Abstract
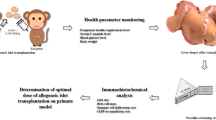
Juvenile (2–23 years old) cynomolgus monkeys are frequently used as recipients in non-human primate islet transplantation studies. The aim of this study was to examine the effects of different doses of streptozotocin (STZ), and find the optimal dose for inducing diabetes in these monkeys. Fifteen juvenile (2–3 years old) cynomolgus monkeys were separated into three groups and administered with different doses of STZ (100, 68 or 60 mg kg−1). Basal and glucose-stimulated blood glucose, insulin, and C-peptide levels, as well as body weights were monitored. Hepatic and renal function tests and pancreatic immunohistochemistry were performed before and after STZ treatment. Monkeys treated with both 100 and 68 mg kg−1 of STZ exhibited continuous hyperglycemia, which coincided with a nearly complete loss of islet β-cells. Two monkeys received 60 mg kg−1 of STZ, but only one became completely diabetic. During the first week following STZ treatment, hepatic and renal function slightly increased in these three groups. However, 24 hours post-STZ, serum total bile acid levels were significantly increased in monkeys treated with 100 mg kg−1 than those treated with 68 mg kg−1 of STZ (P<0.05). These data suggest that 100 mg kg−1 and 68 mg kg−1 of STZ can safely induce diabetes in cynomolgus monkeys aged 2–3 years, but 68 mg kg−1 of STZ, rather than 100 mg kg−1 of STZ, may be more appropriate for inducing diabetes in these monkeys. Furthermore, body surface area, rather than body weight, was a more reliable determinant of dosage, where 700 mg m−2 of STZ should be the lower limit for inducing diabetes in juvenile monkeys.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Shapiro A M, Lakey J R, Ryan E A, et al. Islet transplantation in seven patients with type 1 diabetes mellitus using a glucocorticoid-free immunosuppressive regimen. N Engl J Med, 2000, 343: 230–238
Xiao M, An L, Yang X, et al. Establishing a human pancreatic stem cell line and transplanting induced pancreatic islets to reverse experimental diabetes in rats. Sci China Ser C-Life Sci, 2008, 51: 779–788
Jiang J, Au M, Lu K, et al. Generation of insulin-producing islet-like clusters from human embryonic stem cells. Stem Cells, 2007, 25: 1940–1953
D’Amour K A, Bang A G, Eliazer S, et al. Production of pancreatic hormone-expressing endocrine cells from human embryonic stem cells. Nat Biotechnol, 2006, 24: 1392–1401
Kroon E, Martinson L A, Kadoya K, et al. Pancreatic endoderm derived from human embryonic stem cells generates glucose-responsive insulin-secreting cells in vivo. Nat Biotechnol, 2008, 26: 443–452
Shapiro A M, Ricordi C, Hering B J, et al. International trial of the Edmonton protocol for islet transplantation. N Engl J Med, 2006, 355: 1318–1330
Contreras J L, Jenkins S, Eckhoff D E, et al. Stable alpha- and beta-islet cell function after tolerance induction to pancreatic islet allografts in diabetic primates. Am J Transplant, 2003, 3: 128–138
Kishi Y, Tanaka Y, Shibata H, et al. Variation in the incidence of teratomas after the transplantation of nonhuman primate ES cells into immunodeficient mice. Cell Transplant, 2008, 17: 1095–1102
Kikutani H, Makino S. The murine autoimmune diabetes model: NOD and related strains. Adv Immunol, 1992, 51: 285–322
Greiner D L, Mordes J P, Handler E S, et al. Prothymocyte development in diabetes-prone BB rats: description of a defect that predisposes to immune abnormalities. Transplant Proc, 1987, 19: 976–978
Kawano K, Hirashima T, Mori S, et al. New inbred strain of Long-Evans Tokushima lean rats with IDDM without lymphopenia. Diabetes, 1991, 40: 1375–1381
Cornblath D R, Dellon A L, MacKinnon S E. Spontaneous diabetes mellitus in a rhesus monkey: neurophysiological studies. Muscle Nerve, 1989, 12: 233–235
Sun Y, Ma X, Zhou D, et al. Normalization of diabetes in spontaneously diabetic cynomolgus monkeys by xenografts of microencapsulated porcine islets without immunosuppression. J Clin Invest, 1996, 98: 1417–1422
Wagner J D, Cline J M, Shadoan M K, et al. Naturally occurring and experimental diabetes in cynomolgus monkeys: a comparison of carbohydrate and lipid metabolism and islet pathology. Toxicol Pathol, 2001, 29: 142–148
Lenzen S, Munday R. Thiol-group reactivity, hydrophilicity and stability of alloxan, its reduction products and its Nmethyl derivatives and a comparison with ninhydrin. Biochem Pharmacol, 1991, 42: 1385–1391
Lenzen S, Tiedge M, Jorns A, et al. Alloxan derivatives as a tool for elucidation of the mechanism of the diabetogonic action of alloxan. In: Lessons for Animal Diabetes. Shafrir E, ed. Boston: Birkhauser, 1996. 113–122
Gibbs G E, Wilson R B, Gifford H. Glomerulosclerosis in the long-term alloxan diabetic monkey. Diabetes, 1966, 15: 258–261
Bansal N, Majumdar S, Chakravarti R N. Frequency and size of atherosclerotic plaques in vasectomized diabetic monkeys. Int J Fertil, 1986, 31: 298–304
Theriault B R, Thistlethwaite J R, Levisetti M G, et al. Induction, maintenance, and reversal of streptozotocin-induced insulin-dependent diabetes mellitus in the juvenile cynomolgus monkey (Macaca fascilularis). Transplantation, 1999, 68: 331–337
Koulmanda M, Qipo A, Chebrolu S, et al. The effect of low versus high dose of streptozotocin in cynomolgus monkeys (Macaca fascilularis). Am J Transplant, 2003, 3: 267–272
van der Windt D J, Bottino R, Casu A, et al. Long-term controlled normoglycemia in diabetic non-human primates after transplantation with hCD46 transgenic porcine islets. Am J Transplant, 2009, 9: 2716–2726
Hecht G, Eventov-Friedman S, Rosen C, et al. Embryonic pig pancreatic tissue for the treatment of diabetes in a nonhuman primate model. Proc Natl Acad Sci USA, 2009, 106: 8659–8664
Bottino R, Criscimanna A, Casu A, et al. Recovery of endogenous beta-cell function in nonhuman primates after chemical diabetes induction and islet transplantation. Diabetes, 2009, 58: 442–447
Casu A, Bottino R, Balamurugan A N, et al. Metabolic aspects of pig-to-monkey (Macaca fascicularis) islet transplantation: implications for translation into clinical practice. Diabetologia, 2008, 51: 120–129
Shibata S, Kirchhof N, Matsumoto S, et al. High-dose streptozotocin for diabetes induction in adult rhesus monkeys. Transplant Proc, 2002, 34: 1341–1344
Thomas J M, Contreras J L, Smyth C A, et al. Successful reversal of streptozotocin-induced diabetes with stable allogeneic islet function in a preclinical model of type 1 diabetes. Diabetes, 2001, 50: 1227–1236
Rood P P, Bottino R, Balamurugan A N, et al. Induction of diabetes in cynomolgus monkeys with high-dose streptozotocin: adverse effects and early responses. Pancreas, 2006, 33: 287–292
Wijkstrom M, Kirchhof N, Graham M, et al. Cyclosporine toxicity in immunosuppressed streptozotocin-diabetic nonhuman primates. Toxicology, 2005, 207: 117–127
Ferraris R, Colombatti G, Fiorentini M T, et al. Diagnostic value of serum bile acids and routine liver function tests in hepatobiliary diseases. Sensitivity, specificity and predictive value. Dig Dis Sci, 1983, 28: 129–136
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is published with open access at Springerlink.com
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 2.0 International License (https://creativecommons.org/licenses/by/2.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
About this article
Cite this article
Zou, C., Wang, J., Wang, S. et al. Characterizing the induction of diabetes in juvenile cynomolgus monkeys with different doses of streptozotocin. Sci. China Life Sci. 55, 210–218 (2012). https://doi.org/10.1007/s11427-012-4288-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11427-012-4288-9