Abstract
Introduction
Intraabdominal schwannomas are rare, benign tumors. This study presents a single institution experience with 12 such tumors.
Methods
Between 1991 to 2006, 12 patients with a pathologically proven intraabdominal schwannoma were identified from a series of 216 mesenchymal tumors and were reviewed retrospectively.
Results
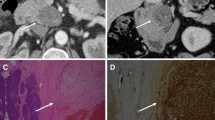
There were nine females and three male patients with a median age of 58 years (range 35–88 years). Eleven patients were symptomatic, and the tumors were located in the stomach (n = 8), jejunum, colon, rectum, and lesser sac. Multiple preoperative investigations including endoscopies with biopsies and computed tomography (CT) scans were performed, but none yielded a correct definitive preoperative diagnosis. The median tumor size was 52 mm (range 18–95 mm). Pathological examination demonstrated the 11 gastrointestinal tract (GIT) schwannomas to be solid homogenous tumors, which were highly cellular and were composed of spindle cells with positive staining for S100 protein. The pathological appearance of the lesser sac schwannoma was distinct as it demonstrated cystic degeneration with hemorrhage and Antoni A and B areas on microscopy typical of soft tissue schwannomas. All 12 patients were disease-free at a median follow-up of 22 months (range 1–120 months).
Conclusion
Intraabdominal schwannomas are rare tumors, which are most frequently located within the GIT. GIT schwannomas are difficult if not impossible to diagnose preoperatively as endoscopic and radiologic findings are nonspecific. The treatment of choice is complete surgical excision because of diagnostic uncertainty, and the long-term outcome is excellent as these lesions are uniformly benign.
Similar content being viewed by others
References
Gubbay AD, Moschilla G, Gray BN, Thompson I. Retroperitoneal schwannoma: A case series and review. Aust N Z J Surg 1995;65:197–200.
Khan AA, Schizas AM, Cresswell AB, Khan MK, Khawaja HT. Digestive tract schwannoma. Dig Surg 2006;23:265–269.
Goh BK, Tan YM, Chung YF, Chow PK, Ooi LL, Wong WK. Retroperitoneal schwannoma. Am J Surg 2006;192:14–18.
Melvin WS, Wilkinson MG. Gastric schwannoma. Clinical and pathologic considerations. Am Surg 1993;59:293–296.
Hou YY, Tan YS, Wang XN, Lu SH, Ji Y, Wang J, Zhu XZ. Schwannoma of the gastrointestinal tract: A clinicopathological, immunohistochemical and ultrastructural study of 33 cases. Histopathology 2006;48:536–545.
Prevot S, Bienvenu L, Vaillant JC, de Saint-Maur PP. Benign schwannoma of the digestive tract. A clinicopathologic and immunohistochemical study of five cases, including a case of esophageal tumor. Am J Surg Pathol 1999;23:431–436.
Bankier AA, Stanek C, Hubsch P. Case report: benign solitary schwannoma of the greater omentum: A rare cause of acute intraperitoneal bleeding—diagnosis by CT. Clin Radiol 1996;51:517–518.
Noonan JD, Minagi H, Margolin R. Benign solitary schwannoma of the lesser peritoneal sac. AJR Am J Roentgenol 1976;125:391.
Fenoglio L, Severini S, Cena P, Migliore E, Bracco C, Pomero F, Panzone S, Cavallero GB, Silvestri A, Brizio R, Borghi F. Common bile duct schwannoma: A case report an review of literature. World J Gastroenterol 2007;13:1275–1278.
Levy AD, Quiles AM, Miettinen M, Sobin LH. Gastrointestinal schwannomas: CT features with clinicopathologic correlation. AJR Am J Roentgenol 2005;184:797–802.
Kwon MS, Lee SS, Ahn GH. Schwannomas of the gastrointestinal tract: Clinicopathological features of 12 cases including a case of esophageal tumor compared with those of gastrointestinal stromal tumors and leiomyomas of the gastrointestinal tract. Pathol Res Pract 2002;198:605–613.
Daimaru Y, Kido H, Hashimoto H, Enjoji M. Benign schwannoma of the gastrointestinal tract: A clinicopathologic and immunohistochemical study. Hum Pathol 1988;19:257–264.
Sarlomo-Rikala M, Miettinen M. Gastric schwannoma—a clinicopathological analysis of six cases. Histopathology 1995;27:355–360.
Toh LM, Wong SK. A case of cystic lesser sac schwannoma. Ann Acad Med Singapore 2006;35:45–48.
Flemming P, Frerker M, Klempnauer J, Pichlmayr R. Benign schwannoma of the liver with cystic changes misinterpreted as hydatid disease. Hepatogastroenterology 1998;45:1764–1766.
Yagishashi N, Kaimori M, Katayama Y, Yagihashi S. Crystalloid formation in gastrointestinal schwannoma. Hum Pathol 1997;28:304–308.
Fletcher CD, Berman JJ, Corless C, et al. Diagnosis of gastrointestinal stromal tumors: A consensus approach. Hum Pathol 2002;33:459–465.
Miettinen M, Shekitka KM, Sobin LH. Schwannomas in the colon and rectum: A clinicopathologic and immunohistochemical study of 20 cases. Am J Surg Pathol 2001;25:846–855.
Agaimy A, Wunsch PH. Gastrointestinal stromal tumors: A regular origin in the muscularis propria, but an extremely diverse gross presentation. A review of 200 cases to critically re-evaluate the concept of so-called extra-gastrointestinal stromal tumours. Langenbecks Arch Surg 2006;391:322–329.
Meittinen M, Virolainen M, Rikala MS. Gastrointestinal stromal tumors. Value of CD34 antigen in their identification and separation from true leiomyomas and schwannomas. Am J Surg Pathol 1995;19:207–216.
Burkill GJ, Badran M, Al-Muderis O, et al. Malignant gastrointestinal stromal tumor: Distribution, imaging features, and pattern of metastatic spread. Radiology 2003;226:527–532.
Levy AD, Remotti HE, Thompson WM, Sobin LH, Miettinen M. Gastrointestinal stromal tumors: Radiologic features with pathologic correlation. Radiographics 2003;23:283–304, 456,quiz 532.
Fujii Y, Taniguchi N, Hosoya Y, Yoshizawa K, Yasuda Y, Nagai H, Itoh K. Gastric schwannoma: Sonographic findings. J Ultrasound Med 2004;23:1527–1530.
Rodriguez SA, Faigel DO. Endoscopic diagnosis of gastrointestinal stromal cell tumors. Curr Opin Gastroenterol 2007;23:539–543.
Bees NR, Ng CS, Dicks-Mireaux C, Kiely EM. Gastric malignant schwannoma in a child. Br J Radiol 1997;70:952–955.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Goh, B.K.P., Chow, P.K.H., Kesavan, S. et al. Intraabdominal Schwannomas: A Single Institution Experience. J Gastrointest Surg 12, 756–760 (2008). https://doi.org/10.1007/s11605-007-0441-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-007-0441-3