Abstract
Introduction
We analyzed the clinicopathological characteristics and outcomes of patients with gastric stump cancer (GSC) to identify important prognostic factors.
Patients and Methods
We retrospectively reviewed clinical reports of 34 patients with GSC treated at Kochi Medical School from 1982 to 2008 to analyze the clinical and pathological factors that influenced patient survival.
Results
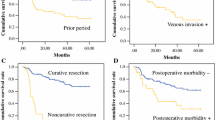
The median interval between initial and second operation was 15.8 years; this interval was significantly longer in patients diagnosed originally with benign disease than in those with previous malignant disease. Histologically, the incidence of diffuse-type cancer was significantly prominent in patients with previous benign gastric disease than in those with previous malignant gastric disease. The overall 5-year survival rate was 53.3%, with presence of lymph node metastasis and pathological serosal invasion of the tumor associated with poor survival. The final analysis revealed tumor located at anastomosis, tumor size greater than 5 cm, serosal invasion, the presence of lymph node metastasis, and stage III or higher to be significantly associated with poor survival.
Conclusions
Follow-up programs after gastrectomy should account for long latency periods of disease. Early detection, attentive observation of anastomotic site, and sufficient surgical resection were important influences on outcome for patients with GSC after Billroth I or Billroth II reconstruction.


Similar content being viewed by others
References
Thorban S, Bottcher K, Etter M, Roder JD, Busch R, Siewert JR. Prognostic factors in gastric stump carcinoma. Ann Surg 2000;231:188–194.
Balfour DC. Factors influencing the life expectancy of patients operated on for gastric ulcer. Ann Surg 1922;76:405–408.
Sinning C, Schaefer N, Standop J, Hirner A, Wolff M. Gastric stump carcinoma: epidemiology and current concepts in pathology and treatment. Eur J Surg Oncol 2007;33:133–139.
Tanigawa N, Nomura E, Niki M, Shinohara H, Nishiguchi K, Okuzawa M, Toyoda M, Morita S. Clinical study to identify specific characteristics of cancer newly developed in the remnant stomach. Gastric Cancer 2002;5:23–28.
Sano T, Sasako M, Kinoshita T, Maruyama K. Recurrence of early gastric cancer: follow-up of 1475 patients and review of the Japanese literature. Cancer 1993;72:3174–3178.
Shimada S, Yagi Y, Shiomori K, Honmyo U, Hayashi N, Matsuo A, Marutsuka T, Ogawa M. Characterization of early gastric cancer and proposal of the optimal therapeutic strategy. Surgery 2001;129:714–719.
Ohashi M, Katai H, Fukagawa T, Gotoda T, Sano T, Sasako M. Cancer of the gastric stump following distal gastrectomy for cancer. Br J Surg 2007;94:92–95.
Ahn HS, Kim JW, Yoo MW, Park DJ, Lee HJ, Lee KU, Yang HK. Clinicopathological features and surgical outcomes of patients with remnant gastric cancer after a distal gastrectomy. Ann Surg Oncol 2008;15:1632–1639.
Japanese Gastric Cancer Association. Japanese classification of gastric carcinoma: 2nd English edition. Gastric Cancer 1998;1:10–24.
Sobin LH, Gospodarowicz MK, Wittekind C (eds). “TNM classification of malignant tumours (7th Edition).” New York: Wiley-Blackwell, 2009.
Wittekind C, Greene F, Hutter RVP, Sobin LH, Henson DE (eds). “TNM supplement: a commentary on uniform use (3rd Edition).” New York: Wiley-Liss, 2003.
Lauren P. The two histological main types of gastric carcinoma: diffuse and so-called intestinal-type carcinoma. An attempt at a histoclinical classification. Acta Pathol Microbiol Scand 1965;64:31–49.
Kaplan EL, Meier P. Nonparametric estimation from incomplete observations. J Am Stat Assoc 1958;53:457.
Schaefer N, Sinning C, Standop J, Overhaus M, Hirner A, Wolff M. Treatment and prognosis of gastric stump carcinoma in comparison with primary proximal gastric cancer. Am J Surg 2007;194:63–67.
Hu X, Tian DY, Cao L, Yi Y. Progression and prognosis of gastric stump cancer. J Surg Oncol 2009;100:472–476.
Han SL, Hua YW, Wang CH, Ji SQ, Zhuang J. Metastatic pattern of lymph node and surgery for gastric stump cancer. J Surg Oncol 2003;82:241–246.
Sasako M, Maruyama K, Kinoshita T, Okabayashi K. Surgical treatment of carcinoma of the gastric stump. Br J Surg 1991;78:822–824.
Kunisaki C, Makino H, Takagawa R, Oshima T, Nagano Y, Kosaka T, Ono HA, Otsuka Y, Akiyama H, Ichikawa Y, Shimada H. Tumor diameter as a prognostic factor in patients with gastric cancer. Ann Surg Oncol 2008;15:1959–1967.
Inomata M, Shiraishi N, Adachi Y, Yasuda K, Aramaki M, Kitano S. Gastric remnant cancer compared with primary proximal gastric cancer. Hepatogastroenterology 2003;50:587–591.
Kaneko K, Kondo H, Shirao K, Yamaguchi H, Yokota T, Yamao G, Sano T, Sasako M, Yoshida S. Early gastric stump cancer following distal gastrectomy. Gut 1998;43:342–344.
An JY, Choi MG, Noh JH, Sohn TS, Kim S. The outcome of patients with remnant primary gastric cancer compared with those having upper one-third gastric cancer. Am J Surg 2007;194:143–147.
Newman E, Brennan MF, Hochwald SN, Harrison LE, Karpeh MS. Gastric remnant carcinoma: just another proximal gastric cancer or a unique entity? Am J Surg 1997;173:292–297.
Piso P, Meyer HJ, Edris C, Jahne J. Surgical therapy of gastric stump carcinoma: a retrospective analysis of 109 patients. Hepatogastroenterology 1999;46:2643–2647.
Matsui N, Yao T, Akazawa K, Nawata H, Tsuneyoshi M. Different characteristics of carcinoma in the gastric remnant: histochemical and immunohistochemical studies. Oncol Rep 2001;8:17–26.
Kaminishi M, Shimizu N, Shiomoyama S, Yamaguchi H, Ogawa T, Sakai S, Kuramoto S, Oohara T. Etiology of gastric remnant cancer with special reference to the effects of denervation of the gastric mucosa. Cancer 1995;75:1490–1496.
Namikawa T, Kitagawa H, Okabayashi T, Sugimoto T, Kobayashi M, Hanazaki K. Roux-en-Y reconstruction is superior to Billroth I reconstruction in reducing reflux esophagitis after distal gastrectomy: special relationship with the angle of His. World J Surg 2010;34:1022–1027.
Talley NJ, Fock KM, Moayyedi P. Gastric Cancer Consensus conference recommends Helicobacter pylori screening and treatment in asymptomatic persons from high-risk populations to prevent gastric cancer. Am J Gastroenterol. 2008;103:510–514.
Nagahata Y, Kawakita N, Azumi Y, Numata N, Yano M, Saitoh Y. Etiological involvement of Helicobacter pylori in ‘reflux’ gastritis after gastrectomy. Am J Gastroenterol 1996;91:2130–2134.
Nakagawara H, Miwa K, Nakamura S, Hattori T. Duodenogastric reflux sustains Helicobacter pylori infection in the gastric stump. Scand J Gastroenterol 2003;38:931–937.
Kaminishi M, Shimizu N, Yamaguchi H, Hashimoto M, Sakai S, Oohara T. Different carcinogenesis in the gastric remnant after gastrectomy for gastric cancer. Cancer 1996;77:1646–1653.
Tanigawa N, Nomura E, Lee SW, Kaminishi M, Sugiyama M, Aikou T, Kitajima M; The Society for the study of postoperative morbidity after gastrectomy. Current state of gastric stump carcinoma in Japan: based on the results of a nationwide survey. World J Surg 2010;34:1540–1547.
Miwa K, Hasegawa H, Fujimura T, Matsumoto H, Miyata R, Kosaka T, Miyazaki I, Hattori T. Duodenal reflux through the pylorus induces gastric adenocarcinoma in the rat. Carcinogenesis 1992;13:2313–2316.
Safatle-Ribeiro AV, Ribeiro U Jr, Reynolds JC. Gastric stump cancer: what is the risk? Dig Dis 1998;16:159–168.
Ojima T, Iwahashi M, Nakamori M, Nakamura M, Naka, T, Katsuda M, Iida T, Tsuji T, Hayata K, Takifuji K, Yamaue H. Clinicopathological characteristics of remnant gastric cancer after a distal gastrectomy. J Gastrointest Surg 2010;14:277–281.
Conflict of interest statement
We certify that there is no actual or potential conflict of interest and no grants or financial support in relation to this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Namikawa, T., Kitagawa, H., Iwabu, J. et al. Tumors Arising at Previous Anastomotic Site may have Poor Prognosis in Patients with Gastric Stump Cancer Following Gastrectomy. J Gastrointest Surg 14, 1923–1930 (2010). https://doi.org/10.1007/s11605-010-1298-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-010-1298-4