glycemic control: the Northern California Kaiser Permanente Diabetes registry*. Am J Med. 2001;111(1):1–9.
Pi-Sunyer FX, Maggio CA, McCarron DA, et al. Multicenter randomized trial of a comprehensive prepared meal program in type 2 diabetes. Diabetes Care. 1999;22(2):191–7.
Weinger K. Psychosocial issues and self-care. Am J Nurs. 2007;107(6 Suppl):34–8. quiz 38.
Peyrot M, Rubin RR, Lauritzen T, Snoek FJ, Matthews DR, Skovlund SE. Psychosocial problems and barriers to improved diabetes management: results of the Cross-National Diabetes Attitudes, Wishes and Needs (DAWN) Study. Diabet Med. 2005;22(10):1379–85.
Rubin RR, M P. Psychological issues and treatment for people with diabetes. J Clin Psychol. 2001;57(4):457–78.
Wdowik MJ, Kendall PA, Harris MA. College students with diabetes: using focus groups and interviews to determine psychosocial issues and barriers to control. Diabetes Educ. 1997;23(5):558–62.
Hoerger TJ, Segel JE, Gregg EW, Saaddine JB. Is glycemic control improving in U.S. adults? Diabetes Care. 2008;31(1):81–6.
Welch GW, Jacobson AM, Polonsky WH. The Problem Areas in Diabetes Scale. An evaluation of its clinical utility. Diabetes Care. 1997;20(5):760–6.
Lloyd CE, Smith J, Weinger K. Stress and diabetes: a review of the links. Diabetes Spectrum. 2005;18(2):121–7.
Weinger K, Jacobson AM. Psychosocial and quality of life correlates of glycemic control during intensive treatment of type 1 diabetes. Patient Educ Couns. 2001;42(2):123–31.
Albright TL, Parchman M, Burge SK. Predictors of self-care behavior in adults with type 2 diabetes: an RRNeST study. Fam Med. 2001;33(5):354–60.
Gonzalez JS, Delahanty LM, Safren SA, Meigs JB, Grant RW. Differentiating symptoms of depression from diabetes-specific distress: relationships with self-care in type 2 diabetes. Diabetologia. 2008;51(10):1822–5.
Gonzalez JS, Safren SA, Cagliero E, et al. Depression, self-care, and medication adherence in type 2 diabetes: relationships across the full range of symptom severity. Diabetes Care. 2007;30(9):2222–7.
Gonzalez JS, Safren SA, Delahanty LM, et al. Symptoms of depression prospectively predict poorer self-care in patients with Type 2 diabetes. Diabet Med. 2008;25(9):1102–7.
Crosson JC, Heisler M, Subramanian U, et al. Physicians' perceptions of barriers to cardiovascular disease risk factor control among patients with diabetes: results from the translating research into action for diabetes (TRIAD) study. J Am Board Fam Med. 2010;23(2):171–8.
Wens J, Vermeire E, Royen PV, Sabbe B, Denekens J. GPs' perspectives of type 2 diabetes patients' adherence to treatment: a qualitative analysis of barriers and solutions. BMC Fam Pract. 2005;6(1):20.
Freeman J, Loewe R. Barriers to communication about diabetes mellitus. Patients' and physicians' different view of the disease. J Fam Pract. 2000;49(6):507–12.
Patton MQ. How to use Qualitative Methods in Evaluation. London: Sage; 1987.
Patton M. Qualitative Evaluation and Research Methods. 2nd ed. Newbury Park: Sage; 1990.
Morse J, Field P. Qualitative Research Methods for Health Profesionals. 2nd ed. Thousand Oaks, CA: Sage Publications; 1995.
Pope C, Mays N. Qualitative Research in Health Care. 2nd ed. London: BMJ Books; 2000.
Krippendorf K. Content Analysis: An Introduction to Its Methodology. 2nd ed. Thousand Oaks, CA: Sage Publications; 2004.
Neuendorf K. The Content Analysis Guidebook. Thousands Oaks, CA: Sage Publications; 2002.
NVivo [computer program]. Version 8. Victoria, Australia: QSR International.
Miles MB, Huberman AM. Qualitative Data Analysis: An Expanded Sourcebook. 2nd ed. Thousand Oaks, California: SAGE Publications, Inc.; 1994.
Russell CK, Gregory DM. Evaluation of qualitative research studies. Evid Based Nurs. 2003;6(2):36–40.
Bennett KK, Compas BE, Beckjord E, Glinder JG. Self-blame and distress among women with newly diagnosed breast cancer. J Behav Med. 2005;28(4):313–23.
Eccleston C, Williams AC, Rogers WS. Patients' and professionals' understandings of the causes of chronic pain: blame, responsibility and identity protection. Soc Sci Med. 1997;45(5):699–709.
Friedman LC, Romero C, Elledge R, et al. Attribution of blame, self-forgiving attitude and psychological adjustment in women with breast cancer. J Behav Med. 2007;30(4):351–7.
Peel E, Parry O, Douglas M, Lawton J. Blood glucose self-monitoring in non-insulin-treated type 2 diabetes: a qualitative study of patients' perspectives. Br J Gen Pract. 2004;54(500):183–8.
Scambler G. Health-related stigma. Sociol Health Illn. 2009;31(3):441–55.
Tuncay T, Musabak I, Gok DE, Kutlu M. The relationship between anxiety, coping strategies and characteristics of patients with diabetes. Health Qual Life Outcomes. 2008;6:79.
Voth J, Sirois FM. The role of self-blame and responsibility in adjustment to inflammatory bowel disease. Rehabil Psychol. 2009;54(1):99–108.
Glinder JG, Compas BE. Self-blame attributions in women with newly diagnosed breast cancer: a prospective study of psychological adjustment. Health Psychol. 1999;18(5):475–81.
Rayman K. GE. Home alone: the experience of women with type 2 diabetes who are new to intensive control. Health Care for Women International. 2004;25:900–15.
Anderson RJ, Freedland KE, Clouse RE, Lustman PJ. The prevalence of comorbid depression in adults with diabetes: a meta-analysis. Diabetes Care. 2001;24(6):1069–78.
Katon W, von Korff M, Ciechanowski P, et al. Behavioral and clinical factors associated with depression among individuals with diabetes. Diabetes Care. 2004;27(4):914–20.
Gonzalez JS, Peyrot M, McCarl LA, et al. Depression and diabetes treatment nonadherence: a meta-analysis. Diabetes Care. 2008;31(12):2398–403.
Ciechanowski PS, Katon WJ, Russo JE, Hirsch IB. The relationship of depressive symptoms to symptom reporting, self-care and glucose control in diabetes. Gen Hosp Psychiatry. 2003;25(4):246–52.
Dyrbye LN, Massie FS Jr, Eacker A, et al. Relationship between burnout and professional conduct and attitudes among US medical students. JAMA. 2010;304(11):1173–80.
Shanafelt TD, Bradley KA, Wipf JE, Back AL. Burnout and self-reported patient care in an internal medicine residency program. Ann Intern Med. 2002;136(5):358–67.
Thomas NK. Resident burnout. JAMA. 2004;292(23):2880–9.
Ritholz MD, Beverly EA, Abrahamson MJ, Brooks KM, Hultgren BA, Weinger K. Physicians' Perceptions of the Type 2 diabetes multidisciplinary treatment team: a qualitative study. Diabetes Educ. 2011;37(6):794–800.
Acknowledgement
This work was supported by the Kathleen P. Welsh Fund, NIDDK RO1-060115, the Diabetes and Endocrinology Research Core NIH P30 DK36836, and the NIH Training Grant No. T32 DK007260. We thank the physicians and patients who shared their experiences and perceptions with us. We also thank Dr. Nadine Palermo, Nicholas Hebert, and Ross Markello for their useful comments on the manuscript.
Conflict of Interest
No author received other support for this grant other than funding from the Kathleen P. Welsh Fund. However, Martin J. Abrahamson, MD has provided consulting services to Novo Nordisk, Halozyme, and Boehringer Ingelheim. No other author has anything to declare.
Author Contributions
E.A.B. conducted interviews; read, coded, and thematically analyzed the transcripts; and wrote the manuscript. M.D.R. conducted interviews; read, coded, and thematically analyzed the transcripts; and reviewed and edited the manuscript. B.A.H. and K.M.B. read, coded, and thematically analyzed the transcripts and reviewed and edited the manuscript. Y.L. analyzed the quantitative data and reviewed and edited the manuscript. M.J.A. reviewed and edited the manuscript. K.W. had the initial idea for this study and wrote the research proposal; read, coded, and thematically analyzed the transcripts; and reviewed and edited the manuscript. All contributors had access to the data and can take responsibility for the integrity of the data and the accuracy of the data analysis.
Author information
Authors and Affiliations
Corresponding author
Additional information
Funded by Kathleen P. Welsh Fund, NIDDK RO1-060115, NIH P30 DK36836, NIH Training Grant No. T32 DK007260
Rights and permissions
About this article
Cite this article
Beverly, E.A., Ritholz, M.D., Brooks, K.M. et al. A Qualitative Study of Perceived Responsibility and Self-Blame in Type 2 Diabetes: Reflections of Physicians and Patients. J GEN INTERN MED 27, 1180–1187 (2012). https://doi.org/10.1007/s11606-012-2070-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-012-2070-0