Abstract
Purpose
This study compared spontaneous bone healing and regeneration obtained with deproteinised bovine graft in residual cavities after mandibular cyst enucleation using computed tomography (CT) Dentascan.
Materials and methods
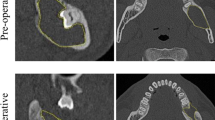
Eighty patients with a radiological diagnosis of mandibular cyst underwent surgical enucleation. Patients were divided into a control group (spontaneous healing, 40 patients) and a test group (deproteinised bovine graft, 40 patients). All patients underwent follow-up CT Dentascan 12 months after the procedure. For each residual cavity, apical-coronal and mesial-distal distance, average pixel intensity and volume were calculated and results compared between two groups using the t test.
Results
The control group showed mean volume, apical-coronal and mesial-distal distance of 703.2±185.3 mm3, 28.6±9.4 mm and 25±2.84 mm, respectively. In the test group, values were 738.2±189.2 mm3, 27.5±3.6 mm and 25.3±2.97 mm, respectively. There was no statistically significant difference between groups.
Average pixel intensity was 1,102.8±124.3 in the test group and 624.9±133.3 in the control group, with a significant difference between groups (p<0.0001).
Conclusions
The significantly higher average pixel intensity observed in the test group demonstrates the cavalue of treatment with biomaterials to obtain earlier bone regeneration.
Riassunto
Obiettivo
Scopo del presente lavoro è valutare mediante tomografia computerizzata (TC)-Dentascan la rigenerazione ossea spontanea e quella ottenuta con innesto di osso bovino deproteinizzato, in cavità residuate ad enucleazione di cisti mandibolari.
Materiali e metodi
Ottanta pazienti con diagnosi radiologica di cisti mandibolare sono stati sottoposti ad intervento di enucleazione. I pazienti sono stati suddivisi in: gruppo controllo, 40 pazienti soggetti a guarigione spontanea; gruppo test, 40 pazienti trattati con osso bovino deproteinizzato. Tutti i soggetti sono stati rivalutati dopo 12 mesi con TC-Dentascan. Per ciascuna cavità residua sono state calcolate distanza apico-coronale e mesio-distale, intensità media dei pixel e volume; tali misure sono state confrontate tra i due gruppi mediante test t di Student.
Risultati
Valore medio di volume, distanza mesiodistale ed apico-coronale sono nel gruppo controllo rispettivamente 703,2±185,3 mm3, 28,6±9,4 mm e 25±2,84 mm; nel gruppo test, invece, sono 738,2±189,2 mm3, 27,5±3,6 mm e 25,3±2,97 mm. Riguardo a tali misure, non si osserva differenza significativa tra i gruppi. Analizzando l’intensità, il valore medio nel gruppo test è 1102,8±124,3 e nel gruppo controllo è 624,9±133,3, con differenza significativa tra i gruppi (p<0,0001).
Conclusioni
I valori di intensità significativamente più elevati nel gruppo test, documentano la validità del trattamento con biomateriali per una rigenerazione ossea più precoce.
Similar content being viewed by others
References/Bibliografia
Belli E, Longo B, Balestra FM (2005) Autogenous platelet-rich plasma in combination with bovine-derived hydroxyapatite xenograft for treatment of a cystic lesion of the jaw. J Craniofac Surg 16:978–980
Baldini N, De Sanctis M, Ferrari M (2011) Deproteinized bovine bone in periodontal and implant surgery. Dent Mater 27:61–70
Chiapasco M, Rossi A, Motta JJ, Crescentini M (2000) Spontaneous bone regeneration after enucleation of large mandibular cysts: a radiographic computed analysis of 27 consecutive cases. J Oral Maxillofac Surg 58:942–948
Camelo M, Nevins ML, Schenk RK et al (1998) Clinical, radiographics and histologic evaluation of human periodontal defects treated with Bio-Oss and Bio-Gide. Int J Periodontics Restorative Dent 18:321–331
Varinauskas V, Gervickas A, Kavoliüniene O (2006) Analysis of odontogenic cysts of the jaws. Medicina (Kaunas) 42:201–207
S’mieszek-Wilczewska J, Koszowski R, Pajak J (2010) Comparison of postoperation bone defects healing of alveolar processes of maxilla and mandible with the use of Bio-Gen and Bio-Oss. J Clin Exp Dent 2:62–68
Hassan KS, Marei HF, Alagl AS (2011) Composite bone graft for treatment of osseous defects after surgical removal of impacted third and second molars: case report and review of the literature. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 112:e8–e15
Camelo M, Nevins ML, Lynch SE et al (2001) Periodontal regeneration with an autogenous bone-Bio-Oss composite graft and a Bio-Gide membrane. Int J Periodontics Restorative Dent 21:109–119
Saavedra-Abril JA, Balhen-Martin C, Zaragoza-Velasco K et al (2010) Dental Multisection CT for the placement of oral implants: technique and applications. Radiographics 30:1975–1991
Kubota Y, Ninomiya T, Oka S et al (2000) Interleukin-1alphadependent regulation of matrix metalloproteinase-9 (MMP-9) secretion and activation in the epithelial cells of odontogenic jaw cysts. J Dent Res 79:1423–1430
Au-Yeung KM, Ahuja AT, Ching AS, Metreweli C (2001) Dentascan in oral imaging. Clin Radiol 56:700–713
Cawood JI, Howell RA (1998) A classification of the eduntulous jaws. Int J Oral Maxillofac Surg 17:232–236
Norton MR, Gamble C (2001) Bone classification: an objective scale of bone density using the computerized tomography scan. Clin Oral Implants Res 12:79–84
Scribano E, Ascenti G, Mazziotti S et al (2003) Computed tomography in dental implantology: medico-legal implications. Radiol Med 105:92–99
Carrafiello G, Dizonno M, Colli V et al (2010) Comparative study of jaws with multislice computed tomography and cone-beam computed tomography. Radiol Med 115:600–611
Taguchi A, Tanimoto K, Akagawa Y et al (1997) Trabecular bone pattern of the mandible. Comparison of panoramic radiography with computed tomography. Dentomaxillofac Radiol 26:85–89
Gahleitner A, Watzek G, Imhof H (2002) Dental CT: imaging technique, anatomy, and pathologic conditions of the jaws. Eur Radiol 13:366–376
Fanucci E, Leporace M, Di Costanzo G et al (2006) Multidetector CT and Dentascan software: dosimetric evaluation and technique improvement. Radiol Med 111:130–138
Carinci F, Piattelli A, Degidi M et al (2006) Genetic effects of anorganic bovine bone (Bio-Oss) on osteoblastlike MG63 cells. Arch Oral Biol 51:154–163
Sollazzo V, Palmieri A, Scapoli L et al (2010) Bio-Oss acts on stem cells derived from peripheral blood. OMJ 25:26–31
Sartori S, Silvestri M, Forni F et al (2003) Ten-year follow-up in a maxillary sinus augmentation using anorganic bovine bone (Bio-Oss). A case report with histomorphometric evaluation. Clin Oral Implants Res 14:369–372
Schlegel AK, Donath K (1998) BIOOSS—a resorbable bone substitute? J Long Term Eff Med Implants 8:201–209
Piattelli M, Favero GA, Scarano A et al (1999) Bone reactions to anorganic bovine bone (Bio-Oss) used in sinus augmentation procedures: a histologic long-term report of 20 cases in humans. Int J Oral Maxillofac Implants 14:835–840
Tietmann C, Bröseler F (2006) Long-term clinical outcome after reconstruction of periodontal defects using a bovine-derived xenograft: a retrospective cohort study. Perio — Periodontal Practices Today 3:75–86
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pappalardo, S., Coronella, M., Lanza, M.L. et al. Multidetector CT Dentascan evaluation of bone regeneration obtained with deproteinised bovine graft in residual cavity after mandibular cyst enucleation. Radiol med 118, 523–533 (2013). https://doi.org/10.1007/s11547-012-0911-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-012-0911-x