Abstract
Introduction
Robotic pancreaticoduodenectomy is slowly gaining acceptance within pancreatic surgery. Advantages have been demonstrated for robotic surgery in other fields, but robust data for pancreaticoduodenectomy is limited. The aim of this study was to compare the short-term outcomes of robotic pancreaticoduodenectomy (RPD) to open pancreaticoduodenectomy (OPD) and laparoscopic pancreaticoduodenectomy (LPD).
Methods
Patients who underwent a pancreaticoduodenectomy between January 2011 and July 2019 at the Johns Hopkins Hospital were included in this retrospective propensity-matched analysis. The RPD cohort was matched to patients who underwent OPD in a 1:2 fashion and LPD in a 1:1 fashion. Short-term outcomes were analyzed for all three cohorts.
Results
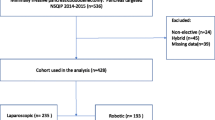
In total, 1644 patients were included, of which 96 (5.8%) underwent RPD, 131 (8.0%) LPD, and 1417 (86.2%) OPD. RPD was associated with a decreased incidence of delayed gastric emptying (9.4%) compared to OPD (23.5%; P = 0.006). The median estimated blood loss was significantly less in the RPD cohort (RPD vs OPD, 150 vs 487 mL; P < 0.001, RPD vs LPD, 125 vs 300 mL; P < 0.001). Compared to OPD, the robotic approach was associated with a shorter median length of stay (median 8 vs 9 days; P = 0.014) and a decrease in wound complications (4.2% vs 16.7%; P = 0.002). The incidence of other postoperative complications was comparable between RPD and OPD, and RPD and LPD.
Conclusion
In the hands of experienced surgeons, RPD may have a modest yet statistically significant reduction in estimated blood loss, postoperative length of stay, wound complications, and delayed gastric emptying comparing to OPD in similar patients.
Similar content being viewed by others
References
Gouma DJ, Van Geenen RCI, Van Gulik TM, De Haan RJ, De Wit LT, Busch ORC, Obertop H (2000) Rates of complications and death after pancreaticoduodenectomy: Risk factors and the impact of hospital volume. Ann Surg 232:786–795 . https://doi.org/10.1097/00000658-200012000-00007
Cameron JL, He J (2015) Two thousand consecutive pancreaticoduodenectomies. In: Journal of the American College of Surgeons. Elsevier Inc., pp 530–536
van Hilst J, de Rooij T, Klompmaker S, Rawashdeh M, Aleotti F, Al-Sarireh B, Alseidi A, Ateeb Z, Balzano G, Berrevoet F, Björnsson B, Boggi U, Busch OR, Butturini G, Casadei R, Del Chiaro M, Chikhladze S, Cipriani F, van Dam R, Damoli I, van Dieren S, Dokmak S, Edwin B, van Eijck C, Fabre J-M, Falconi M, Farges O, Fernández-Cruz L, Forgione A, Frigerio I, Fuks D, Gavazzi F, Gayet B, Giardino A, Groot Koerkamp B, Hackert T, Hassenpflug M, Kabir I, Keck T, Khatkov I, Kusar M, Lombardo C, Marchegiani G, Marshall R, Menon K V., Montorsi M, Orville M, de Pastena M, Pietrabissa A, Poves I, Primrose J, Pugliese R, Ricci C, Roberts K, Røsok B, Sahakyan MA, Sánchez-Cabús S, Sandström P, Scovel L, Solaini L, Soonawalla Z, Souche FR, Sutcliffe RP, Tiberio GA, Tomazic A, Troisi R, Wellner U, White S, Wittel UA, Zerbi A, Bassi C, Besselink MG, Abu Hilal M (2019) Minimally Invasive versus Open Distal Pancreatectomy for Ductal Adenocarcinoma (DIPLOMA). Ann Surg 269:10–17 . https://doi.org/10.1097/SLA.0000000000002561
Luketich JD, Pennathur A, Awais O, Levy RM, Keeley S, Shende M, Christie NA, Weksler B, Landreneau RJ, Abbas G, Schuchert MJ, Nason KS (2012) Outcomes after minimally invasive esophagectomy: Review of over 1000 patients. Ann Surg 256:95–103 . https://doi.org/10.1097/SLA.0b013e3182590603
Gagner M, Pomp A (1994) Laparoscopic pylorus-preserving pancreatoduodenectomy. Surg Endosc 8:408–410 . https://doi.org/10.1007/BF00642443
van Hilst J, De Rooij T, Bosscha K, Brinkman DJ, Van Dieren S, Dijkgraaf MG, Gerhards MF, De Hingh IH, Karsten TM, Lips DJ, Luyer MD, Busch OR, Festen S, Besselink MG, Marsman HA, Van Gulik TM, Wicherts DA, Eshuis WJ, Stibbe LA, Nieveen van Dijkum EJ, Van Hooft JE, Fockens P, Van Laarhoven HW, Wilmink JW, Van de Vijver MJ, Bijlsma MF, Verheij J, Nio CY, Van Lienden KP, Van Tienhoven G, Schoorlemmer A, Creemers GJ, Van Eijck CH, Groot Koerkamp B, Bruno MJ, Eskens F, Nuyttens JJ, Pek C, Van der Schelling GP, Seerden TC, Patijn GA, Nieuwenhuijs VB, De Groot JW, Bonsing BA, Vahrmeijer A, Swijnenburg RJ, Mieog JSD, Van der Harst E, Den Dulk M, Olde Damink S, Dejong CH, Van Dam R, De Vos JM, Liem MS, Van Laarhoven CJ, Van Goor H, Van den Boezem PB, Van der Kolk BM, Stommel MW, Hermans JJ, Van Geenen EJ, Radema SA, Brosens LA, Scheepers JJ, Roos D, Boerma D, Te Riele W, Van Santvoort HC, Bollen TL, Wit F, Molenaar IQ, Haj Mohammad N, Van Leeuwen MS, Roele A, De Jong KP, De Meijer VE, Klaase JM, Kazemier G, Zonderhuis B, Daams F, Meijerink MR, Latenstein A, Van Rijssen LB, Nota C, Van Halsema E, Van Veldhuisen E, Vogel J, Janssen K, Scholten L, Daamen L, Walma M, Strijker M, Prins M, Zwart M, Suker M, Rombouts S, Mungroop T, Vissers F, Korrel M (2019) Laparoscopic versus open pancreatoduodenectomy for pancreatic or periampullary tumours (LEOPARD-2): a multicentre, patient-blinded, randomised controlled phase 2/3 trial. Lancet Gastroenterol Hepatol 4:199–207 . https://doi.org/10.1016/S2468-1253(19)30004-4
Wright JD, Ananth C V., Lewin SN, Burke WM, Lu YS, Neugut AI, Herzog TJ, Hershman DL (2013) Robotically assisted vs laparoscopic hysterectomy among women with benign gynecologic disease. JAMA - J Am Med Assoc 309:689–698 . https://doi.org/10.1001/jama.2013.186
Huang X, Wang L, Zheng X, Wang X (2017) Comparison of perioperative, functional, and oncologic outcomes between standard laparoscopic and robotic-assisted radical prostatectomy: a systemic review and meta-analysis. Surg Endosc 31:1045–1060 . https://doi.org/10.1007/s00464-016-5125-1
Siddaiah-Subramanya M, Tiang K, Nyandowe M (2017) A New Era of Minimally Invasive Surgery: Progress and Development of Major Technical Innovations in General Surgery Over the Last Decade. Surg J 03:e163–e166 . https://doi.org/10.1055/s-0037-1608651
De Rooij T, Lu MZ, Steen MW, Gerhards MF, Dijkgraaf MG, Busch OR, Lips DJ, Festen S, Besselink MG (2016) Minimally Invasive Versus Open Pancreatoduodenectomy: Systematic Review and Meta-analysis of Comparative Cohort and Registry Studies. Ann Surg 264:257–267 . https://doi.org/10.1097/SLA.0000000000001660
Abdelgadir Adam M, Choudhury K, Dinan MA, Reed SD, Scheri RP, Blazer DG, Roman SA, Sosa JA (2015) Minimally invasive versus open pancreaticoduodenectomy for cancer: Practice patterns and short-term outcomes among 7061 patients. Ann Surg 262:372–377 . https://doi.org/10.1097/SLA.0000000000001055
Giulianotti PC, Coratti A, Angelini M, Sbrana F, Cecconi S, Balestracci T, Caravaglios G (2003) Robotics in general surgery: Personal experience in a large community hospital. Arch Surg 138:777–784 . https://doi.org/10.1001/archsurg.138.7.777
Shi Y, Jin J, Qiu W, Weng Y, Wang J, Zhao S, Huo Z, Qin K, Wang Y, Chen H, Deng X, Peng C, Shen B (2020) Short-term Outcomes after Robot-Assisted vs Open Pancreaticoduodenectomy after the Learning Curve. JAMA Surg. https://doi.org/10.1001/jamasurg.2020.0021
Torphy RJ, Friedman C, Halpern A, Chapman BC, Ahrendt SS, McCarter MM, Edil BH, Schulick RD, Gleisner A (2019) Comparing Short-term and Oncologic Outcomes of Minimally Invasive Versus Open Pancreaticoduodenectomy Across Low and High Volume Centers. Ann Surg 270:1147–1155 . https://doi.org/10.1097/SLA.0000000000002810
Pernar LIM, Robertson FC, Tavakkoli • Ali, Sheu EG, David •, Brooks C, Douglas •, Smink S An appraisal of the learning curve in robotic general surgery. https://doi.org/10.1007/s00464-017-5520-2
Zhang T, Zhao ZM, Gao YX, Lau WY, Liu R (2019) The learning curve for a surgeon in robot-assisted laparoscopic pancreaticoduodenectomy: a retrospective study in a high-volume pancreatic center. Surg Endosc 33:2927–2933 . https://doi.org/10.1007/s00464-018-6595-0
Boone BA, Zenati M, Hogg ME, Steve J, Moser AJ, Bartlett DL, Zeh HJ, Zureikat AH (2015) Assessment of quality outcomes for robotic pancreaticoduodenectomy: Identification of the learning curve. JAMA Surg 150:416–422 . https://doi.org/10.1001/jamasurg.2015.17
Vining CC, Hogg ME (2020) How to train and evaluate minimally invasive pancreas surgery. J Surg Oncol 122:41–48 . https://doi.org/10.1002/jso.25912
Galvez D, Sorber R, Javed AA, He J (2017) Technical considerations for the fully robotic pancreaticoduodenectomy. J Vis Surg 3:81–81 . https://doi.org/10.21037/jovs.2017.05.08
Magge D, Zureikat A, Hogg M, Zeh HJ (2016) Minimally Invasive Approaches to Pancreatic Surgery. Surg. Oncol. Clin. N. Am. 25:273–286
Edil BH, Cooper MA, Makary MA (2014) Laparoscopic Pancreaticojejunostomy Using a Barbed Suture: A Novel Technique. J Laparoendosc Adv Surg Tech 24:887–891 . https://doi.org/10.1089/lap.2014.0053
Isaji S, Mizuno S, Windsor JA, Bassi C, Fernández-del Castillo C, Hackert T, Hayasaki A, Katz MHG, Kim SW, Kishiwada M, Kitagawa H, Michalski CW, Wolfgang CL (2018) International consensus on definition and criteria of borderline resectable pancreatic ductal adenocarcinoma 2017. Pancreatology 18:2–11 . https://doi.org/10.1016/j.pan.2017.11.011
Baker EH, Ross SW, Seshadri R, Swan RZ, Iannitti DA, Vrochides D, Martinie JB (2015) Robotic pancreaticoduodenectomy for pancreatic adenocarcinoma: Role in 2014 and beyond. J. Gastrointest. Oncol. 6:396–405
Rashid OM, Mullinax JE, Pimiento JM, Meredith KL, Malafa MP (2015) Robotic Whipple Procedure for Pancreatic Cancer: The Moffitt Cancer Center Pathway. Cancer Control 22:340–51 . https://doi.org/10.1177/107327481502200313
Wente MN, Bassi C, Dervenis C, Fingerhut A, Gouma DJ, Izbicki JR, Neoptolemos JP, Padbury RT, Sarr MG, Traverso LW, Yeo CJ, Büchler MW (2007) Delayed gastric emptying (DGE) after pancreatic surgery: A suggested definition by the International Study Group of Pancreatic Surgery (ISGPS). Surgery 142:761–768 . https://doi.org/10.1016/j.surg.2007.05.005
Bassi C, Marchegiani G, Dervenis C, Sarr M, Abu Hilal M, Adham M, Allen P, Andersson R, Asbun HJ, Besselink MG, Conlon K, Del Chiaro M, Falconi M, Fernandez-Cruz L, Fernandez-del Castillo C, Fingerhut A, Friess H, Gouma DJ, Hackert T, Izbicki J, Lillemoe KD, Neoptolemos JP, Olah A, Schulick R, Shrikhande S V., Takada T, Takaori K, Traverso W, Vollmer CR, Wolfgang CL, Yeo CJ, Salvia R, Buchler M (2017) The 2016 update of the International Study Group (ISGPS) definition and grading of postoperative pancreatic fistula: 11 Years After. Surg. (United States) 161:584–591
Imai K (2018) Package “MatchIt” Title Nonparametric Preprocessing for Parametric Causal Inference. https://doi.org/10.1093/pan/mpl013
Braga M, Capretti G, Pecorelli N, Balzano G, Doglioni C, Ariotti R, Di Carlo V (2011) A Prognostic Score to Predict Major Complications After Pancreaticoduodenectomy. Ann Surg 254:702–708 . https://doi.org/10.1097/SLA.0b013e31823598fb
Hackett NJ, De Oliveira GS, Jain UK, Kim JYS (2015) ASA class is a reliable independent predictor of medical complications and mortality following surgery. Int J Surg 18:184–190 . https://doi.org/10.1016/j.ijsu.2015.04.079
House MG, Fong Y, Arnaoutakis DJ, Sharma R, Winston CB, Protic M, Gonen M, Olson SH, Kurtz RC, Brennan MF, Allen PJ (2008) Preoperative predictors for complications after pancreaticoduodenectomy: Impact of BMI and body fat distribution. J Gastrointest Surg 12:270–278 . https://doi.org/10.1007/s11605-007-0421-7
Rosso E, Casnedi S, Pessaux P, Oussoultzoglou E, Panaro F, Mahfud M, Jaeck D, Bachellier P (2009) The role of “Fatty Pancreas” and of BMI in the occurrence of pancreatic fistula after pancreaticoduodenectomy. J Gastrointest Surg 13:1845–1851 . https://doi.org/10.1007/s11605-009-0974-8
Hashimoto Y, Traverso LW (2010) Incidence of pancreatic anastomotic failure and delayed gastric emptying after pancreatoduodenectomy in 507 consecutive patients: Use of a web-based calculator to improve homogeneity of definition. Surgery 147:503–515 . https://doi.org/10.1016/j.surg.2009.10.034
Zureikat AH, Moser AJ, Boone BA, Bartlett DL, Zenati M, Zeh HJ (2013) 250 robotic pancreatic resections safety and feasibility. In: Annals of Surgery. Ann Surg, pp 554–559
Boggi U, Signori S, De Lio N, Perrone VG, Vistoli F, Belluomini M, Cappelli C, Amorese G, Mosca F (2013) Feasibility of robotic pancreaticoduodenectomy. Br J Surg 100:917–925 . https://doi.org/10.1002/bjs.9135
Asbun HJ, Stauffer JA (2012) Laparoscopic vs open pancreaticoduodenectomy: Overall outcomes and severity of complications using the accordion severity grading system. J Am Coll Surg 215:810–819 . https://doi.org/10.1016/j.jamcollsurg.2012.08.006
He S, Ding D, Wright MJ, Groshek L, Javed AA, Ka-Wan Chu K, Burkhart RA, Cameron JL, Weiss MJ, Wolfgang CL, He J (2020) The impact of high body mass index on patients undergoing robotic pancreatectomy: A propensity matched analysis. Surg (United States) 167:556–559 . https://doi.org/10.1016/j.surg.2019.11.002
Zureikat AH, Postlewait LM, Liu Y, Gillespie TW, Weber SM, Abbott DE, Ahmad SA, Maithel SK, Hogg ME, Zenati M, Cho CS, Salem A, Xia B, Steve J, Nguyen TK, Keshava HB, Chalikonda S, Walsh RM, Talamonti MS, Stocker SJ, Bentrem DJ, Lumpkin S, Kim HJ, Zeh HJ, Kooby DA (2016) A multi-institutional comparison of perioperative outcomes of robotic and open pancreaticoduodenectomy. In: Annals of Surgery. Lippincott Williams and Wilkins, pp 640–649
Croome KP, Farnell MB, Que FG, Reid-Lombardo Km, Truty MJ, Nagorney DM, Kendrick ML (2014) Total Laparoscopic Pancreaticoduodenectomy for Pancreatic Ductal Adenocarcinoma. Ann Surg 260:633–640 . https://doi.org/10.1097/SLA.0000000000000937
Nakamura T, Ambo Y, Noji T, Okada N, Takada M, Shimizu T, Suzuki O, Nakamura F, Kashimura N, Kishida A, Hirano S (2015) Reduction of the Incidence of Delayed Gastric Emptying in Side-to-Side Gastrojejunostomy in Subtotal Stomach-Preserving Pancreaticoduodenectomy. J Gastrointest Surg 19:1425–1432 . https://doi.org/10.1007/s11605-015-2870-8
Tsutaho A, Nakamura T, Asano T, Okamura K, Tsuchikawa T, Noji T, Nakanishi Y, Tanaka K, Murakami S, Kurashima Y, Ebihara Y, Shichinohe T, Ito YM, Hirano S (2017) Delayed Gastric Emptying in Side-to-Side Gastrojejunostomy in Pancreaticoduodenectomy: Result of a Propensity Score Matching. J Gastrointest Surg 21:1635–1642 . https://doi.org/10.1007/s11605-017-3540-9
Stauffer JA, Coppola A, Villacreses D, Mody • Kabir, Johnson E, Li Z, Asbun HJ Laparoscopic versus open pancreaticoduodenectomy for pancreatic adenocarcinoma: long-term results at a single institution. https://doi.org/10.1007/s00464-016-5222-1
Author information
Authors and Affiliations
Contributions
AF van Oosten; D Ding; J He: project development, data analysis and collection, manuscript writing
J Habib; A Irfan; R Schmocker; E Sereni; B Kinny-Köster; M Wright; V Groot; I. Molenaar: data collection, manuscript editing
J Cameron; M Makary; R Burkhart; W Burns; C Wolfgang: data collection, manuscript editing
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
van Oosten, A.F., Ding, D., Habib, J.R. et al. Perioperative Outcomes of Robotic Pancreaticoduodenectomy: a Propensity-Matched Analysis to Open and Laparoscopic Pancreaticoduodenectomy. J Gastrointest Surg 25, 1795–1804 (2021). https://doi.org/10.1007/s11605-020-04869-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-020-04869-z