Abstract
Background
Declining incidence of gastric cancer in the USA has presumably resulted in lower rates of major gastrectomy for cancer. The impact on perioperative outcomes remains undefined. The aims of this study were to characterize national trends in frequency of major gastrectomy for cancer, identify factors associated with in-hospital mortality, and examine outcome disparities by race/ethnicity.
Methods
Nationwide inpatient sample data from 1993 to 2013 were queried for procedural and diagnostic codes (ICD-9) relating to total and partial gastrectomy procedures. Gastric resections for cancer were compared to those for peptic ulcer disease for reference. Patient demographics, comorbidity score, mortality, and hospital characteristics were recorded as covariates.
Results
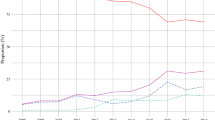
A significant decrease in annual rates of partial and total gastrectomy was observed from 1993 to 2013 (p < 0.0001). The change in absolute number and percent decline was greater for partial gastrectomy (− 39.3%) than total gastrectomy (− 19%). There was a 34.0% decrease in gastrectomy for cancer in Whites and a 61.2% increase among Hispanic patients over two decades. In-hospital mortality also significantly decreased over the study period (7.7% to 2.7%). Factors associated with lower mortality rates included male sex and treatment at urban teaching hospitals. Analysis of trends revealed that gastrectomy for cancer was performed with increasing frequency at urban teaching hospitals.
Conclusions
The frequency of major gastric resections in the USA has declined over two decades. Overall, in-hospital mortality rates also have decreased significantly. Declining in-hospital mortality after gastrectomy for cancer is associated with more frequent treatment at urban teaching hospitals.




Similar content being viewed by others
References
Weil PHB, R. From Billroth to PCV: a century of gastric surgery. World journal of surgery. 1999;23(7):736–42.
SEER Cancer Stat Facts: Stomach Cancer. Available from: https://seer.cancer.gov/statfacts/html/stomach.html; [cited 2017 Aug 11].
Lawrence W, Menck HR, Steele GD, Winchester DP. The National Cancer Data Base report on gastric cancer. Cancer. 1995;75(7):1734–44.
Lipof T, Shapiro D, Kozol RA. Surgical perspectives in peptic ulcer disease and gastritis. World J Gastroenterol. 2006;12(20):3248–52.
Schwesinger WH, Page CP, Sirinek KR, Gaskill HV, 3rd, Melnick G, Strodel WE. Operations for peptic ulcer disease: paradigm lost. Journal of gastrointestinal surgery : official journal of the Society for Surgery of the Alimentary Tract. 2001;5(4):438–43.
Ng EK, Lam YH, Sung JJ, Yung MY, To KF, Chan AC, Lee DW, Law BK, Lau JY, Ling TK, Lau WY, Chung SC. Eradication of Helicobacter pylori prevents recurrence of ulcer after simple closure of duodenal ulcer perforation: randomized controlled trial. Annals of surgery. 2000;231(2):153–8.
Feinstein LB, Holman RC, Yorita Christensen KL, Steiner CA, Swerdlow DL. Trends in hospitalizations for peptic ulcer disease, United States, 1998-2005. Emerg Infect Dis. 2010;16(9):1410–8.
Wainess RM, Dimick JB, Upchurch GR, Jr., Cowan JA, Mulholland MW. Epidemiology of surgically treated gastric cancer in the United States, 1988-2000. Journal of gastrointestinal surgery : official journal of the Society for Surgery of the Alimentary Tract. 2003;7(7):879–83.
Wang YR, Richter JE, Dempsey DT. Trends and outcomes of hospitalizations for peptic ulcer disease in the United States, 1993 to 2006. Annals of surgery. 2010;251(1):51–8. https://doi.org/10.1097/SLA.0b013e3181b975b8.
Lui FH, Tuan B, Swenson SL, Wong RJ. Ethnic disparities in gastric cancer incidence and survival in the USA: an updated analysis of 1992-2009 SEER data. Digestive diseases and sciences. 2014;59(12):3027–34. https://doi.org/10.1007/s10620-014-3275-3.
Healthcare Cost and Utilization Project (HCUP): overview of the Nationwide Inpatient Sample (NIS) [online]. [cited 2017 Apr 13]; Available from: http://www.hcup-us.ahrq.gov/nisoverview.jsp.
Healthcare Cost and Utilization Project (HCUP). Description of data elements: Nationwide Inpatient Sample (NIS). [cited 2017 Apr 13]; Available from: http://www.hcup-us.ahrq.gov/db/nation/nis/NISCORE_A-Lv3.pdf.
Healthcare Cost and Utilization Project (HCUP). Trend Weights for HCUP NIS Data. [cited 2017 Nov 11]; Available from: http://www.hcup-us.ahrq.gov/db/nation/nis/trendweights.jsp.
Houchens RE, A. Final Report on Calculating Nationwide Inpatient Sample (NIS) Variances for Data Years 2011 and Earlier. 2015. HCUP Methods Series Report # 2003-02 ONLINE. December 14, 2015. U.S. Agency for Healthcare Research and Quality. Available: http://www.hcup-us.ahrq.gov/reports/methods/methods.jsp.
Siegel RL, Miller KD, Jemal A. Cancer Statistics, 2017. CA: a cancer journal for clinicians. 2017;67(1):7–30. https://doi.org/10.3322/caac.21387.
Sarosi GA, Jr., Jaiswal KR, Nwariaku FE, Asolati M, Fleming JB, Anthony T. Surgical therapy of peptic ulcers in the 21st century: more common than you think. American journal of surgery. 2005;190(5):775–9. https://doi.org/10.1016/j.amjsurg.2005.07.019.
Wang H, Pawlik TM, Duncan MD, Hui X, Selvarajah S, Canner JK, Haider AH, Ahuja N, Schneider EB. Inpatient survival after gastrectomy for gastric cancer in the 21st century. The Journal of surgical research. 2014;190(1):72–8. https://doi.org/10.1016/j.jss.2014.03.015.
Smith JK, McPhee JT, Hill JS, Whalen GF, Sullivan ME, Litwin DE, Anderson FA, Tseng JF. National outcomes after gastric resection for neoplasm. Archives of surgery (Chicago, Ill : 1960). 2007;142(4):387-93.
Ellis RJ, Merkow RP. Exploring the Underlying Mechanisms of the Volume-Outcome Relationship in Complex Cancer Care. Annals of surgical oncology. 2017;24(8):2067–8.
Reavis KM, Hinojosa MW, Smith BR, Wooldridge JB, Krishnan S, Nguyen NT. Hospital volume is not a predictor of outcomes after gastrectomy for neoplasm. The American surgeon. 2009;75(10):932–6.
Wang A, Squires MH, 3rd, Melis M, Poultsides GA, Norton JA, Jin LX, Fields RC, Spolverato G, Pawlik TM, Votanopoulos KI, Levine EA, Schmidt C, Bloomston M, Cho CS, Weber S, Berman R, Pachter HL, Newman E, Staley CA, Maithel SK, Hatzaras I. Stage-Specific Prognostic Effect of Race in Patients with Resectable Gastric Adenocarcinoma: An 8-Institution Study of the US Gastric Cancer Collaborative. Journal of the American College of Surgeons. 2016;222(4):633–43. https://doi.org/10.1016/j.jamcollsurg.2015.12.043.
Anderson WF, Camargo MC, Fraumeni JF, Jr., Correa P, Rosenberg PS, Rabkin CS. Age-specific trends in incidence of noncardia gastric cancer in US adults. Jama. 2010;303(17):1723–8. https://doi.org/10.1001/jama.2010.496.
Merchant SJ, Kim J, Choi AH, Sun V, Chao J, Nelson R. A rising trend in the incidence of advanced gastric cancer in young Hispanic men. Gastric cancer : official journal of the International Gastric Cancer Association and the Japanese Gastric Cancer Association. 2017;20(2):226–34. https://doi.org/10.1007/s10120-016-0603-7.
Wu X, Chen VW, Andrews PA, Ruiz B, Correa P. Incidence of esophageal and gastric cancers among Hispanics, non-Hispanic whites and non-Hispanic blacks in the United States: subsite and histology differences. Cancer causes & control : CCC. 2007;18(6):585–93. https://doi.org/10.1007/s10552-007-9000-1.
Passel JS, Cohn D, H. LM. Census 2010: 50 Million Latinos, Hispanics account for more than half of nation's growth in past decade. . Washington DC: Pew Hispanic Center. 2011.
Kim J, Sun CL, Mailey B, Prendergast C, Artinyan A, Bhatia S, Pigazzi A, Ellenhorn JD. Race and ethnicity correlate with survival in patients with gastric adenocarcinoma. Annals of oncology : official journal of the European Society for Medical Oncology. 2010;21(1):152–60. https://doi.org/10.1093/annonc/mdp290.
Kanotra R, Ahmed M, Patel N, Thakkar B, Solanki S, Tareen S, Fasullo MJ, Kesavan M, Nalluri N, Khan A, Pau D, Deeb L, Abergel J, Das A. Seasonal Variations and Trends in Hospitalization for Peptic Ulcer Disease in the United States: A 12-Year Analysis of the Nationwide Inpatient Sample. Cureus. 2016;8(10):e854. https://doi.org/10.7759/cureus.854.
Acknowledgements
The authors wish to thank Harshini Chinnasamy for her assistance with data acquisition.
Author information
Authors and Affiliations
Contributions
Study conception and design: E.M. Groh, N. Hyun, B.I. Graubard, J.L. Davis.
Acquisition of data: E.M. Groh, N. Hyun.
Analysis and interpretation of data: E.M. Groh, N. Hyun, D. Check, T. Heller, B.I. Graubard, J.M. Hernandez, R.T. Ripley, J.L. Davis.
Drafting of manuscript: E.M. Groh, N. Hyun, T. Heller, R.T. Ripley, J.M. Hernandez, J.L. Davis.
Critical revisions: E.M. Groh, N. Hyun, D. Check, T. Heller, B.I. Graubard, R.T. Ripley, J.M. Hernandez, J.L. Davis.
Corresponding author
Ethics declarations
Funding
This study was supported by the Intramural Research Program, National Cancer Institute, National Institutes of Health.
Additional information
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 15 kb)
Rights and permissions
About this article
Cite this article
Groh, E.M., Hyun, N., Check, D. et al. Trends in Major Gastrectomy for Cancer: Frequency and Outcomes. J Gastrointest Surg 23, 1748–1757 (2019). https://doi.org/10.1007/s11605-018-4061-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-018-4061-x