Abstract
Objectives
The role of laparoscopic hepatectomy (LH) for intrahepatic cholangiocarcinoma (ICC) remains indefinite, though the utilization of this minimally invasive approach has been increasing for ICC. We herein performed a meta-analysis to investigate this issue.
Methods
Six retrospective studies including 384 patients who had undergone LH and 2147 patients who had undergone open hepatectomy (OH) for ICC were included. The fixed-effects or random-effects models were utilized for data analysis.
Results
Compared with patients who had undergone OH for ICC, patients who had undergone LH for ICC experienced more R0 resections (81.6 versus 73.8%, risk ratio (RR) = 1.08, 95% confidence interval (CI) 1.02–1.14; P = 0.008) but less major hepatectomies (37.7 versus 54.2%, RR = 0.69, 95% CI 0.60–0.79; P < 0.0001), less lymph node dissections (38.0 versus 61.5%, RR = 0.62, 95% CI 0.54–0.70; P < 0.0001), and smaller tumor size resected (4.14 versus 4.94 cm, weighted mean difference = − 0.80 cm, 95% CI − 1.38 to − 0.22 cm; P = 0.007). No significant difference was observed in other perioperative results (all P > 0.05) or overall survival (hazard ratio (HR) = 1.38, 95% CI 0.63–3.02; P = 0.43).
Conclusions
LH has comparable safety, feasibility, and oncological efficacy to that of OH for ICC and has superiority in R0 resection over OH. It may be time to consider LH for ICC only if a more thorough effort on lymph node dissection is undertaken in selective patients at experienced centers.


Similar content being viewed by others
References
Razumilava N, Gores GJ. Cholangiocarcinoma. The Lancet 2014; 383: 2168–2179.
Banales JM, Cardinale V, Carpino G, et al. Expert consensus document: Cholangiocarcinoma: current knowledge and future perspectives consensus statement from the European Network for the Study of Cholangiocarcinoma (ENS-CCA). Nat Rev Gastroenterol Hepatol 2016; 13: 261–280.
Sirica AE, Gores GJ, Groopman JD, et al. Intrahepatic Cholangiocarcinoma: Continuing Challenges and Translational Advances. Hepatology 2018; 69:1803–1815.
Ransome E, Tong L, Espinosa J, et al. Trends in surgery and disparities in receipt of surgery for intrahepatic cholangiocarcinoma in the US: 2005-2014. J Gastrointest Oncol 2019; 10: 339–347.
Antwi SO, Mousa OY, Patel T. Racial, Ethnic, and Age Disparities in Incidence and Survival of Intrahepatic Cholangiocarcinoma in the United States; 1995-2014. Ann Hepatol 2018; 17: 274–285.
Chan KM, Tsai CY, Yeh CN, et al. Characterization of intrahepatic cholangiocarcinoma after curative resection: outcome, prognostic factor, and recurrence. BMC Gastroenterology 2018;18:180.
Choi SB, Kim KS, Choi JY, et al. The prognosis and survival outcome of intrahepatic cholangiocarcinoma following surgical resection: association of lymph node metastasis and lymph node dissection with survival. Ann Surg Oncol 2009; 16: 3048–3056.
Uchiyama K, Yamamoto M, Yamaue H, et al. Impact of nodal involvement on surgical outcomes of intrahepatic cholangiocarcinoma: a multicenter analysis by the Study Group for Hepatic Surgery of the Japanese Society of Hepato-Biliary-Pancreatic Surgery. J Hepatobiliary Pancreat Sci 2011; 18: 443–452.
Lurje G, Bednarsch J, Czigany Z, et al. The prognostic role of lymphovascular invasion and lymph node metastasis in perihilar and intrahepatic cholangiocarcinoma. Eur J Surg Oncol 2019; 45:1468-1478.
Mahul B. Amin, Stephen Edge, Frederick Greene, et al. AJCC Cancer Staging Manual, 8th edition. Springer International Publishing 2017; 297–299Hardcover ISBN. 978-3-319-40617-6.
Zhang XF, Chakedis J, Bagante F, et al. Trends in use of lymphadenectomy in surgery with curative intent for intrahepatic cholangiocarcinoma. Br J Surg 2018; 105: 857–866.
Kim SH, Han DH, Choi GH, et al. Oncologic Impact of Lymph Node Dissection for Intrahepatic Cholangiocarcinoma: a Propensity Score-Matched Study. J Gastrointest Surg 2018; 23:538–544.
Li DY, Zhang HB, Yang N, et al. Routine lymph node dissection may be not suitable for all intrahepatic cholangiocarcinoma patients: Results of a monocentric series. World J Gastroenterol 2013; 19:9084–9091.
Zhou R, Lu D, Li W, et al. Is lymph node dissection necessary for resectable intrahepatic cholangiocarcinoma? A systematic review and meta-analysis. HPB (Oxford) 2019; 21:784–792.
Ciria R, Cherqui D, Geller DA, et al. Comparative Short-term Benefits of Laparoscopic Liver Resection: 9000 Cases and Climbing. Ann Surg 2016; 263: 761–777.
Xiangfei M, Yinzhe X, Yingwei P, et al. Open versus laparoscopic hepatic resection for hepatocellular carcinoma: a systematic review and meta-analysis. Surg Endosc 2019; 33:2396–2418.
Uy BJ, Han HS, Yoon YS, et al. Laparoscopic Liver Resection for Intrahepatic Cholangiocarcinoma. J Laparoendosc Adv Surg Tech A 2015; 25:272–277.
Ratti F, Cipriani F, Ariotti R, et al. Safety and feasibility of laparoscopic liver resection with associated lymphadenectomy for intrahepatic cholangiocarcinoma: a propensity score-based case-matched analysis from a single institution. Surg Endosc 2016; 30: 1999–2010.
Lee W, Park JH, Kim JY, et al. Comparison of perioperative and oncologic outcomes between open and laparoscopic liver resection for intrahepatic cholangiocarcinoma. Surg Endosc 2016; 30: 4835–4840.
Wei F, Lu C, Cai L, et al. Can laparoscopic liver resection provide a favorable option for patients with large or multiple intrahepatic cholangiocarcinomas? Surg Endosc 2017; 31: 3646–3655.
Moher D, Liberati A, Tetzlaff J, et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. J Clin Epidemiol 2009; 62:1006–1012.
Stroup DF, Berlin JA, Morton SC, et al. Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA. 2000; 283:2008–2012.
Wells GA, Shea B, O’Connell D, et al. The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. [Cited 1 Jun 2019.] Available from URL: http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp
Hozo SP, Djulbegovic B, Hozo I. Estimating the mean and variance from the median, range, and the size of a sample. BMC Med Res Methodol 2005; 5:13.
Tierney JF, Stewart LA, Ghersi D, et al. Practical methods for incorporating summary time-to-event data into meta-analysis. Trials 2007; 8:16.
Kinoshita M, Kanazawa A, Takemura S, et al. Indications for laparoscopic liver resection of mass-forming intrahepatic cholangiocarcinoma. Asian J Endosc Surg. 2019 Mar 28. https://doi.org/10.1111/ases.12703. [Epub ahead of print]
Martin SP, Drake J, Wach MM, et al. Laparoscopic Approach to Intrahepatic Cholangiocarcinoma is Associated with an Exacerbation of Inadequate Nodal Staging. Ann Surg Oncol 2019;26:1851–1857.
Ratti F, Fiorentini G, Cipriani F, et al. Perioperative and Long-Term Outcomes of Laparoscopic Versus Open Lymphadenectomy for Biliary Tumors: A Propensity-Score-Based, Case-Matched Analysis. Ann Surg Oncol 2019;26:564–575.
Buell JF, Cherqui D, Geller DA, et al. The international position on laparoscopic liver surgery: The Louisville Statement, 2008. Ann Surg 2009;250:825–830.
Wakabayashi G, Cherqui D, Geller DA, et al. Recommendations for laparoscopic liver resection: a report from the second international consensus conference held in Morioka. Ann Surg 2015; 261:619–629.
Jiang S, Wang Z, Ou M, et al. Laparoscopic Versus Open Hepatectomy in Short- and Long-Term Outcomes of the Hepatocellular Carcinoma Patients with Cirrhosis: A Systematic Review and Meta-Analysis. J Laparoendosc Adv Surg Tech A; 2019 Jan 31. https://doi.org/10.1089/lap.2018.0588. [Epub ahead of print].
Ciria R, Ocaña S, Gomez-Luque I, et al. A systematic review and meta-analysis comparing the short- and long-term outcomes for laparoscopic and open liver resections for liver metastases from colorectal cancer. Surg Endosc. 2019 Apr 15. https://doi.org/10.1007/s00464-019-06774-2.
Harimoto N, Shimada M, Tsujita E, et al. Laparoscopic hepatectomy and dissection of lymph nodes for intrahepatic cholangiocarcinoma. Case report. Surg Endosc 2002; 16:1806.
Abu Hilal M, Badran A, Di Fabio F, et al. Pure Laparoscopic En Bloc Left Hemihepatectomy and Caudate Lobe Resection in Patients with Intrahepatic Cholangiocarcinoma. J Laparoendosc Adv Surg Tech A 2011;21:845–849.
Takahashi M, Wakabayashi G, Nitta H, et al. Pure laparoscopic right hepatectomy by anterior approach with hanging maneuver for large intrahepatic cholangiocarcinoma. Surg Endosc 2013; 27:4732–4733.
Saito Y, Yamada S, Imura S, et al. A learning curve for laparoscopic liver resection: an effective training system and standardization of technique. Transl Gastroenterol Hepatol 2018; 3:45.
Jia C, Li H, Wen N, et al. Laparoscopic liver resection: a review of current indications and surgical techniques. Hepatobiliary Surg Nutr 2018; 7:277–288.
Ogiso S, Nomi T, Araki K, et al. Laparoscopy-Specific Surgical Concepts for Hepatectomy Based on the Laparoscopic Caudal View: A Key to Reboot Surgeons’ Minds. Annals of Surgical Oncology 2015; 22: S327–333.
Nomi T, Hokuto D, Yoshikawa T, et al. A Novel Navigation for Laparoscopic Anatomic Liver Resection Using Indocyanine Green Fluorescence. Ann Surg Oncol 2018; 25: 3982.
Aoki T, Murakami M, Koizumi T, et al. Determination of the surgical margin in laparoscopic liver resections using infrared indocyanine green fluorescence. Langenbecks Arch Surg 2018; 403: 671–680.
Wu L, Tsilimigras DI, Paredes AZ, et al. Trends in the Incidence, Treatment and Outcomes of Patients with Intrahepatic Cholangiocarcinoma in the USA: Facility Type is Associated with Margin Status, Use of Lymphadenectomy and Overall Survival. World J Surg 2019; 43: 1777–1787.
Zhang XF, Lv Y, Weiss M, et al. Should Utilization of Lymphadenectomy Vary According to Morphologic Subtype of Intrahepatic Cholangiocarcinoma? Ann Surg Oncol 2019; 26: 2242–2250.
Morine Y, Shimada M. The value of systematic lymph node dissection for intrahepatic cholangiocarcinoma from the viewpoint of liver lymphatics. J Gastroenterol 2015; 50:913–927.
Lendoire JC, Gil L, Imventarza O. Intrahepatic cholangiocarcinoma surgery: the impact of lymphadenectomy. Chin Clin Oncol 2018; 7: 53.
Bagante F, Spolverato G, Weiss M, et al. Surgical Management of Intrahepatic Cholangiocarcinoma in Patients with Cirrhosis: Impact of Lymphadenectomy on Peri-Operative Outcomes. World J Surg. 2018;42:2551–2560.
Author information
Authors and Affiliations
Contributions
FQ Wei conceived and designed the study. G Wang, JY Ding, and TN Yu acquired and analyzed the data. CW Dou and CW Zhang interpreted the data. FQ Wei wrote the manuscript. G Wang helped to revise the manuscript. All authors read and approved the manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethics Approval and Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Table S1
Meta-analysis of baseline characteristics. (DOCX 97 kb)
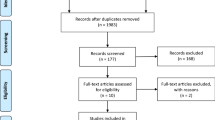
Figure S1
Flowchart of included studies. (PNG 69 kb)
Figure S2
Results of the meta-analysis on perioperative outcomes: (A) The mean difference of operation time in minutes in laparoscopic hepatectomy (LH) in comparison with open hepatectomy (OH); (B) The mean difference of blood loss in milliliter in LH in comparison with OH; (C) The T1 stage tumors rate in LH in comparison with OH; (D)The well differentiation tumors rate in LH in comparison with OH; (E) The morbidity rate in LH in comparison with OH; (F) The mean difference of hospital stay in days in LH in comparison with OH. (PNG 469 kb)
Rights and permissions
About this article
Cite this article
Wei, F., Wang, G., Ding, J. et al. Is It Time to Consider Laparoscopic Hepatectomy for Intrahepatic Cholangiocarcinoma? A Meta-Analysis. J Gastrointest Surg 24, 2244–2250 (2020). https://doi.org/10.1007/s11605-019-04404-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-019-04404-9