Abstract
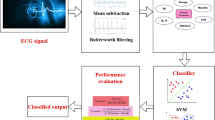
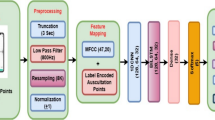
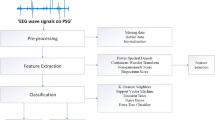
Globally, respiratory disorders are a great health burden, affecting as well as destroying human lives; pneumonia is one among them. Pneumonia stages can progress from mild stage to even towards deadly if it is misdiagnosed. Misdiagnosis happens as it exhibits the symptoms identical to other respiratory diseases. Respiratory sound (RS)-based detection of pneumonia could be the most perfect, convenient, as well as the economical solution to this serious problem. This paper presents a novel method to detect pneumonia based on RS. This study is carried out over 310 pneumonia RS and 318 healthy RS, recorded from a hospital. The noises from each RS are eliminated using the Butterworth band pass filter and sparsity-assisted signal smoothing algorithm. Approximate entropy, Shannon entropy, fractal dimension, and largest Lyapunov exponent are the nonlinear features, which are extracted from each denoised RS. The extracted features are inputted to support vector machine classifiers to distinguish pneumonia RS and healthy RS. This method discriminates against pneumonia and healthy RS with 99.8% classification accuracy, 99.8% sensitivity, 99.6% specificity, 99.6% positive predictive value, 99.6% F1-score, and area under curve value of 1.0. Future endeavours will be to examine the efficacy of the proposed algorithm to diagnose pneumonia from the real-time RS acquired from a pneumonia patient in a hospital. This proposed work could be a great support to clinicians in diagnosing pneumonia based on RS.
Graphical Abstract





Similar content being viewed by others
References
McAllister DA, Liu L, Shi T, Chu Y, Reed C, Burrows J, Adeloye D, Rudan I, Black RE, Campbell H, Nair H (2019) Global, regional, and national estimates of pneumonia morbidity and mortality in children younger than 5 years between 2000 and 2015: a systematic analysis. Lancet Glob Health 7(1):e47-57
Rudan I, Tomaskovic L, Boschi-Pinto C, Campbell H (2004) Global estimate of the incidence of clinical pneumonia among children under five years of age. Bull World Health Organ 82(12):895–903
Torres A, Peetermans WE, Viegi G, Blasi F (2013) Risk factors for community-acquired pneumonia in adults in Europe: a literature review. Thorax 68(11):1057–1065
Fonseca Lima EJ, Mello MJ, Albuquerque MD, Lopes MI, Serra GH, Lima DE, Correia JB (2016) Risk factors for community-acquired pneumonia in children under five years of age in the post-pneumococcal conjugate vaccine era in Brazil: a case control study. BMC Pediatr 16(1):1–9
Laushkina Z (2015) The analysis of factors associated with misdiagnosis pneumonia in TB hospital. Eur Respir J 46:PA1524. https://doi.org/10.1183/13993003.congress-2015.PA1524
Feng AN, Cai HR, Zhou Q, Zhang YF, Meng FQ (2014) Diagnostic problems related to acute fibrinous and organizing pneumonia: misdiagnosis in 2 cases of lung consolidation and occupying lesions. Int J Clin Exp Pathol 7(7):4493
Kwon MR, Lee HY, Cho JH, Um SW (2015) Lung infarction due to pulmonary vein stenosis after ablation therapy for atrial fibrillation misdiagnosed as organizing pneumonia: sequential changes on CT in two cases. Korean J Radiol 16(4):942–946
Oh SY, Kim MY, Kim JE, Kim SS, Park TS, Kim DS, Choi CM (2015) Evolving early lung cancers detected during follow-up of idiopathic interstitial pneumonia: serial CT features. Am J Roentgenol 204(6):1190–1196
Bakare OO, Fadaka AO, Klein A, Keyster M, Pretorius A (2020) Diagnostic approaches of pneumonia for commercial-scale biomedical applications: an overview. All Life 13(1):532–547
Haider NS, Behera AK (2022) Respiratory sound denoising using sparsity-assisted signal smoothing algorithm. Biocybern Biomed Eng 42(2):481–93
Andres E, Gass R, Charloux A, Brandt C, Hentzler A (2018) Respiratory sound analysis in the era of evidence-based medicine and the world of medicine 2.0. J Med life 11(2):89
Kwon AM, Kang K (2022) A temporal dependency feature in lower dimension for lung sound signal classification. Sci Rep 12(1):1–11
Ellington LE, Gilman RH, Tielsch JM, Steinhoff M, Figueroa D, Rodriguez S, Caffo B, Tracey B, Elhilali M, West J, Checkley W (2012) Computerised lung sound analysis to improve the specificity of paediatric pneumonia diagnosis in resource-poor settings: protocol and methods for an observational study. BMJ open 2(1). https://doi.org/10.1136/bmjopen-2011-000506
Sánchez Morillo D, Leon Jimenez A, Moreno SA (2013) Computer-aided diagnosis of pneumonia in patients with chronic obstructive pulmonary disease. J Am Med Inform Assoc 20(e1):e111–e117
Pinho C, Oliveira A, Jácome C, Rodrigues J, Marques A (2015) Automatic crackle detection algorithm based on fractal dimension and box filtering. Procedia Comput Sci 64:705–712
Jindal V, Agarwal V, Kalaivani S (2018) Respiratory sound analysis for detection of pulmonary diseases. IEEE Applied Signal Processing Conference (ASPCON) 293–296. https://doi.org/10.1109/aspcon.2018.8748284
Naqvi SZ, Choudhry MA (2020) An automated system for classification of chronic obstructive pulmonary disease and pneumonia patients using lung sound analysis. Sensors 20(22):6512
Fraiwan M, Fraiwan L, Alkhodari M, Hassanin O (2021) Recognition of pulmonary diseases from lung sounds using convolutional neural networks and long short-term memory. J Ambient Intell Humaniz Comput 1–3. https://doi.org/10.1007/s12652-021-03184-y
Vidhya B, Nikhil Madhav M, Suresh Kumar M, Kalanandini S (2022) AI based diagnosis of pneumonia. Wireless Pers Commun 126(4):3677–3692
Alqudah AM, Qazan S, Obeidat YM (2022) Deep learning models for detecting respiratory pathologies from raw lung auscultation sounds. Soft Comput 26(24):13405–13429
Delgado-Bonal A, Marshak A (2019) Approximate entropy and sample entropy: a comprehensive tutorial. Entropy 21(6):541
Don S (2020) Random subset feature selection and classification of lung sound. Procedia Comput Sci 167:313–322
do Nascimento Neto J, de Vasconcellos RM, Ferreira AA (2022) Estimating largest Lyapunov exponents in aeroelastic signals. International Journal of Dynamics and Control 1–9. https://doi.org/10.1007/s40435-021-00833-0
Ahsan MM, Luna SA, Siddique Z (2022) Machine-learning-based disease diagnosis: a comprehensive review. InHealthcare 10(3):541 (MDPI)
Chang V, Ganatra MA, Hall K, Golightly L, Xu QA (2022) An assessment of machine learning models and algorithms for early prediction and diagnosis of diabetes using health indicators. Healthc Analytics 2:100118
Hasija S, Akash P, Hemanth MB, Kumar A, Sharma S (2022) A novel approach for detection of COVID-19 and Pneumonia using only binary classification from chest CT-scans. Neuroscience Informatics 2(4). https://doi.org/10.1016/j.neuri.2022.100069
Haider NS, Behera AK (2022) Computerized lung sound based classification of asthma and chronic obstructive pulmonary disease (COPD). Biocybern Biomed Eng 42(1):42–59
Author information
Authors and Affiliations
Contributions
The author Dr. Nishi Shahnaj Haider has contributed in preparation of the relevant software coding and writing of the manuscript. Author Dr. Ajoy K Behera has contributed to data collection from the hospital.
Corresponding author
Ethics declarations
Ethics approval
The study was approved by the institutional ethical clearance and the study was carried out strictly as per the guidelines issued by the ethical committee.
Consent to participate
Written informed consent was taken from the individuals before enrolling them for the data collection.
Consent for publication
The participant has consented to the submission of the case report to the journal.
Competing interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Haider, N.S., Behera, A.K. Computerized respiratory sound based diagnosis of pneumonia. Med Biol Eng Comput 62, 95–106 (2024). https://doi.org/10.1007/s11517-023-02935-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11517-023-02935-7