Abstract
Objective
Melanoblasts are the cell source of regeneration for pigment restoration. The ability to differentiate into mature melanocytes is the essential feature of melanoblasts in depigmentation diseases. Cold atmospheric plasma is an ionized gas with near-room temperature and highly reactive species that has been shown to induce stem cell differentiation. The aim of the study was to explore the effect of cold atmospheric plasma on the differentiation of melanoblast progenitor cells.
Methods
In this study, melanoblasts were exposed to the plasma jet and the cell morphology was observed. The cell cycle and cell proliferation were detected. Furthermore, the cell immunofluorescence and the detection of melanin particle and nitric oxide were carried out to investigate the differentiation of melanoblast progenitor cells.
Results
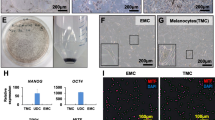
Cells that were treated with the plasma had longer and more synaptic structures, and the G1 phase of cell cycle was prolonged in the treated group. More melanin synthesis-related proteins and melanin particles were produced after plasma treatment. Nitric oxide was one of the active components generated by the plasma jet, and the nitric oxide content in the cell culture medium of the treated group increased.
Conclusion
These results indicate that an increase in nitric oxide production caused by a plasma jet can promote cell differentiation. The application of plasma provides an innovative strategy for the treatment of depigmentation diseases.
Similar content being viewed by others
References
Birlea SA, Costin GE, Roop DR, et al. Trends in regenerative medicine: repigmentation in vitiligo through melanocyte stem cell mobilization. Med Res Rev, 2017,37(4):907–935
Yu S, Lan CE, Yu HS. Mechanisms of repigmentation induced by photobiomodulation therapy in vitiligo. Exp Dermatol, 2019,28(Suppl 1):10–14
Goldstein NB, Koster MI, Hoaglin LG, et al. Narrow band ultraviolet B treatment for human vitiligo is associated with proliferation, migration, and differentiation of melanocyte precursors. J Invest Dermatol, 2015,135(8):2068–2076
Birlea SA, Goldstein NB, Norris DA. Repigmentation through melanocyte regeneration in vitiligo. Dermatol Clin, 2017,35(2):205–218
Ostrikov K, Neyts EC, Meyyappan M. Plasma nanoscience: from nano-solids in plasmas to nanoplasmas in solids. Adv Phys, 2013,62(2):113–224
Keidar M, Walk R, Shashurin A, et al. Cold plasma selectivity and the possibility of a paradigm shift in cancer therapy. Br J Cancer, 2011,105(9):1295–1301
Ouf SA, El-Adly AA, Mohamed AH. Inhibitory effect of silver nanoparticles mediated by atmospheric pressure air cold plasma jet against dermatophyte fungi. J Med Microbiol, 2015,64(10):1151–1161
Dubuc A, Monsarrat P, Virard F, et al. Use of cold-atmospheric plasma in oncology: a concise systematic review. Ther Adv Med Oncol, 2018,10:1–12
Zhao SS, Han R, Li Y, et al. Investigation of the mechanism of enhanced and directed differentiation of neural stem cells by an atmospheric plasma jet: A genelevel study. J Appl Phys, 2019,125(16):11
Yan D, Sherman JH, Keidar M. Cold atmospheric plasma, a novel promising anti-cancer treatment modality. Oncotarget, 2017,8(9):15977–15995
Alimoradi H, Greish K, Gamble AB, et al. Controlled delivery of nitric oxide for cancer therapy. Pharm Nanotechnol, 2019,7(4):279–303
Seabra AB, Duran N. Nanoparticulated nitric oxide donors and their biomedical applications. Mini Rev Med Chem, 2017,17(3):216–223
Sharma JN, Al-Omran A, Parvathy SS. Role of nitric oxide in inflammatory diseases. Inflammopharmacology, 2007,15(6):252–259
Dong Y, Cao J, Wang H, et al. Nitric oxide enhances the sensitivity of alpaca melanocytes to respond to alpha-melanocyte-stimulating hormone by up-regulating melanocortin-1 receptor. Biophys Res Commun, 2010,396(4):849–853
Park J, Lee H, Lee HJ, et al. Non-thermal atmospheric pressure plasma efficiently promotes the proliferation of adipose tissue-derived stem cells by activating NO-response pathways. Sci Rep, 2016,6:39298
Jang JY, Hong YJ, Lim J, et al. Cold atmospheric plasma (CAP), a novel physicochemical source, induces neural differentiation through cross-talk between the specific RONS cascade and Trk/Ras/ERK signaling pathway. Biomaterials, 2018,156:258–273
Yang K, Chen J, Jiang W, et al. Conditional immortalization establishes a repertoire of mouse melanocyte progenitors with distinct melanogenic differentiation potential. J Invest Dermatol, 2012,132(10):2479–2483
Petit V, Larue L. Any route for melanoblasts to colonize the skin! Exp Dermatol, 2016,25(9):669–673
Motohashi T, Kunisada T. Melanoblasts as multipotent cells in murine skin. Methods Mol Biol, 2019,1879:257–266
Cichorek M, Wachulska M, Stasiewicz A, et al. Skin melanocytes: biology and development. Postepy Dermatol Alergol, 2013,30(1):30–41
Zhang R, Zhu W. Advance in research of hair follicle-derived melanocyte stem cells. J Clin Dermatol, 2011,40(3):181–183
Vandamme N, Berx G. From neural crest cells to melanocytes: cellular plasticity during development and beyond. Cell Mol Life Sci, 2019,76(10):1919–1934
Yonetani S, Moriyama M, Nishigori C, et al. In vitro expansion of immature melanoblasts and their ability to repopulate melanocyte stem cells in the hair follicle. J Invest Dermatol, 2008,128(2):408–420
Qiu WM, Chuong CM, Lei MX. Regulation of melanocyte stem cells in the pigmentation of skin and its appendages: Biological patterning and therapeutic potentials. Exp Dermatol, 2019,28(4):395–405
Chou WC, Takeo M, Rabbani P, et al. Direct migration of follicular melanocyte stem cells to the epidermis after wounding or UVB irradiation is dependent on Mc1r signaling. Nat Med, 2013,19(7):924–9
Nishimura EK. Melanocyte stem cells: a melanocyte reservoir in hair follicles for hair and skin pigmentation. Pigment Cell Melanoma Res, 2011,24(3):401–410
Liu LJ, Michowski W, Kolodziejczyk A, et al. The cell cycle in stem cell proliferation, pluripotency and differentiation. Nat Cell Biol, 2019,21(9):1060–1067
Wang MA, Cheng XQ, Zhu W, et al. Design of biomimetic and bioactive cold plasma-modified nanostructured scaffolds for enhanced osteogenic differentiation of bone marrow-derived mesenchymal stem cells. Tissue Eng, Part A, 2014,20(5–6):1060–1071
Ermakov A, Ermakova O, Skavulyak A, et al. The effects of the low temperature argon plasma on stem cells proliferation and regeneration in planarians. Plasma Processes Polym, 2016,13(8):788–801
Siu A, Volotskova O, Cheng XQ, et al. Differential effects of cold atmospheric plasma in the treatment of malignant glioma. Plos One, 2015,10(6):14
Xiong Z, Zhao S, Yan X. Nerve stem cell differentiation by a one-step cold atmospheric plasma treatment in vitro. J Vis Exp, 2019,143:e58663
Park J, Lee H, Lee HJ, et al. Non-thermal atmospheric pressure plasma is an excellent tool to activate proliferation in various mesoderm-derived human adult stem cells. Free Radic Biol Med, 2019,134:374–384
Wu H, Park HY. Protein kinase C-beta-mediated complex formation between tyrosinase and TRP-1. Biochem Bioph Res Co, 2003,311(4):948–953
Xiong Z, Zhao S, Mao X, et al. Selective neuronal differentiation of neural stem cells induced by nanosecond microplasma agitation. Stem Cell Res, 2014,12(2):387–399
Elsaadany M, Subramanian G, Ayan H, et al. Exogenous nitric oxide (NO) generated by NO-plasma treatment modulates osteoprogenitor cells early differentiation. J Phys D: Appl Phys, 2015,48(34):345401
Tsatmali M, Graham A, Szatkowski D, et al. alpha-Melanocyte-stimulating hormone modulates nitric oxide production in melanocytes. J Invest Dermatol, 2000,114(3):520–526
Dong Y, Wang H, Cao J, et al. Nitric oxide enhances melanogenesis of alpaca skin melanocytes in vitro by activating the MITF phosphorylation. Mol Cell Biochem, 2011,352(1–2):255–260
Author information
Authors and Affiliations
Corresponding authors
Additional information
Conflict of Interest Statement
The authors declare no potential conflicts of interest.
Rights and permissions
About this article
Cite this article
Nie, Xq., Li, Yh., Zhou, T. et al. Effect of An Atmospheric Plasma Jet on the Differentiation of Melanoblast Progenitor. CURR MED SCI 42, 629–634 (2022). https://doi.org/10.1007/s11596-022-2542-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-022-2542-3