Abstract
Background
Dichotomous models like Milan Criteria represent the routinely used tools for predicting the outcome of patients with hepatocellular carcinoma (HCC). However, a paradigm shift from a dichotomous to continuous prognostic stratification should represent a good strategy for improving the prediction process. Recently, the tumor burden score (TBS) has been proposed for selecting patients with colorectal liver metastases. To date, TBS has not been validated in a large HCC population. The main objective of this study was to evaluate the prognostic power of TBS in an HCC population treated with different curative and palliative modalities.
Methods
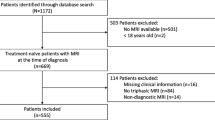
Prospectively collected data from consecutive HCC patients managed in 24 institutions participating in the ITA.LI.CA group between Jan 2002 and Mar 2015 were analyzed (n = 4759). A sub-analysis focused on 3909 patients with the radiological evidence of vascular invasion or metastatic disease was also performed.
Results
TBS demonstrated the best discriminative ability when compared to MC and other tumor-specific scores. At multivariable Cox regression analysis, TBS was an independent risk factor of overall survival, with a 6% increased risk for patient death for each point increase in TBS. At survival analysis, when TBS ≥ 8 was connected with MELD ≥ 15 and alpha-fetoprotein ≥ 1000 ng/mL, patients presenting all these three risk factors presented the worst results (p value < 0.0001).
Conclusions
Survival prediction of HCC patients was very well done using TBS model, even stratifying the population in relation to the presence of metastases and/or vascular invasion. TBS model was the best in terms of discriminatory ability and goodness of fit when compared with other continuous or binary variables. Its incorporation in a model composed by tumor- and liver function-related variables further increases its survival prediction.


Similar content being viewed by others
Abbreviations
- ABL:
-
ablation
- AFP:
-
alpha fetoprotein
- AIC:
-
Akaike information criterion
- AJCC:
-
American Joint Committee on Cancer
- BCLC:
-
Barcelona Clinic Liver Cancer
- BSC:
-
best supportive care
- CI:
-
confidence intervals
- CPS:
-
Child-Pugh score
- CT:
-
computerized tomography
- DOR:
-
diagnostic odds ratio
- ECOG PST:
-
Eastern Cooperative Oncology Group performance status
- HCC:
-
hepatocellular carcinoma
- HR:
-
hazard ratio
- IAT:
-
intra-arterial therapies
- IQR:
-
interquartile ranges
- ITA.LI.CA.:
-
Italian Liver Cancer
- LR:
-
liver resection
- LT:
-
liver transplantation
- MC:
-
Milan Criteria
- MELD:
-
model for end-stage liver disease
- MRI:
-
magnetic resonance imaging
- ROC:
-
receiver-operating curve
- SOR:
-
sorafenib
- TBS:
-
tumor burden score
- TNM:
-
tumor/node/metastasis
- TTD:
-
total tumor diameter
- TTV:
-
total tumor volume
- UCSFC:
-
University of California San Francisco Criteria
References
Mazzaferro V, Regalia E, Doci R, Andreola S, Pulvirenti A, Bozzetti F, Montalto F, Ammatuna M, Morabito A, Gennari L: Liver transplantation for the treatment of small hepatocellular carcinomas in patients with cirrhosis. N Engl J Med 1996;334:693–9.
Mazzaferro V, Bhoori S, Sposito C, Bongini M, Langer M, Miceli R, Mariani L: Milan criteria in liver transplantation for hepatocellular carcinoma: an evidence-based analysis of 15 years of experience. Liver Transpl 2011;17:S44–57.
Bruix J, Sherman M, Llovet JM, Beaugrand M, Lencioni R, Burroughs AK, Christensen E, Pagliaro L, Colombo M, Rodés J; EASL Panel of Experts on HCC: Clinical management of hepatocellular carcinoma. Conclusions of the Barcelona-2000 EASL conference. European Association for the Study of the Liver. J Hepatol 2001;35:421–30.
EASL–EORTC Clinical Practice Guidelines: Management of hepatocellular carcinoma: J Hepatol 2012;56:908–943.
Bruix J, Sherman M; American Association for the Study of Liver Diseases: Management of hepatocellular carcinoma: an update. Hepatology 2011;53:1020–2.
Vitale A, Burra P, Frigo AC, Trevisani F, Farinati F, Spolverato G, Volk M, Giannini EG, Ciccarese F, Piscaglia F, Rapaccini GL, Di Marco M, Caturelli E, Zoli M, Borzio F, Cabibbo G, Felder M, Gasbarrini A, Sacco R, Foschi FG, Missale G, Morisco F, Svegliati Baroni G, Virdone R, Cillo U; Italian Liver Cancer (ITA.LI.CA) group: Survival benefit of liver resection for patients with hepatocellular carcinoma across different Barcelona Clinic Liver Cancer stages: a multicentre study. J Hepatol 2015;62:617–24.
Toso C, Kneteman NM, James Shapiro AM, Bigam DL: The estimated number of patients with hepatocellular carcinoma selected for liver transplantation using expanded selection criteria. Transpl Int 2009;22:869–75.
Mazzaferro V, Llovet JM, Miceli R, Bhoori S, Schiavo M, Mariani L, Camerini T, Roayaie S, Schwartz ME, Grazi GL, Adam R, Neuhaus P, Salizzoni M, Bruix J, Forner A, De Carlis L, Cillo U, Burroughs AK, Troisi R, Rossi M, Gerunda GE, Lerut J, Belghiti J, Boin I, Gugenheim J, Rochling F, Van Hoek B, Majno P; Metroticket Investigator Study Group: Predicting survival after liver transplantation in patients with hepatocellular carcinoma beyond the Milan criteria: a retrospective, exploratory analysis. Lancet Oncol 2009;10:35–43.
Sasaki K, Morioka D, Conci S, Margonis GA, Sawada Y, Ruzzenente A, Kumamoto T, Iacono C, Andreatos N, Guglielmi A, Endo I, Pawlik TM: The Tumor Burden Score: A New "Metro-ticket" Prognostic tool for colorectal liver metastases based on tumor size and number of tumors. Ann Surg 2018;267:132–141.
Akaike’s criteria. In: Armitage P, Colton T, eds Encyclopedia of Biostatistics. Chichester: Wiley; 1998. p. 123–124.
Rodriguez JD, Perez A, Lozano JA. Sensitivity analysis of k-fold cross validation in prediction error estimation. IEEE Trans Pattern Anal Mach Intell 2010;32:569–575.
Shah SA, Tan JC, McGilvray ID, Cattral MS, Cleary SP, Levy GA, Greig PD, Grant DR: Accuracy of staging as a predictor for recurrence after liver transplantation for hepatocellular carcinoma. Transplantation 2006;81:1633–9.
Lee DH, Lee JM, Baek JH, Shin CI, Han JK, Choi BI: Diagnostic performance of gadoxetic acid-enhanced liver MR imaging in the detection of HCCs and allocation of transplant recipients on the basis of the Milan criteria and UNOS guidelines: correlation with histopathologic findings. Radiology 2015;274:149–60.
Royston P, Altman DG, Sauerbrei W: Dichotomizing continuous predictors in 18 multiple regression: a bad idea. Stat Med. 2006 Jan 15;25(1):127–41.
Mazzaferro V: Results of liver transplantation: with or without Milan criteria? Liver Transpl 2007;13:S44–7.
Yao FY, Ferrell L, Bass NM, Watson JJ, Bacchetti P, Venook A, Ascher NL, Roberts JP: Liver transplantation for hepatocellular carcinoma: expansion of the tumor size limits does not adversely impact survival. Hepatology 2001;33:1394–403.
Lai Q, Avolio AW, Manzia TM, Sorge R, Agnes S, Tisone G, Berloco PB, Rossi M: Combination of biological and morphological parameters for the selection of patients with hepatocellular carcinoma waiting for liver transplantation. Clin Transplant 2012;26:E125–31.
Toso C, Trotter J, Wei A, Bigam DL, Shah S, Lancaster J, Grant DR, Greig PD, Shapiro AM, Kneteman NM: Total tumor volume predicts risk of recurrence following liver transplantation in patients with hepatocellular carcinoma. Liver Transpl 2008;14:1107–15.
Toso C, Meeberg G, Hernandez-Alejandro R, Dufour JF, Marotta P, Majno P, Kneteman NM: Total tumor volume and alpha-fetoprotein for selection of transplant candidates with hepatocellular carcinoma: A prospective validation. Hepatology 2015;62:158–65.
Sasaki K, Firl DJ, Hashimoto K, Fujiki M, Diago-Uso T, Quintini C, Eghtesad B, Fung JJ, Aucejo FN, Miller CM: Development and validation of the HALT-HCC score to predict mortality in liver transplant recipients with hepatocellular carcinoma: a retrospective cohort analysis. Lancet Gastroenterol Hepatol 2017;2:595–603.
Farinati F, Vitale A, Spolverato G, Pawlik TM, Huo TL, Lee YH, Frigo AC, Giacomin A, Giannini EG, Ciccarese F, Piscaglia F, Rapaccini GL, Di Marco M, Caturelli E, Zoli M, Borzio F, Cabibbo G, Felder M, Sacco R, Morisco F, Biasini E, Foschi FG, Gasbarrini A, Svegliati Baroni G, Virdone R, Masotto A, Trevisani F, Cillo U; ITA.LI.CA study group: Development and Validation of a New Prognostic System for Patients with Hepatocellular Carcinoma. PLoS Med 2016;13:e1002006.
Lerut J, Lai Q: Morphology does not tell us the entire story: biological behavior improves our ability to select patients with hepatocellular carcinoma waiting for liver transplantation. Hepatobiliary Pancreat Dis Int 2015;14:570–1.
Cillo U, Vitale A, Bassanello M, Boccagni P, Brolese A, Zanus G, Burra P, Fagiuoli S, Farinati F, Rugge M, D'Amico DF: Liver transplantation for the treatment of moderately or well-differentiated hepatocellular carcinoma. Ann Surg 2004;239:150–9.
Mehta N, Dodge JL, Goel A, Roberts JP, Hirose R, Yao FY: Identification of liver transplant candidates with hepatocellular carcinoma and a very low dropout risk: implications for the current organ allocation policy. Liver Transpl 2013;19:1343–53.
Duvoux C, Roudot-Thoraval F, Decaens T, Pessione F, Badran H, Piardi T, Francoz C, Compagnon P, Vanlemmens C, Dumortier J, Dharancy S, Gugenheim J, Bernard PH, Adam R, Radenne S, Muscari F, Conti F, Hardwigsen J, Pageaux GP, Chazouillères O, Salame E, Hilleret MN, Lebray P, Abergel A, Debette-Gratien M, Kluger MD, Mallat A, Azoulay D, Cherqui D; Liver Transplantation French Study Group: Liver transplantation for hepatocellular carcinoma: a model including α-fetoprotein improves the performance of Milan criteria. Gastroenterology 2012;143:986–94.
Lai Q, Avolio AW, Graziadei I, Otto G, Rossi M, Tisone G, Goffette P, Vogel W, Pitton MB, Lerut J; European Hepatocellular Cancer Liver Transplant Study Group: Alpha-fetoprotein and modified response evaluation criteria in solid tumors progression after locoregional therapy as predictors of hepatocellular cancer recurrence and death after transplantation. Liver Transpl 2013;19:1108–18.
Lai Q, Castro Santa E, Rico Juri JM, Pinheiro RS, Lerut J: Neutrophil and platelet-to-lymphocyte ratio as new predictors of dropout and recurrence after liver transplantation for hepatocellular cancer. Transpl Int 2014;27:32–41.
Acknowledgements
Other members of the ITA.LI.CA group
Dipartimento di Scienze Mediche e Chirurgiche, Alma Mater Studiorum-Università di Bologna: Maurizio Biselli, Laura Bucci, Paolo Caraceni, Alessandro Cucchetti, Marco Domenicali, Chiara Faggiano, Francesca Garuti, Annagiulia Gramenzi, Alessandro Granito, Donatella Magalotti, Giulia Negrini, Fabio Piscaglia, Matteo Ravaioli, Carla Serra, Francesco Tovoli, Federico Ravaioli, Giovanni Marasco; Dipartimento di Scienze Chirurgiche e Gastroenterologiche, Università di Padova: Giulia Peserico, Filippo Pelizzaro, Paola Todesca, Caterina Pozzan; Dipartimento di Medicina Interna, Unità di Gastroenterologia, IRCCS-Azienda Ospedaliera Universitaria San Martino-IST, Università di Genova: Matteo Brunacci, Alessandro Moscatelli, Gaia Pellegatta, Vincenzo Savarino; Unità Operativa di Chirurgia, Policlinico S. Marco, Zingonia: Paolo Del Poggio, Stefano Olmi; Unità di Medicina Interna e Gastroenterologia, Complesso Integrato Columbus, Università Cattolica di Roma, Roma: Nicoletta de Matthaeis; Unità Operativa di Medicina, Azienda Ospedaliera Bolognini, Seriate, Italia: Claudia Balsamo, Elena Vavassori; Unità Operativa di Gastroenterologia, Ospedale Belcolle, Viterbo: Paola Roselli, Valentina Lauria, Giorgio Pelecca; Unità Operativa di Medicina Protetta, Ospedale Belcolle, Viterbo: Serena Dell’Isola, Anna Maria Ialungo, Elena Rastrelli; Dipartimento Biomedico di Medicina Interna e Specialistica, Unità di Gastroenterologia, Università di Palermo: Calogero Cammà, Marcello Maida, Andrea Costantino; Dipartimento Biomedico di Medicina Interna e Specialistica, Unità di Medicina Interna 2, Azienda Ospedaliera Ospedali Riuniti Villa Sofia-Cervello, Palermo: Andrea Affronti-Emanuele Orlando-Maria Rosa Barcellona; Ospedale Regionale di Bolzano, Unità di Gastroenterologia, Bolzano: Andrea Mega; Unità di Medicina Interna e Gastroenterologia, Policlinico Gemelli, Università Cattolica di Roma, Roma: Emanuele Rinninella; Unità Operativa Gastroenterologia e Malattie del Ricambio, Azienda Ospedaliero-Universitaria Pisana, Pisa: Valeria Mismas; Dipartimento di Medicina Interna, Ospedale per gli Infermi di Faenza, Faenza: Anna Chiara Dall’Aglio, Vittoria Bevilacqua, Andrea Casadei Gardini, Giorgio Ercolani, Erica Fiorini, Arianna Lanzi, Federica Mirici Cappa; Unità di Malattie Infettive ed. Epatologia, Azienda Ospedaliero-Universitaria di Parma: Elisabetta Biasini, Andrea Olivani; Dipartimento di Medicina Clinica e Chirurgia, Unità di Gastroenterologia, Università di Napoli “Federico II”, Napoli: Maria Guarino; Clinica di Gastroenterologia, Università Politecnica delle Marche, Ancona: Alessio Ortolani, Alba Kostandini; Unità di Gastroenterologia, Ospedale Sacro Cuore Don Calabria, Negrar: Maria Chiaramonte, Fabiana Marchetti, Matteo Valerio; Dipartimento di Medicina Diagnostica e Prevenzione, Azienda ospedaliero-universitaria di Bologna, Unità Operativa di Radiologia: Alberta Cappelli, Rita Golfieri, Cristina Mosconi, Matteo Renzulli; Dipartimento di Medicina Clinica e Chirurgia, Unità di Epato-Gastroenterologia, Università di Napoli “Federico II”, Napoli: Piero Coccoli, Marco Sanduzzi Zamparelli; Medicina Interna ed. Epatologia, Dipartimento di Medicina Sperimentale e Clinica–Università di Firenze, Firenze: Andrea Lorenzo Inghilesi, Sami Aburas.
Contributors
AV, QL, FT, and TMP were responsible for the conception, design and analysis of the study, and for editing the final report; AV, QL, FT, and TMP wrote the paper; FF, LB, EGG, LN, FC, GLR, MDM, EC, MZ, FB, RS, GC, RV, FM, MF, FM, LB, AG, GSB, FGF, GM, AM, GN, AC, and MB were involved with the collection and interpretation of data; FF, LB, EGG, LN, FC, GLR, MDM, EC, MZ, FB, RS, GC, RV, FM, MF, FM, LB, AG, GSB, FGF, GM, AM, GN, AC, and MB participated in data management and manuscript review.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
The Institutional Review Board of the participating institutions approved the study. Informed consent was obtained as usual in clinical, surgical, and radiological practice. Patients gave written consent for procedures performed including use of data for medical and research purposes.
Conflict of Interest
The authors declare that they have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Vitale, A., Lai, Q., Farinati, F. et al. Utility of Tumor Burden Score to Stratify Prognosis of Patients with Hepatocellular Cancer: Results of 4759 Cases from ITA.LI.CA Study Group. J Gastrointest Surg 22, 859–871 (2018). https://doi.org/10.1007/s11605-018-3688-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-018-3688-y