Abstract
Background
Racial disparities exist in patients with rectal cancer with respect to both treatment and survival. Minority-serving hospitals (MSHs) provide healthcare to a disproportionately large percent of minority patients in the USA. We examined the effects of rectal cancer treatment at MSH to understand drivers of these disparities.
Methods
The NCDB was queried (2004–2015), and patients diagnosed with stage II or III rectal adenocarcinoma were identified. Racial case mix distribution was calculated at the institutional level, and MSHs were defined as those within the top decile of Black and Hispanic patients. Logistic regression was used to identify predictors of receipt of standard of care treatment. Survival was assessed using the Kaplan-Meier method, and Cox proportional hazards models were used to evaluate adjusted risk of death. Analyses were clustered by facility.
Results
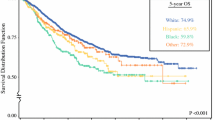
A total of 68,842 patients met the inclusion criteria. Of these patients, 63,242 (91.9%) were treated at non-MSH, and 5600 (8.1%) were treated at MSH. In multivariable analysis, treatment at MSH (OR 0.70 95%CI 0.61–0.80 p < 0.001) and Black race (OR 0.75 95%CI 0.70–0.81 p < 0.001) were associated with significantly lower odds of receiving standard of care. In adjusted analysis, Black patients had a significantly higher risk of mortality (HR 1.20 95%CI 1.14–1.26 p < 0.001).
Conclusions
Treatment at MSH institutions and Black race were associated with significantly decreased odds of receipt of recommended standard therapy for locally advanced rectal adenocarcinoma. Survival was worse for Black patients compared to White patients despite adjustment for receipt of standard of care.


Similar content being viewed by others
References
ACS. Cancer Facts & Figures 2019 Atlanta, GA: American Cancer Society; 2019 [Available from: https://www.cancer.org/cancer/colon-rectal-cancer/about/key-statistics.html.
Carethers JM. Systemic treatment of advanced colorectal cancer: tailoring therapy to the tumor. Therap Adv Gastroenterol. 2008;1(1):33-42.
Daly MC, Jung AD, Hanseman DJ, Shah SA, Paquette IM. Surviving rectal cancer: examination of racial disparities surrounding access to care. J Surg Res. 2017;211:100-6.
Morris AM, Wei Y, Birkmeyer NJ, Birkmeyer JD. Racial disparities in late survival after rectal cancer surgery. J Am Coll Surg. 2006;203(6):787-94.
Morris AM, Billingsley KG, Baxter NN, Baldwin LM. Racial disparities in rectal cancer treatment: a population-based analysis. Arch Surg. 2004;139(2):151-5; discussion 6.
Marcella S, Miller JE. Racial differences in colorectal cancer mortality. The importance of stage and socioeconomic status. J Clin Epidemiol. 2001;54(4):359-66.
NCCN. National Comprehensive Cancer Network Clinical Practice Guidelines in Oncology: Rectal Cancer (Version 3.2018) 2018 [Available from: https://www.nccn.org/professionals/physician_gls/pdf/rectal.pdf.
Jha AK, Orav EJ, Li Z, Epstein AM. Concentration and quality of hospitals that care for elderly black patients. Arch Intern Med. 2007;167(11):1177-82.
Tsai TC, Orav EJ, Joynt KE. Disparities in surgical 30-day readmission rates for Medicare beneficiaries by race and site of care. Ann Surg. 2014;259(6):1086-90.
Shih T, Ryan AM, Gonzalez AA, Dimick JB. Medicare's Hospital Readmissions Reduction Program in Surgery May Disproportionately Affect Minority-serving Hospitals. Ann Surg. 2015;261(6):1027-31.
Cheng EM, Keyhani S, Ofner S, Williams LS, Hebert PL, Ordin DL, et al. Lower use of carotid artery imaging at minority-serving hospitals. Neurology. 2012;79(2):138-44.
Creanga AA, Bateman BT, Mhyre JM, Kuklina E, Shilkrut A, Callaghan WM. Performance of racial and ethnic minority-serving hospitals on delivery-related indicators. Am J Obstet Gynecol. 2014;211(6):647.e1-16.e1.
Fletcher SA, Gild P, Cole AP, Vetterlein MW, Kibel AS, Choueiri TK, et al. The effect of treatment at minority-serving hospitals on outcomes for bladder cancer. Urol Oncol. 2018;36(5):238 e7-e17.
Hasnain-Wynia R, Kang R, Landrum MB, Vogeli C, Baker DW, Weissman JS. Racial and ethnic disparities within and between hospitals for inpatient quality of care: an examination of patient-level Hospital Quality Alliance measures. J Health Care Poor Underserved. 2010;21(2):629-48.
Krimphove MJ, Fletcher SA, Cole AP, Berg S, Sun M, Lipsitz SR, et al. Quality of Care in the Treatment of Localized Intermediate and High Risk Prostate Cancer at Minority Serving Hospitals. J Urol. 2019.
Winchester DP, Stewart AK, Phillips JL, Ward EE. The national cancer data base: past, present, and future. Ann Surg Oncol. 2010;17(1):4-7.
Figueroa JF, Zheng J, Orav EJ, Epstein AM, Jha AK. Medicare Program Associated With Narrowing Hospital Readmission Disparities Between Black And White Patients. Health Aff (Millwood). 2018;37(4):654-61.
Deyo RA, Cherkin DC, Ciol MA. Adapting a clinical comorbidity index for use with ICD-9-CM administrative databases. J Clin Epidemiol. 1992;45(6):613-9.
Berho M, Narang R, Van Koughnett JA, Wexner SD. Modern multidisciplinary perioperative management of rectal cancer. JAMA Surg. 2015;150(3):260-6.
Cedermark B, Dahlberg M, Glimelius B, Påhlman L, Rutqvist LE, Wilking N, et al. Improved survival with preoperative radiotherapy in resectable rectal cancer. N Engl J Med. 1997;336(14):980-7.
Folkesson J, Birgisson H, Pahlman L, Cedermark B, Glimelius B, Gunnarsson U. Swedish Rectal Cancer Trial: long lasting benefits from radiotherapy on survival and local recurrence rate. J Clin Oncol. 2005;23(24):5644-50.
van Gijn W, Marijnen CA, Nagtegaal ID, Kranenbarg EM, Putter H, Wiggers T, et al. Preoperative radiotherapy combined with total mesorectal excision for resectable rectal cancer: 12-year follow-up of the multicentre, randomised controlled TME trial. Lancet Oncol. 2011;12(6):575-82.
Ward E, Halpern M, Schrag N, Cokkinides V, DeSantis C, Bandi P, et al. Association of insurance with cancer care utilization and outcomes. CA Cancer J Clin. 2008;58(1):9-31.
Faigle R, Cooper LA, Gottesman RF. Lower carotid revascularization rates after stroke in racial/ethnic minority-serving US hospitals. Neurology. 2019;92(23):e2653-e60.
Ashktorab H, Vilmenay K, Brim H, Laiyemo AO, Kibreab A, Nouraie M. Colorectal Cancer in Young African Americans: Is It Time to Revisit Guidelines and Prevention? Dig Dis Sci. 2016;61(10):3026-30.
Alexander DD, Waterbor J, Hughes T, Funkhouser E, Grizzle W, Manne U. African-American and Caucasian disparities in colorectal cancer mortality and survival by data source: an epidemiologic review. Cancer Biomark. 2007;3(6):301-13.
Ellis L, Canchola AJ, Spiegel D, Ladabaum U, Haile R, Gomez SL. Racial and Ethnic Disparities in Cancer Survival: The Contribution of Tumor, Sociodemographic, Institutional, and Neighborhood Characteristics. J Clin Oncol. 2018;36(1):25-33.
Govindarajan R, Shah RV, Erkman LG, Hutchins LF. Racial differences in the outcome of patients with colorectal carcinoma. Cancer. 2003;97(2):493-8.
Clegg LX, Li FP, Hankey BF, Chu K, Edwards BK. Cancer survival among US whites and minorities: a SEER (Surveillance, Epidemiology, and End Results) Program population-based study. Arch Intern Med. 2002;162(17):1985-93.
Roetzheim RG, Pal N, Gonzalez EC, Ferrante JM, Van Durme DJ, Krischer JP. Effects of health insurance and race on colorectal cancer treatments and outcomes. Am J Public Health. 2000;90(11):1746-54.
Berry J, Bumpers K, Ogunlade V, Glover R, Davis S, Counts-Spriggs M, et al. Examining racial disparities in colorectal cancer care. J Psychosoc Oncol. 2009;27(1):59-83.
Lee DY, Teng A, Pedersen RC, Tavangari FR, Attaluri V, McLemore EC, et al. Racial and Socioeconomic Treatment Disparities in Adolescents and Young Adults with Stage II-III Rectal Cancer. Ann Surg Oncol. 2017;24(2):311-8.
Rapp J, Tuminello S, Alpert N, Flores RM, Taioli E. Disparities in surgery for early-stage cancer: the impact of refusal. Cancer Causes Control. 2019.
Rahouma M, Harrison S, Kamel M, Nasar A, Lee B, Port J, et al. Consequences of Refusing Surgery for Esophageal Cancer: A National Cancer Database Analysis. Ann Thorac Surg. 2018;106(5):1476-83.
Fields AC, Lu PW, Yoo J, Irani J, Goldberg JE, Bleday R, et al. Treatment of stage I-III rectal cancer: Who is refusing surgery? J Surg Oncol. 2020.
Lu PW, Fields AC, Yoo J, Irani J, Goldberg JE, Bleday R, et al. Sociodemographic predictors of surgery refusal in patients with stage I-III colon cancer. J Surg Oncol. 2020.
Penner LA, Harper FWK, Dovidio JF, Albrecht TL, Hamel LM, Senft N, et al. The impact of Black cancer patients' race-related beliefs and attitudes on racially-discordant oncology interactions: A field study. Soc Sci Med. 2017;191:99-108.
Adams LB, Richmond J, Corbie-Smith G, Powell W. Medical Mistrust and Colorectal Cancer Screening Among African Americans. J Community Health. 2017;42(5):1044-61.
Ko CW, Kreuter W, Baldwin LM. Persistent demographic differences in colorectal cancer screening utilization despite Medicare reimbursement. BMC Gastroenterol. 2005;5:10.
Monson JR, Probst CP, Wexner SD, Remzi FH, Fleshman JW, Garcia-Aguilar J, et al. Failure of evidence-based cancer care in the United States: the association between rectal cancer treatment, cancer center volume, and geography. Ann Surg. 2014;260(4):625-31; discussion 31-2.
Brady JT, Xu Z, Scarberry KB, Saad A, Fleming FJ, Remzi FH, et al. Evaluating the Current Status of Rectal Cancer Care in the US: Where We Stand at the Start of the Commission on Cancer's National Accreditation Program for Rectal Cancer. J Am Coll Surg. 2018;226(5):881-90.
American College of Surgeons. National Accreditation Program for Rectal Cancer (NAPRC) 2017 [Available from: https://www.facs.org/quality-programs/cancer/naprc.
Antunez AG, Kanters AE, Regenbogen SE. Evaluation of Access to Hospitals Most Ready to Achieve National Accreditation for Rectal Cancer Treatment. JAMA Surg. 2019.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
QDT receives honoraria from Astellas, Bayer, Intuitive Surgical, and InsighTec. All the other authors declare no conflicts.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This study was presented as a podium presentation at the 14th annual Academic Surgical Congress, held February 5-7, 2019 in Houston, TX.
Rights and permissions
About this article
Cite this article
Lu, P.W., Scully, R.E., Fields, A.C. et al. Racial Disparities in Treatment for Rectal Cancer at Minority-Serving Hospitals. J Gastrointest Surg 25, 1847–1856 (2021). https://doi.org/10.1007/s11605-020-04744-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-020-04744-x