Abstract
Background
Small-bowel obstruction is a frequent disorder in emergency medicine and represents a major burden for patients and health care systems worldwide. Within the past years, progress has been made regarding the management of small-bowel obstructions, including the use of contrast agent swallow as a tool in the decision-making process.
Objectives
This is a prospective controlled study investigating the central role of contrast agent swallow in the diagnostic and treatment algorithm for small-bowel obstruction at a university department of surgery. Endpoints were the correct identification of patients who needed operative treatment and the accuracy of a conservative treatment decision including the analysis of dropout from this routine algorithm.
Methods
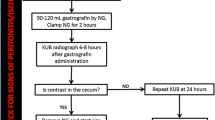
We performed a single-center analysis of 181 consecutive patients diagnosed with a small-bowel obstruction based on clinical, radiologic, and sonographic findings. Patients with clinical signs of strangulation or peritonitis underwent immediate surgery (group 1). Patients without signs of peritonitis and incomplete stop in the initial abdominal plain film were considered eligible for Gastrografin® challenge (group 2).
Results
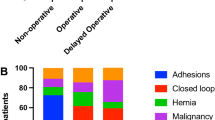
Seventy-six of the 181 patients (42.0%) underwent immediate surgery. A Gastrografin® challenge was initialized in 105 of the 181 patients (58.0%). Twenty of these 105 patients (19.1%) with persisting or progressive symptoms and absence of contrast agent in the colon after 12 and 24 h subsequently underwent surgery. Here, a segmental bowel resection was necessary in 6 of these 20 patients (30.0%). In 16 out of 20 patients (80.0%) who failed the Gastrografin® challenge, a corresponding correlate in terms of a strangulation was detected intraoperatively. The Gastrografin® challenge had a specificity of 96% and a sensitivity of 100%; accuracy to predict the need for exploration was 96%.
Conclusion
A straightforward algorithm based mainly on contrast agent swallow for patients with small-bowel obstructions enabled a timely and very accurate differentiation between patients qualifying for conservative and operative treatment.



Similar content being viewed by others
References
Ray NF, Denton WG, Thamer M, Henderson SC, Perry S. Abdominal adhesiolysis: inpatient care and expenditures in the United States in 1994. J Am Coll Surg. 1998; 186: 1Y9.
Branco BC, Barmparas G, Schnüriger B, Inaba K, Chan LS, Demetriades D. Systematic review and meta-analysis of the diagnostic and therapeutic role of water-soluble contrast agent in adhesive small bowel obstruction. Br J Surg 2010; 97: 470–478.
Seror D, Feigin E, Szold A, Allweis TM, Carmon M, Nissan S, Freund HR. How conservatively can postoperative small bowel obstruction be treated? Am J Surg. 1993; 165: 121–125.
Fevang BT, Fevang J, Stangeland L, Soreide O, Svanes K, Viste A. Complications and death after surgical treatment of small bowel obstruction: a 35-year institutional experience. Ann Surg. 2000; 231: 529–537.
HK Choi, Chu KW, Law WL. Therapeutic value of Gastrografin in adhesive small bowel obstruction after unsuccessful conservative treatment: a prospective randomized trial. Ann Surg. 2002; 236: 1–6.
Goussous N, Eiken PW, Bannon MP, Zielinski MD. Enhancement of a small bowel obstruction model using the gastrografin® challenge test. J Gastrointest Surg. 2013;17: 110–116.
Di Saverio S, Catena F, Ansaloni L, Gavioli M, Valentino M, et al. Water soluble contrast medium (gastrografin) value in adhesive small intestine obstruction (ASIO): a prospective randomised controlled clinical trial. World J Surg. 2008; 32: 2293–2304.
Assalia A, Kopelman D, Bahous H, Klein Y, Hashmonai M. Gastrografin for mechanical partial, small bowel obstruction due to adhesions. Harefuah. 1997; 132: 629–633.
Bass KN, Jones B, Bulkley GB. Current management of small-bowel obstruction. Adv Surg. 1997; 31:1–34.
Assalia A, Schein M, Kopelman D, Hirshberg A, Hashmonai M. Therapeutic effect of oral Gastrografin in adhesive, partial small-bowel obstruction: a prospective randomized trial. Surgery. 1994; 115: 433–437.
Biondo S, Pares D, Mora L, Martí Ragué J, Kreisler E, Jaurrieta E. Randomized clinical study of gastrografin administration in patients with adhesive small bowel obstruction. Br J Surg. 2003; 90: 542–546.
Abbas SM, Bissett IP, Parry BR. Meta-analysis of oral water-soluble contrast agent in the management of adhesive small bowel obstruction. Br J Surg. 2007; 94: 404–411.
Taylor MR, Lalani N. Adult small bowel obstruction. Acad Emerg Med. 2013; 20: 528–44.
Sheedy SP, Earnest F IV, Fletcher JG, Fidler JL, Hoskin TL. CT of small-bowel ischemia associated with obstruction in emergency department patients: diagnostic performance evaluation. Radiology 2006; 241: 729–736.
Klar E, Rahmanian PB, Bücker A, Hauenstein K, Jauch KW, Luther B. Acute mesenteric ischemia: a vascular emergency. Dtsch Arztebl Int. 2012; 109: 249–56.
Bickell NA, Federman AD, Aufses AH Jr. Influence of time on risk of bowel resection in complete small bowel obstruction. J Am Coll Surg. 2005; 201: 847Y854.
Acknowledgements
We would like to thank Robin Vasan, M.D., Research Fellow at the Massachusetts General Hospital in Boston for the language revision of the manuscript.
Author information
Authors and Affiliations
Contributions
Kuehn F analyzed and interpreted data and drafted the manuscript. Klar E and Weinrich M have done substantial contributions to conception and design of the study. Ehmann S has collected and analyzed data. Pergolini I helped to perform statistical analysis. Kloker K helped to collect and analyze data. Klar E has revised the article critically for important intellectual content; the article has been approved to be published by all authors.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Kuehn, F., Weinrich, M., Ehmann, S. et al. Defining the Need for Surgery in Small-Bowel Obstruction. J Gastrointest Surg 21, 1136–1141 (2017). https://doi.org/10.1007/s11605-017-3418-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-017-3418-x