Abstract
Introduction
An increased transdiaphragmatic pressure gradient (TGP) is a main element for distal gastroesophageal reflux disease (GERD). The role of TGP for proximal reflux is still unclear. This study aims to evaluate the presence, severity, and importance of proximal reflux in relationship to the TGP, comparing healthy volunteers, obese individuals, and patients with chronic obstructive pulmonary disease (COPD).
Methods
We studied 114 individuals comprising 19 healthy lean volunteers, 47 obese individuals (mean body mass index 45 ± 7 kg/m2), and 48 patients with COPD. All patients underwent high-resolution manometry and dual-channel esophageal pH monitoring. Esophageal motility, thoracic pressure (TP), abdominal pressure (AP), TGP, DeMeester score, and % of proximal acid exposure time (pAET) were recorded.
Results
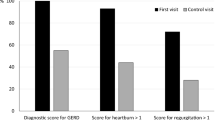
Pathologic distal GERD was found in 0, 44, and 57% of the volunteers, obese, and COPD groups, respectively. pAET was similar among groups, only higher for obese individuals GERD + as compared to obese individuals GERD − and COPD GERD −. pAET did not correlate with any parameter in healthy individuals, but it correlated with AP in the obese, TP in the COPD individuals, and TGP and DeMeester score in both groups. When all individuals were analyzed as a total, pAET correlated with AP, TGP, and DeMeester score. DeMeester score was the only independent variable that correlated with pAET.
Conclusions
Our results show that (a) TGP is an important mechanism associated with distal esophageal acid exposure and this fact is linked with proximal acid exposure and (b) obesity and COPD both seem to be primary causes for GERD but not directly for proximal reflux.

Similar content being viewed by others
References
Del Grande LM, Herbella FAM, Katayama RC, Schlottmann F, Patti MG. The role of the transdiaphragmatic pressure gradient in the pathophysiology of gastroesophageal reflux disease. Arq Gastroenterol. 2018 Nov;55suppl 1(Suppl 1):13-17. Epub 2018 Aug 6. Review.
Nadaleto BF, Herbella FA, Patti MG. Gastroesophageal reflux disease in the obese: Pathophysiology and treatment. Surgery. 2016 Feb; 159(2):475-86. https://doi.org/10.1016/j.surg.2015.04.034.
Del Grande L, Herbella FAM, Katayama RC, Lima WG, Patti MG. Transdiaphragmatic Pressure Gradient (TGP) Has a Central Role in the Pathophysiology of Gastroesophageal Reflux Disease (GERD) in the Obese and it Correlates with Abdominal Circumference but Not with Body Mass Index (BMI). Obes Surg 2020 Apr; 30(4):1424-1428.
Pandolfino JE, El-Serag HB, Zhang Q, et al. Obesity: a challenge to esophagogastric junction integrity. Gastroenterology 2006; 130:639-649.5.
Casanova C, Baudet JS, del Valle Velasco M, Martin JM, Aguirre-Jaime A, de Torres JP, Celli BR. Increased gastro-oesophageal reflux disease in patients with severe COPD. Eur Respir J. 2004 Jun; 23(6):841-5.
Del Grande LM, Herbella FA, Bigatao AM, Abrao H, Jardim JR, Patti MG. Pathophysiology of gastroesophageal reflux in patients with chronic pulmonary obstructive disease is linked to an increased transdiafragmatic pressure gradient and not to a defective esophagogstric barrier. J Gastrointest Surg. 2016 Jan 20(1):104-10.
Neto SC, Herbella FA, Silva LC, Patti MG. Ratio between proximal/distal gastroesophageal reflux does not discriminate abnormal proximal reflux. World J Surg. 2014 Apr; 38(4):890-6.
Vaezi MF, Katzka D, Zerbib F. Extraesophageal Symptoms and Diseases Attributed to GERD: Where is the Pendulum Swinging Now? Clin Gastroenterol Hepatol. 2018 Jul; 16(7):1018-1029. https://doi.org/10.1016/j.cgh.2018.02.001. Epub 2018 Feb 7.
Merati AL, Lim HJ, Ulualp SO et al (2005) Meta-analysis of upper probe measurements in normal subjects and patients with laryngopharyngeal reflux. Ann Otol Rhinol Laryngol 114:177– 18.
Patti MG, Debas HT, Pellegrini CA. Clinical and functional characterization of high gastroesophageal reflux. Am J Surg. 1993 Jan; 165(1):163-6; discussion 166-8.
Neto RML, Herbella FAM, Schlottmann F, Patti MG. Does DeMeester score still define GERD? Dis Esophagus. 2019 May 1;32(5):doy118. https://doi.org/10.1093/dote/doy118.
Ayazi S, Hagen J A, Zehetner J et al. Proximal esophageal pH monitoring: improved definition of normal values and determination of a composite pH score. J Am Coll Surg 2010; 210: 345–50.
Zerbib F, Roman S, Bruley Des Varannes S, Gourcerol G, Coffin B, Ropert A, Lepicard P, Mion F; Groupe Français De Neuro-Gastroentérologie. Normal values of pharyngeal and esophageal 24hour pH impedance in individul son and of therapy and inter observer reproducibility. Clin Gastroenterol Hepatol. 2013 Apr;11(4):366-72. https://doi.org/10.1016/j.cgh.2012.10.041. Epub 2012 Nov 8.
Tack, J., & Pandolfino, J. E. (2018). Pathophysiology of Gastroesophageal Reflux Disease. Gastroenterology, 154(2), 277–288. doi: https://doi.org/10.1053/j.gastro.2017.09.047
Ribolsi M, Balestrieri P, Holloway RH, Emerenziani S, Cicala M. Intra-bolus pressure and esophagogastric gradient, assessed with high-resolution manometry, are associated with acid exposure and proximal migration of refluxate. Dis Esophagus. 2016 Nov;29(8):1020-1026.
Pauwels A, Blondeau K, Dupont LJ, Sifrim D. Mechanisms of increased gastroesophageal reflux in patients with cystic fibrosis. Am J Gastroenterol. 2012 Sep;107(9):1346-53. https://doi.org/10.1038/ajg.2012.213. Epub 2012 Jul 10.
Ricci G, Amella C, Forti E, Rossi A, Bersani G, Dari S, Pasini V, Maimone A, Alvisi V. 24-h pH-metry and multichannel intraluminal impedance monitoring in obese patients with and without gastroesophageal reflux disease symptoms. Obes Surg. 2011 Jan;21(1):48-53. https://doi.org/10.1007/s11695-010-0275-z.
Valezi AC, Herbella FAM, Schlottmann F, Patti MG. Gastroesophageal Reflux Disease in Obese Patients. J Laparoendosc Adv Surg Tech A. 2018 Aug;28(8):949-952. https://doi.org/10.1089/lap.2018.0395
Herbella FA, Sweet MP, Tedesco P, Nipomnick I, Patti MG. Gastroesophageal reflux disease and obesity. Pathophysiology and implications for treatment. J Gastrointest Surg. 2007 Mar; 11(3):286-90
Sweet MP, Herbella FA, Leard L, Hoopes C, Golden J, Hays S, Patti MG. The prevalence of distal and proximal gastroesophageal reflux in patients awaiting lung transplantation. Ann Surg. 2006 Oct;244(4):491-7.
Allaix ME, Fisichella PM, Noth I, Mendez BM, Patti MG. The pulmonary side of reflux disease: from heartburn to lung fibrosis. J Gastrointest Surg. 2013 Aug; 17(8):1526-35.
Kempainen RR, Savik K, Whelan TP, Dunitz JM, Herrington CS, Billings JL. High prevalence of proximal and distal gastroesophageal reflux disease in advanced COPD. Chest. 2007 Jun;131(6):1666-71
Pellegrini CA, DeMeester TR., Johnson, LF, Skinner DB. Gastroesophageal reflux and pulmonary aspiration: incidence, functional abnormality, and results of surgical therapy. Surgery 1979; 86:110–118.
Sweet MP, Patti MG, Hoopes C, Hays SR, Golden JA. Gastro-oesophageal reflux and aspiration in patients with advanced lung disease. Thorax. 2009 Feb;64(2):167-73.
Amarasiri DL, Pathmeswaran A, de Silva HJ, Ranasinha CD. Response of the airways and autonomic nervous system to acid perfusion of the esophagus in patients with asthma: a laboratory study. BMC Pulm Med. 2013 Jun 2; 13:33.
Author information
Authors and Affiliations
Contributions
Conception and design, acquisition of data, analysis and interpretation of data, drafting the article: LMDG, FAMH.Acquisition of data, review for intellectual content, final approval of the version to be published: LMDG, FAMH.
Conception and design, review for intellectual content, final approval of the version to be published: LMDG, FAMH, MGP.
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Plenary session presentation at the SSAT annual meeting, 2020
Rights and permissions
About this article
Cite this article
Del Grande, L.d.M., Herbella, F.A.M. & Patti, M.G. The Role of the Transdiaphragmatic Pressure Gradient (TGP) in the Pathophysiology of Proximal Reflux. J Gastrointest Surg 25, 351–356 (2021). https://doi.org/10.1007/s11605-020-04849-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-020-04849-3