Abstract
Background
Portal vein stenosis develops in 3.4–14% of split liver transplantation1,2,–3 and its early detection and treatment are essential to achieve long-term graft survival,2,3,4,–5 although the diagnostic capability of conventional modalities such as Doppler ultrasound and computed tomography is limited.1,1,,4,5
Methods
This study used computational fluid dynamics to analyze portal vein hemodynamics in the management of post-transplant portal vein stenosis. To perform computational fluid dynamics analyses, three-dimensional portal vein model was created using computed tomographic DICOM data. The inlet flow condition was set according the flow velocity measured on Doppler ultrasonography. Finally, portal vein flow was simulated on a fluid analysis software (Software Cradle, Japan).
Results
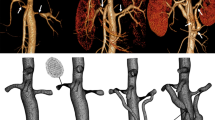
An 18-month-old girl underwent liver transplantation using a left lateral graft for biliary atresia. At the post-transplant 1-week evaluation, the computational fluid dynamics streamline analysis visualized vortices and an accelerated flow with a velocity ratio < 2 around the anastomotic site. The wall shear stress analysis revealed a high wall shear stress area within the post-anastomotic portal vein. At the post-transplant 6-month evaluation, the streamline analysis illustrated the increased vortices and worsening flow acceleration to reach the proposed diagnostic criteria (velocity ratio > 3:1).3,5 The pressure analysis revealed a positive pressure gradient of 3.8 mmHg across the stenotic site. Based on the findings, the patient underwent percutaneous transhepatic portal venoplasty with balloon dilation. The post-treatment analyses confirmed the improvement of a jet flow, vortices, a high wall shear stress, and a pressure gradient.
Discussion
The computational fluid dynamics analyses are useful for prediction, early detection, and follow-up of post-transplant portal vein stenosis and would be a promising technology in post-transplant management.
Similar content being viewed by others
References
Buell JF, Funaki B, Cronin DC, et al. Long-term venous complications after full-size and segmental pediatric liver transplantation. Ann Surg 2002; 236(5):658-66.
Cheng YF, Ou HY, Tsang LL, et al. Vascular stents in the management of portal venous complications in living donor liver transplantation. Am J Transplant 2010; 10(5):1276-83.
Yabuta M, Shibata T, Shinozuka K, et al. Long-term outcome of percutaneous transhepatic balloon angioplasty for portal vein stenosis after pediatric living donor liver transplantation: a single institute's experience. J Vasc Interv Radiol 2014; 25(9):1406-12.
Shibata T, Itoh K, Kubo T, et al. Percutaneous transhepatic balloon dilation of portal venous stenosis in patients with living donor liver transplantation. Radiology 2005; 235(3):1078-83.
Huang TL, Cheng YF, Chen TY, et al. Doppler ultrasound evaluation of postoperative portal vein stenosis in adult living donor liver transplantation. Transplant Proc 2010; 42(3):879-81.
Funding
This work was supported by the Medical Research Fund, Takeda Science Foundation.
Author information
Authors and Affiliations
Contributions
Conception and design of the work: S Ogiso, M Nakamura, K Itatani, N Kurata, and Y Ogura
Acquisition and analysis of the data: S Ogiso, M Nakamura, T Tanaka, K Komiya, and K Jobara
Interpretation of the data: S Ogiso, M Nakamura, H Kamei, Y Onishi, K Itatani, and Y Ogura
Drafting the work: S Ogiso, M Nakamura, T Tanaka, and Y Ogura
Critical revision: H Kamei, Y Onishi, K Itatani, K Komiya, K Jobara, and N Kurata
All authors approved the final version of the article and agreed to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
(WMV 37639 kb)
Rights and permissions
About this article
Cite this article
Ogiso, S., Nakamura, M., Tanaka, T. et al. Computational Fluid Dynamics-Based Blood Flow Assessment Facilitates Optimal Management of Portal Vein Stenosis After Liver Transplantation. J Gastrointest Surg 24, 460–461 (2020). https://doi.org/10.1007/s11605-019-04279-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-019-04279-w