Abstract
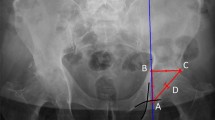
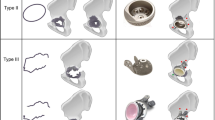
Proper alignment of acetabular implantation is necessary for good patient outcomes and preventing complications or additional surgeries in total hip arthroplasty (THA). Rotation of the pelvis in lateral decubitus (LD) is typically not accounted for as surgeons use the surgery table as a reference plane to align implants. This study compared four techniques to measure 3D pelvic rotations in LD position using computer models. CT scans of 19 subjects in LD position were used to create 3D pelvis models. Pelvic rotations were measured by three users using four techniques: landmark (LM), defined plane (DP), anterior pelvic plane (APP), and plane of best symmetry (POBS) methods. Measurements were analysed for intra-user reliability and relationships between methods were assessed using intraclass correlation coefficient, standard error of measurement, and coefficient of determination. The POBS method exhibited the highest inter-observer reliability and is recommended as a new measurement technique to measure pelvic rotations before THA surgery. The LM method exhibited low reliability but may be suitable for expert users familiar with pelvic landmarks. The APP method should only be used when the patients’ APP planes are known in neutral standing and side-lying postures. The DP method is not recommended due to substantial individual variability.

Graphical abstract




Similar content being viewed by others
References
Tannast M, Langlotz U, Siebenrock KA, Wiese M, Bernsmann K, Langlotz F (2005) Anatomic referencing of cup orientation in total hip arthroplasty. Clin Orthop Relat Res 436:144–150. https://doi.org/10.1097/01.blo.0000157657.22894.29
Kalteis T, Handel M, Herbst B, Grifka J, Renkawitz T (2009) In vitro investigation of the influence of pelvic tilt on acetabular cup alignment. J Arthroplast 24:152–157. https://doi.org/10.1016/j.arth.2007.12.014
Eddine TA, Migaud H, Chantelot C, Cotten A, Fontaine C, Duquennoy A (2001) Variations of pelvic anteversion in the lying and standing positions of 24 control subjects and implications for CT measurement of position of prosthetic cup. Surg Radiol 23(2):105–110. https://doi.org/10.1007/s00276-001-0105-z
Shon WY, Gupta S, Biswal S, Hur CY, Jajodia N, Hong SJ, Myung JS (2008) Validation of a simple radiographic method to determine variations in pelvic and acetabular cup sagittal plane alignment after total hip arthroplasty. Skelet Radiol 37(12):1119–1127. https://doi.org/10.1007/s00256-008-0550-4
Grammatopoulos G, Pandit HG, da Assunção R, Taylor A, McLardy-Smith P, De Smet KA, Murray DW, Gill HS (2014) Pelvic position and movement during hip replacement. Bone Joint J 96-B(7):876–883. https://doi.org/10.1302/0301-620X.96B7.32107
Kanazawa M, Nakashima Y, Ohishi M, Hamai S, Motomura G, Yamamoto T, Fukushi J, Ushijima T, Hara D, Iwamoto Y (2016) Pelvic tilt and movement during total hip arthroplasty in the lateral decubitus position. Mod Rheumatol 26(3):435–440. https://doi.org/10.3109/14397595.2015.1092914
Shon WY, Sharma V, Keon OJ, Moon JG, Suh DH (2014) Can pelvic tilting be ignored in total hip arthroplasty? Int J Surg Case 5(9):633–636. https://doi.org/10.1016/j.ijscr.2014.07.015
McCollum DE, Gray W (1990) Dislocation after total hip arthroplasty: causes and prevention. Clin Orthop Relat Res 261:159–170
Turner RS (1994) Postoperative total hip prosthetic femoral head dislocations. Incidence, etiologic factors, and management. Clin Orthop Relat Res 301:196–204
DeChenne CL, Jayaram U, Lovell T, Dong N, Cusick M (2005) A novel acetabular alignment guide for THR using selective anatomic landmarks on the pelvis. J Biomech 38(9):1902–1908. https://doi.org/10.1016/j.jbiomech.2004.08.011
Haenle M, Heitner A, Mittelmeier W, Barbano R, Scholz R, Steinhauser E, Bader R (2007) Assessment of cup position from plain radiographs: impact of pelvic tilting. Surg Radiol Anat 29(1):29–35. https://doi.org/10.1007/s00276-006-0167-z
Nishihara S, Sugano N, Nakahodo K, Sasama T, Nishii T, Sato Y, Tamura S, Yonenobu K, Yoshikawa H, Ochi T (2000) Measurement of pelvic tilting angle during total hip arthroplasty using a computer navigation system. Lect Notes Comput Sci 1935:1176–1179. https://doi.org/10.1007/978-3-540-40899-4_124
Tezuka T, Inaba Y, Kobayashi N, Ike H, Kubota S, Kawamura M, Saito T (2015) Influence of pelvic tilt on polyethylene wear after total hip arthroplasty. Biomed Res Int 2015:1–6. https://doi.org/10.1155/2015/327217
Miki H, Kyo T, Sugano N (2012) Anatomical hip range of motion after implantation during total hip arthroplasty with a large change in pelvic inclination. J Arthroplast 27(9):1641–1650. https://doi.org/10.1016/j.arth.2012.03.002
Beckmann J, Lüring C, Tingart M, Anders S, Grifka J, Köck FX (2009) Cup positioning in THA: current status and pitfalls. A systemic evaluation of literature. Arch Orthop Trauma Surg 129(7):863–872. https://doi.org/10.1007/s00402-008-0686-7
Maratt JD, Esposito CI, McLawhorn AS, Jerabek SA, Padgett DE, Mayman DJ (2014) Pelvic tilt in patients undergoing total hip arthroplasty: when does it matter? J Arthroplast 30(3):387–391. https://doi.org/10.1016/j.arth.2014.10.014
Wan Z, Malik A, Jaramaz B, Chao L, Dorr LD (2008) Imaging and navigation of acetabular component position in THA. Clin Orthop Relat Res 467:32–42. https://doi.org/10.1007/s11999-008-0597-5
Mellano CR, Spitzer AI (2015) How does pelvic rotation of tilt affect radiographic measurement of acetabular component inclination angle during THA? J Orthop 12(4):222–227. https://doi.org/10.1016/j.jor.2015.05.009
Craiovan B, Renkawitz T, Weber M, Grifka J, Nolte L, Zheng G (2014) Is the acetabular cup orientation after total hip arthroplasty on a two dimension or three dimension model accurate? Int Orthop 38(10):2009–2015. https://doi.org/10.1007/s00264-014-2336-8
Rousseau MA, Lazennec JY, Boyer P, Mora N, Gorin M, Catonné Y (2009) Optimization of total hip arthroplasty implantation: is the anterior pelvic plane concept valid? J Arthroplast 24(1):22–26. https://doi.org/10.1016/j.arth.2007.12.015
Blondel B, Parratte S, Tropiano P, Pauly V, Aubaniac JM, Argenson JN (2009) Pelvic tilt measurement before and after total hip arthroplasty. Orthop Traumatol Surg 95(8):568–572. https://doi.org/10.1016/j.otsr.2009.08.004
Siebenrock KA, Kalbermatten DF, Ganz R (2002) Effect of pelvic tilt on acetabular retroversion: a study of pelves from cadavers. Clin Orthop Relat Res 407:241–248. https://doi.org/10.1097/00003086-200302000-00033
Tannast M, Murphy SB, Langlotz F, Anderson SE, Siebenrock KA (2006) Estimation of pelvic tilt on anteroposterior X-rays--a comparison of six parameters. Skelet Radiol 35(3):149–155. https://doi.org/10.1007/s00256-005-0050-8
Kalteis T, Handel M, Herold T, Perlick L, Paetzel C, Grifka J (2006) Position of the acetabular cup--accuracy of radiographic calculation compared to CT-based measurement. Eur J Dermatol 58:294–300. https://doi.org/10.1016/j.ejrad.2005.10.003
Hill S, Franco-Sepulveda E, Komeili A, Trovato A, Parent E, Hill D, Lou E, Adeeb S (2014) Assessing asymmetry using reflection and rotoinversion in biomedical engineering applications. Proc Inst Mech Eng H 228(5):523–529. https://doi.org/10.1177/0954411914531115
Baclig MM, Westover LM, Adeeb S (2019) Categorizing three-dimensional symmetry using reflection, rotoinversion, and translation symmetry. Symmetry 11(9):1132. https://doi.org/10.3390/sym11091132
Ho C, Parent EC, Watkins E, Moreau MJ, Hedden D, El-Rich M, Adeeb S (2015) Asymmetry assessment using surface topography in healthy adolescents. Symmetry 7(3):1436–1454. https://doi.org/10.3390/sym7031436
Komeili A, Westover LM, Parent EC, Moreau M, El-Rich M, Adeeb S (2014) Surface topography asymmetry maps categorizing external deformity in scoliosis. Spine J 14(6):973–983. https://doi.org/10.1016/j.spinee.2013.09.032
Digioia AM 3rd, Jaramaz B, Plakseychuk AY, Moody JE Jr, Nikou C, Labarca RS, Levison TJ, Picard F (2002) Comparison of a mechanical acetabular alignment guide with computer placement of the socket. J Arthroplast 17(3):359–364. https://doi.org/10.1054/arth.2002.30411
Wako Y, Nakamura J, Miura M, Kawarai Y, Sugano M, Nawata K (2018) Interobserver and intraobserver reliability of three-dimensional preoperative planning software in total hip arthroplasty. J Arthroplast 33(2):601–697. https://doi.org/10.1016/j.arth.2017.08.031
Journe A, Sadaka J, Belicourt C, Sautet A (2012) New method for measuring acetabular component positioning with EOS imaging: feasibility study on dry bone. Int Orthop 36:2205–2209. https://doi.org/10.1007/s00264-012-1650-2
Manjunath KS, Soruban V, Gopalakrishna KG (2015) Evaluation of radiologic methods of assessing cup anteversion in total hip replacement. Eur J Orthop Surg Traumatol 25:1285–1292. https://doi.org/10.1007/s00590-015-1702-6
Dorr LD, Wan Z, Malik A, Zhu J, Dastane M, Deshmane P (2009) A comparison of surgeon estimation and computed tomography measurement of femoral component anteversion in cementless total hip arthroplasty. J Bone Joint Surg Am 91(11):2598–2604. https://doi.org/10.2106/JBJS.H.01225
Demzik AL, Alvi HM, Delagrammaticas DE, Martell JM, Beal MD, Manning DW (2016) Inter-rater and intra-rater repeatability and reliability of EOS 3-dimensional imaging analysis software. J Arthroplast 31(5):1091–1095. https://doi.org/10.1016/j.arth.2015.11.026
Barbier O, Skalli W, Mainard L (2014) The reliability of the anterior pelvic plane for computer navigated acetabular component placement during total hip arthroplasty: prospective study with the EOS imaging system. Orthop Traumatol 100(6):S287–S291. https://doi.org/10.1016/j.otsr.2014.07.003
Loftus M, Ma Y, Ghelman B (2015) Acetabular version measurement in total hip arthroplasty: the impact of inclination and the value of multi-planar CT reformation. HSS J 11:65–70. https://doi.org/10.1007/s11420-014-9416-6
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The authors declare that they have no conflict of interest.
All procedures performed in studies involving human participants were in accordance with the ethical standards of the University of Alberta Health Research Ethics Board Health Panel (Pro00053235 and Pro00089030) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
This article does not contain any studies with animals performed by any of the authors.
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Meredith Stadnyk and Tao Liu are co-1st authors
Rights and permissions
About this article
Cite this article
Stadnyk, M., Liu, T., Arezodar, F.F. et al. Analysis of four methods of measuring three-dimensional pelvic tilt in the lateral decubitus position. Med Biol Eng Comput 58, 2387–2396 (2020). https://doi.org/10.1007/s11517-020-02235-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11517-020-02235-4