Abstract
Objective
To evaluate the long-term outcome and prognostic factors of patients with nasopharyngeal carcinoma (NPC) from low-endemic regions of China who received definitive intensity-modulated radiation therapy (IMRT).
Methods
The clinical data from 608 patients with newly-diagnosed non-metastatic NPC who have received initial treatment at our cancer center from January, 2008 to December, 2013 were retrospectively reviewed. All patients received definitive IMRT, and 87.7% received platinum-based chemotherapy.
Results
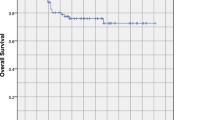
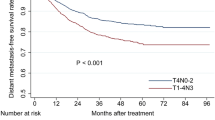
The median follow-up duration was 51 months (follow-up rate, 98.5%; range, 10–106 months) for the entire cohort. The 5-year overall survival rate was 79.7%. The 5-year local relapse-free survival rate, regional relapse-free survival rate, distant metastasis-free survival rate and progression-free survival rate were 92.4%, 93.3%, 79.2% and 74.3%, respectively. A total of 153 patients had experienced treatment failure, with distant metastasis as the primary cause in 77.1% (118/153). Patients with T4 or N3 diseases had a significantly poorer prognosis than other subcategories. Stage T4 and N3 were closely associated with distant metastasis, with the metastatic rate of 29.3% and 45.5%, respectively.
Conclusion
IMRT provides patients with non-metastatic NPC with satisfactory long-term survival. Both T stage and N stage are important prognostic factors for NPC patients. Patients with T4 or N3 diseases have significantly increased distant metastatic rates and poor survival time.
Similar content being viewed by others
References
Sun X, Su S, Chen C, et al. Long-term outcomes of intensity-modulated radiotherapy for 868 patients with nasopharyngeal carcinoma: an analysis of survival and treatment toxicities. Radiother Oncol, 2014,110(3):398–403
Lin S, Lu JJ, Han L, et al. Sequential chemotherapy and intensity-modulated radiation therapy in the management of locoregionally advanced nasopharyngeal carcinoma: experience of 370 consecutive cases. BMC Cancer, 2010,10(1):39
Ou X, Zhou X, Shi Q, et al. Treatment outcomes and late toxicities of 869 patients with nasopharyngeal carcinoma treated with definitive intensity modulated radiation therapy: new insight into the value of total dose of cisplatin and radiation boost. Oncotarget, 2015,6(35):38 381–38 397
Zhang MX, Li J, Shen GP, et al. Intensity-modulated radiotherapy prolongs the survival of patients with nasopharyngeal carcinoma compared with conventional two-dimensional radiotherapy: A 10-year experience with a large cohort and long follow-up. Eur J Cancer, 2015,51(17):2587–2595
Zhao LN, Zhou B, Shi M, et al. Clinical outcome for nasopharyngeal carcinoma with predominantly WHO II histology treated with intensity-modulated radiation therapy in non-endemic region of China. Oral Oncol, 2012,48(9):864–869
Parkin D, Whelan S, Ferlay J, et al. Cancer incidence in five continents. IARC Sci Publications, 2002,155(3):1–781
Thompson L. World Health Organization classification of tumours: pathology and genetics of head and neck tumours. Ear Nose Throat J, 2006,85(2):74
Chen Y, Sun Y, Liang SB, et al. Progress report of a randomized trial comparing long-term survival and late toxicity of concurrent chemoradiotherapy with adjuvant chemotherapy versus radiotherapy alone in patients with stage III to IVB nasopharyngeal carcinoma from endemic regions of China. Cancer, 2013,119(2):2230–2238
Chen Y, Hu XF, Wang Y, et al. Is maximum primary tumor diameter still a prognostic factor in patients with nasopharyngeal carcinoma treated using intensity-modulated radiotherapy? BMC Cancer, 2015,15(1):305
Hwang JM, Fu KK, Phillips TL. Results and prognostic factors in the retreatment of locally recurrent nasopharyngeal carcinoma. Int J Radiat Oncol Biol Phys, 1998,41(5):1099–1111
Al-Sarraf M, LeBlanc M, Giri PG, et al. Chemoradiotherapy versus radiotherapy in patients with advanced nasopharyngeal cancer: phase III randomized Intergroup study 0099. J Clin Oncol, 1998,16(4):1310–1317
Cheng SH, Yen KL, Jian JJ, et al. Examining prognostic factors and patterns of failure in nasopharyngeal carcinoma following concomitant radiotherapy and chemotherapy: impact on future clinical trials. Int J Radiat Oncol Biol Phys, 2001,50(3):717–726
Cheung F, Chan O, Ng WT, et al. The prognostic value of histological typing in nasopharyngeal carcinoma. Oral Oncology, 2012,48(5):429–433
Farias TP, Dias FL, Lima RA, et al. Prognostic factors and outcome for nasopharyngeal carcinoma. Arch Otolaryngol Head Neck Surg, 2003,129(7):794–799
Heng DM, Wee J, Fong KW, et al. Prognostic factors in 677 patients in Singapore with nondisseminated nasopharyngeal carcinoma. Cancer, 1999,86(10):1912–1920
Perez CA, Devineni VR, Marcial-Vega V, et al. Carcinoma of the nasopharynx: factors affecting prognosis. Int J Radiat Oncol Biol Phys, 1992,23(2):271–280
Shanmugaratnam K. Histological typing of nasopharyngeal carcinoma. IARC Sci Publ, 1978, (20):3–12
Wang HY, Chang YL, To KF, et al. A new prognostic histopathologic classification of nasopharyngeal carcinoma. Chin J Cancer, 2016,35(1):41
Jemal A, Bray F, Center MM, et al. Global cancer statistics. CA Cancer J Clin, 2011,61(2):69–90
Chang KP, Chang YT, Wu CC, et al. Multiplexed immunobead-based profiling of cytokine markers for detection of nasopharyngeal carcinoma and prognosis of patient survival. Head Neck, 2011,33(6):886–897
Wang WY, Twu CW, Chen HH, et al. Plasma EBV DNA Clearance Rate as a Novel Prognostic Marker for Metastatic/Recurrent Nasopharyngeal Carcinoma. Clinical Cancer Research, 2010,16(3):1016–1024
Chen L, Mao YP, Xie FY, et al. The seventh edition of the UICC/AJCC staging system for nasopharyngeal carcinoma is prognostically useful for patients treated with intensity-modulated radiotherapy from an endemic area in China. Radiother Oncol, 2012,104(3):331–337
Zong J, Lin S, Lin J, et al. Impact of intensity-modulated radiotherapy on nasopharyngeal carcinoma: Validation of the 7th edition AJCC staging system. Oral Oncology, 2015,51(3):254–259
Kang M, Zhou P, Wei T, et al. A new T staging system for nasopharyngeal carcinoma based on intensity-modulated radiation therapy: results from a prospective multicentric clinical study. Am J Cancer Res, 2017,7(2):346–356
Giuliano A E, Connolly J L, Edge SB, et al. Head and Neck cancers-major changes in the American Joint Committee on cancer eighth edition cancer staging manual. CA Cancer J Clin, 2017,67(2):122–137
Kang M, Zhou P, Li G, et al. Validation of the 8th edition of the UICC/AJCC staging system for nasopharyngeal carcinoma treated with intensity-modulated radiotherapy. Oncotarget, 2017,8(41):70586–70594
Lai SZ, Li WF, Chen L, et al. How does intensity-modulated radiotherapy versus conventional two-dimensional radiotherapy influence the treatment results in nasopharyngeal carcinoma patients? Int J Radiat Oncol Biol Phys, 2011,80(3):661–668
Kang M, Long J, Li G, et al. A new staging system for nasopharyngeal carcinoma based on intensity-modulated radiation therapy: results of a prospective multicentric clinical study. Oncotarget, 2016,7(12):15252–15261
Zhou Q, He Y, Zhao Y, et al. A Study of 358 Cases of Locally Advanced Nasopharyngeal Carcinoma Receiving Intensity-Modulated Radiation Therapy: Improving the Seventh Edition of the American Joint Committee on Cancer T-Staging System. Biomed Res Int, 2017,2017:1419676
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
The authors declare that they have no competing interests.
Author Gang WU is a member of the Editorial Board for Current Medical Science. The paper was handled by the other editor and has undergone rigrous peer review process. Author Gang WU was not involved in the journal’s review of, or decisions related to, this manuscript.
Rights and permissions
About this article
Cite this article
Huang, J., Yang, Zy., Wu, B. et al. Long-term Therapeutic Outcome and Prognostic Factors of Patients with Nasopharyngeal Carcinoma Receiving Intensity-modulated Radiotherapy: An Analysis of 608 Patients from Low-endemic Regions of China. CURR MED SCI 41, 737–745 (2021). https://doi.org/10.1007/s11596-021-2405-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-021-2405-3