Abstract
Purpose
To determine the incidence and clinical relevance of extra-intestinal incidental findings (IF) in a cohort of patients with proven or suspected Crohn disease (CD) examined with magnetic resonance enterography (MR-E) in a single University Centre.
Methods
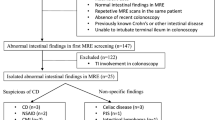
Between January 2018 and June 2019, 182 patients with proven or suspected CD with a planned first MR-E examination, were retrospectively included in this study. Incidental findings were considered as any abnormality identified in the absence of previous clinically suspected or known disease. IF were categorized as unremarkable, benign or potentially relevant findings requiring further imaging or specific treatment.
Results
Of the 182 revised MR-E, extra-intestinal IF were recorded in 70 cases (38.5%); 35 (50%) incidental lesions were recognized as non-significant, 24 (34%) as benign and 11 (16%) as clinically relevant. Moreover, there was a positive correlation between IF and patients’ age (p < 0.0001).
Conclusions
In our experience, a high number of IF (38.5%) was found, with a prevalence that increases with patients’ age. Clinically relevant findings were found in 16% of MR-E. This means that MR-E is a useful tool to detect IF, therefore, the presence of a radiologist during the image acquisition is crucial in adding sequences to the examination.



Similar content being viewed by others
References
Kim SH (2015) Computed tomography enterography and magnetic resonance enterography in the diagnosis of Crohn’s disease. Intest Res 13(1):27–38. https://doi.org/10.5217/ir.2015.13.1.27
Masselli G, Casciani E, Polettini E, Gualdi G (2008) Comparison of MR enteroclysis with MR enterography and conventional enteroclysis in patients with Crohn’s disease. Eur Radiol 18(3):438–447. https://doi.org/10.1007/s00330-007-0763-2
Laghi A, Borrelli O, Paolantonio P, Dito L, Buena de Mesquita M, Falconieri P, Passariello R, Cucchiara S (2003) Contrast enhanced magnetic resonance imaging of the terminal ileum in children with Crohn’s disease. Gut 52(3):393–397
Ognibene NM, Basile M, Di Maurizio M, Petrillo G, De Filippi C (2016) Features and perspectives of MR enterography for pediatric Crohn disease assessment. Radiol Med 121(5):362–377. https://doi.org/10.1007/s11547-015-0613-2
Macarini L, Stoppino LP, Centola A, Muscarella S, Fortunato F, Coppolino F, Della Valle N, Ierardi V, Milillo P, Vinci R (2013) Assessment of activity of Crohn’s disease of the ileum and large bowel: proposal for a new multiparameter MR enterography score. Radiol Med 118(2):181–195. https://doi.org/10.1007/s11547-012-0841-7
Tolan DJ, Greenhalgh R, Zealley IA, Halligan S, Taylor SA (2010) MR enterographic manifestations of small bowel Crohn disease. Radiographics 30(2):367–384
Scardapane A, Ambrosi A, Salinaro E, Mancini ME, Principi M, Di Leo A, Lorusso F, Stabile Ianora AA, Angelelli G (2015) Assessment of disease activity in small Bowel Crohn’s disease: comparison between endoscopy and magnetic resonance enterography using MRIA and modified MRIA score. Gastroenterol Res Pract 2015:1–7. https://doi.org/10.1155/2015/159641
Fujii T, Naganuma M, Kitazume Y, Saito E, Nagahori M, Ohtsuka K, Watanabe M (2014) Advancing magnetic resonance imaging in Crohn’s disease. Digestion 89(1):24–30. https://doi.org/10.1159/000356210
Athanasakos A, Mazioti A, Economopoulos N, Kontopoulou C, Stathis G, Filippiadis D, Spyridopoulos T, Alexopoulou E (2015) Inflammatory bowel disease-the role of cross-sectional imaging techniques in the investigation of the small bowel. Insights Imaging 6(1):73–83. https://doi.org/10.1007/s13244-014-0377-6
Jensen MD, Nathan T, Kjeldsen J, Rafaelsen SR (2010) Incidental findings at MRI-enterography in patients with suspected or known Crohn’s disease. World J Gastroenterol 16(1):76–82
Herfarth HH, Grunert M, Klebl F, Strauch U, Feuerbach S, Scholmerich J, Rogler G, Schreyer AG (2009) Frequency and nature of incidental extra-enteric lesions found on magnetic resonance enterography (MR-E) in patients with inflammatory bowel diseases (IBD). PLoS ONE 4(4):e4863. https://doi.org/10.1371/journal.pone.0004863
Machaalany J, Yam Y, Ruddy TD, Abraham A, Chen L, Beanlands RS, Chow BJ (2009) Potential clinical and economic consequences of noncardiac incidental findings on cardiac computed tomography. J Am Coll Cardiol 54(16):1533–1541. https://doi.org/10.1016/j.jacc.2009.06.026
Stone JH (2006) Incidentalomas–clinical correlation and translational science required. N Engl J Med 354(26):2748–2749. https://doi.org/10.1056/NEJMp058264
Patel MD, Ascher SM, Paspulati RM, Shanbhogue AK, Siegelman ES, Stein MW, Berland LL (2013) Managing incidental findings on abdominal and pelvic CT and MRI, part 1: white paper of the ACR Incidental Findings Committee II on adnexal findings. J Am Coll Radiol 10(9):675–681. https://doi.org/10.1016/j.jacr.2013.05.023
Khosa F, Krinsky G, Macari M, Yucel EK, Berland LL (2013) Managing incidental findings on abdominal and pelvic CT and MRI, Part 2: white paper of the ACR Incidental Findings Committee II on vascular findings. J Am Coll Radiol 10(10):789–794. https://doi.org/10.1016/j.jacr.2013.05.021
Heller MT, Harisinghani M, Neitlich JD, Yeghiayan P, Berland LL (2013) Managing incidental findings on abdominal and pelvic CT and MRI, part 3: white paper of the ACR Incidental Findings Committee II on splenic and nodal findings. J Am Coll Radiol 10(11):833–839. https://doi.org/10.1016/j.jacr.2013.05.020
Sebastian S, Araujo C, Neitlich JD, Berland LL (2013) Managing incidental findings on abdominal and pelvic CT and MRI, Part 4: white paper of the ACR Incidental Findings Committee II on gallbladder and biliary findings. J Am Coll Radiol 10(12):953–956. https://doi.org/10.1016/j.jacr.2013.05.022
Berland LL (2013) Overview of white papers of the ACR incidental findings committee ii on adnexal, vascular, splenic, nodal, gallbladder, and biliary findings. J Am Coll Radiol 10(9):672–674. https://doi.org/10.1016/j.jacr.2013.05.012
Parker LS (2008) The future of incidental findings: should they be viewed as benefits. J Law Med Ethics 36(2):341–351. https://doi.org/10.1111/j.1748-720x.2008.00278.x
Reiner BI (2009) The challenges, opportunities, and imperative of structured reporting in medical imaging. J Digit Imaging 22(6):562–568. https://doi.org/10.1007/s10278-009-9239-z
Berland LL, Silverman SG, Gore RM, Mayo-Smith WW, Megibow AJ, Yee J, Brink JA, Baker ME, Federle MP, Foley WD, Francis IR, Herts BR, Israel GM, Krinsky G, Platt JF, Shuman WP, Taylor AJ (2010) Managing incidental findings on abdominal CT: white paper of the ACR incidental findings committee. J Am Coll Radiol 7(10):754–773. https://doi.org/10.1016/j.jacr.2010.06.013
Hellstrom M, Svensson MH, Lasson A (2004) Extracolonic and incidental findings on CT colonography (virtual colonoscopy). AJR Am J Roentgenol 182(3):631–638. https://doi.org/10.2214/ajr.182.3.1820631
Hassan C, Pickhardt PJ, Laghi A, Kim DH, Zullo A, Iafrate F, Di Giulio L, Morini S (2008) Computed tomographic colonography to screen for colorectal cancer, extracolonic cancer, and aortic aneurysm: model simulation with cost-effectiveness analysis. Arch Intern Med 168(7):696–705. https://doi.org/10.1001/archinte.168.7.696
Hara AK, Johnson CD, MacCarty RL, Welch TJ (2000) Incidental extracolonic findings at CT colonography. Radiology 215(2):353–357. https://doi.org/10.1148/radiology.215.2.r00ap33353
Zhang XM, Mitchell DG, Dohke M, Holland GA, Parker L (2002) Pancreatic cysts: depiction on single-shot fast spin-echo MR images. Radiology 223(2):547–553. https://doi.org/10.1148/radiol.2232010815
Tanaka M, Fernandez-del Castillo C, Adsay V, Chari S, Falconi M, Jang JY, Kimura W, Levy P, Pitman MB, Schmidt CM, Shimizu M, Wolfgang CL, Yamaguchi K, Yamao K (2012) International consensus guidelines 2012 for the management of IPMN and MCN of the pancreas. Pancreatology 12(3):183–197. https://doi.org/10.1016/j.pan.2012.04.004
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The Local ethical committee was informed and approved this retrospective study.
Informed consent
An informed consent was signed by all the patients regarding the possible use of their data for retrospective studies.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lorusso, F., Principi, M., Pedote, P. et al. Prevalence and clinical significance of incidental extra-intestinal findings in MR enterography: experience of a single University Centre. Radiol med 126, 181–188 (2021). https://doi.org/10.1007/s11547-020-01235-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-020-01235-6