Abstract
Background
Surgical resection for patients with hepatic and extrahepatic colorectal metastases remains controversial. This study aimed to determine the efficacy of curative resection of distant extrahepatic metastatic lesions in patients with colorectal liver metastases (CRLM).
Methods
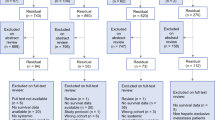
From 2007 to 2019, 377 patients with CRLM were treated; of these, 323 patients underwent hepatectomy, and 54 patients with extrahepatic metastases (EHM) had received only chemotherapy. Survival and recurrence were compared between patients with and without EHM. Variables potentially associated with survival were analyzed in univariate and multivariate analyses.
Results
Among patients who underwent hepatectomy, the median, 3-, and 5-year overall survival rates for patients with EHM (n = 60) were 32 months, 47%, and 28%, respectively, while those for patients without EHM (n = 263) were 115 months, 79%, and 66%, respectively (p < 0.001). Furthermore, outcomes were similar in R2 patients with EHM and those with unresectable tumors. However, outcomes were significantly better in the R0/1 group than in the R2 and unresectable groups (p < 0.001). Among patients with EHM, multivariate analysis revealed that higher clinical risk score, incomplete resection of all EHM, extrahepatic disease detected intraoperatively, and previous treatment with neoadjuvant chemotherapy were independently associated with worse survival.
Conclusions
In patients with CRLM with EHM (liver + one organ), gross curative resection is necessary when surgical treatment is contemplated, and resection of liver metastases should be performed in patients with CRLM with smaller and fewer tumors (e.g., H1).



Similar content being viewed by others
References
Dekker E, Tanis PJ, Vleugels JLA et al. Colorectal cancer. Lancet 2019; 394: 1467–1480.
Abdalla EK, Vauthey JN, Ellis LM et al. Recurrence and outcomes following hepatic resection, radiofrequency ablation, and combined resection/ablation for colorectal liver metastases. Ann Surg 2004; 239: 818–825; discussion 825–817.
Martin LW, Warren RS. Current management of colorectal liver metastases. Surg Oncol Clin N Am 2000; 9: 853–876; discussion 877–858.
Nordlinger B, Sorbye H, Glimelius B et al. Perioperative FOLFOX4 chemotherapy and surgery versus surgery alone for resectable liver metastases from colorectal cancer (EORTC 40983): long-term results of a randomised, controlled, phase 3 trial. Lancet Oncol 2013; 14: 1208–1215.
Penna C, Nordlinger B. Colorectal metastasis (liver and lung). Surg Clin North Am 2002; 82: 1075–1090, x-xi.
Adam R. Developing strategies for liver metastases from colorectal cancer. Semin Oncol 2007; 34: S7–11.
Lam VW, Spiro C, Laurence JM et al. A systematic review of clinical response and survival outcomes of downsizing systemic chemotherapy and rescue liver surgery in patients with initially unresectable colorectal liver metastases. Ann Surg Oncol 2012; 19: 1292–1301.
Chua TC, Saxena A, Liauw W et al. Hepatectomy and resection of concomitant extrahepatic disease for colorectal liver metastases--a systematic review. Eur J Cancer 2012; 48: 1757–1765.
Carpizo DR, Are C, Jarnagin W et al. Liver resection for metastatic colorectal cancer in patients with concurrent extrahepatic disease: results in 127 patients treated at a single center. Ann Surg Oncol 2009; 16: 2138–2146.
Kobayashi H, Kotake K, Sugihara K. Outcomes of surgery without HIPEC for synchronous peritoneal metastasis from colorectal cancer: data from a multi-center registry. Int J Clin Oncol 2014; 19: 98–105.
Shida D, Tsukamoto S, Ochiai H, Kanemitsu Y. Long-Term Outcomes After R0 Resection of Synchronous Peritoneal Metastasis from Colorectal Cancer Without Cytoreductive Surgery or Hyperthermic Intraperitoneal Chemotherapy. Ann Surg Oncol 2018; 25: 173–178.
Yamazaki K, Nagase M, Tamagawa H et al. Randomized phase III study of bevacizumab plus FOLFIRI and bevacizumab plus mFOLFOX6 as first-line treatment for patients with metastatic colorectal cancer (WJOG4407G). Ann Oncol 2016; 27: 1539–1546.
Yamada Y, Takahari D, Matsumoto H et al. Leucovorin, fluorouracil, and oxaliplatin plus bevacizumab versus S-1 and oxaliplatin plus bevacizumab in patients with metastatic colorectal cancer (SOFT): an open-label, non-inferiority, randomised phase 3 trial. Lancet Oncol 2013; 14: 1278–1286.
Loupakis F, Cremolini C, Masi G et al. Initial therapy with FOLFOXIRI and bevacizumab for metastatic colorectal cancer. N Engl J Med 2014; 371: 1609–1618.
Andres A, Mentha G, Adam R et al. Surgical management of patients with colorectal cancer and simultaneous liver and lung metastases. Br J Surg 2015; 102: 691–699.
Hadden WJ, de Reuver PR, Brown K et al. Resection of colorectal liver metastases and extra-hepatic disease: a systematic review and proportional meta-analysis of survival outcomes. HPB (Oxford) 2016; 18: 209–220.
Pulitano C, Bodingbauer M, Aldrighetti L et al. Liver resection for colorectal metastases in presence of extrahepatic disease: results from an international multi-institutional analysis. Ann Surg Oncol 2011; 18: 1380–1388.
Hirokawa F, Hayashi M, Miyamoto Y et al. A novel method using the VIO soft-coagulation system for liver resection. Surgery 2011; 149: 438–444.
Japanese Society for Cancer of the Colon and Rectum. Japanese Classification of Colorectal, Appendiceal, and Anal Carcinoma: the 3d English Edition [Secondary Publication]. J Anus Rectum Colon 2019; 3: 175–195.
Watanabe K, Nagai K, Kobayashi A et al. Factors influencing survival after complete resection of pulmonary metastases from colorectal cancer. Br J Surg 2009; 96: 1058–1065.
Kanemitsu Y, Kato T, Hirai T, Yasui K. Preoperative probability model for predicting overall survival after resection of pulmonary metastases from colorectal cancer. Br J Surg 2004; 91: 112–120.
Iida T, Nomori H, Shiba M et al. Prognostic factors after pulmonary metastasectomy for colorectal cancer and rationale for determining surgical indications: a retrospective analysis. Ann Surg 2013; 257: 1059–1064.
Huang CQ, Yang XJ, Yu Y et al. Cytoreductive surgery plus hyperthermic intraperitoneal chemotherapy improves survival for patients with peritoneal carcinomatosis from colorectal cancer: a phase II study from a Chinese center. PLoS One 2014; 9: e108509.
Goere D, Malka D, Tzanis D et al. Is there a possibility of a cure in patients with colorectal peritoneal carcinomatosis amenable to complete cytoreductive surgery and intraperitoneal chemotherapy? Ann Surg 2013; 257: 1065–1071.
Nakai N, Yamaguchi T, Kinugasa Y et al. Long-term outcomes after resection of para-aortic lymph node metastasis from left-sided colon and rectal cancer. Int J Colorectal Dis 2017; 32: 999–1007.
Min BS, Kim JS, Kim NK et al. Extended lymph node dissection for rectal cancer with radiologically diagnosed extramesenteric lymph node metastasis. Ann Surg Oncol 2009; 16: 3271–3278.
Choi PW, Kim HC, Kim AY et al. Extensive lymphadenectomy in colorectal cancer with isolated para-aortic lymph node metastasis below the level of renal vessels. J Surg Oncol 2010; 101: 66–71.
Elias D, Sideris L, Pocard M et al. Results of R0 resection for colorectal liver metastases associated with extrahepatic disease. Ann Surg Oncol 2004; 11: 274–280.
Elias D, Ouellet JF, Bellon N et al. Extrahepatic disease does not contraindicate hepatectomy for colorectal liver metastases. Br J Surg 2003; 90: 567–574.
Adam R, de Haas RJ, Wicherts DA et al. Concomitant extrahepatic disease in patients with colorectal liver metastases: when is there a place for surgery? Ann Surg 2011; 253: 349–359.
Hasselgren K, Isaksson B, Ardnor B et al. Liver resection is beneficial for patients with colorectal liver metastases and extrahepatic disease. Ann Transl Med 2020; 8: 109.
Leung U, Gonen M, Allen PJ et al. Colorectal Cancer Liver Metastases and Concurrent Extrahepatic Disease Treated With Resection. Ann Surg 2017; 265: 158–165.
Nagakura S, Shirai Y, Yamato Y et al. Simultaneous detection of colorectal carcinoma liver and lung metastases does not warrant resection. J Am Coll Surg 2001; 193: 153–160.
Siebenhuner AR, Guller U, Warschkow R. Population-based SEER analysis of survival in colorectal cancer patients with or without resection of lung and liver metastases. BMC Cancer 2020; 20: 246.
Beckurts KT, Holscher AH, Thorban S et al. Significance of lymph node involvement at the hepatic hilum in the resection of colorectal liver metastases. Br J Surg 1997; 84: 1081–1084.
Nakamura S, Suzuki S, Konno H. Resection of hepatic metastases of colorectal carcinoma: 20 years' experience. J Hepatobiliary Pancreat Surg 1999; 6: 16–22.
Rodgers MS, McCall JL. Surgery for colorectal liver metastases with hepatic lymph node involvement: a systematic review. Br J Surg 2000; 87: 1142–1155.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
We declare no commercial interests related to this study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hirokawa, F., Komeda, K., Asakuma, M. et al. Is Surgical Treatment Effective or Contraindicated in Patients with Colorectal Cancer Liver Metastases Exhibiting Extrahepatic Metastasis?. J Gastrointest Surg 26, 594–601 (2022). https://doi.org/10.1007/s11605-021-05122-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-021-05122-x