Abstract
Background
Randomized studies indicated that 88–95 % of patients with acute appendicitis recover on antibiotics without surgery, although it is unclear which patient would benefit with high probability on antibiotics. We hypothesized that patients with phlegmonous appendicitis should be a group where antibiotics may be a sufficient treatment. Accordingly, our aim was to propose a model to support treatment application for unselected patients with acute appendicitis.
Methods
Retrospective analyses of preoperative clinical and laboratory variables in 384 consecutive adult patients, who underwent appendectomy with histological examination of the appendix, were evaluated by logistic regressions. The proposed mathematical model was then evaluated on a prospectively collected population based material of 581 consecutive patients offered antibiotics as their first line treatment of acute appendicitis.
Results
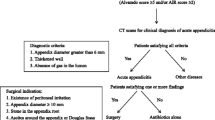
Patients with assumed appendicitis who fulfilled all criteria with CRP <60 g/L, WCC <12 × 109/L, and age <60 years had 89 % probability to have phlegmonous appendicitis. When these criteria were applied retrospectively on a prospective material, 88 % of operated patients had phlegmonous inflammation and 89 % had recovered on antibiotics without surgery.
Conclusion
Standard clinical and laboratory tests are individually weak predictors of phlegmonous appendicitis, but can be used in combinations as a bedside instrument to select patients suitable for antibiotic therapy.

Similar content being viewed by others
References
Tingstedt B, Johansson J, Nehez L, Andersson R. Late abdominal complaints after appendectomy–readmissions during long-term follow-up. Digestive surgery. 2004;21:23–7.
Andersson RE. Small bowel obstruction after appendicectomy. The British journal of surgery. 2001;88:1387–91.
Blomqvist PG, Andersson RE, Granath F, Lambe MP, Ekbom AR. Mortality after appendectomy in Sweden, 1987–1996. Annals of surgery. 2001;233:455–60.
Andersson RE. The natural history and traditional management of appendicitis revisited: spontaneous resolution and predominance of prehospital perforations imply that a correct diagnosis is more important than an early diagnosis. World journal of surgery. 2007;31:86–92.
Liu K, Ahanchi S, Pisaneschi M, Lin I, Walter R. Can acute appendicitis be treated by antibiotics alone? The American surgeon. 2007;73:1161–5.
Varadhan KK, Humes DJ, Neal KR, Lobo DN. Antibiotic therapy versus appendectomy for acute appendicitis: a meta-analysis. World J Surg. 2009;34:199–209.
Styrud J, Eriksson S, Nilsson I, Ahlberg G, Haapaniemi S, Neovius G, Rex L, Badume I, Granstrom L. Appendectomy versus antibiotic treatment in acute appendicitis. a prospective multicenter randomized controlled trial. World journal of surgery. 2006;30:1033–7.
Hansson J, Korner U, Khorram-Manesh A, Solberg A, Lundholm K. Randomized clinical trial of antibiotic therapy versus appendicectomy as primary treatment of acute appendicitis in unselected patients. The British journal of surgery. 2009;96:473–81.
Andersson RE, Hugander AP, Ghazi SH, Ravn H, Offenbartl SK, Nystrom PO, Olaison GP. Diagnostic value of disease history, clinical presentation, and inflammatory parameters of appendicitis. World journal of surgery. 1999;23:133–40.
Andersson R, Hugander A, Thulin A, Nystrom PO, Olaison G. Indications for operation in suspected appendicitis and incidence of perforation. BMJ. 1994;308:107–10.
Kraemer M, Kremer K, Leppert R, Yang Q, Ohmann C, Fuchs KH. Perforating appendicitis: is it a separate disease? Acute Abdominal Pain Study Group. The European journal of surgery = Acta chirurgica. 1999;165:473–80.
Carr NJ. The pathology of acute appendicitis. Annals of diagnostic pathology. 2000;4:46–58.
Hansson J, Korner U, Ludwigs K, Johnsson E, Jonsson C, Lundholm K. Antibiotics as first-line therapy for acute appendicitis: evidence for a change in clinical practice. World journal of surgery. 2012;36:2028–36.
Lamps LW. Appendicitis and infections of the appendix. Seminars in diagnostic pathology. 2004;21:86–97.
Andersson R, Hugander A, Thulin A, Nystrom PO, Olaison G. Clusters of acute appendicitis: further evidence for an infectious aetiology. International journal of epidemiology. 1995;24:829–33.
Lau WY, Teoh-Chan CH, Fan ST, Yam WC, Lau KF, Wong SH. The bacteriology and septic complication of patients with appendicitis. Annals of surgery. 1984;200:576–81.
Bennion RS, Baron EJ, Thompson JE, Jr., Downes J, Summanen P, Talan DA, Finegold SM. The bacteriology of gangrenous and perforated appendicitis–revisited. Annals of surgery. 1990;211:165–71.
Baron EJ, Bennion R, Thompson J, Strong C, Summanen P, McTeague M, Finegold SM. A microbiological comparison between acute and complicated appendicitis. Clinical infectious diseases : an official publication of the Infectious Diseases Society of America. 1992;14:227–31.
Gronroos JM, Gronroos P. Leucocyte count and C-reactive protein in the diagnosis of acute appendicitis. The British journal of surgery. 1999;86:501–4.
Korner H, Soreide JA, Sondenaa K. Diagnostic accuracy of inflammatory markers in patients operated on for suspected acute appendicitis: a receiver operating characteristic curve analysis. The European journal of surgery = Acta chirurgica. 1999;165:679–85.
Acknowledgments
This study is supported by grants from Region Västra Götaland, Gothenburg Medical Society, the Swedish government (LUA-ALF).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hansson, J., Khorram-Manesh, A., Alwindawe, A. et al. A Model to Select Patients Who May Benefit from Antibiotic Therapy as the First Line Treatment of Acute Appendicitis at High Probability. J Gastrointest Surg 18, 961–967 (2014). https://doi.org/10.1007/s11605-013-2413-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-013-2413-0