ABSTRACT
BACKGROUND
Clinical practice guidelines (CPG) are meant to consider important values such as patient preferences.
OBJECTIVE
To assess how well clinical practice guidelines (CPGs) integrate evidence on patient preferences compared with that on treatment effectiveness.
DESIGN
A cross-sectional review of a listing in 2006 of CPGs judged to be the best in their fields by an external joint government and medical association body.
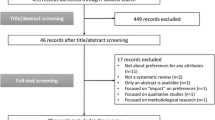
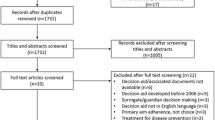
STUDY SELECTION
Exclusion criterion was unavailability in electronic format. Sixty-five of 71 listed CPGs met selection criteria.
MEASUREMENTS
Two instruments originally constructed to evaluate the overall quality of CPGs were adapted to specifically assess the quality of integrating information on patient preference vs. treatment effectiveness. Counts of words and references in each CPG associated with patient preferences vs. treatment effectiveness were performed. Two reviewers independently assessed each CPG.
MAIN RESULTS
Based on our adapted instruments, CPGs scored significantly higher (p < 0.001) on the quality of integrating treatment effectiveness compared with patient preferences evidence (mean instrument one scores on a scale of 0.25 to 1.00: 0.65 vs. 0.43; mean instrument two scores on a scale of 0 to 1: 0.58 vs. 0.18). The average percentage of the total word count dedicated to treatment effectiveness was 24.2% compared with 4.6% for patient preferences. The average percentage of references citing treatment effectiveness evidence was 36.6% compared with 6.0% for patient preferences.
CONCLUSION
High quality CPGs poorly integrate evidence on patient preferences. Barriers to incorporating preference evidence into CPGs should be addressed.

Similar content being viewed by others
REFERENCES
Singer DE, Albers GW, Dalen JE, Go AS, Halperin JL, Manning WJ. Antithrombotic therapy in atrial fibrillation: the Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy. Chest. 2004;126:429S–456S.
Holoweiko M. What cookbook medicine will mean for you. Med Econ. 1989; 66: 118–20, 125–117, 130–113.
Sackett D, Strauss S, Richardson W, Rosenberg W, Haynes R. Evidence-based medicine: how to practice and teach EBM. 2nd ed. London: Churchill Livingstone; 2000.
Hayward RS, Wilson MC, Tunis SR, Bass EB, Guyatt G. Users’ guides to the medical literature. VIII. How to use clinical practice guidelines. A. Are the recommendations valid? The Evidence-Based Medicine Working Group. JAMA. 1995;274:570–4.
Gafni A, Charles C, Whelan T. The physician-patient encounter: the physician as a perfect agent for the patient versus the informed treatment decision-making model. Soc Sci Med. 1998;47:347–54.
Ristvedt SL, McFarland EG, Weinstock LB, Thyssen EP. Patient preferences for CT colonography, conventional colonoscopy and bowel preparation. Am J Gastroenterol. 2003;98:578–85.
Ross CK, Steward CA, Sinacore JM. The importance of patient preferences in the measurement of health care satisfaction. Medical Care. 1993;31:1138–49.
Gold MR, Siegel JE, Russell LB, Weinstein MC, eds. Cost-Effectiveness in Health and Medicine. New York: Oxford University Press; 1996.
Gage BF, Cardinalli AB, Owens DK. The effect of stroke and stroke prophylaxis with aspirin or warfarin on quality of life. Arch Intern Med. 1996;156:1829–36.
Sox H, Marton K, Blatt M, Higgins M. Medical Decision MakingLondon: RSM Press; 2006.
Samsa GP, Matchar DB, Goldstein L, et al. Utilities for major stroke: results from a survey of preferences among persons at increased risk for stroke. Am Heart J. 136(4 Pt 1):703–713.
Bajorek BV, Ogle SJ, Duguid MJ, Shenfield GM, Krass I. Management of warfarin in atrial fibrillation: views of health professionals, older patients and their carers. Med J Aust. 2007;186:175–80.
Fuller R, Dudley N, Blacktop J. Avoidance hierarchies and preferences for anticoagulation—semi-qualitative analysis of older patients’ views about stroke prevention and the use of warfarin. Age Ageing. 2004;33:608–11.
Man-Son-Hing M, Laupacis A, O’Connor AM, et al. A patient decision aid regarding antithrombotic therapy for stroke prevention in atrial fibrillation: a randomized controlled trial. JAMA. 1999;282:737–43.
Man-Son-Hing M, O’Connor AM, Drake E, Biggs J, Hum V, Laupacis A. The effect of qualitative vs. quantitative presentation of probability estimates on patient decision-making: a randomized trial. Health Expect. 5:246–255
Coulter A. Paternalism or partnership? Patients have grown up—and there’s no going back. BMJ. 1999;319:719–20.
Barry MJ. Involving patients in medical decisions, how can physicians do better? JAMA. 1999;282:2356–7.
Bensing J. Bridging the gap. The separate worlds of evidence-based medicine and patient-centered medicine. Patient Educ Couns. 2000;39:17–25.
Schunemann HJ, Fretheim A, Oxman AD. Improving the use of research evidence in guideline development: 10. Integrating values and consumer involvement. Health Res Policy Syst. 2006;4: 22.
Owens DK. Spine update. Patient preferences and the development of practice guidelines. Spine. 1998;23:1073–9.
Cabana MD, Rand CS, Powe NR, et al. Why don’t physicians follow clinical practice guidelines. JAMA. 1999;282:1458–65.
Advancing the use of evidence-based clinical practice guidelines. Guidelines Advisory Committee. August 9, 2006. (Accessed January 15, 2007, at http://www.gacguidelines.ca)
Development and validation of an international appraisal instrument for assessing the quality of clinical practice guidelines: the AGREE project. Qual Saf Health Care. 2003;12:18–23.
International Statistical Classication of Diseases and Related Health Problems 10th Revision. World Health Organization. May 4, 2006. (Accessed October 1, 2006, at http://www.who.int/classifications/apps/icd/icd10online)
Shaneyfelt TM, Mayo-Smith MF, Rothwangl J. Are guidelines following guidelines? The methodological quality of clinical practice guidelines in the peer-reviewed medical literature. JAMA. 1999;281:1900–5.
Canadian Health Services Research Foundation. Weighing up the evidence: Making evidence-informed guidance accurate, achievable and acceptable. Ottawa (ON): Canadian Health Services Research Foundation; 2006.
Schattner A, Fletcher RH. Research evidence and the individual patient. Q J Med. 2003;96:1–5.
Marks DF, Murray M, Evans B, Willig C, Woodall C, Sykes CM. Health psychology: theory, research and practice. 2nd ed. Thousand Oaks, CA: Sage; 2005.
Green J, Britten N. Qualitative research and evidence based medicine. BMJ. 1998;316:1230–2.
Ryan M, Farrar S. Using conjoint analysis to elicit preference for health care. BMJ. 2000;320:1530–3.
Zimmer L. Qualitative meta-synthesis: a question of dialoguing with texts. J Adv Nurs. 2006;53:311–8.
Feldman RD, Zou GY, Vandervoort MK, Wong CJ, Nelson SA, Feagan BG. A simplified approach to the treatment of uncomplicated hypertension. A cluster randomized, controlled trial. Hypertension. 2009 Feb 23 [epub ahead of print].
Cantor SB, Spann SJ, Volk RJ, Cardenas MP, Warren MM. Prostate cancer screening: a decision analysis. J Fam Pract. 1995;41:33–41.
Krahn MD, Mahoney JE, Eckman MH, Trachtenberg J, Pauker SG, Detsky AS. Screening for prostate cancer. A decision analytic view. JAMA. 1994;272:773–80.
Frosch DL, Bhatnagar V, Tally S, Hamori CJ, Kaplan RM. A randomized controlled trial comparing alternative approaches for men considering prostate cancer screening. Arch Intern Med. 2008;168:363–9.
McAlister F, Laupacis A, Man-Son-Hing M, et al. Making choices: an atrial fibrillation treatment decision-making aid. Ottawa Health Decision Centre, Clinical Epidemiology Unit (Accessed March 2009, at http://www.canadianstrokenetwork.ca/eng/tools/downloads/decision.atrialfib.physicians.pdf)
Acknowledgements
The authors would like to thank Dr. Andreas Laupacis for discussing this project’s feasibility, Dr. Antoine Boivin for helpful discussions and for sharing his unpublished work, Drs. Rachel Chong, Geoffrey Nguyen and Angeline Chong for reviewing drafts, and the Toronto Health Economics Network for their comments on this manuscript. Funding/Support: Ms. Chen was supported by a Student Research Award from the Faculty of Pharmacy, University of Toronto. Dr. Naglie is supported by the Mary Trimmer Chair in Geriatric Medicine at the University of Toronto. Dr. Krahn is supposed by the F. Norman Hughes Chair in Pharmacoeconomics at the University of Toronto.
Conflict of interest
None disclosed.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOC 84 KB)
Rights and permissions
About this article
Cite this article
Chong, C.A., Chen, Ij., Naglie, G. et al. How Well Do Guidelines Incorporate Evidence on Patient Preferences?. J GEN INTERN MED 24, 977–982 (2009). https://doi.org/10.1007/s11606-009-0987-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-009-0987-8