Abstract
Objective
Patients with chronic ulcerative colitis (UC) often have mental symptoms such as depression and anxiety, and stress can lead to gastrointestinal diseases. However, the correlation between mental stress and UC is unclear. In this paper, chronic unpredictable mild stress (CUMS) was utilized to evaluate the involvement of mental factors in the pathogenesis of UC.
Methods
The CUMS model was used to evaluate the direct/indirect involvement of mental factors in the pathogenesis of UC. The behavior was evaluated by the open field, forced swimming, and tail suspension tests. Body weight, the disease activity index (DAI) score, colon length, and HE staining of colon tissue were used to evaluate the action of CUMS and fluoxetine.
Results
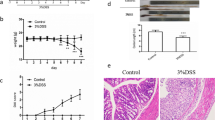
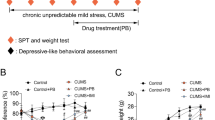
The results showed that weight loss and the DAI score increased in CUMS mice, but they had no meaningful effect on colon length and morphological structure of colon tissue. However, CUMS aggravated dextran sulfate sodium (DSS)-induced colon length shortening and colon morphological structure damage. Fluoxetine significantly improved the DAI score, shortened colon length, and damaged morphology and structure of the colons induced by CUMS combined with DSS in mice. Fluoxetine also decreased the level of IL-6 in the serum and the TNF-α and IFN-γ levels of colon tissue. Fluoxetine simultaneously improved behavioral abnormalities induced by CUMS combined with DSS in mice.
Conclusion
CUMS aggravated the UC symptoms induced by DSS, and fluoxetine could improve the UC symptoms due to its improvement in the inflammatory level and behavioral abnormalities.
Similar content being viewed by others
References
Feuerstein JD, Moss AC, Farraye FA. Ulcerative Colitis. Mayo Clin Proc, 2019,94(7):1357–1373
Du L, Ha C. Epidemiology and Pathogenesis of Ulcerative Colitis. Gastroenterol Clin North Am, 2020,49(4):643–654
Ungaro R, Mehandru S, Allen PB, et al. Ulcerative colitis. Lancet, 2017,389(10080):1756–1770
Carvello M, Watfah J, Spinelli A. The Management of the Hospitalized Ulcerative Colitis Patient, the Medical-Surgical Conundrum. Curr Gastroenterol Rep, 2021,23(12):25
Kózka M, Skowron W, Bodys-Cupak I. Determinants of the level of anxiety and fears in a group of patients with ulcerative colitis. Ann Agric Environ Med, 2019,26(2):337–340
Rubin DT, Ananthakrishnan AN, Siegel CA, et al. ACG Clinical Guideline: Ulcerative Colitis in Adults. Am J Gastroenterol, 2019,114(3):384–413
Raine T, Bonovas S, Burisch J, et al. ECCO Guidelines on Therapeutics in Ulcerative Colitis: Medical Treatment. J Crohns Colitis, 2022,16(1):2–17
Domínguez Jiménez JL, Pelado García EM, Copado Herrera R. Mesalazine-induced acute hepatitis. Gastroenterol Hepatol, 2015,38(4):302–303
Kotlyar DS, Lewis JD, Beaugerie L, et al. Risk of lymphoma in patients with inflammatory bowel disease treated with azathioprine and 6-mercaptopurine: a meta-analysis. Clin Gastroenterol Hepatol, 2015,13(5):847–858
Atreya R, Neurath MF, Siegmund B. Personalizing Treatment in IBD: Hype or Reality in 2020? Can We Predict Response to Anti-TNF? Front Med, 2020,7:517
Tavakoli P, Vollmer-Conna U, Hadzi-Pavlovic D, et al. A Review of Inflammatory Bowel Disease: A Model of Microbial, Immune and Neuropsychological Integration. Public Health Rev, 2021,42:1603990
Yuan X, Chen B. Depression and anxiety in patients with active ulcerative colitis: crosstalk of gut microbiota, metabolomics and proteomics. Gut Microbes, 2021,13(1):1987779
Gao X, Tang Y, Lei N, et al. Symptoms of anxiety/depression is associated with more aggressive inflammatory bowel disease. Sci Rep, 2021,11(1):1440
Vicentini FA, Szamosi JC, Rossi L, et al. Colitis-associated microbiota drives changes in behaviour in male mice in the absence of inflammation. Brain, Behav, and Immun, 2022,102:266–278
Yousefi-Manesh H, Dejban P, Mumtaz F, et al. Risperidone attenuates acetic acid-induced colitis in rats through inhibition of TLR4/NF-kB signaling pathway. Immunopharmacol Immunotoxicol, 2020,42(5):464–472
Minaiyan M, Hajhashemi V, Rabbani M, et al. Evaluation of anti-colitic effect of fluvoxamine against acetic acid-induced colitis in normal and reserpinized depressed rats. Eur J Pharmacol, 2015,746:293–300
Li N, Lu Y. Forty Cases of Adjuvant Therapy for Elderly Patients with Ulcerative Colitis Assciated with Anxiety /Depression by Paroxetine Hydrochloride. Herald of Medicine (Chinese), 2015,34(7):903–906
Zhou Y, Wu J. Efficacy of sertraline hydrochloride in the treatment of ulcerative colitis with depression. Chinese Journal of Digestion (Chinese), 2015,35(9):595–598
Yang Z. Clinical effect of Deanxit combined with mesalazine in the treatment of ulcerative colitis. Mod Diagn Treat (Chinese), 2013,24(17):3920–3920
Shi X. Clinical efficacy of sertraline hydrochloride combined with mesalazine in the treatment of ulcerative colitis with depression. Chin J Clin Rational Drug Use (Chinese), 2016,9(23):46–47
Zhang Z, Yang L, Wang B, et al. Protective role of liriodendrin in mice with dextran sulphate sodium-induced ulcerative colitis. Int Immunopharmacol, 2017,52:203–210
Li Y, Adam R, Colombel JF, et al. A characterization of proinflammatory cytokines in dextran sulfate sodium-induced chronic relapsing colitis mice model. Int Immunopharmacol, 2018,60:194–201
Sun L, Zhang H, Cao Y, et al. Fluoxetine ameliorates dysbiosis in a depression model induced by chronic unpredicted mild stress in mice. Int J Med Sci, 2019,16(9):1260–1270
Wu H, Wang R, Qin X, et al. Effects of chronic stress on depressive-like behaviors and JMJD3 expression in the prefrontal cortex and hippocampus of C57BL/6 and ob/ob mice. J Psychiatr Res, 2021,133:142–155
Archer J. Tests for emotionality in rats and mice: a review. Anim Behav, 1973,21(2):205–235
Bourin M, Mocaër E, Porsolt R. Antidepressant-like activity of S 20098 (agomelatine) in the forced swimming test in rodents: involvement of melatonin and serotonin receptors. J Psychiatry Neurosci, 2004,29(2):126–133
Antoniuk S, Bijata M, Ponimaskin E, et al. Chronic unpredictable mild stress for modeling depression in rodents: Meta-analysis of model reliability. Neurosci Biobehav Rev, 2019,99:101–116
Marcinkute M, Afshinjavid S, Fatokun AA, et al. Fluoxetine selectively induces p53-independent apoptosis in human colorectal cancer cells. Eur J Pharmacol, 2019,857:172441
Tatiya-Aphiradee N, Chatuphonprasert W, Jarukamjorn K. Immune response and inflammatory pathway of ulcerative colitis. J Basic Clin Physiol Pharmacol, 2018,30(1):1–10
Zhu L, Gu P, Shen H. Protective effects of berberine hydrochloride on DSS-induced ulcerative colitis in rats. Int Immunopharmacol, 2019,68:242–251
Barberio B, Zamani M, Black CJ, et al. Prevalence of symptoms of anxiety and depression in patients with inflammatory bowel disease: a systematic review and meta-analysis. Lancet Gastroenterol Hepatol, 2021,6(5):359–370
Li K, Yan L, Zhang Y, et al. Seahorse treatment improves depression-like behavior in mice exposed to CUMS through reducing inflammation/oxidants and restoring neurotransmitter and neurotrophin function. J Ethnopharmacol, 2020,250:112487
Ford AC, Sperber AD, M. Corsetti, et al. Irritable bowel syndrome. Lancet, 2020,396(10263):1675–1688
Xu H, Cai F, Li P, et al. Characterization and Analysis of the Temporal and Spatial Dynamic of Several Enteritis Modeling Methodologies. Front Immunol, 2021,12:727664
Zhao J, Li C, Jing X, et al. Corylin ameliorates chronic ulcerative colitis via regulating the gut-brain axis and promoting 5-hydroxytryptophan production in the colon. Phytomedicine, 2023,110:154651
Samantha D, Idalia G, Fabiola T, et al. Interplay between Serotonin, Immune Response, and Intestinal Dysbiosis in Inflammatory Bowel Disease. Int J Mol Sci, 2022,23(24):15632
Yu F, Huang S, Zhang H, et al. Comparison of 5-hydroxytryptophan signaling pathway characteristics in diarrhea-predominant irritable bowel syndrome and ulcerative colitis. World J Gastroenterol, 2016,22(12):3451–3459
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
The authors declare no conflicts of interest.
Additional information
This project was supported by grants from the National Natural Science Foundation Youth Project of China (No. 81703716), Jiangxi Science Foundation for Distinguished Young Scholars (No. 20224ACB216019), the Natural Science Foundation of Jiangxi Province (No. 20202BABL206151 and No. 20202BABL216026), Youth Talents Project of Jiangxi Science and Technology Normal University (No. 2017QNBJRC006), Doctoral Startup Fund of Jiangxi Science and Technology Normal University (No. 2019BSQD015), Department Education Science and Technology Research Project of Jiangxi (No. GJJ201134), the Open Project of Jiangxi Provincial Key Laboratory of Drug Design and Evaluation (No. JKD-KF-2104), and the National Undergraduate Training Program for Innovation of China (No. 202211318024).
Rights and permissions
About this article
Cite this article
Zhao, T., Zhou, Yx., Wang, Rj. et al. Fluoxetine Ameliorates the Aggravation of UC Symptoms in C57BL/6 Mice Induced by CUMS. CURR MED SCI 43, 1033–1042 (2023). https://doi.org/10.1007/s11596-023-2743-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-023-2743-4