Abstract
Background
Colorectal liver metastases that demonstrate a complete radiographic response during chemotherapy are increasingly common with advances in chemotherapy regimens and are described as disappearing liver metastases (DLMs). However, these DLMs often continue to harbor residual viable tumor. If these tumors are found in the operating room with ultrasound (US), they should be treated. The intraoperative sonographic visualization of these lesions, however, can be hindered by chemotherapy-associated liver parenchyma changes. The objective of this study was to evaluate the use of an intraoperative image guidance system, Explorer (Analogic Corporation, Peabody, MA), to aid surgeons in the identification of DLMs initially undetected by US alone.
Study Design
In a single-arm prospective trial, patients with colorectal liver metastases undergoing liver resection and/or ablation with one or more DLMs during neoadjuvant chemotherapy were enrolled. Intraoperatively, DLMs were localized with conventional US. Any DLM not found by conventional US was re-evaluated with the image guidance system. The primary outcome was the proportion of sonographically occult DLMs subsequently located by image-guided US.
Results
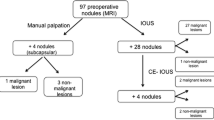
Between April 2016 and November 2017, 25 patients with 61 DLMs were enrolled. Thirty-eight DLMs (62%) in 14 patients (56%) were not identified with US alone. Six (16%) DLMs in five patients (36%) were subsequently located with assistance of the image guidance system. The image guidance changed the intraoperative surgical plan in four of these patients.
Conclusions
Image guidance can aid surgeons in the identification of initially sonographically occult DLMs and facilitate the complete surgical clearance of all sites of liver disease.



Similar content being viewed by others
References
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2015. CA: a cancer journal for clinicians. 2015 Jan-Feb;65(1):5–29.
Steele G, Jr., Ravikumar TS. Resection of hepatic metastases from colorectal cancer. Biologic perspective. Annals of surgery. 1989 Aug;210(2):127–38.
Qiu M, Hu J, Yang D, Cosgrove DP, Xu R. Pattern of distant metastases in colorectal cancer: a SEER based study. Oncotarget. 2015 Nov 17;6(36):38658–66.
Adam R, Wicherts DA, de Haas RJ, et al. Complete pathologic response after preoperative chemotherapy for colorectal liver metastases: myth or reality?, Journal of clinical oncology : official journal of the American Society of Clinical Oncology. 2008 Apr 1;26(10):1635–41.
Auer RC, White RR, Kemeny NE, et al. Predictors of a true complete response among disappearing liver metastases from colorectal cancer after chemotherapy. Cancer. 2010 Mar 15;116(6):1502–9.
Ferrero A, Langella S, Russolillo N, Vigano L, Lo Tesoriere R, Capussotti L. Intraoperative detection of disappearing colorectal liver metastases as a predictor of residual disease. Journal of gastrointestinal surgery : official journal of the Society for Surgery of the Alimentary Tract. 2012 Apr;16(4):806–14.
van Vledder MG, de Jong MC, Pawlik TM, Schulick RD, Diaz LA, Choti MA. Disappearing colorectal liver metastases after chemotherapy: should we be concerned? Journal of gastrointestinal surgery : official journal of the Society for Surgery of the Alimentary Tract. 2010 Nov;14(11):1691–700.
Peppercorn PD, Reznek RH, Wilson P, Slevin ML, Gupta RK. Demonstration of hepatic steatosis by computerized tomography in patients receiving 5-fluorouracil-based therapy for advanced colorectal cancer. British journal of cancer. 1998 Jun;77(11):2008–11.
Zorzi D, Laurent A, Pawlik TM, Lauwers GY, Vauthey JN, Abdalla EK. Chemotherapy-associated hepatotoxicity and surgery for colorectal liver metastases. The British journal of surgery. 2007 Mar;94(3):274–86.
Carpenter S, Fong Y. Management of disappearing colorectal hepatic metastases. Advances in surgery. 2010;44:269–79.
Valls C, Iannacconne R, Alba E, et al. Fat in the liver: diagnosis and characterization. European radiology. 2006 Oct;16(10):2292–308.
Jolesz FA, Kikinis R, Talos IF. Neuronavigation in interventional MR imaging. Frameless stereotaxy. Neuroimaging clinics of North America. 2001 Nov;11(4):685–93, ix.
Benardete EA, Leonard MA, Weiner HL. Comparison of frameless stereotactic systems: accuracy, precision, and applications. Neurosurgery. 2001 Dec;49(6):1409–15; discussion 15-6.
Nasser R, Drazin D, Nakhla J, et al. Resection of spinal column tumors utilizing image-guided navigation: a multicenter analysis. Neurosurg Focus. 2016 Aug;41(2):E15.
Zumwalt TJ, Goel A. Immunotherapy of Metastatic Colorectal Cancer: Prevailing Challenges and New Perspectives. Current colorectal cancer reports. 2015 Jun 1;11(3):125–40.
Pishnamaz M, Wilkmann C, Na HS, et al. Electromagnetic Real Time Navigation in the Region of the Posterior Pelvic Ring: An Experimental In-Vitro Feasibility Study and Comparison of Image Guided Techniques. PloS one. 2016;11(2):e0148199.
Kingham TP, Scherer MA, Neese BW, Clements LW, Stefansic JD, Jarnagin WR. Image-guided liver surgery: intraoperative projection of computed tomography images utilizing tracked ultrasound. HPB : the official journal of the International Hepato Pancreato Biliary Association. 2012 Sep;14(9):594–603.
Kingham TP, Pak LM, Simpson AL, et al. 3D image guidance assisted identification of colorectal cancer liver metastases not seen on intraoperative ultrasound: results from a prospective trial. HPB (Oxford). 2018 Mar;20(3):260–67.
Kingham TP, Jayaraman S, Clements LW, Scherer MA, Stefansic JD, Jarnagin WR. Evolution of image-guided liver surgery: transition from open to laparoscopic procedures. Journal of gastrointestinal surgery : official journal of the Society for Surgery of the Alimentary Tract. 2013 Jul;17(7):1274–82.
van Vledder MG, Torbenson MS, Pawlik TM, et al. The effect of steatosis on echogenicity of colorectal liver metastases on intraoperative ultrasonography, Archives of surgery (Chicago, Ill : 1960). 2010 Jul;145(7):661–7.
Karoui M, Penna C, Amin-Hashem M, et al. Influence of preoperative chemotherapy on the risk of major hepatectomy for colorectal liver metastases. Annals of surgery. 2006 Jan;243(1):1–7.
Fernandez FG, Ritter J, Goodwin JW, Linehan DC, Hawkins WG, Strasberg SM. Effect of steatohepatitis associated with irinotecan or oxaliplatin pretreatment on resectability of hepatic colorectal metastases. Journal of the American College of Surgeons. 2005 Jun;200(6):845–53.
Kneuertz PJ, Maithel SK, Staley CA, Kooby DA. Chemotherapy-associated liver injury: impact on surgical management of colorectal cancer liver metastases. Annals of surgical oncology. 2011 Jan;18(1):181–90.
Benoist S, Brouquet A, Penna C, et al. Complete response of colorectal liver metastases after chemotherapy: does it mean cure?, Journal of clinical oncology : official journal of the American Society of Clinical Oncology. 2006 Aug 20;24(24):3939–45.
Arita J, Ono Y, Takahashi M, Inoue Y, Takahashi Y, Saiura A. Usefulness of contrast-enhanced intraoperative ultrasound in identifying disappearing liver metastases from colorectal carcinoma after chemotherapy. Annals of surgical oncology. 2014 Jun;21 Suppl 3:S390–7.
Sturesson C, Nilsson J, Lindell G, Andersson RG, Keussen I. Disappearing liver metastases from colorectal cancer: impact of modern imaging modalities. HPB (Oxford). 2015 Nov;17(11):983–7.
Torzilli G, Botea F, Donadon M, et al. Criteria for the selective use of contrast-enhanced intra-operative ultrasound during surgery for colorectal liver metastases. HPB : the official journal of the International Hepato Pancreato Biliary Association. 2014 Nov;16(11):994–1001.
Zendel A, Lahat E, Dreznik Y, Zakai BB, Eshkenazy R, Ariche A. “Vanishing liver metastases”-A real challenge for liver surgeons. Hepatobiliary surgery and nutrition. 2014 Oct;3(5):295–302.
Fowler KJ, Linehan DC, Menias CO. Colorectal liver metastases: state of the art imaging. Annals of surgical oncology. 2013 Apr;20(4):1185–93.
Niekel MC, Bipat S, Stoker J. Diagnostic imaging of colorectal liver metastases with CT, MR imaging, FDG PET, and/or FDG PET/CT: a meta-analysis of prospective studies including patients who have not previously undergone treatment. Radiology. 2010 Dec;257(3):674–84.
Park MJ, Hong N, Han K, et al. Use of Imaging to Predict Complete Response of Colorectal Liver Metastases after Chemotherapy: MR Imaging versus CT Imaging. Radiology. 2017 Aug;284(2):423–31.
Author information
Authors and Affiliations
Contributions
LMP contributed to study conception and design, data acquisition, analysis, and interpretation; manuscript drafting and revision; and final approval of this version for publication, and agrees to be accountable for all aspects of this work. JG contributed to data acquisition, analysis, and interpretation; manuscript drafting and revision; and final approval of this version for publication, and agrees to be accountable for all aspects of this work. PJA, VPB, MID, RPD, and WRJ contributed to study design, data acquisition, and interpretation; manuscript drafting and revision; and final approval of this version for publication, and agree to be accountable for all aspects of this work. MIM contributed to study conception, data interpretation, manuscript revision, and final approval of this version for publication, and agrees to be accountable for all aspects of this work. ALS and TPK contributed to study conception and design, data acquisition, analysis, and interpretation; manuscript drafting and revision; and final approval of this version for publication, and agree to be accountable for all aspects of this work.
Corresponding author
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This study was presented as an ePoster at the 13th World Congress of the International Hepato-Pancreato-Biliary Association in Geneva, Switzerland, September 4–7, 2018.
Rights and permissions
About this article
Cite this article
Pak, L.M., Gagnière, J., Allen, P.J. et al. Utility of Image Guidance in the Localization of Disappearing Colorectal Liver Metastases. J Gastrointest Surg 23, 760–767 (2019). https://doi.org/10.1007/s11605-019-04106-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-019-04106-2