Abstract
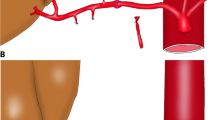
Arterial revascularization during liver transplantation is normally achieved by anastomosing the graft hepatic artery to the largest artery available at the recipient pedicle—either the common hepatic artery (CHA) or an accessory right hepatic artery (RHA) originating from the superior mesenteric artery (SMA). When a small caliber RHA is present, the artery is ligated and a single anastomosis with the CHA is performed. In the absence of a vascular reconstruction of the graft, the gastroduodenal artery is usually ligated as well. In this article, we describe a new type of arterial anastomosis in the case of a small accessory RHA and/or severe graft hepatic artery atherosclerosis that is commonly seen in elderly donors. To our knowledge, these are the first cases reported in the literature. This technique can be easily performed without increasing the arterial revascularization time or increasing the risk of complications associated with arteriosclerotic arteries. A 12-month follow-up revealed excellent function of the liver grafts.



Similar content being viewed by others
References
Pakosz-Golanowsha M, Lubikowski J, Post M, Jarosz K, Zasada-Cedro K, Milkiewicz P, Wójcicki M. The arterial anastomosis in liver transplantation: complications, treatment and outcome. Hepatogastroenterology. 2010 Nov-Dec;57(104):1477–82.
Maluf D, Clark BD, Cotterell AH, Posner MP, Fisher RA.Massive hepatic artery atherosclerosis of an otherwise suitable donor liver: a case report. Transplant Proc. 2004 Jun;36(5):1438–41.
Stange BJ, Glanemann M, Nuessler NC, Settmacher U, Steinmüller T, Neuhaus P. Hepatic artery thrombosis after adult liver transplantation. Liver Transpl. 2003 Jun;9(6):612–20.
Michels NA. Newer anatomy of the liver and its variant blood supply and collateral circulation. Am J Surg. 1966 Sep;112(3):337–47.
Silva MA, Jambulingam PS, Gunson BK, Mayer D, Buckels JA, Mirza DF, Bramhall SR. Hepatic artery thrombosis following orthotopic liver transplantation: a 10-year experience from a single centre in the United Kingdom. Liver Transpl. 2006 Jan;12(1):146–51.
Omori S, Ishizaki Y, Sugo H, Yoshimoto J, Imamura H, Yamataka A, Kawasaki S. Direct measurement of hepatic blood flow during living donor liver transplantation in children. J Pediatr Surg. 2010 Mar;45(3):545–8.
Aoki T, Imamura H, Kaneko J, Sakamoto Y, Matsuyama Y, Kokudo N, Sugawara Y, Makuuchi M. Intraoperative direct measurement of hepatic arterial buffer response in patients with or without cirrhosis. Liver Transpl. 2005 Jun;11(6):684–91.
Panaro F, Bouyabrine H, Carabalona JP, Marchand JP, Jaber S, Navarro F. Hepatic artery kinking during liver transplantation: survey and prospective intraoperative flow measurement. J Gastrointest Surg. 2012 Aug;16(8):1524–30.
Panaro F, Gallix B, Bouyabrine H, Ramos J, Addeo P, Testa G, Carabalona JP, Pageaux G, Domergue J, Navarro F. Liver transplantation and spontaneous neovascularization after arterial thrombosis: "the neovascularized liver". Transpl Int. 2011 Sep;24(9):949–57.
Ishigami K. Does variant hepatic artery anatomy in a liver transplant recipient increase the risk of hepatic artery complications after transplantation?. AJR Am J Roentgenol, 2004 Dec;183(6):1577–84.
Kornasiewicz O, Dudek K, Lewandowski Z, Grat ZM, Scibisz A, Nyckowski P, Krawczyk M. Low incidence of hepatic artery thrombosis after hepatic artery reconstruction during liver transplantation. Transplant Proc. 2009 Oct;41(8):3138–40.
Yaprak O, Demirbas T, Duran C, Dayangac M, Akyildiz M, Tokat Y, Yuzer Y. Living donor liver hilar variations: surgical approaches and implications. Hepatobiliary Pancreat Dis Int. 2011 Oct;10(5):474–9.
Conflict of interest
The authors of this manuscript have no conflicts of interest to disclose.
Funding
The authors have declared no funding.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Panaro, F., Chauvat, J., Carabalona, JP. et al. Double Arterial Anastomosis in Liver Transplantation: Is Two Better than One?. J Gastrointest Surg 17, 1512–1515 (2013). https://doi.org/10.1007/s11605-013-2154-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-013-2154-0