Abstract
Purpose
The purpose of the study was to assess the role of atopy on the development of appendicitis. Acute appendicitis is the most common indication for emergent laparotomy especially in the late teens and early 20s. The pathogenesis generally begins with luminal obstruction caused by fecal mass, seeds, stricture, and bacterial, parasitic, or viral infections. The present study was designed to evaluate whether allergic reaction is indeed an undefined leading factor for luminal obstruction.
Material and Methods
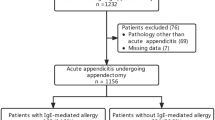
Mix inhalant and food prick tests were performed in 111 patients who underwent appendectomy for acute appendicitis and in 100 control patients. The material of appendectomy was examined, acute appendicitis was verified and graded according to the severity of inflammation and eosinophilic infiltration rate in the wall of appendix by a pathologist. Demographic data were recorded, and peripheral eosinophil count was also performed.
Results
Mix prick test of 33 patients (29.7%) and food prick test of 14 patients (12.6%) were positive in study group when compared with 7 patients (7%) and 1 patient (1%) in control group (p < 0.001). A total of 38 patients (34.2%) in the study group were reactive with mix or food prick test when compared with 8 patients (8%) in control group. There was no significant difference between eosinophilic infiltration rate, peripheral eosinophil count, severity of inflammation, and Alvarado score of mix prick test positive and negative patients in study group.
Conclusion
Atopy incidence in patients with acute appendicitis was significantly higher when compared with control group. However, eosinophilic infiltration rate, inflammation grade, and peripheral eosinophil count were not able to explain the relationship between the two conditions. Atopy is a risk factor for acute appendicitis.
Similar content being viewed by others
References
National Center for Health Statistics. Ambulatory and inpatient procedures in the United States, 1996. National Center for Health Statistics Series 13 (No. 139); 2004
Jones PF. Suspected acute appendicitis: trends in management over 30 years. Br J Surg 2001;88:1570–1577.
Prystowsky JB, Pugh CM, Nagle AP. Current problems in surgery. Appendicitis. Curr Probl Surg 2005;42:688–742.
Alvarado A. A practical score for the early diagnosis of acute appendicitis. Ann Emerg Med 1986;15:557–564.
Seibold F. Food-induced immune responses as origin of bowel disease? Digestion 2005;71:251–260.
Xie H, He SH. Roles of histamine and its receptors in allergic and inflammatory bowel disease. World J Gastroenterol 2005;11:2851–2857.
Sicherer SH. Food allergy. Lancet 2002;360:701–710.
Pires GV, Souza HS, Elia CC, Zaltman C, Carvalho AT, Tortori CJ, Garrofé HC, Lapa e Silva JR. Small bowel of patients with asthma and allergic rhinitis: absence of inflammation despite the presence of major cellular components of allergic inflammation. Allergy Asthma Proc 2004;25:253–259.
Bolukbas FF, Bolukbas C, Uzunkoy A, Baba F, Horoz M, Ozturk E. A dramatic response to ketotifen in a case of eosinophilic gastroenteritis mimicking abdominal emergency. Dig Dis Sci 2004;49:1782–1785.
Madhotra R, Eloubeidi MA, Cunningham JT, Lewin D, Hoffman B. Eosinophilic gastroenteritis masquerading as ampullary adenoma. J Clin Gastroenterol 2002;34:240–242.
Tran D, Salloum L, Tshibaka C, Moser R. Eosinophilic gastroenteritis mimicking acute appendicitis. Am Surg 2000;66:990–992.
Noodleman JS. Eosinophilic appendicitis. Demonstration of Strongyloides stercoralis as a causative agent. Arch Pathol Lab Med 1981;105:148–149.
Nadler S, Cappell MS, Bhatt B, Matano S, Kure K. Appendiceal infection by Entamoeba histolytica and Strongyloides stercoralis presenting like acute appendicitis. Dig Dis Sci 1990;35:603–608.
Yun MY, Cho YU, Park IS, Choi SK, Kim SJ, Shin SH, Kim KR. Eosinophilic gastroenteritis presenting as small bowel obstruction: a case report and review of the literature. World J Gastroenterol 2007;13:1758–1760.
Schwab D, Müller S, Aigner T, Neureiter D, Kirchner T, Hahn EG, Raithel M. Functional and morphologic characterization of eosinophils in the lower intestinal mucosa of patients with food allergy. Am J Gastroenterol 2003;98:1525–1534.
Vieths S, Scheurer S, Ballmer-Weber B. Current understanding of cross- reactivity of food allergens and pollen. Ann N Y Acad Sci 2002;964:47–68.
Magnusson J, Lin XP, Dahlman-Höglund A, Hanson LA, Telemo E, Magnusson O, Bengtsson U, Ahlstedt S. Seasonal intestinal inflammation in patients with birch pollen allergy. J Allergy Clin Immunol 2003;112:45–51.
Khan S. Eosinophilic gastroenteritis. Best Pract Res Clin Gastroenterol 2005;19:177–198.
von Wattenwyl F, Zimmermann A, Netzer P. Synchronous first manifestation of an idiopathic eosinophilic gastroenteritis and bronchial asthma. Eur J Gastroenterol Hepatol 2001;13:721–725.
Untersmayr E, Jensen-Jarolim E. The effect of gastric digestion on food allergy. Curr Opin Allergy Clin Immunol 2006;6:214–219.
Noudeh YJ, Sadigh N, Ahmadnia AY. Epidemiologic features, seasonal variations and false positive rate of acute appendicitis in Shahr-e-Rey, Tehran. Int J Surg 2007;5:95–98.
Bousquet PJ, Chatzi L, Jarvis D, Burney P. Assessing skin prick tests reliability in ECRHS-I. Allergy 2007;63:341–346
Eng PA, Borer-Reinhold M, Heijnen IA, Gnehm HP. Twelve-year follow-up after discontinuation of preseasonal grass pollen immunotherapy in childhood. Allergy 2006;61:198–201.
Kay AB. Skin tests in allergy and allergic disease. Vol:2. Oxford: Blackwell Science, 1997, pp 1008–1009.
Kupczyk M, Kupryś I, Bocheńska-Marciniak M, Górski P, Kuna P. Ranitidine (150 mg daily) inhibits wheal, flare, and itching reactions in skin-prick tests. Allergy Asthma Proc 2007;28:711–5.
Rao KS, Menon PK, Hilman BC, Sebastian CS, Bairnsfather L. Duration of the suppressive effect of tricyclic antidepressants on histamine-induced wheal-and-flare reactions in human skin. J Allergy Clin Immunol 1988;82:752–7.
Kalliomaki MA. Food allergy and irritable bowel syndrome. Curr Opin Gastroenterol 2005;21:708–711.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Harlak, A., Gulec, M., Mentes, O. et al. Atopy is a Risk Factor for Acute Appendicitis? A Prospective Clinical Study. J Gastrointest Surg 12, 1251–1256 (2008). https://doi.org/10.1007/s11605-008-0511-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-008-0511-1