Abstract
Purpose
Accurately predicting the treatment response in patients with Crohn’s disease (CD) receiving infliximab therapy is crucial for clinical decision-making. We aimed to construct a prediction model incorporating radiomics and body composition features derived from computed tomography (CT) enterography for identifying individuals at high risk for infliximab treatment failure.
Methods
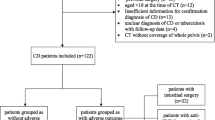
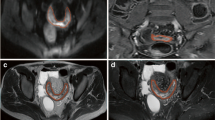
This retrospective study included 137 patients with CD between 2015 and 2021, who were divided into a training cohort and a validation cohort with a ratio of 7:3. Patients underwent CT enterography examinations within 1 month before infliximab initiation. Radiomic features of the intestinal segments involved were extracted, and body composition features were measured at the level of the L3 lumbar vertebra. A model that combined radiomics with body composition was constructed. The primary outcome was the occurrence of infliximab treatment failure within 1 year. The model performance was evaluated using discrimination, calibration, and decision curves.
Results
Fifty-two patients (38.0%) showed infliximab treatment failure. Eight significant radiomic features were used to develop the radiomics model. The model incorporating radiomics model score, skeletal muscle index (SMI), and creeping fat showed good discrimination for predicting infliximab treatment failure, with an area under the curve (AUC) of 0.88 (95% CI 0.81, 0.95) in the training cohort and 0.83 (95% CI 0.66, 1.00) in the validation cohort. The favorable clinical application was observed using decision curve analysis.
Conclusions
We constructed a comprehensive model incorporating radiomics and muscle volume, which could potentially be used to facilitate the individualized prediction of infliximab treatment response in patients with CD.




Similar content being viewed by others
Data availability
Data are available upon reasonable request and pursuant to appropriate agreements.
References
Torres J, Mehandru S, Colombel JF, Peyrin-Biroulet L (2017) Crohn’s disease. Lancet 389(10080):1741–1755. https://doi.org/10.1016/S0140-6736(16)31711-1
Peyrin-Biroulet L, Loftus EV Jr, Colombel JF, Sandborn WJ (2010) The natural history of adult Crohn’s disease in population-based cohorts. Am J Gastroenterol 105(2):289–297. https://doi.org/10.1038/ajg.2009.579
Leal RF, Planell N, Kajekar R, Lozano JJ, Ordas I, Dotti I, Esteller M, Masamunt MC, Parmar H, Ricart E, Panes J, Salas A (2015) Identification of inflammatory mediators in patients with Crohn’s disease unresponsive to anti-TNFalpha therapy. Gut 64(2):233–242. https://doi.org/10.1136/gutjnl-2013-306518
Torres J, Bonovas S, Doherty G, Kucharzik T, Gisbert JP, Raine T, Adamina M, Armuzzi A, Bachmann O, Bager P, Biancone L, Bokemeyer B, Bossuyt P, Burisch J, Collins P, El-Hussuna A, Ellul P, Frei-Lanter C, Furfaro F, Gingert C, Gionchetti P, Gomollon F, Gonzalez-Lorenzo M, Gordon H, Hlavaty T, Juillerat P, Katsanos K, Kopylov U, Krustins E, Lytras T, Maaser C, Magro F, Marshall JK, Myrelid P, Pellino G, Rosa I, Sabino J, Savarino E, Spinelli A, Stassen L, Uzzan M, Vavricka S, Verstockt B, Warusavitarne J, Zmora O, Fiorino G (2020) ECCO guidelines on therapeutics in Crohn’s disease: medical treatment. J Crohns Colitis 14(1):4–22. https://doi.org/10.1093/ecco-jcc/jjz180
Cushing K, Higgins PDR (2021) Management of Crohn disease: a review. JAMA 325(1):69–80. https://doi.org/10.1001/jama.2020.18936
Singh S, Fumery M, Sandborn WJ, Murad MH (2018) Systematic review and network meta-analysis: first- and second-line biologic therapies for moderate-severe Crohn’s disease. Aliment Pharmacol Ther 48(4):394–409. https://doi.org/10.1111/apt.14852
Allez M, Karmiris K, Louis E, Van Assche G, Ben-Horin S, Klein A, Van der Woude J, Baert F, Eliakim R, Katsanos K, Brynskov J, Steinwurz F, Danese S, Vermeire S, Teillaud JL, Lemann M, Chowers Y (2010) Report of the ECCO pathogenesis workshop on anti-TNF therapy failures in inflammatory bowel diseases: definitions, frequency and pharmacological aspects. J Crohns Colitis 4(4):355–366. https://doi.org/10.1016/j.crohns.2010.04.004
Schreiber S, Colombel JF, Bloomfield R, Nikolaus S, Scholmerich J, Panes J, Sandborn WJ, Investigators PRS (2010) Increased response and remission rates in short-duration Crohn’s disease with subcutaneous certolizumab pegol: an analysis of PRECiSE 2 randomized maintenance trial data. Am J Gastroenterol 105(7):1574–1582. https://doi.org/10.1038/ajg.2010.78
Gisbert JP, Panes J (2009) Loss of response and requirement of infliximab dose intensification in Crohn’s disease: a review. Am J Gastroenterol 104(3):760–767. https://doi.org/10.1038/ajg.2008.88
Li L, Chen R, Zhang Y, Zhou G, Chen B, Zeng Z, Chen M, Zhang S (2021) A novel model based on serum biomarkers to predict primary non-response to infliximab in Crohn’s disease. Front Immunol 12:646673. https://doi.org/10.3389/fimmu.2021.646673
Zapater P, Almenara S, Gutierrez A, Sempere L, Garcia M, Laveda R, Martinez A, Scharl M, Cameo JI, Linares R, Gonzalez-Navajas JM, Wiest R, Rogler G, Frances R (2019) Actual anti-TNF trough levels relate to serum IL-10 in drug-responding patients with Crohn’s disease. Inflamm Bowel Dis 25(8):1357–1366. https://doi.org/10.1093/ibd/izz012
Kennedy NA, Heap GA, Green HD, Hamilton B, Bewshea C, Walker GJ, Thomas A, Nice R, Perry MH, Bouri S, Chanchlani N, Heerasing NM, Hendy P, Lin S, Gaya DR, Cummings JRF, Selinger CP, Lees CW, Hart AL, Parkes M, Sebastian S, Mansfield JC, Irving PM, Lindsay J, Russell RK, McDonald TJ, McGovern D, Goodhand JR, Ahmad T, Group UKIBDPS (2019) Predictors of anti-TNF treatment failure in anti-TNF-naive patients with active luminal Crohn’s disease: a prospective, multicentre, cohort study. Lancet Gastroenterol Hepatol 4(5):341–353. https://doi.org/10.1016/S2468-1253(19)30012-3
Gisbert JP, Chaparro M (2020) Predictors of primary response to biologic treatment [Anti-TNF, Vedolizumab, and Ustekinumab] in patients with inflammatory bowel disease: from basic science to clinical practice. J Crohns Colitis 14(5):694–709. https://doi.org/10.1093/ecco-jcc/jjz195
Bruining DH, Zimmermann EM, Loftus EV Jr, Sandborn WJ, Sauer CG, Strong SA, Society of Abdominal Radiology Crohn’s Disease-Focused P (2018) Consensus recommendations for evaluation, interpretation, and utilization of computed tomography and magnetic resonance enterography in patients with small bowel Crohn’s disease. Radiology 286(3):776–799. https://doi.org/10.1148/radiol.2018171737
Ognibene NM, Basile M, Di Maurizio M, Petrillo G, De Filippi C (2016) Features and perspectives of MR enterography for pediatric Crohn disease assessment. Radiol Med 121(5):362–377. https://doi.org/10.1007/s11547-015-0613-2
Cicero G, Alibrandi A, Blandino A, Ascenti V, Fries W, Viola A, Mazziotti S (2023) DWI ratios: New indexes for Crohn’s disease activity at magnetic resonance enterography? Radiol Med (Torino) 128(1):16–26. https://doi.org/10.1007/s11547-022-01573-7
Napolitano M, Munari AM, Di Leo G, Panarisi NAR, Zuin G, Fava G, Vecchi M, Sardanelli F, Zuccotti GV (2021) MR enterography grading of pediatric ileocolonic Crohn disease activity based on a single bowel segment. Radiol Med (Torino) 126(11):1396–1406. https://doi.org/10.1007/s11547-021-01409-w
Rimola J, Torres J, Kumar S, Taylor SA, Kucharzik T (2022) Recent advances in clinical practice: advances in cross-sectional imaging in inflammatory bowel disease. Gut 71(12):2587–2597. https://doi.org/10.1136/gutjnl-2021-326562
Baker ME, Hara AK, Platt JF, Maglinte DD, Fletcher JG (2015) CT enterography for Crohn’s disease: optimal technique and imaging issues. Abdom Imaging 40(5):938–952. https://doi.org/10.1007/s00261-015-0357-4
Lambin P, Rios-Velazquez E, Leijenaar R, Carvalho S, van Stiphout RGPM, Granton P, Zegers CML, Gillies R, Boellard R, Dekker A, Aerts HJWL (2012) Radiomics: extracting more information from medical images using advanced feature analysis. Eur J Cancer 48(4):441–446. https://doi.org/10.1016/j.ejca.2011.11.036
Gillies RJ, Kinahan PE, Hricak H (2016) Radiomics: images are more than pictures. They Are Data Radiology 278(2):563–577. https://doi.org/10.1148/radiol.2015151169
Zhu C, Hu J, Wang X, Li C, Gao Y, Li J, Ge Y, Wu X (2022) A novel clinical radiomics nomogram at baseline to predict mucosal healing in Crohn’s disease patients treated with infliximab. Eur Radiol 32(10):6628–6636. https://doi.org/10.1007/s00330-022-08989-9
Li X, Liang D, Meng J, Zhou J, Chen Z, Huang S, Lu B, Qiu Y, Baker ME, Ye Z, Cao Q, Wang M, Yuan C, Chen Z, Feng S, Zhang Y, Iacucci M, Ghosh S, Rieder F, Sun C, Chen M, Li Z, Mao R, Huang B, Feng ST (2021) Development and validation of a novel computed-tomography enterography radiomic approach for characterization of intestinal fibrosis in Crohn’s disease. Gastroenterology 160(7):2303–2316. https://doi.org/10.1053/j.gastro.2021.02.027
Cruz-Jentoft AJ, Sayer AA (2019) Sarcopenia. Lancet 393(10191):2636–2646. https://doi.org/10.1016/S0140-6736(19)31138-9
Ryan E, McNicholas D, Creavin B, Kelly ME, Walsh T, Beddy D (2019) Sarcopenia and inflammatory bowel disease: a systematic review. Inflamm Bowel Dis 25(1):67–73. https://doi.org/10.1093/ibd/izy212
Grillot J, D’Engremont C, Parmentier AL, Lakkis Z, Piton G, Cazaux D, Gay C, De Billy M, Koch S, Borot S, Vuitton L (2020) Sarcopenia and visceral obesity assessed by computed tomography are associated with adverse outcomes in patients with Crohn’s disease. Clin Nutr 39(10):3024–3030. https://doi.org/10.1016/j.clnu.2020.01.001
Adams DW, Gurwara S, Silver HJ, Horst SN, Beaulieu DB, Schwartz DA, Seidner DL (2017) Sarcopenia is common in overweight patients with inflammatory bowel disease and may predict need for surgery. Inflamm Bowel Dis 23(7):1182–1186. https://doi.org/10.1097/MIB.0000000000001128
Holt DQ, Varma P, Strauss BJG, Rajadurai AS, Moore GT (2017) Low muscle mass at initiation of anti-TNF therapy for inflammatory bowel disease is associated with early treatment failure: a retrospective analysis. Eur J Clin Nutr 71(6):773–777. https://doi.org/10.1038/ejcn.2017.10
Maaser C, Sturm A, Vavricka SR, Kucharzik T, Fiorino G, Annese V, Calabrese E, Baumgart DC, Bettenworth D, Borralho Nunes P, Burisch J, Castiglione F, Eliakim R, Ellul P, Gonzalez-Lama Y, Gordon H, Halligan S, Katsanos K, Kopylov U, Kotze PG, Krustins E, Laghi A, Limdi JK, Rieder F, Rimola J, Taylor SA, Tolan D, van Rheenen P, Verstockt B, Stoker J, European CS, Colitis O, Abdominal R (2019) ECCO-ESGAR guideline for diagnostic assessment in IBD Part 1: initial diagnosis, monitoring of known IBD, detection of complications. J Crohns Colitis 13(2):144–164. https://doi.org/10.1093/ecco-jcc/jjy113
Campbell JP, Teigen L, Manski S, Blumhof B, Guglielmo FF, Shivashankar R, Shmidt E (2022) Sarcopenia is more prevalent among inflammatory bowel disease patients undergoing surgery and predicts progression to surgery among medically treated patients. Inflamm Bowel Dis 28(12):1844–1850. https://doi.org/10.1093/ibd/izac013
Montano-Loza AJ, Mazurak VC, Ebadi M, Meza-Junco J, Sawyer MB, Baracos VE, Kneteman N (2018) Visceral adiposity increases risk for hepatocellular carcinoma in male patients with cirrhosis and recurrence after liver transplant. Hepatology 67(3):914–923. https://doi.org/10.1002/hep.29578
Mourtzakis M, Prado CM, Lieffers JR, Reiman T, McCargar LJ, Baracos VE (2008) A practical and precise approach to quantification of body composition in cancer patients using computed tomography images acquired during routine care. Appl Physiol Nutr Metab 33(5):997–1006. https://doi.org/10.1139/H08-075
Yueying C, Jing F, Qi F, Jun S (2023) Infliximab response associates with radiologic findings in bio-naive Crohn’s disease. Eur Radiol. https://doi.org/10.1007/s00330-023-09542-y
Zhu C, Wang X, Wang S, Hu J, Gao Y, Li C, Li J, Wu X (2023) Development and validation of a clinical radiomics nomogram to predict secondary loss of response to infliximab in Crohn’s disease patients. Heliyon 9(4):e14594. https://doi.org/10.1016/j.heliyon.2023.e14594
Ordas I, Rimola J, Alfaro I, Rodriguez S, Castro-Poceiro J, Ramirez-Morros A, Gallego M, Giner A, Barastegui R, Fernandez-Clotet A, Masamunt M, Ricart E, Panes J (2019) Development and validation of a simplified magnetic resonance index of activity for Crohn’s disease. Gastroenterology 157(2):432–439. https://doi.org/10.1053/j.gastro.2019.03.051
Lafeuille P, Hordonneau C, Vignette J, Blayac L, Dapoigny M, Reymond M, Rouquette O, Sollelis E, Boube M, Magnin B, Pereira B, Buisson A (2021) Transmural healing and MRI healing are associated with lower risk of bowel damage progression than endoscopic mucosal healing in Crohn’s disease. Aliment Pharmacol Ther 53(5):577–586. https://doi.org/10.1111/apt.16232
Minordi LM, Larosa L, Barbaro B, Angelino A, Broglia D, Cipri C, Scaldaferri F, Manfredi R, Natale L (2023) How the radiologist must reason for a correct diagnosis in patients with small bowel mural thickening studied by CT or MRI: a pictorial review. Curr Probl Diagn Radiol 52(5):393–411. https://doi.org/10.1067/j.cpradiol.2023.03.006
Vilela EG (2012) Evaluation of inflammatory activity in Crohn’s disease and ulcerative colitis. World J Gastroenterol. https://doi.org/10.3748/wjg.v18.i9.872
Guglielmo FF, Anupindi SA, Fletcher JG, Al-Hawary MM, Dillman JR, Grand DJ, Bruining DH, Chatterji M, Darge K, Fidler JL, Gandhi NS, Gee MS, Grajo JR, Huang C, Jaffe TA, Park SH, Rimola J, Soto JA, Taouli B, Taylor SA, Baker ME (2020) Small bowel crohn disease at CT and MR enterography: imaging atlas and glossary of terms. Radiographics 40(2):354–375. https://doi.org/10.1148/rg.2020190091
Bettenworth D, Bokemeyer A, Baker M, Mao R, Parker CE, Nguyen T, Ma C, Panés J, Rimola J, Fletcher JG, Jairath V, Feagan BG, Rieder F (2019) Assessment of Crohn’s disease-associated small bowel strictures and fibrosis on cross-sectional imaging: a systematic review. Gut 68(6):1115–1126. https://doi.org/10.1136/gutjnl-2018-318081
Chirra P, Sharma A, Bera K, Cohn HM, Kurowski JA, Amann K, Rivero MJ, Madabhushi A, Lu C, Paspulati R, Stein SL, Katz JA, Viswanath SE, Dave M (2022) Integrating radiomics with clinicoradiological scoring can predict high-risk patients who need surgery in Crohn’s disease: a pilot study. Inflamm Bowel Dis. https://doi.org/10.1093/ibd/izac211
Li XH, Feng ST, Cao QH, Coffey JC, Baker ME, Huang L, Fang ZN, Qiu Y, Lu BL, Chen ZH, Li Y, Bettenworth D, Iacucci M, Sun CH, Ghosh S, Rieder F, Chen MH, Li ZP, Mao R (2021) Degree of creeping fat assessed by computed tomography enterography is associated with intestinal fibrotic stricture in patients with Crohn’s disease: a potentially novel mesenteric creeping fat index. J Crohns Colitis 15(7):1161–1173. https://doi.org/10.1093/ecco-jcc/jjab005
Ha CWY, Martin A, Sepich-Poore GD, Shi B, Wang Y, Gouin K, Humphrey G, Sanders K, Ratnayake Y, Chan KSL, Hendrick G, Caldera JR, Arias C, Moskowitz JE, Ho Sui SJ, Yang S, Underhill D, Brady MJ, Knott S, Kaihara K, Steinbaugh MJ, Li H, McGovern DPB, Knight R, Fleshner P, Devkota S (2020) Translocation of viable gut microbiota to mesenteric adipose drives formation of creeping fat in humans. Cell 183(3):666–683. https://doi.org/10.1016/j.cell.2020.09.009
Chang JT (2020) Pathophysiology of inflammatory bowel diseases. N Engl J Med 383(27):2652–2664. https://doi.org/10.1056/NEJMra2002697
Caenepeel C, Sadat Seyed Tabib N, Vieira-Silva S, Vermeire S (2020) Review article: how the intestinal microbiota may reflect disease activity and influence therapeutic outcome in inflammatory bowel disease. Aliment Pharmacol Ther 52(9):1453–1468. https://doi.org/10.1111/apt.16096
Acknowledgements
Thanks to Professor Liu Zhenguo who played an important role in the revision process of the paper and helped with the language revision.
Funding
This work was supported by the National Natural Science Foundation of China (81771827 and 82071986), the Science and Technology Project of Hunan Province (2021RC4017), the Furong Scholars Programme of Hunan Province (2022), and the Wisdom Accumulation and Talent Cultivation Project of the Third Xiangya Hospital of Central South University (2020).
Author information
Authors and Affiliations
Contributions
All authors approved the final version of the article, including the authorship list. The scientific guarantor of this publication is FS who performed data analysis, figure visualizations, and initial draft writing. MM and ZF kindly provided statistical advice for this manuscript. PR and ZF provided clinical input on experimental design, assistance in editing the manuscript and jointly conceived and supervised the project, designed the experiments, oversaw the analysis, and wrote and edited the final manuscript. WH, FS, and SZ performed detailed chart review, extracted clinical variables, quality evaluation, and radiomic analysis of CT enterography scans.
Corresponding authors
Ethics declarations
Conflict of interest
The authors of this manuscript declare no relevant financial disclosures or conflicts of interest. The authors confirm that the article is not under consideration for publication elsewhere. Each author has participated sufficiently to take public responsibility for the manuscript content.
Ethical approval
Institutional Review Board approval from the Ethics Committee of The Third Xiangya Hospital of Central South University (Changsha, China) was obtained.
Informed consent
Informed consent was waived for the retrospective nature of the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Song, F., Ma, M., Zeng, S. et al. CT enterography-based radiomics combined with body composition to predict infliximab treatment failure in Crohn’s disease. Radiol med 129, 175–187 (2024). https://doi.org/10.1007/s11547-023-01748-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-023-01748-w