Summary
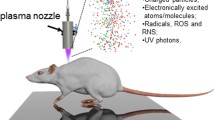
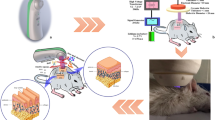
The present study evaluated the effect of non-thermal plasma on skin wound healing in BalB/c mice. Two 6-mm wounds along the both sides of the spine were created on the back of each mouse (n=80) by using a punch biopsy. The mice were assigned randomly into two groups, with 40 animals in each group: a non-thermal plasma group in which the mice were treated with the non-thermal plasma; a control group in which the mice were left to heal naturally. Wound healing was evaluated on postoperative days (POD) 4, 7, 10 and 14 (n=5 per group in each POD) by percentage of wound closure. The mice was euthanized on POD 1, 4, 7, 10, 14, 21, 28 and 35 (n=1 in each POD). The wounds were removed, routinely fixed, paraffin-embedded, sectioned and HE-stained. A modified scoring system was used to evaluate the wounds. The results showed that acute inflammation peaked on POD 4 in non-thermal plasma group, earlier than in control group in which acute inflammation reached a peak on POD 7, and the acute inflammation scores were much lower in non-thermal group than in control group on POD 7 (P<0.05). The amount of granular tissue was greater on POD 4 and 7 in non-thermal group than in control group (P<0.05). The re-epithelialization score and the neovasularization score were increased significantly in non-thermal group when compared with control group on POD 7 and 10 (P<0.05 for all). The count of bacterial colonies was 103 CFU/mL on POD 4 and <20 CFU/mL on POD 7, significantly lower than that in control group (109 CFU/mL on POD 4 and >1012 CFU/mL on the POD 7) (P<0.05). It was suggested that the non-thermal plasma facilitates the wound healing by suppressing bacterial colonization.
Similar content being viewed by others
References
Stoffels E, Sakiyama Y, Graves DB. Cold atmospheric plasma: charged species and their interactions with cells and tissues. IEEE Trans Plasma Sci, 2008,36(4):1441–1457
Ginsberg GG, Barkun AN, Bosco JJ, et al. The argon plasma coagulator. Gastrointestinal Endosc, 2002,55(7): 807–810
Coulombe S, Leveille V, Yonson S, et al. Miniature atmospheric pressure glow discharge torch (APGD-t) for local biomedical applications. Pure Applied Chemistry, 2006,78(6):1147–1156
Kieft IE, Kurdi M, Stoffels E. Reattachment and apoptosis after plasma-needle treatment of cultured cells. IEEE Trans Plasma Sci, 2006,34(4):1331–1336
Fridman G, Peddinghaus M, Ayan H, et al. Blood coagulation and living tissue sterilization by floating-electrode dielectric barrier discharge in air. Plasma Che Plasma P, 2006,26(4):425–442
Fridman G, Shereshevsky A, Peddinghaus M, et al. Bio-medical applications of non-thermal atmospheric pressure plasma, in 37th AIAA Plasmadynamics and Lasers Conference, 2006, San Francisco, California
Gottrup F. Optimizing wound treatment through health care structuring and profession. Wound Rep Reg, 2004,12:129–133
Ekici Y, Emiroglu R, Ozdemir H, et al. Effect of rapamycin on wound healing: an experimental study. Transplant Proc, 2007,39(4):1201–1203
Yilmaz N, Comelekoglu U, Aktas S, et al. Effect of low-energy gallium arsenide (GaAs, 904 nm) laser irradiation on wound healing in rat skin. Wounds, 2006,18(11):323–328
Efron PA, Moldawer LL. Cytokines and wound healing: the role of cytokine and anticytokine therapy in the repair response. J Burn Care Rehabil, 2004,25:149–160
Schwentker A, Vodovotz Y, Weller R, et al. Nitric oxide and wound repair: role of cytokines? Nitric Oxide, 2002, 7(1):1–10
Howdieshell TR, Webb WL, Sathyanarayna, et al. Inhibition of inducible nitric oxide synthase results in reductions in wound vascular endothelial growth factor expression, granulation tissue formation, and local perfusion. Surgery, 2003,133:528–537
Schwentker A, Billiar TR. Nitric oxide and wound repair. Surg Clin North Am, 2003,83:521–530
Bowler PG, Duerden BI, and Armstrong DG. Wound microbiology and associated approaches to wound management. Clin Microbiol Rev, 2001,14:244–269
Monica L. Burts et al. Use of atmospheric non-thermal plasma as a disinfectant for objects contaminated with methicillin-resistant Staphylococcus aureus. Am J Infect Control, 2009,37(9):729–733
Lu XP, Jiang ZH, Xiong Q, et al. A single electrode room-temperature plasma jet device for biomedical applications. Appl Phys Lett, 2008,92(15):1504–1507
Poonawala T, Levay-young BK, Hebbel RP, et al. Opioids heal ischemic wounds in the rat. Wound Rep Reg, 2005,13:165–174
Kawalec JS, Hetherington VJ, Pfennigwerth TC, et al. Effect of a diode laser on wound healing by using diabetic and nondiabetic mice. J Foot Ankle Surg, 2004, 43:214–220
Abramov Y, Golden B, Sullivan M, et al. Histologic characterization of vaginal vs. abdominal surgical wound healing in a rabbit model. Wound Rep Reg, 2007, 15(1):80–86
Henry G, Garner WL. Inflammatory mediators in wound healing. Surg Clin North Am, 2003,83:483–507
O’Kane S. Wound remodelling and scaring. J Wound Care, 2002,11(8):296–299
Werner S, Grose R. Regulation of wound healing by growth factors and cytokines. Physicl Rev, 2003,83:835–870
Author information
Authors and Affiliations
Corresponding author
Additional information
Both authors contributed equally to this work.
The project was supported by grants from the National Natural Sciences Foundation of China (Nos. 10875048, 30700717).
Rights and permissions
About this article
Cite this article
Yu, Y., Tan, M., Chen, H. et al. Non-thermal plasma suppresses bacterial colonization on skin wound and promotes wound healing in mice. J. Huazhong Univ. Sci. Technol. [Med. Sci.] 31, 390–394 (2011). https://doi.org/10.1007/s11596-011-0387-2
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-011-0387-2