Abstract
Background
A long-lasting and efficient method of managing obesity and therapeutic associated comorbidities is bariatric surgery. However, a debated comparison between one-anastomosis gastric bypass (OAGB) and sleeve gastrectomy is still essential (SG). The goal of this study is to evaluate outcomes using RCT and NRCT from 2015 to 2022.
Methods
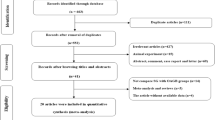
By contrasting the OAGB and SG for bariatric surgery from January 2015 to September 2022, an RCT and NRCT were prospectively gathered using the PubMed, Cochrane Library, and MEDLINE databases of published research. This meta-statistical analysis was carried out in RevMan 5.4, and the best effect model was selected based on heterogeneity.
Results
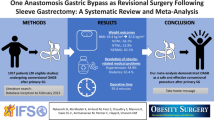
Twelve retrospective studies describing 6344 patients (3725 OAGB and 2619 SG) satisfied the inclusion criteria. A statistically significant result was in %EWL first year (MD = 8.03, 95% CI: 4.54–11.52, P < 0.05), second year (MD = 8.94, 95% CI: 2.95–14.94, P < 0.05), third year (MD = 8.93, 95% CI: 5.75–12.10, P < 0.05), fourth year (MD = 15.09, 95% CI:0.87–29.31, P < 0.05), and fifth year (MD = 14.25, 95% CI: 5.34, P < 0.05). OAGB was associated with a lower rate of remission in dyslipidemia, hypertension, diabetes mellitus, and hemorrhage. However, OAGB increased the incidence of GERD and leakage.
Conclusions
In terms of weight loss and comorbidity remission, OAGB is more effective than SG, although postoperative consequences are rather comparable between the two methods.






















Similar content being viewed by others
Data Availability
The data presented in this study are available upon reasonable request.
References
World Health Organization. Obesity and overweight fact sheet 2016. Available at: http://www.who.int/mediacentre/factsheets/fs311/en/. Last accessed March 6, 2017 - Search. https://cn.bing.com/search?q=World+Health+Organization.+Obesity+and+overweight+fact+sheet+2016.+Available+at%3A+http%3A%2F%2Fwww.who.int%2Fmediacentre%2Ffactsheets%2Ffs311%2Fen%2F.+Last+accessed+March+6%2C+2017&form=ANNTH1&refig=eceb4ceeee244a5cb1bb9e1c0deae32d. Accessed 25 Nov 2022
National Institute of Diabetes and Digestive and Kidney Diseases. Overweight and obesity statisti - Search. https://cn.bing.com/search?q=National+Institute+of+Diabetes+and+Digestive+and+Kidney+Diseases.+Overweight+and+obesity+statisti&qs=n&form=QBRE&sp=-1&pq=national+institute+of+diabetes+and+digestive+and+kidney+diseases.+overweight+and+obesity+statisti&sc=0-97&sk=&cvid=EAE0223B216E453DA011617C6C2C7564&ghsh=0&ghacc=0&ghpl=. Accessed 25 Nov 2022
Buchwald H, Avidor Y, Braunwald E, Jensen MD, Pories W, Fahrbach K, Schoelles K (2004) Bariatric surgery: a systematic review and meta-analysis. JAMA 292: 1724–1737
Lee WJ, Huang Mte, Wang W, Lin CM, Chen TC, Lai IR (2004) Effects of obesity surgery on the metabolic syndrome. Arch Surg 139: 1088–1092
Flum DR, Dellinger EP (2004) Impact of gastric bypass operation on survival: a population-based analysis. J Am Coll Surg 199: 543–551
Angrisani L, Santonicola A, Iovino P, Vitiello A, Zundel N, Buchwald H, Scopinaro N (2017) Bariatric Surgery and Endoluminal Procedures: IFSO Worldwide Survey 2014. Obes Surg 27: 2279–2289
Boza C, Salinas J, Salgado N, Pérez G, Raddatz A, Funke R, Pimentel F, Ibáñez L (2012) Laparoscopic sleeve gastrectomy as a stand-alone procedure for morbid obesity: report of 1,000 cases and 3-year follow-up. Obes Surg 22: 866–871
Mahawar KK, Jennings N, Brown J, Gupta A, Balupuri S, Small PK (2013) “Mini” gastric bypass: systematic review of a controversial procedure. Obes Surg 23: 1890–1898
Cumpston M, Li T, Page MJ, Chandler J, Welch VA, Higgins JP, Thomas J (2019) Updated guidance for trusted systematic reviews: a new edition of the Cochrane Handbook for Systematic Reviews of Interventions. Cochrane Database Syst Rev 10: ED000142
Slim K, Nini E, Forestier D, Kwiatkowski F, Panis Y, Chipponi J (2003) Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg 73: 712–716
Higgins JPT, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327: 557–560
Musella M, Apers J, Rheinwalt K, et al (2016) Efficacy of Bariatric Surgery in Type 2 Diabetes Mellitus Remission: the Role of Mini Gastric Bypass/One Anastomosis Gastric Bypass and Sleeve Gastrectomy at 1 Year of Follow-up. A European survey. Obes Surg 26: 933–940
Lee WJ, Pok EH, Almulaifi A, Tsou JJ, Ser KH, Lee YC (2015) Medium-Term Results of Laparoscopic Sleeve Gastrectomy: a Matched Comparison with Gastric Bypass. Obes Surg 25: 1431–1438
Madhok B, Mahawar KK, Boyle M, Carr WRJ, Jennings N, Schroeder N, Balupuri S, Small PK (2016) Management of Super-super Obese Patients: Comparison Between Mini (One Anastomosis) Gastric Bypass and Sleeve Gastrectomy. Obes Surg 26: 1646–1649
Kansou G, Lechaux D, Delarue J, Badic B, le Gall M, Guillerm S, Bail JP, Thereaux J (2016) Laparoscopic sleeve gastrectomy versus laparoscopic mini gastric bypass: One year outcomes. Int J Surg 33 Pt A: 18–22
Plamper A, Lingohr P, Nadal J, Rheinwalt KP (2017) Comparison of mini-gastric bypass with sleeve gastrectomy in a mainly super-obese patient group: first results. Surg Endosc 31: 1156–1162
Seetharamaiah S, Tantia O, Goyal G, Chaudhuri T, Khanna S, Singh JP, Ahuja A (2017) LSG vs OAGB-1 Year Follow-up Data-a Randomized Control Trial. Obes Surg 27: 948–954
Alkhalifah N, Lee WJ, Hai TC, Ser KH, Chen JC, Wu CC (2018) 15-year experience of laparoscopic single anastomosis (mini-)gastric bypass: comparison with other bariatric procedures. Surg Endosc 32: 3024–3031
Shivakumar S, Tantia O, Goyal G, Chaudhuri T, Khanna S, Ahuja A, Poddar A, Majumdar K (2018) LSG vs MGB-OAGB-3 Year Follow-up Data: a Randomised Control Trial. Obes Surg 28: 2820–2828
Ruiz-Tovar J, Carbajo MA, Jimenez JM, Castro MJ, Gonzalez G, Ortiz-de-Solorzano J, Zubiaga L (2019) Long-term follow-up after sleeve gastrectomy versus Roux-en-Y gastric bypass versus one-anastomosis gastric bypass: a prospective randomized comparative study of weight loss and remission of comorbidities. Surg Endosc 33: 401–410
Toh BC, Chan WH, Eng AKH, Lim EKW, Lim CH, Tham KW, Fook-Chong S, Tan JTH (2018) Five-year long-term clinical outcome after bariatric metabolic surgery: A multi-ethnic Asian population in Singapore. Diabetes, Obesity and Metabolism. 20: 1762–1765.
Jain M, Tantia O, Goyal G, Chaudhuri T, Khanna S, Poddar A, Majumdar K, Gupta S (2021) LSG vs MGB-OAGB: 5-Year Follow-up Data and Comparative Outcome of the Two Procedures over Long Term-Results of a Randomised Control Trial. Obes Surg 31: 1223–1232
Schmitz SMT, Alizai PH, Kroh A, Schipper S, Brozat JF, Plamper A, Neumann UP, Rheinwalt K, Ulmer TF (2022) Clinical outcomes after one anastomosis gastric bypass versus sleeve gastrectomy in super-super-obese patients. Surg Endosc 36: 4401–4407
Tucker ON, Szomstein S, Rosenthal RJ (2008) Indications for sleeve gastrectomy as a primary procedure for weight loss in the morbidly obese. J Gastrointest Surg 12: 662–667
Robert M, Espalieu P, Pelascini E, et al (2019) Efficacy and safety of one anastomosis gastric bypass versus Roux-en-Y gastric bypass for obesity (YOMEGA): a multicentre, randomised, open-label, non-inferiority trial. Lancet 393: 1299–1309
Mahawar KK, Carr WRJ, Balupuri S, Small PK (2014) Controversy surrounding “mini” gastric bypass. Obes Surg 24: 324–333
Wu C, Bai R, Yan W, Yan M, Song M (2020) Clinical Outcomes of One Anastomosis Gastric Bypass Versus Sleeve Gastrectomy for Morbid Obesity. Obes Surg 30: 1021–1031
Wang FG, Yu ZP, Yan WM, Yan M, Song MM (2017) Comparison of safety and effectiveness between laparoscopic mini-gastric bypass and laparoscopic sleeve gastrectomy: A meta-analysis and systematic review. Medicine. https://doi.org/10.1097/MD.0000000000008924
Quan Y, Huang A, Ye M, Xu M, Zhuang B, Zhang P, Yu B, Min Z (2015) Efficacy of Laparoscopic Mini Gastric Bypass for Obesity and Type 2 Diabetes Mellitus: A Systematic Review and Meta-Analysis. Gastroenterol Res Pract. https://doi.org/10.1155/2015/152852
Magouliotis DE, Tasiopoulou VS, Svokos AA, Svokos KA, Sioka E, Zacharoulis D (2017) One-Anastomosis Gastric Bypass Versus Sleeve Gastrectomy for Morbid Obesity: a Systematic Review and Meta-analysis. Obes Surg 27: 2479–2487
Gletsu-Miller N, Wright BN (2013) Mineral Malnutrition Following Bariatric Surgery. Advances in Nutrition 4: 506–517
Weng TC, Chang CH, Dong YH, Chang YC, Chuang LM (2015) Anaemia and related nutrient deficiencies after Roux-en-Y gastric bypass surgery: A systematic review and meta-analysis. BMJ Open 5: e006964
Pech N, Meyer F, Lippert H, Manger T, Stroh C (2012) Complications and nutrient deficiencies two years after sleeve gastrectomy. BMC Surg 12: 1–7
Acknowledgements
We thank Northern Jiangsu People’s Hospital for helpful statistical advice.
Funding
The National Natural Science Foundation of China (No. 81972269) and Key Laboratory of Basic and Clinical Transformation of Digestive and Metabolic Diseases, Yangzhou, China (YZ2020159).
Author information
Authors and Affiliations
Contributions
Muhammad Ali wrote the manuscript and participated in data analysis, Yang Wang in the manuscript selection and study design, and Jin Ji and Wei Wang helped in data collection. Final manuscript review by Daorong Wang.
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
Not applicable.
Consent for Publication
The manuscript is not under consideration for publication elsewhere.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ali, M., Wang, Y., Ji, J. et al. One Anastomosis Gastric Bypass Versus Sleeve Gastrectomy for Obesity: a Systemic Review and Meta-analysis. J Gastrointest Surg 27, 2226–2244 (2023). https://doi.org/10.1007/s11605-023-05782-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-023-05782-x