Abstract
Stress urinary incontinence (SUI) or urine leakage from urethra occurs due to an increase in abdominal pressure resulting from stress like a cough or jumping height. SUI is more frequent among post-menopausal women. In the absence of bladder contraction, vesical pressure exceeds urethral pressure leading to urine leakage. The main aim of this study is to utilize fluid-structure interaction techniques to model bladder and urethra computationally under an external pressure like sneezing. Both models have been developed with linear elastic properties for the bladder wall while the patient model has also been simulated utilizing the Mooney-Rivlin solid model. The results show a good agreement between the clinical data and the predicted values of the computational models, specifically the pressure at the center of the bladder. There is 1.3% difference between the predicted vesical pressure and the vesical pressure obtained from urodynamic tests. It can be concluded that the accuracy of the predicted pressure in the center of the bladder is significantly higher for the simulation assuming nonlinear material property (hyperelastic) for the bladder in comparison to the accuracy of the linear elastic model. The model is beneficial for exploring treatment solutions for SUI disorder.

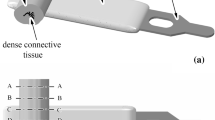
3D processing of bladder deformation during abdominal pressure of a the physiological model and b the pathological model (starting from left to right and up to down, consecutively)








Similar content being viewed by others
References
Wilson L, Brown JS, Shin GP, Luc K-O, Subak LL (2001) Annual direct cost of urinary incontinence. Obstet Gynecol 98:398–406
Hardy LA, Chang CH, Myers EM, Kennelly MJ, Fried NM (2017) Computer simulations of thermal tissue remodeling during transvaginal and transurethral laser treatment of female stress urinary incontinence. Lasers Surg Med 49:198–205
Dias N, Peng Y, Khavari R, Nakib NA, Sweet RM, Timm GW et al (2017) Pelvic floor dynamics during high-impact athletic activities: a computational modeling study. Clin Biomech (Bristol, Avon) 41:20–27
Enhorning G (1961) Simultaneous recording of intravesical and intra-urethral pressure. Acta Chir Scand:1–68
Petros PEP, Ulmsten UI (1990) An integral theory of female urinary incontinence: experimental and clinical considerations. Acta Obstet Gynecol Scand 69:7–31
Ashton-Miller J, DeLANCEY JO (2014) Functional anatomy of the female pelvic floor. In: Bø K, Berghmans B, Mørkved S, van Kampen M (eds) Evidence based physical therapy for the pelvic floor—bridging science and clinical practice, pp 19–33
Bhattarai A, Staat M (2018) Modelling of soft connective tissues to investigate female pelvic floor dysfunctions. Comput Math Methods Med 2018
Peng Y, Miller BD, Boone TB, Zhang Y (2018) Modern theories of pelvic floor support. Curr Urol Rep 19:9
Kim K-J (1994) Biomedical analyses of female stress urinary incontinence: University of Michigan
Haridas B, Hong H, Minoguchi R, Owens S, Osborn T (2006) PelvicSim—a computational-experimental system for biomechanical evaluation of female pelvic floor organ disorders and associated minimally invasive interventions. Stud Health Technol Inf 119:182–187
Spirka T, Kenton K, Brubaker L, Damaser MS (2013) Effect of material properties on predicted vesical pressure during a cough in a simplified computational model of the bladder and urethra. Ann Biomed Eng 41:185–194
Vahidi B, Fatouraee N (2007) Mathematical modeling of the ureteral peristaltic flow with fluid structure interaction. Measurements 5:6
Vahidi B, Fatouraee N (2012) A biomechanical simulation of ureteral flow during peristalsis using intraluminal morphometric data. J Theor Biol 298:42–50
Vahidi B, Fatouraee N, Imanparast A, Moghadam AN (2011) A mathematical simulation of the ureter: effects of the model parameters on ureteral pressure/flow relations. J Biomech Eng 133:031004
Damaser MS, Lehman SL (1995) The effect of urinary bladder shape on its mechanics during filling. J Biomech 28:725–732
Zhang Y, Kim S, Erdman AG, Roberts KP, Timm GW (2009) Feasibility of using a computer modeling approach to study SUI induced by landing a jump. Ann Biomed Eng 37:1425–1433
van Leijsen SAL, Kluivers KB, Mol BWJ, Broekhuis SR, Milani FL, Vaart CHVD et al (2009) Protocol for the value of urodynamics prior to stress incontinence surgery (VUSIS) study: a multicenter randomized controlled trial to assess the cost effectiveness of urodynamics in women with symptoms of stress urinary incontinence in whom surgical treatment is considered. BMC Women's Health 9:22
Drake R, Vogl AW, Mitchell AW (2009) Gray’s Anatomy for Students-Rental: With STUDENT CONSULT Online Access: Elsevier Health Sciences.
Netter FH (2006) Atlas of human anatomy, vol 548. Saunders, Elsevier, Philadelphia, p 547
DeLancey JO (1997) The pathophysiology of stress urinary incontinence in women and its implications for surgical treatment. World J Urol 15:268–274
Delancey JO, Ashton-miller JA (2004) Pathophysiology of adult urinary incontinence. Gastroenterology 126:S23–S32
Sampselle CM, DeLancey JO (1998) Anatomy of female continence. Journal of WOCN 25:63–74
Chan L, The S, Titus J, Tse V (2005) P14. 02: The value of bladder wall thickness measurement in the assessment of overactive bladder syndrome. Ultrasound Obstet Gynecol 26:460–460
Backman K (1971) Effective urethral diameter, Hydrodynamics of Micturition. Charles C. Thomas, Springfield, p 250
Hosein RA, Griffiths DJ (1990) Computer simulation of the neural control of bladder and urethra. Neurourol Urodyn 9:601–618
Janda Š, Van Der Helm FC, de Blok SB (2003) Measuring morphological parameters of the pelvic floor for finite element modelling purposes. J Biomech 36:749–757
d'Aulignac D, Martins J, Pires E, Mascarenhas T, Jorge RN (2005) A shell finite element model of the pelvic floor muscles. Comput Methods Biomech Biomed Eng 8:339–347
(2019) R. ANSYS Mechanical, Help System, Explicit Dynamics Analysis Guide, 7.9.5, ANSYS, Inc
Bastiaanssen E, Van Leeuwen J, Vanderschoot J, Redert P (1996) A myocybernetic model of the lower urinary tract. J Theor Biol 178:113–133
Yamada HS (1970) In: Evans FG (ed) Strength of biological materials. Williams and Wilkins, Baltimore
Bakken L, Anderson P (1967) The complete equation of state handbook. Sandia Corporation SCL-TM-67-118
Griffiths D (1969) Urethral elasticity and micturition hydrodynamics in females. Med Biol Eng 7:201–215
Spángberg A, Terió H, Engberg A, Ask P (1989) Quantification of urethral function based on Griffiths’ model of flow through elastic tubes. Neurourol Urodyn 8:29–52
Bastiaanssen E, Vanderschoot J, Van Leeuwen J (1996) State-space analysis of a myocybernetic model of the lower urinary tract. J Theor Biol 180:215–227
Griffiths D (1971) Hydrodynamics of male micturition—I theory of steady flow through elastic-walled tubes. Med Biol Eng 9:581–588
Horak M, Křen J (2003) Mathematical model of the male urinary tract. Math Comput Simul 61:573–581
van Mastrigt R, Griffiths D (1986) An evaluation of contractility parameters determined from isometric contractions and micturition studies. Urol Res 14:45–52
Fielding JR, Griffiths D, Versi E, Mulkern R, Lee M, Jolesz F (1998) MR imaging of pelvic floor continence mechanisms in the supine and sitting positions. AJR Am J Roentgenol 171:1607–1610
Lotz HT, Remeijer P, van Herk M, Lebesque JV, de Bois JA, Zijp LJ, Moonen LM (2004) A model to predict bladder shapes from changes in bladder and rectal filling. Med Phys 31:1415–1423
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 314 kb).
Rights and permissions
About this article
Cite this article
Barzegari, M., Vahidi, B., Safarinejad, M.R. et al. A computational analysis of the effect of supporting organs on predicted vesical pressure in stress urinary incontinence. Med Biol Eng Comput 58, 1079–1089 (2020). https://doi.org/10.1007/s11517-020-02148-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11517-020-02148-2