Abstract
Purpose
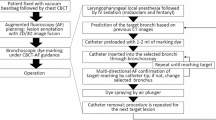
We developed a novel augmented fluoroscopy-guided intrathoracic stamping technique for localizing small pulmonary nodules in the hybrid operating room. We conducted an observational study to investigate the feasibility of this technique and retrospectively compared two augmented fluoroscopy-guided approaches: intrathoracic and transbronchial.
Methods
From August 2020 to March 2023, consecutive patients underwent single-stage augmented fluoroscopy-guided localization under general anaesthesia. This included intrathoracic stamping and bronchoscopic lung marking, followed by thoracoscopic resection in a hybrid operating room. Comparative analyses were performed between the two groups.
Results
The data of 50 patients in the intrathoracic stamping and 67 patients in the bronchoscopic lung marking groups were analysed. No significant difference was noted in demographic data between the groups, except a larger lesion depth in the bronchoscopic lung marking group (14.7 ± 11.7 vs 11.0 ± 5.8 mm, p = 0.029). Dye localization was successfully performed in 49 intrathoracic stamping group patients (98.0%) and 67 bronchoscopic lung marking group patients (100%). No major procedure-related complications occurred in either group; however, the time flow (total anaesthesia time/global operating room time) was longer, and the radiation exposure (fluoroscopy duration/total dose area product) was larger in the bronchoscopic lung marking group.
Conclusions
Augmented fluoroscopic stamping localization under intubated general anaesthesia is feasible and safe, providing an alternative with less global operating room time and lower radiation exposure for image-guided thoracoscopic surgery in the hybrid operating room.




Similar content being viewed by others
Data availability
The authors confirm that the data generated during and/or analysed during the current study and the raw data that support the findings in this study are available from the corresponding author upon reasonable request.
References
National Lung Screening Trial Research Team, Aberle DR, Adams AM, Berg CD, Black WC, Clapp JD, Fagerstrom RM, Gareen IF, Gatsonis C, Marcus PM, Sicks JD (2011) Reduced lung-cancer mortality with low-dose computed tomographic screening. N Engl J Med 365:395–409. https://doi.org/10.1056/NEJMoa1102873
Burzic A, O’Dowd EL, Baldwin DR (2022) The future of lung cancer screening: Current challenges and research priorities. Cancer Manag Res 14:637–645. https://doi.org/10.2147/CMAR.S293877
Lin MW, Chen JS (2016) Image-guided techniques for localizing pulmonary nodules in thoracoscopic surgery. J Thorac Dis 8:S749-S755. https://doi.org/10.21037/jtd.2016.09.71
National Comprehensive Cancer Network (2020) NCCN Clinical Practice Guidelines in Oncology: Lung Cancer Screening; Version 1.2020. www.nccn.org/professionals/physician_gls/f_guidelines.asp. Accessed 6 July 2023
Zhao ZR, Lau RW, Ng CS (2016) Hybrid theatre and alternative localization techniques in conventional and single-port video-assisted thoracoscopic surgery. J Thorac Dis 8:S319-327. https://doi.org/10.3978/j.issn.2072-1439.2016.02.27
Yang SM, Ko WC, Lin MW, Hsu HH, Chan CY, Wu IH, Chang YC, Chen JS (2016) Image-guided thoracoscopic surgery with dye localization in a hybrid operating room. J Thorac Dis 8:S681–S689. https://doi.org/10.21037/jtd.2016.09.55
Lempel JK, Raymond DP (2019) Intraoperative percutaneous microcoil localization of small peripheral pulmonary nodules using cone-beam CT in a hybrid operating room. AJR Am J Roentgenol 213:778–781. https://doi.org/10.2214/AJR.19.21175
Leow OQY, Chao YK (2019) Individualized strategies for intraoperative localization of non-palpable pulmonary nodules in a hybrid operating room. Front Surg 6:32. https://doi.org/10.3389/fsurg.2019.00032
Park CH, Han K, Hur J, Lee SM, Lee JW, Hwang SH, Seo JS, Lee KH, Kwon W, Kim TH, Choi BW (2017) Comparative effectiveness and safety of preoperative lung localization for pulmonary nodules: a systematic review and meta-analysis. Chest 151:316–328. https://doi.org/10.1016/j.chest.2016.09.017
Chi CL, Gao X, Tai CC, Chao YK (2022) Preoperative percutaneous localization of multiple ipsilateral pulmonary nodules: a systematic review. Formos J Surg 55:81–86. https://doi.org/10.4103/fjs.fjs_108_22
Starnes SL, Wolujewicz M, Guitron J, Williams V, Scheler J, Ristagno R (2018) Radiotracer localization of nonpalpable pulmonary nodules: a single-centre experience. J Thorac Cardiovasc Surg 156:1986–1992. https://doi.org/10.1016/j.jtcvs.2018.03.152
Saito Y (2022) Recent advances in electromagnetic navigation bronchoscopy for localization of peripheral pulmonary nodules. J Thorac Dis 14:802–804. https://doi.org/10.21037/jtd-22-179
Yang SM, Yu KL, Lin JH, Lin KS, Liu YL, Sun SE, Meng LH, Ko HJ (2019) Cumulative experience of preoperative real-time augmented fluoroscopy-guided endobronchial dye marking for small pulmonary nodules: an analysis of 30 initial patients. J Formos Med Assoc 118:1232–1238. https://doi.org/10.1016/j.jfma.2019.04.017
Hogarth DK (2018) Use of augmented fluoroscopic imaging during diagnostic bronchoscopy. Future Oncol 14:2247–2252. https://doi.org/10.2217/fon-2017-0686
Cicenia J, Bhadra K, Sethi S, Nader DA, Whitten P, Hogarth DK (2021) Augmented fluoroscopy: a new and novel navigation platform for peripheral bronchoscopy. J Bronchology Interv Pulmonol 28:116–123. https://doi.org/10.1097/LBR.0000000000000722
Yang SM, Yu KL, Lin KH, Liu YL, Sun SE, Meng LH, Ko HJ (2020) Real-time augmented fluoroscopy-guided lung marking for thoracoscopic resection of small pulmonary nodules. Surg Endosc 34:477–484. https://doi.org/10.1007/s00464-019-06972-y
Kawada M, Okubo T, Poudel S, Suzuki Y, Kawarada Y, Kitashiro S, Okushiba S, Katoh H (2013) A new marking technique for peripheral lung nodules avoiding pleural puncture: the intrathoracic stamping method. Interact Cardiovasc Thorac Surg 16:381–383. https://doi.org/10.1093/icvts/ivs521
Yang SM, Chung WY, Ko HJ, Chen LC, Chang LK, Chang HC, Kuo SW, Ho MC (2023) Single-stage augmented fluoroscopic bronchoscopy localization and thoracoscopic resection of small pulmonary nodules in a hybrid operating room. Eur J Cardiothorac Surg 63:ezac541. https://doi.org/10.1093/ejcts/ezac541
Yang SM, Yu KL, Lin KS, Liu YL, Sun SE, Meng LH, Ko HJ (2020) Localization of small pulmonary nodules using augmented fluoroscopic bronchoscopy: experience from 100 consecutive cases. World J Surg 44:2418–2425. https://doi.org/10.1007/s00268-020-05434-0
Kamiyoshihara M, Ibe T, Kawatani N, Ohsawa F, Yoshikawa R, Shimizu K (2016) A convenient method for identifying a small pulmonary nodule using a dyed swab and geometric mapping. J Thorac Dis 44:2418–2425. https://doi.org/10.21037/jtd.2016.08.62
Fujikawa R, Otsuki Y, Nakamura H, Funai K, Nakamura T (2020) Marking method for peripheral non-palpable pulmonary nodules using a mobile computed tomography scanner with a navigation system. Gen Thorac Cardiovas Surg 68:1220–1223. https://doi.org/10.1007/s11748-020-01332-3
Saito Y, Watanabe T, Kanamoto Y, Asami M, Yokote F, Dejima H, Morooka H, Ibi T, Yamauchi Y, Takahashi N, Ikeya T, Sakao Y, Kawamura M (2022) A pilot study of intraoperative localization of peripheral small pulmonary tumors by cone-beam computed tomography: sandwich marking technique. J Thorac Dis 14:2845–2854. https://doi.org/10.21037/jtd-22-190
Nagano M, Sato M (2023) Ten-year outcome and development of virtual-assisted lung mapping in thoracic surgery. Cancers (Basel) 15:1971. https://doi.org/10.3390/cancers15071971
Acknowledgements
This work was supported by a grant from the National Taiwan University Hospital, Hsin-Chu Branch, Taiwan [Grant Number 111-BIH008].
Author information
Authors and Affiliations
Contributions
Shun-Mao Yang: Conceptualization; Data curation; Formal analysis; Funding acquisition; Investigation; Methodology; Project administration; Resources; Software; Validation; Visualization; Writing—original draft; Writing—review & editing. Shwetambara Malwade: Investigation; Methodology; Data curation; Writing—original draft; Writing—review & editing. Wen-Yuan Chung: Data curation; Formal analysis; Project administration; Software; Visualization. Wen-Ting Wu: Data curation; Formal analysis; Project administration. Lun-Che Chen: Data curation; Formal analysis; Investigation; Project administration; Validation; Writing—review & editing. Ling-Kai Chang: Data curation; Formal analysis; Investigation; Methodology; Visualization; Writing—review & editing. Hao-Chun Chang: Data curation; Formal analysis; Investigation; Project administration; Writing—review & editing. Pak-Si Chan: Conceptualization; Data curation; Investigation; Project administration; Writing—review & editing. Shuenn-Wen Kuo: Conceptualization; Investigation; Methodology; Supervision; Writing—review & editing. All authors approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
Shwetambara Malwade works for Siemens Healthcare as a research scientist. Shun-Mao Yang, Wen-Yuan Chung, Wen-Ting Wu, Lun-Che Chen, Ling-Kai Chang, Hao-Chun Chang, Pak-Si Chan, and Shuenn-Wen Kuo have no conflicts of interest or financial ties to disclose.
Ethical approval
This study was performed in accordance with the principles of the Declaration of Helsinki and its later amendments. Approval was granted by the Research Ethics Committee of the National Taiwan University Hospital (approval number: 202304131RINC).
Informed consent
Individual consent for this retrospective analysis was waived.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yang, SM., Malwade, S., Chung, WY. et al. Augmented fluoroscopy-guided dye localization for small pulmonary nodules in hybrid operating room: intrathoracic stamping versus transbronchial marking. Int J CARS (2024). https://doi.org/10.1007/s11548-024-03146-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11548-024-03146-7