Abstract
Background
Positive volume–outcomes relationships have been demonstrated for hepatic resection using arbitrary criteria to define high-volume centers. The safety of training programs has not been evaluated. The association of surgical volume, as a continuous variable and the influence of a surgical residency and a fellowship program on outcomes after major hepatectomy were determined.
Methods
The Nationwide Inpatient Sample (NIS) was queried from 1998 to 2006. Quantification of patients’ comorbidities was made using the Charlson index, and mortality, and complication rates were determined. Institutions’ annual case volumes were correlated with risk-adjusted outcomes over time, as well as presence or absence of residency or fellowship training program using logistic regression modeling.
Results
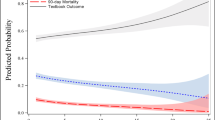
A total of 5,298 major hepatectomies were recorded, representing a weighted nationwide total of 26,396 cases. In-hospital unadjusted mortality for the study period was 6%. Adjusting for comorbidities, greater major hepatectomy volume was associated with improvements in the incidence of most measured complications, with plateauing of mortality of between 2% and 3% at approximately 50 cases per year. The mortality rate increased once greater than approximately 70 cases were performed per annum. Hospitals supporting a surgical residency program had lower overall morbidity and mortality. A fellowship program however was not associated with overall lower morbidity and mortality and appeared to result in a higher rate of certain complications.
Conclusions
Greater annual major hepatectomy volume improves outcomes with reduced mortality up to a certain point. The presence of surgical residency program but not a fellowship program is associated with reduced predicted morbidity and mortality.

Similar content being viewed by others
References
Nagasue N, Yukaya H. Liver resection for hepatocellular carcinoma: results from 150 consecutive patients. Cancer Chemother Pharmacol 1989; 23 Suppl:S78–82.
Fan ST, Lai EC, Lo CM, et al. Hospital mortality of major hepatectomy for hepatocellular carcinoma associated with cirrhosis. Arch Surg 1995; 130(2):198–203.
Thompson HH, Tompkins RK, Longmire WP, Jr. Major hepatic resection. A 25-year experience. Ann Surg 1983; 197(4):375–88.
Vauthey JN, Pawlik TM, Abdalla EK, et al. Is extended hepatectomy for hepatobiliary malignancy justified? Ann Surg 2004; 239(5):722–30; discussion 730–2.
Torzilli G, Makuuchi M, Inoue K, et al. No-mortality liver resection for hepatocellular carcinoma in cirrhotic and noncirrhotic patients: is there a way? A prospective analysis of our approach. Arch Surg 1999; 134(9):984–92.
Asiyanbola B, Chang D, Gleisner AL, et al. Operative mortality after hepatic resection: are literature-based rates broadly applicable? J Gastrointest Surg 2008; 12(5):842–51.
Birkmeyer JD, Sun Y, Goldfaden A, et al. Volume and process of care in high-risk cancer surgery. Cancer 2006; 106(11):2476–81.
Birkmeyer JD, Stukel TA, Siewers AE, et al. Surgeon volume and operative mortality in the United States. N Engl J Med 2003; 349(22):2117–27.
Birkmeyer JD, Siewers AE, Finlayson EV, et al. Hospital volume and surgical mortality in the United States. N Engl J Med 2002; 346(15):1128–37.
Harmon JW, Tang DG, Gordon TA, et al. Hospital volume can serve as a surrogate for surgeon volume for achieving excellent outcomes in colorectal resection. Ann Surg 1999; 230(3):404–11; discussion 411–3.
Csikesz NG, Simons JP, Tseng JF, et al. Surgical specialization and operative mortality in hepato-pancreatico-biliary (HPB) surgery. J Gastrointest Surg 2008; 12(9):1534–9.
Eppsteiner RW, Csikesz NG, Simons JP, et al. High volume and outcome after liver resection: surgeon or center? J Gastrointest Surg 2008; 12(10):1709–16; discussion 1716.
Kohn GP, Galanko JA, Meyers MO, et al. National trends in esophageal surgery—are outcomes as good as we believe? J Gastrointest Surg 2009; 13(11):1900-10.
HCUP Nationwide Inpatient Sample (NIS). Healthcare Cost and Utilization Project (HCUP). 1998–2006. Agency for Healthcare Research and Quality, Rockville, MD. Available at: www.hcup-us.ahrq.gov/nisoverview.jsp. Accessed 11 September 2008.
International Hepato-Pancreato-Biliary Association (IHPBA) Fellowship Registry. Available at: http://www.ihpba.org/fellowship-reg-zone1.html. Accessed 11 September 2008.
The Fellowship Council website. Directory of Fellowships. Available at: https://fellowshipcouncil.org/directory/browse2.php. Accessed 11 September 2008.
Society of Surgical Oncology (SSO) training programs. Available at: http://www.surgonc.org/default.aspx?id = 60. Accessed 11 September 2008.
Accreditation Council for Graduate Medical Education website. Available at: http://www.acgme.org/adspublic/. Access 26 November 2008.
American Medical Association website. FREIDA Online GME program search results. Available at: https://freida.ama-assn.org/Freida/user/programSearchSubmitDispatch.do. Accessed 26 November 2008.
Santry HP, Gillen DL, Lauderdale DS. Trends in bariatric surgical procedures. JAMA 2005; 294(15):1909–17.
Kohn GP, Galanko JA, Overby DW, et al. Volume-outcome relationships and other influences of outcome in bariatric surgery. Surg Endosc 2009; 23(S1):149.
Finlayson SR. The volume-outcome debate revisited. Am Surg 2006; 72(11):1038–42; discussion 1061-9, 1133-48.
Hall WH, Ramachandran R, Narayan S, et al. An electronic application for rapidly calculating Charlson comorbidity score. BMC Cancer 2004; 4:94.
Timaran CH, Rosero EB, Smith ST, et al. Trends and outcomes of concurrent carotid revascularization and coronary bypass. J Vasc Surg 2008; 48(2):355–360; discussion 360–1.
Hansel NN, Merriman B, Haponik EF, et al. Hospitalizations for tuberculosis in the United States in 2000: predictors of in-hospital mortality. Chest 2004; 126(4):1079–86.
Metzger R, Bollschweiler E, Vallbohmer D, et al. High volume centers for esophagectomy: what is the number needed to achieve low postoperative mortality? Dis Esophagus 2004; 17(4):310–4.
Kohn GP, Galanko JA, Overby DW, et al. Recent trends in bariatric surgery case volume in the United States. Surgery 2009; 146(2):375–80.
Nikfarjam M, Shereef S, Kimchi ET, et al. Survival outcomes of patients with colorectal liver metastases following hepatic resection or ablation in the era of effective chemotherapy. Ann Surg Oncol 2008; 16(7):1860-7.
Acknowledgements
For conception and design: GPK, MN; for acquisition of data: GPK; for analysis: GPK and MN; for drafting of manuscript: GPK, MN; for critical revision: GPK, MN; for statistical expertise: GPK. The authors acknowledge the general statistical assistance provided by JA Galanko, Ph.D. of the University of North Carolina at Chapel Hill, NC.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Kohn, G.P., Nikfarjam, M. The Effect of Surgical Volume and the Provision of Residency and Fellowship Training on Complications of Major Hepatic Resection. J Gastrointest Surg 14, 1981–1989 (2010). https://doi.org/10.1007/s11605-010-1310-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-010-1310-z