Abstract
Introduction
Despite of advances in modern surgical and intensive care treatment, perioperative mortality remains high in patients with liver cirrhosis undergoing nonhepatic general surgery. In the few existing articles, mortality was reported to be as high as 70% in patients with poor liver function (high Child or model for end-stage liver disease (MELD) score). Since data are limited, we analyzed our recent experience with cirrhotic patients undergoing emergent or elective nonhepatic general surgery at a German university hospital.
Methods
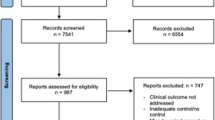
Since 2000, 138 nonhepatic general surgical procedures (99 intra-abdominal, 39 abdominal wall) were performed in patients with liver cirrhosis. Liver cirrhosis was preoperatively classified according to the Child (41 Child A, 59 B, 38 C) and the MELD score (MELD median 13). Sixty-eight (49%) of the patients underwent emergent operations. Most abdominal wall operations were for hernias. Intra-abdominal operations consisted of GI tract procedures (n = 53), cholecystectomies (n = 15), and various others (n = 31). Perioperative data were gained by retrospective analysis.
Results
Overall perioperative mortality in all 138 cases was 28% (9% in elective surgery, 47% in emergent surgery; p < 0.001). Perioperative mortality was higher after intra-abdominal than after abdominal wall operations (35% vs. 8%; p = 0.001) or in patients requiring transfusions (43% vs. 5% without transfusions; p < 0.001). Perioperative mortality increased with the Child score (10% Child A, 17% Child B, 63% Child C; p < 0.01) and the MELD score (9% MELD <10, 19% MELD 10–15, 54% MELD >15; p < 0.001). Univariately, further factors like American Society of Anesthesiologists (ASA) score and various preoperative laboratory values were also associated with perioperative mortality. By multivariate analysis of all 138 operations, the Child and ASA classifications, intraoperative transfusions, and a preoperative sodium <130 mmol/l, but not the MELD score, were independent prognostic factors.
Analysis of elective operations revealed only a preoperatively increased creatinine as risk factor for perioperative mortality. In emergent operations again, Child class, blood transfusions, and low sodium level, but not the MELD score, predicted postoperative mortality.
Conclusions
Our results demonstrate that perioperative mortality remains high in patients with liver cirrhosis undergoing general surgery, especially in emergent situations. Patients with poor liver function and/or need for blood transfusions even had a very high mortality. In our experience, the Child score (together with other variables) independently correlates with perioperative mortality in emergent operations whereas the MELD score was inferior in predicting the outcome.
Similar content being viewed by others
References
Teh, SH, Nagorney, DM, Stevens, SR, Offord, KP, Therneau, TM, Plevak, DJ, Talwalkar, JA, Kim, WR, and Kamath, PS. Risk factors for mortality after surgery in patients with cirrhosis. Gastroenterology.2007;132:1261–1269.
Rice, HE, O’Keefe, GE, Helton, WS, and Johansen, K. Morbid prognostic features in patients with chronic liver failure undergoing nonhepatic surgery. Arch Surg.1997;132:880–884.
Friedman, LS. The risk of surgery in patients with liver disease. Hepatology.1999;29:1617–1623.
Csikesz, NG, Nguyen, LN, Tseng, JF, and Shah, SA. Nationwide volume and mortality after elective surgery in cirrhotic patients. J Am Coll Surg.2009;208:96–103.
Befeler, AS, Palmer, DE, Hoffman, M, Longo, W, Solomon, H, and Di Bisceglie, AM. The safety of intra-abdominal surgery in patients with cirrhosis: model for end-stage liver disease score is superior to Child–Turcotte–Pugh classification in predicting outcome. Arch Surg.2005;140:650–654.
Farnsworth, N, Fagan, SP, Berger, DH, and Awad, SS. Child–Turcotte–Pugh versus MELD score as a predictor of outcome after elective and emergent surgery in cirrhotic patients. Am J Surg.2004;188:580–583.
Fong, Y, Sun, RL, Jarnagin, W, and Blumgart, LH. An analysis of 412 cases of hepatocellular carcinoma at a Western center. Ann Surg.1999; 229:790–799.
Belghiti, J, Regimbeau, JM, Durand, F, Kianmanesh, AR, Dondero, F, Terris, B, Sauvanet, A, Farges, O, and Degos, F. Resection of hepatocellular carcinoma: a European experience on 328 cases. Hepatogastroenterology.2002;49:41–46.
Ercolani, G, Grazi, GL, Ravaioli, M, Del Gaudio, M, Gardini, A, Cescon, M, Varotti, G, Cetta, F, and Cavallari, A. Liver resection for hepatocellular carcinoma on cirrhosis: univariate and multivariate analysis of risk factors for intrahepatic recurrence. Ann Surg.2003;237:536–543.
Rayya, F, Harms, J, Bartels, M, Uhlmann, D, Hauss, J, and Fangmann, J. Results of resection and transplantation for hepatocellular carcinoma in cirrhosis and noncirrhosis. Transplant Proc.2008;40:933–935.
Neeff, H, Makowiec, F, Harder, J, Gumpp, V, Klock, A, Thimme, R, Drognitz, O, and Hopt, UT. Hepatic resection for hepatocellular carcinoma—results and analysis of the current literature. Zentralbl Chir.2009;134:127–135.
Mansour, A, Watson, W, Shayani, V, and Pickleman, J. Abdominal operations in patients with cirrhosis: still a major surgical challenge. Surgery.1997;122:730–735.
Hoteit, MA, Ghazale, AH, Bain, AJ, Rosenberg, ES, Easley, KA, Anania, FA, and Rutherford, RE. Model for end-stage liver disease score versus Child score in predicting the outcome of surgical procedures in patients with cirrhosis. World J Gastroenterol.2008;14:1774–1780.
del Olmo, JA, Flor-Lorente, B, Flor-Civera, B, Rodriguez, F, Serra, MA, Escudero, A, Lledó, S, and Rodrigo, JM. Risk factors for nonhepatic surgery in patients with cirrhosis. World J Surg.2003;27:647–652.
Garrison, RN, Cryer, HM, Howard, DA, and Polk, HC. Clarification of risk factors for abdominal operations in patients with hepatic cirrhosis. Ann Surg.1984;199:648–655.
Suman, A, Barnes, DS, Zein, NN, Levinthal, GN, Connor, JT, and Carey, WD. Predicting outcome after cardiac surgery in patients with cirrhosis: a comparison of Child–Pugh and MELD scores. Clin Gastroenterol Hepatol.2004;2:719–723.
Child, C. G. and Turcotte, J. G. Surgery and portal hypertension. In: Child, C. G. The Liver and portal hypertension ed. Philadelphia: Saunders; 1964:50–52.
Kamath, PS, Wiesner, RH, Malinchoc, M, Kremers, W, Therneau, TM, Kosberg, CL, D’Amico, G, Dickson, ER, and Kim, WR. A model to predict survival in patients with end-stage liver disease. Hepatology.2001;33:464–470.
Keats, AS. The ASA classification of physical status—a recapitulation. Anesthesiology.1978;49:233–236.
Franzetta, M, Raimondo, D, Giammanco, M, Di Trapani, B, Passariello, P, Sammartano, A, and Di Gesù, G. Prognostic factors of cirrhotic patients in extra-hepatic surgery. Minerva Chir.2003;58:541–544.
Ziser, A, Plevak, DJ, Wiesner, RH, Rakela, J, Offord, KP, and Brown, DL. Morbidity and mortality in cirrhotic patients undergoing anesthesia and surgery. Anesthesiology.1999;90:42–53.
Northup, PG, Wanamaker, RC, Lee, VD, Adams, RB, and Berg, CL. Model for end-stage liver disease (MELD) predicts nontransplant surgical mortality in patients with cirrhosis. Ann Surg.2005;242:244–251.
O’Leary, JG and Friedman, LS. Predicting surgical risk in patients with cirrhosis: from art to science. Gastroenterology.2007;132:1609–1611.
Telem, DA, Schiano, T, Goldstone, R, Han, DK, Buch, KE, Chin, EH, Nguyen, SQ, and Divino, CM. Factors that predict outcome of abdominal operations in patients with advanced cirrhosis. Clin Gastroenterol Hepatol.2009;8(5):451–457
Schroeder, RA, Marroquin, CE, Bute, BP, Khuri, S, Henderson, WG, and Kuo, PC. Predictive indices of morbidity and mortality after liver resection. Ann Surg.2006;243:373–379.
Huo, TI, Wang, YW, Yang, YY, Lin, HC, Lee, PC, Hou, MC, Lee, FY, and Lee, SD. Model for end-stage liver disease score to serum sodium ratio index as a prognostic predictor and its correlation with portal pressure in patients with liver cirrhosis. Liver Int.2007;27:498–506.
Lv, XH, Liu, HB, Wang, Y, Wang, BY, Song, M, and Sun, MJ. Validation of model for end-stage liver disease score to serum sodium ratio index as a prognostic predictor in patients with cirrhosis. J Gastroenterol Hepatol.2009;24:1547–1553.
Kim, WR, Biggins, SW, Kremers, WK, Wiesner, RH, Kamath, PS, Benson, JT, Edwards, E, and Therneau, TM. Hyponatremia and mortality among patients on the liver-transplant waiting list. N Engl J Med.2008;359:1018–1026.
Cárdenas, A and Ginès, P. Predicting mortality in cirrhosis—serum sodium helps. N Engl J Med.2008;359:1060–1062.
O’Leary, JG, Yachimski, PS, and Friedman, LS. Surgery in the patient with liver disease. Clin Liver Dis.2009;13:211–231.
Adam, U, Makowiec, F, Riediger, H, Keck, T, Kröger, JC, Uhrmeister, P, and Hopt, UT. Pancreatic head resection for chronic pancreatitis in patients with extrahepatic generalized portal hypertension. Surgery.2004;135:411–418.
Gouma, DJ, van Geenen, RC, van Gulik, TM, de Haan, RJ, de Wit, LT, Busch, OR, and Obertop, H. Rates of complications and death after pancreaticoduodenectomy: risk factors and the impact of hospital volume. Ann Surg.2000;232:786–795.
Litmathe, J, Kurt, M, Feindt, P, Gams, E, and Boeken, U. The impact of pre- and postoperative renal dysfunction on outcome of patients undergoing coronary artery bypass grafting (CABG). Thorac Cardiovasc Surg.2009;57:460–463.
Poon, RT-P and Fan, ST. Hepatectomy for hepatocellular carcinoma: patient selection and postoperative outcome. Liver Transpl.2004;10:S39–S45.
Melendez, J, Ferri, E, Zwillman, M, Fischer, M, DeMatteo, R, Leung, D, Jarnagin, W, Fong, Y, and Blumgart, LH. Extended hepatic resection: a 6-year retrospective study of risk factors for perioperative mortality. J Am Coll Surg.2001;192:47–53.
Sidawy, AN, Aidinian, G, Johnson, ON, White, PW, DeZee, KJ, and Henderson, WG. Effect of chronic renal insufficiency on outcomes of carotid endarterectomy. J Vasc Surg.2008;48:1423–1430.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Neeff, H., Mariaskin, D., Spangenberg, HC. et al. Perioperative Mortality After Non-hepatic General Surgery in Patients with Liver Cirrhosis: an Analysis of 138 Operations in the 2000s Using Child and MELD Scores. J Gastrointest Surg 15, 1–11 (2011). https://doi.org/10.1007/s11605-010-1366-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-010-1366-9