Abstract
Purpose
The study was conducted to search for confident radiological signs in symptomatic cases of accessory bones. A normal accessory bone appearance on X-ray does not exclude that the accessory bone is the source of the discomfort; because of this, MRI examination can later be applied as part of the diagnosis.
Methods
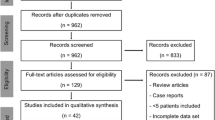
We retrospectively analysed cases of 64 patients with recognized 70 symptomatic accessory bones of the foot. The average age was 29.2 (range 8–42) years. We included only patients with X-ray and MRI examinations. We investigated the following radiological features of the bone (structural and signal) in relation to soft tissue.
Results
The most constant symptoms identified in our study were bone marrow oedema (93%) and soft tissue oedema (77%). Changes in structures in which accessory bones were located or in adjacent structures to accessory bone were identified: tendon changes 51%, fluid adjacent to bone 51% and tenosynovitis 46%. MRI revealed changes in bone structure that are not seen on X-ray, including changes in contour (28%), sclerosis (3%) or osteonecrosis (3%).
Conclusions
MRI plays an important role in determining whether accessory bones cause symptoms because it shows specific and accurate changes in accessory bone and/or in adjacent soft tissue.






Similar content being viewed by others
References
Cheong IY, Kang HJ, Ko H, Sung J, Song YM, Hwang JH (2017) Genetic influence on accessory navicular bone in the foot: a Korean twin and family study. Twin Res Hum Genet 20(03):236–241. https://doi.org/10.1017/thg.2017.21
Keles-Celik N, Kose O, Sekerci R, Aytac G, Turan A, Güler F (2019) Accessory ossicles of the foot and ankle: disorders and a review of the literature. Cureus 9(11):e1881. https://doi.org/10.7759/cureus.1881
Kiter Esat, Erdag Namik, Karatosun Vasfi, Gunal Izge (1999) Tibialis posterior tendon abnormalities in feet with accessory navicular bone and flatfoot. Acta Orthop Scand 70(6):618–621. https://doi.org/10.3109/17453679908997852
Kotov G, Iliev A, Landzhov B, Dimitrova IN, Slavchev S, Georgiev GP, Georgiev GP (2016) A clinical, radiographic and histological study of the accessory navicular bone. Praemedicus 33(1):6
Vaz A, Trippia CR (2018) Small but troublesome: accessory ossicles with clinical significance. Radiol Bras 51(4):248–256. https://doi.org/10.1590/0100-3984.2017.0147
Vora BMK, Wong BSS (2018) Common accessory ossicles of the foot: imaging features, pitfalls and associated pathology. Singap Med J 59(4):183–189. https://doi.org/10.11622/smedj.2018046
Zwiers R, Baltes TPA, Opdam KTM, Wiegerinck JI, van Dijk CN (2018) Prevalence of os trigonum on CT imaging. Foot Ankle Int 39(3):338–342. https://doi.org/10.1177/1071100717740937
Arslan Serdar, Bakdik Suleyman, Oncu Fatih, Karahan Ali, Durmaz Mehmet, Ozen Kemal, Cicekbasi Aynur (2018) Incidence and anatomical variability of accessory and sesamoid bones of the foot. Ann Med Res 25(4):420. https://doi.org/10.5455/annalsmedres.2018.05.078
Chao W (2004) Os trigonum. Foot Ankle Clin 9(4):787–796. https://doi.org/10.1016/j.fcl.2004.06.006
Kıter E, Erduran M, Günal I (2000) Inheritance of the accessory navicular bone. Arch Orthop Trauma Surg 120(10):582–583. https://doi.org/10.1007/s004020000143
Kalbouneh Heba, Alajoulin Omar, Alsalem Mohammad, Humoud Noor, Shawaqfeh Jamil, Alkhoujah Mohammad, Abu-Hassan Hana, Mahafza Waleed, Badran Darwish (2017) Incidence and anatomical variations of accessory navicular bone in patients with foot pain: a retrospective radiographic analysis: accessory navicular bone. Clin Anat 30(4):436–444. https://doi.org/10.1002/ca.22876
Bearcroft PWP, Guy S, Bradley M, Robinson F (2006) MRI of the ankle: effect on diagnostic confidence and patient management. AJR Am J Roentgenol 187(5):1327–1331. https://doi.org/10.2214/AJR.05.1071
Kose O (2012) The accessory ossicles of the foot and ankle; a diagnostic pitfall in emergency department in context of foot and ankle trauma. J Acad Emerg Med 11(2):106–114. https://doi.org/10.5152/jaem.2012.002
Mellado JM, Ramos A, Salvadó E, Camins A, Danús M, Saurí A (2003) Accessory ossicles and sesamoid bones of the ankle and foot: imaging findings, clinical significance and differential diagnosis. Eur Radiol 13(Suppl 4):L164–L177. https://doi.org/10.1007/s00330-003-2011-8
Maffulli N, Lepore L, Francobandiera C (1990) Traumatic lesions of some accessory bones of the foot in sports activity. J Am Podiatr Med Assoc 80(2):86–90. https://doi.org/10.7547/87507315-80-2-86
Ugolini PA, Raikin SM (2004) The accessory navicular. Foot Ankle Clin 9(1):165–180. https://doi.org/10.1016/S1083-7515(03)00176-1
Bae S, Kang Y, Song YS, Lee WW (2019) Maximum standardized uptake value of foot SPECT/CT using tc-99 m hdp in patients with accessory navicular bone as a predictor of surgical treatment. Medicine 98(2):e14022. https://doi.org/10.1097/MD.0000000000014022
Bernaerts A, Vanhoenacker FM, Van de Perre S, De Schepper AM, Parizel PM (2004) Accessory navicular bone: not such a normal variant. JBR BTR 4:250–251
Issever AS, Minden K, Eshed I, Hermann KGA (2007) Accessory navicular bone: when ankle pain does not originate from the ankle. Clin Rheumatol 26(12):2143–2144. https://doi.org/10.1007/s10067-007-0624-z
Mansoor Sahibzada N, Rathore Farooq A (2017) Symptomatic accessory navicular bone: a case series. Egypt Rheumatol 39(4):263–266. https://doi.org/10.1016/j.ejr.2017.02.003
Jegal H, Park YU, Kim JS, Choo HS, Seo YU, Lee KT (2016) Accessory navicular syndrome in athlete vs general population. Foot Ankle Int 37(8):862–867. https://doi.org/10.1177/1071100716644791
Kumahashi Nobuyuki, Kuwata Suguru, Imade Shinji, Uchio Yuji (2017) Osteomyelitis of the accessory and body of the navicular bone: a case report. J Pediatr Orthop B 26(6):515–518. https://doi.org/10.1097/BPB.0000000000000429
Chuang Yi-Wen, Tsai Wen-San, Chen Kai-Hua, Hsu Hung-Chih (2012) Clinical use of high-resolution ultrasonography for the diagnosis of type II accessory navicular bone. Am J Phys Med Rehabilit 91(2):177–181. https://doi.org/10.1097/PHM.0b013e318232846d
Mosel LD, Kat E, Voyvodic F (2004) Imaging of the symptomatic type II accessory navicular bone. Australas Radiol 48(2):267–271. https://doi.org/10.1111/j.1440-1673.2004.01286.x
Fredrick Lori A, Beall Douglas P, Ly Justin Q, Fish Jon R (2005) The symptomatic accessory navicular bone: a report and discussion of the clinical presentation. Curr Probl Diagn Radiol 34(2):47–50. https://doi.org/10.1067/j.cpradiol.2004.12.004
Leonard Zachary C, Fortin Paul T (2010) Adolescent accessory navicular. Foot Ankle Clin 15(2):337–347. https://doi.org/10.1016/j.fcl.2010.02.004
Knapik DM, Archibald HD, Xie KK, Liu RW (2019) A retrospective study on factors predictive of operative intervention in symptomatic accessory navicular. J Child Orthop 13(1):107–113. https://doi.org/10.1302/1863-2548.13.180168
Seehausen DA, Harris LR, Kay RM, Pace JL (2016) Accessory navicular is associated with wider and more prominent navicular bone in pediatric patients by radiographic measurement. J Pediatr Orthop 36(5):521–525. https://doi.org/10.1097/BPO.0000000000000489
Sella EJ, Lawson JP (1987) Biomechanics of the accessory navicular synchondrosis. Foot Ankle 8(3):156–163. https://doi.org/10.1177/107110078700800310
Sella EJ, Lawson JP, Ogden JA (1986) The accessory navicular synchondrosis. Clin Orthop Relat Res. https://doi.org/10.1097/00003086-198608000-00042
Nault Marie-Lyne, Kocher Mininder S, Micheli Lyle J (2014) Os trigonum syndrome. J Am Acad Orthop Surg 22(9):545–553. https://doi.org/10.5435/JAAOS-22-09-545
Brodsky AE, Khalil MA (1986) Talar compression syndrome. Am J Sports Med 14(6):472–476. https://doi.org/10.1177/036354658601400607
Weiss WM, Sanders EJ, Crates JM, Barber FA (2015) Arthroscopic excision of a symptomatic os trigonum. Arthrosc J Arthrosc Relat Surg 31(11):2082–2088. https://doi.org/10.1016/j.arthro.2015.04.086
Sobel M, Pavlov H, Geppert MJ, Thompson FM, DiCarlo EF, Davis WH (1994) Painful os peroneum syndrome: a spectrum of conditions responsible for plantar lateral foot pain. Foot Ankle Int 15(3):112–124. https://doi.org/10.1177/107110079401500306
Favinger Jennifer L, Richardson Michael L, Chew Felix S (2018) Progressive retraction of a fractured os peroneum suggesting repetitive injury to the peroneus longus tendon. Radiol Case Rep 13(1):216–219. https://doi.org/10.1016/j.radcr.2017.11.006
Smith Jeremy T, Johnson Anne H, Heckman James D (2011) Nonoperative treatment of an os peroneum fracture in a high-level athlete: a case report. Clin Orthop Relat Res 469(5):1498–1501. https://doi.org/10.1007/s11999-011-1812-3
Oh SJ, Kim YH, Kim SK, Kim MW (2012) Painful os peroneum syndrome presenting as lateral plantar foot pain. Ann Rehabilit Med 36(1):163–166. https://doi.org/10.5535/arm.2012.36.1.163
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by PS, MP, HK and JS. The first draft of the manuscript was written by PS, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
None of the authors declare a conflict of interest.
Ethical approval
The Institutional Ethics Committee was informed about the ongoing study, and the Committee stated no need for its approval (Number AKBE257/2019).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Szaro, P., Polaczek, M., Świątkowski, J. et al. How to increase the accuracy of the diagnosis of the accessory bone of the foot?. Radiol med 125, 188–196 (2020). https://doi.org/10.1007/s11547-019-01104-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-019-01104-x