Abstract
Introduction
Parastomal hernia is a debilitating complication of stoma creation. Parastomal hernia repair with mesh reduces recurrence rates in open and laparoscopic settings. Recent comparative studies conflict with previously pooled data on optimal mesh repair technique. The objective of this study is to examine parastomal hernia recurrence rates after Sugarbaker and keyhole repairs by performing an updated systematic review and meta-analysis of comparative studies.
Methods
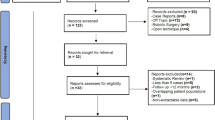
A systematic review of PubMed, MEDLINE, EMBASE, the Cochrane database, SCOPUS, and the PROSPERO registry was performed according to PRISMA 2020 guidelines (PROSPERO ID: CRD42021290483). Studies comparing parastomal hernia recurrences after Sugarbaker and keyhole repairs were included. Studies with overlapping patient cohorts (duplicate data), non-comparative studies, studies that did not report the primary outcome of interest, and studies not in the English language were excluded. Study bias was assessed using the Newcastle–Ottawa scale. Pooled mean differences (MD), odds ratios (OR), and risk ratios (RR) with 95% confidence intervals (CI) were calculated. Heterogeneity was assessed using the I2 statistic. Forest plots and funnel plots were generated. Study quality was analyzed using MINORS. Additional subgroup analysis of modern studies was performed.
Results
Ten comparative studies published between 2005 and 2021 from 5 countries were included for analysis comprising 347 Sugarbaker repairs and 246 keyhole repairs. There were no differences in patient age, sex, or BMI between the groups. There was no difference between the groups regarding surgical site infection (OR 0.78; CI 0.31–1.98; P = 0.61) or post-operative bowel obstruction (OR 0.76; CI 0.23–2.56; P = 0.66). Sugarbaker repairs were significantly less often associated with parastomal hernia recurrence when compared to keyhole repairs (OR 0.38; CI 0.18–0.78; P = 0.008). There was no significant heterogeneity among the studies comparing parastomal hernia recurrence (I2 = 32%; P = 0.15). Quality analysis revealed a median MINORS score of 11 (range 6–16). Subgroup analysis of studies performed after the previously published pooled analysis (2015–2021) revealed no significant difference in parastomal hernia recurrence between the two groups (OR 0.58; CI 0.24–1.38; P = 0.22) with a significant subgroup effect (P = 0.05).
Conclusions
Though there were lower rates of parastomal hernia recurrence with Sugarbaker repairs on overall analysis, this phenomenon disappeared on subgroup analysis of modern studies. Randomized controlled trials with contemporary cohorts would help further evaluate these repairs and minimize potential bias.







Similar content being viewed by others
References
Sohn YJ, Moon SM, Shin US et al. Incidence and risk factors of parastomal hernia. J Korean Soc Coloproctol 2012; 28 (5): 241-246.
Carne PW, Robertson GM, Frizelle FA. Parastomal hernia. The British journal of surgery 2003; 90 (7): 784-793.
Arumugam PJ, Bevan L, Macdonald L et al. A prospective audit of stomas--analysis of risk factors and complications and their management. Colorectal Dis 2003; 5 (1): 49-52.
Rubin MS, Schoetz DJ, Jr., Matthews JB. Parastomal hernia. Is stoma relocation superior to fascial repair? Arch Surg 1994; 129 (4): 413–418; discussion 418–419.
Hansson BM, Slater NJ, van der Velden AS et al. Surgical techniques for parastomal hernia repair: a systematic review of the literature. Annals of surgery 2012; 255 (4): 685-695.
Cheung MT, Chia NH, Chiu WY. Surgical treatment of parastomal hernia complicating sigmoid colostomies. Dis Colon Rectum 2001; 44 (2): 266-270.
Stelzner S, Hellmich G, Ludwig K. Repair of paracolostomy hernias with a prosthetic mesh in the intraperitoneal onlay position: modified Sugarbaker technique. Dis Colon Rectum 2004; 47 (2): 185-191.
Hansson BM, Morales-Conde S, Mussack T et al. The laparoscopic modified Sugarbaker technique is safe and has a low recurrence rate: a multicenter cohort study. Surg Endosc 2013; 27 (2): 494-500.
Sugarbaker PH. Peritoneal approach to prosthetic mesh repair of paraostomy hernias. Annals of surgery 1985; 201 (3): 344-346.
Hansson BM, de Hingh IH, Bleichrodt RP. Laparoscopic parastomal hernia repair is feasible and safe: early results of a prospective clinical study including 55 consecutive patients. Surg Endosc 2007; 21 (6): 989-993.
Hansson BM, Bleichrodt RP, de Hingh IH. Laparoscopic parastomal hernia repair using a keyhole technique results in a high recurrence rate. Surg Endosc 2009; 23 (7): 1456-1459.
Safadi B. Laparoscopic repair of parastomal hernias: early results. Surg Endosc 2004; 18 (4): 676-680.
LeBlanc KA, Bellanger DE, Whitaker JM et al. Laparoscopic parastomal hernia repair. Hernia 2005; 9 (2): 140-144.
Berger D, Bientzle M. Laparoscopic repair of parastomal hernias: a single surgeon’s experience in 66 patients. Dis Colon Rectum 2007; 50 (10): 1668-1673.
Mancini GJ, McClusky DA, 3rd, Khaitan L et al. Laparoscopic parastomal hernia repair using a nonslit mesh technique. Surg Endosc 2007; 21 (9): 1487-1491.
McLemore EC, Harold KL, Efron JE et al. Parastomal hernia: short-term outcome after laparoscopic and conventional repairs. Surg Innov 2007; 14 (3): 199-204.
Muysoms F. Laparoscopic repair of parastomal hernias with a modified Sugarbaker technique. Acta Chir Belg 2007; 107 (4): 476-480.
Berger D, Bientzle M. Polyvinylidene fluoride: a suitable mesh material for laparoscopic incisional and parastomal hernia repair! A prospective, observational study with 344 patients. Hernia 2009; 13 (2): 167-172.
Craft RO, Huguet KL, McLemore EC et al. Laparoscopic parastomal hernia repair. Hernia 2008; 12 (2): 137-140.
Pastor DM, Pauli EM, Koltun WA et al. Parastomal hernia repair: a single center experience. Jsls 2009; 13 (2): 170-175.
Jani K. Laparoscopic paracolostomy hernia repair: a retrospective case series at a tertiary care center. Surg Laparosc Endosc Percutan Tech 2010; 20 (6): 395-398.
Wara P, Andersen LM. Long-term follow-up of laparoscopic repair of parastomal hernia using a bilayer mesh with a slit. Surg Endosc 2011; 25 (2): 526-530.
Asif A, Ruiz M, Yetasook A et al. Laparoscopic modified Sugarbaker technique results in superior recurrence rate. Surg Endosc 2012; 26 (12): 3430-3434.
Mizrahi H, Bhattacharya P, Parker MC. Laparoscopic slit mesh repair of parastomal hernia using a designated mesh: long-term results. Surg Endosc 2012; 26 (1): 267-270.
DeAsis FJ, Lapin B, Gitelis ME et al. Current state of laparoscopic parastomal hernia repair: A meta-analysis. World journal of gastroenterology 2015; 21 (28): 8670-8677.
Gameza VA, Bell Lybecker M, Wara P. Laparoscopic Keyhole Versus Sugarbaker Repair in Parastomal Hernia: A Long-Term Case-Controlled Prospective Study of Consecutive Patients. J Laparoendosc Adv Surg Tech A 2020; 30 (7): 783-789.
Mäkäräinen-Uhlbäck E, Vironen J, Falenius V et al. Parastomal Hernia: A Retrospective Nationwide Cohort Study Comparing Different Techniques with Long-Term Follow-Up. World journal of surgery 2021; 45 (6): 1742-1749.
Oma E, Pilsgaard B, Jorgensen LN. Clinical outcomes after parastomal hernia repair with a polyester monofilament composite mesh: a cohort study of 79 consecutive patients. Hernia 2018; 22 (2): 371-377.
McKibbon KA, Walker-Dilks C, Haynes RB et al. Beyond ACP Journal Club: how to harness MEDLINE for prognosis problems. ACP J Club 1995; 123 (1): A12-14.
Slim K, Nini E, Forestier D et al. Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg 2003; 73 (9): 712-716.
Wells G SB, O’Connell D, Peterson J, Welch V, Losos M, Tugwell P. The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. 2021. 2013.
Guyatt GH, Oxman AD, Vist GE et al. GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. BMJ (Clinical research ed) 2008; 336 (7650): 924-926.
Hozo SP, Djulbegovic B, Hozo I. Estimating the mean and variance from the median, range, and the size of a sample. BMC medical research methodology 2005; 5: 13.
Higgins JPT TJ, Chandler J, Cumpston M, Li T, Page MJ, Welch VA Cochrane Handbook for Systematic Reviews of Interventions version 6.2 (updated February 2021). Cochrane, 2021.
Mantel N, Haenszel W. Statistical aspects of the analysis of data from retrospective studies of disease. Journal of the National Cancer Institute 1959; 22 (4): 719-748.
West SL, Gartlehner G, Mansfield AJ et al. AHRQ Methods for Effective Health Care. Comparative Effectiveness Review Methods: Clinical Heterogeneity, Rockville (MD): Agency for Healthcare Research and Quality (US) 2010.
Higgins JP, Thompson SG, Deeks JJ et al. Measuring inconsistency in meta-analyses. BMJ (Clinical research ed) 2003; 327 (7414): 557-560.
Köhler G, Mayer F, Wundsam H et al. Changes in the Surgical Management of Parastomal Hernias Over 15 Years: Results of 135 Cases. World journal of surgery 2015; 39 (11): 2795-2804.
Egger M, Davey Smith G, Schneider M et al. Bias in meta-analysis detected by a simple, graphical test. BMJ (Clinical research ed) 1997; 315 (7109): 629-634.
Sterne JAC, Harbord RM. Funnel Plots in Meta-analysis. The Stata Journal 2004; 4 (2): 127-141.
Helgstrand F, Rosenberg J, Kehlet H et al. Risk of morbidity, mortality, and recurrence after parastomal hernia repair: a nationwide study. Dis Colon Rectum 2013; 56 (11): 1265-1272.
DeAsis FJ, Linn JG, Lapin B et al. Modified laparoscopic Sugarbaker repair decreases recurrence rates of parastomal hernia. Surgery 2015; 158 (4): 954–959; discussion 959–961.
Hansson BM, van Nieuwenhoven EJ, Bleichrodt RP. Promising new technique in the repair of parastomal hernia. Surg Endosc 2003; 17 (11): 1789-1791.
Halm JA, de Wall LL, Steyerberg EW et al. Intraperitoneal polypropylene mesh hernia repair complicates subsequent abdominal surgery. World journal of surgery 2007; 31 (2): 423–429; discussion 430.
Keller P, Totten CF, Plymale MA et al. Laparoscopic parastomal hernia repair delays recurrence relative to open repair. Surg Endosc 2021; 35 (1): 415-422.
Soliani G, De Troia A, Portinari M et al. Laparoscopic versus open incisional hernia repair: a retrospective cohort study with costs analysis on 269 patients. Hernia 2017; 21 (4): 609-618.
Richardson M GP, Donegan S. Interpretation of subgroup analyses in systematic reviews: A tutorial. Clinical Epidemiology and Global Health 2019; 7 (2): 192-198.
Acknowledgements
Paul Gahn, UTHSC Interlibrary Loan Staff
Carolyn Polk, UTHSC Interlibrary Loan Staff
Wanda Booker-Wade, UTHSC Interlibrary Loan Staff
Author information
Authors and Affiliations
Contributions
The authors included each contributed substantially to this research as per the guidelines of the International Committee of Medical Journal Editors (ICMJE).
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fleming, A.M., Phillips, A.L., Drake, J.A. et al. Sugarbaker Versus Keyhole Repair for Parastomal Hernia: a Systematic Review and Meta-analysis of Comparative Studies. J Gastrointest Surg 27, 573–584 (2023). https://doi.org/10.1007/s11605-022-05412-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-022-05412-y