Abstract
Background
Thus far, no ideal substitutions have been developed for completely replacing the extrahepatic bile duct (EHBD).
Methods
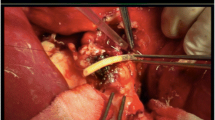
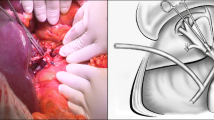
We used a bioabsorbable polymer tube (BAPT) for the complete reconstruction of an EHBD in pigs. A 2-cm-long EHBD was resected from the duodenal side, and a 4-cm-long BAPT graft was implanted at that site. The animals were re-laparotomized at 1 or 4 months after the grafting; subsequently, gross, histological, and blood chemical studies were performed.
Results
At 1 month after grafting, tubular structure was observed in all resected specimens, and the lumen of the graft site had remnants of degraded BAPT. Gross examination at 4 months after grafting revealed that the BAPT had been completely absorbed, and the graft site was indistinguishable from the native extrahepatic bile duct. The lengths of the graft region at 4 months were 70% of the replaced BAPT. Simultaneously performed histological examination revealed the growth of a neo-bile duct at the graft site, with an epithelium identical to that of the native bile duct.
Conclusion
The BAPT graft implanted in this study completely replaced the EHBD defect. Hence, BAPT has the potential for application as a novel treatment modality for hepatobiliary diseases.







Similar content being viewed by others
References
Lillemoe KD, Melton GB, Cameron JL, Pitt HA, Campbell KA, Talamini MA, Sauter PA, Coleman J, Yeo CJ. Postoperative bile duct strictures: management and outcome in the 1990s. Ann Surg. 2000;232:430–441.
Shah SA, Grant DR, McGilvray ID, Greig PD, Selzner M, Lilly LB, Girgrah N, Levy GA, Cattral MS. Biliary strictures in 130 consecutive right lobe living donor liver transplant recipients: results of a Western center. Am J Transplant. 2007;7:161–167.
Walsh RM, Henderson JM, Vogt DP, Brown N. Long-term outcome of biliary reconstruction for bile duct injuries from laparoscopic cholecystectomies. Surgery. 2007;142:450–456; discussion 456–457
Jang JY, Kim SW, Park DJ, Ahn YJ, Yoon YS, Choi MG, Suh KS, Lee KU, Park YH. Actual long-term outcome of extrahepatic bile duct cancer after surgical resection. Ann Surg. 2005;241:77–84.
Chuang JH, Lee SY, Chen WJ, Hsieh CS, Chang NK, Lo SK. Changes in bacterial concentration in the liver correlate with that in the hepaticojejunostomy after bile duct reconstruction: implication in the pathogenesis of postoperative cholangitis. World J Surg. 2001;25:1512–1518.
Hsieh CS, Huang LT, Huang CC, Wu JJ, Chuang JH. Bacteria ascend to liver from the bilioenteric conduit after choledochojejunostomy in the cholestatic rat. Pediatr Surg Int. 2003;19:699–702.
Kurumado K, Nagai T, Kondo Y, Abe H. Long-term observations on morphological changes of choledochal epithelium after choledochoenterostomy in rats. Dig Dis Sci. 1994;39:809–820.
Bettschart V, Clayton RA, Parks RW, Garden OJ, Bellamy CO. Cholangiocarcinoma arising after biliary-enteric drainage procedures for benign disease. Gut. 2002;51:128–129.
Herba MJ, Casola G, Bret PM, Lough J, Hampson LG. Cholangiocarcinoma as a late complication of choledochoenteric anastomoses. AJR Am J Roentgenol. 1986;147:513–515.
Maeda A, Yokoi S, Kunou T, Saeki S, Murata T, Niinomi N, Uesaka K. Bile duct cancer developing 21 years after choledochoduodenostomy. Dig Surg. 2003;20:331–334.
Tocchi A, Mazzoni G, Liotta G, Lepre L, Cassini D, Miccini M. Late development of bile duct cancer in patients who had biliary-enteric drainage for benign disease: a follow-up study of more than 1,000 patients. Ann Surg. 2001;234:210–214.
Miyazawa M, Torii T, Toshimitsu Y, Okada K, Koyama I, Ikada Y. A tissue-engineered artificial bile duct grown to resemble the native bile duct. Am J Transplant. 2005;5:1541–1547.
Aikawa M, Miyazawa M, Okada K, Toshimitsu Y, Okamoto K, Akimoto N, Koyama I, Ikada Y. Development of a novel reflux-free bilioenteric anastomosis procedure by using a bioabsorbable polymer tube. J Hepatobiliary Pancreat Sci. 2010;17:284–290.
Aikawa M, Miyazawa M, Okamoto K, Toshimitsu Y, Torii T, Okada K, Akimoto N, Ohtani Y, Koyama I, Yoshito I. A novel treatment for bile duct injury with a tissue-engineered bioabsorbable polymer patch. Surgery. 2010;147:575–580.
Aydin M, Bakir B, Kosem M, Kisli E, Genccelep M. Biliary tract reconstruction with autologous rectus sheath graft—an experimental study. Hepatogastroenterology. 2005;52:1019–1022.
Belzer FO, Watts JM, Ross HB, Dunphy JE. Auto-reconstruction of the common bile duct after venous patch graft. Ann Surg. 1965;162:346–355.
Bottger T, Mann B, Pickel B, Weber W, Sorger K, Junginger T. [Animal experiment studies of pedicled small intestine transplantation as partial extrahepatic bile duct replacement]. Langenbecks Arch Chir. 1991;376:77–84.
Bandura WP, Arbulu A. Experimental replacement of the common bile duct with Teflon graft. Am Surg. 1961;27:518–524.
Christensen M, Laursen HB, Rokkjaer M, Jensen PF, Yasuda Y, Mortensen FV. Reconstruction of the common bile duct by a vascular prosthetic graft: an experimental study in pigs. J Hepatobiliary Pancreat Surg. 2005;12:231–234.
Gomez NA, Alvarez LR, Mite A, Andrade JP, Alvarez JR, Vargas PE, Tomala NE, Vivas AF, Zapatier JA. Repair of bile duct injuries with Gore-Tex vascular grafts: experimental study in dogs. J Gastrointest Surg. 2002;6:116–120.
Mendelowitz DS, Beal JM. Expanded polytetrafluoroethylene in reconstruction of the canine biliary system. Am J Surg. 1982;143:221–224.
Gomez NA, Zapatier JA, Vargas PE. Re: Small intestinal submucosa as a bioscaffold for biliary tract regeneration. Surgery. 2004;135:460.
Rosen M, Ponsky J, Petras R, Fanning A, Brody F, Duperier F. Small intestinal submucosa as a bioscaffold for biliary tract regeneration. Surgery. 2002;132:480–486.
Conflicts of Interest
We do not have any financial interests to disclose in this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Aikawa, M., Miyazawa, M., Okamoto, K. et al. An Extrahepatic Bile Duct Grafting Using a Bioabsorbable Polymer Tube. J Gastrointest Surg 16, 529–534 (2012). https://doi.org/10.1007/s11605-011-1801-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-011-1801-6