Abstract
Background
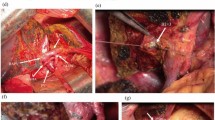
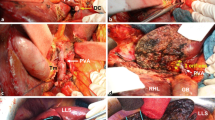
“Hilar en bloc resection” using a no-touch technique has been advocated as a standard procedure in right-sided hepatectomies for treatment of perihilar cholangiocarcinoma (PHC). In principle, it has never been reported for left-sided tumors. The aim is to describe the procedures of total hilar en bloc resection with left hemihepatectomy and caudate lobectomy (THER-LH) for advanced PHC and discuss feasibility and clinical significance of this novel technique.
Methods
A retrospective study using a prospectively maintained database was performed to identify eight patients who had received THER-LH for advanced PHC from January 2013 to December 2015. The clinicopathological features, surgical procedures, and outcomes of these patients form the basis this study.
Results
The operative time was 546 ± 158 (380–870) min, and estimated blood loss was 875 ± 690 (400–2500) ml. Time of vessel resection and reconstruction was 25.6 ± 12.3 min for the portal vein and 19.1 ± 4.9 min for the hepatic artery. Time of hilum clamping was 27.3 ± 11.9 (15–41) min. Two patients had Clavien-Dindo grade II and IVa complications of bile leakage with one developing intraabdominal abscess and bleeding. There was no perioperative mortality. Histopathologic examination revealed that all of eight patients had tubular adenocarcinoma with microscopic invasion to the resected hepatic arteries and portal veins in seven patients. Negative bile duct margins were achieved in all of them. Three patients developed recurrence and died at 11, 18, and 24 months postoperatively. The remaining patients were alive at the time of last follow-up. The median survival was 24 months with one patient achieving a disease-free survival of 50 months.
Conclusion
THER-LH is a technically demanding procedure that is safe and feasible that may have some beneficial effects on the prognosis of these patients with advanced PHC. Further studies are required to confirm the oncological superiority and survival benefits of this novel technique.





Similar content being viewed by others
References
Abbas S, Sandroussi C. Systematic review and meta-analysis of the role of vascular resection in the treatment of hilar cholangiocarcinoma. HPB : the official journal of the International Hepato Pancreato Biliary Association. 2013;15(7):492–503.
Gerhards MF, van Gulik TM, de Wit LT, Obertop H, Gouma DJ. Evaluation of morbidity and mortality after resection for hilar cholangiocarcinoma—a single center experience. Surgery. 2000;127(4):395–404.
Hemming AW, Mekeel K, Khanna A, Baquerizo A, Kim RD. Portal vein resection in management of hilar cholangiocarcinoma. Journal of the American College of Surgeons. 2011;212(4):604–613; discussion 613-606.
Ota T, Araida T, Yamamoto M, Takasaki K. Operative outcome and problems of right hepatic lobectomy with pancreatoduodenectomy for advanced carcinoma of the biliary tract. Journal of hepato-biliary-pancreatic surgery. 2007;14(2):155–158.
Miyazaki M, Kato A, Ito H, et al. Combined vascular resection in operative resection for hilar cholangiocarcinoma: does it work or not? Surgery. 2007;141(5):581–588.
Hidalgo E, Asthana S, Nishio H, et al. Surgery for hilar cholangiocarcinoma: the Leeds experience. European journal of surgical oncology : the journal of the European Society of Surgical Oncology and the British Association of Surgical Oncology. 2008;34(7):787–794.
Konstadoulakis MM, Roayaie S, Gomatos IP, et al. Aggressive surgical resection for hilar cholangiocarcinoma: is it justified? Audit of a single center’s experience. American journal of surgery. 2008;196(2):160–169.
Sakamoto Y, Sano T, Shimada K, et al. Clinical significance of reconstruction of the right hepatic artery for biliary malignancy. Langenbeck's archives of surgery / Deutsche Gesellschaft fur Chirurgie. 2006;391(3):203–208.
Nagino M, Nimura Y, Nishio H, et al. Hepatectomy with simultaneous resection of the portal vein and hepatic artery for advanced perihilar cholangiocarcinoma: an audit of 50 consecutive cases. Annals of surgery. 2010;252(1):115–123.
Neuhaus P, Jonas S, Bechstein WO, et al. Extended resections for hilar cholangiocarcinoma. Annals of surgery. 1999;230(6):808–818; discussion 819.
Neuhaus P, Thelen A, Jonas S, et al. Oncological superiority of hilar en bloc resection for the treatment of hilar cholangiocarcinoma. Annals of surgical oncology. 2012;19(5):1602–1608.
Govil S, Reddy MS, Rela M. Surgical resection techniques for locally advanced hilar cholangiocarcinoma. Langenbeck's archives of surgery / Deutsche Gesellschaft fur Chirurgie. 2014;399(6):707–716.
Hirano S, Kondo S, Tanaka E, Shichinohe T, Tsuchikawa T, Kato K. No-touch resection of hilar malignancies with right hepatectomy and routine portal reconstruction. Journal of hepato-biliary-pancreatic surgery. 2009;16(4):502–507.
Tamoto E, Hirano S, Tsuchikawa T, et al. Portal vein resection using the no-touch technique with a hepatectomy for hilar cholangiocarcinoma. HPB : the official journal of the International Hepato Pancreato Biliary Association. 2014;16(1):56–61.
Belghiti J, Guevara OA, Noun R, Saldinger PF, Kianmanesh R. Liver hanging maneuver: a safe approach to right hepatectomy without liver mobilization. Journal of the American College of Surgeons. 2001;193(1):109–111.
Edge SB BD, Compton CC, et al. Perihilar bile ducts. In: AJCC Cancer Staging Handbook. 7th ed. Chicago, IL: Springer; 2010:718.
Dindo D, Demartines D, Clavien PA. Classification of Surgical Complications A New Proposal With Evaluation in a Cohort of 6336 Patients and Results of a Survey. Ann Surg. 2004;240(2): 205–213.
Koch M, Garden OJ, Padbury R, et al. Bile leakage after hepatobiliary and pancreatic surgery: A definition and grading of severity by the International Study Group of Liver Surgery. Surgery 2011;149(5):680–688.
Ebata T, Nagino M, Kamiya J, Uesaka K, Nagasaka T, Nimura Y. Hepatectomy with portal vein resection for hilar cholangiocarcinoma: audit of 52 consecutive cases. Annals of surgery. 2003;238(5):720–727.
Miyazaki M, Kimura F, Shimizu H, et al. Recent advance in the treatment of hilar cholangiocarcinoma: hepatectomy with vascular resection. Journal of hepato-biliary-pancreatic surgery. 2007;14(5):463–468.
Ebata T, Ito T, Yokoyama Y et al. Surgical technique of hepatectomy combined with simultaneous resection of hepatic artery and portal vein for perihilar cholangiocarcinoma (with video) J Hepatobiliary Pancreat Sci June 2014; 21:E57–E61.
Smyrniotis V, Farantos C, Kostopanagiotou G, Arkadopoulos N. Vascular control during hepatectomy: review of methods and results. World journal of surgery. 2005;29(11):1384–1396.
Midorikawa Y, Kubota K, Takayama T, et al. A comparative study of postoperative complications after hepatectomy in patients with and without chronic liver disease. Surgery. 1999;126(3):484–491.
Smyrniotis VE, Kostopanagiotou GG, Contis JC, et al. Selective hepatic vascular exclusion versus Pringle maneuver in major liver resections: prospective study. World journal of surgery. 2003;27(7):765–769.
House MG, D’Angelica MI, Jarnagin R. Cancer of the bile ducts: extrahepatic biliary tumors. In: Blumgart’s Surgery of the Liver, Biliary Tract, and Pancreas. 5th ed. Philadelphia, PA:Elsevier; 2012:783.
Acknowledgements
The authors are grateful to Yu Xi for her assistance in preparing the manuscript.
Funding
The Scientific Innovation Team Project of Ningbo (Fund Number 2013B82010)
Author information
Authors and Affiliations
Corresponding author
Additional information
Synopsis
We described our technique of total hilar en bloc resection with left hemihepatectomy and caudate lobectomy for eight patients with advanced PHC and discussed its feasibility. It is a technically demanding procedure that is safe and feasible and may have some beneficial effects on the prognosis of these patients.
Rights and permissions
About this article
Cite this article
De Lu, C., Huang, J., Wu, S.D. et al. Total Hilar En Bloc Resection with Left Hemihepatectomy and Caudate Lobectomy: a Novel Approach for Treatment of Left-Sided Perihilar Cholangiocarcinoma (with Video). J Gastrointest Surg 21, 1906–1914 (2017). https://doi.org/10.1007/s11605-017-3561-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-017-3561-4