Abstract
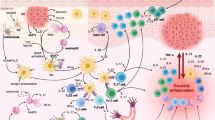
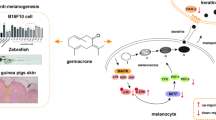
Psoriasis is a chronic inflammatory skin disorder characterized by abnormal keratinocytes proliferation and multiple immune cells infiltration in the dermis and epidermis. Although most psoriasis-related researches have been concentrated on the interleukin-23 (IL-23)/interleukin-17 (IL-17) axis, new data suggest that keratinocytes also play a pivotal role in psoriasis. Previously, we found that punicalagin (PUN), a bioactive ellagitannin extracted from Pericarpium Granati (the pericarpium of Punica granatum L.), exerts a therapeutic effect on psoriasis. However, the underlying mechanism, especially its potential modulatory effect on keratinocytes, remains obscure. Our study aims to reveal the potential regulatory effect and its underlying cellular mechanism of PUN on the hyperproliferation of keratinocytes. We used tumor necrosis factor α (TNF-α), IL-17A and interleukin-6 (IL-6) to induce abnormal proliferation of HaCaT cells (Human Keratinocytes Cells) in vitro. Then, we evaluated the effects of PUN through MTT assay, EdU staining and cell cycle detection. Finally, we explored the underlying cellular mechanisms of PUN via RNA-sequencing, WB in vitro and in vivo. Here, we found that PUN can directly and dose-dependently decrease TNF-α, IL-17A and IL-6-induced abnormal proliferation of HaCaT cells in vitro. Mechanically, PUN suppresses the hyperproliferation of keratinocytes through repressing S-phase kinase-associated protein 2 (SKP2) expression in vitro and in vivo. Moreover, overexpression of SKP2 can partly abolish PUN-mediated inhibition of aberrantly proliferative keratinocytes. These results illustrate that PUN can reduce the severity of psoriasis through directly repressing SKP2-mediated abnormal proliferation of keratinocytes, which gives new insight into the therapeutic mechanism of PUN on psoriasis. Moreover, these findings imply that PUN might be a promising drug candidate for the treatment of psoriasis.
Graphical Abstract




Similar content being viewed by others
Abbreviations
- DEGs:
-
Differentially expressed genes
- DEX:
-
Dexamethasone cream
- GSEA:
-
Gene set enrichment analysis
- IL-6:
-
Interleukin-6
- IL-17A:
-
Interleukin-17A
- IL-23:
-
Interleukin-23
- IMQ:
-
Imiquimod
- KEGG:
-
Kyoto encyclopedia of genes and genomes
- PUN:
-
Punicalagin
- SCF:
-
SKP1/Cullin1/F-box protein complex
- SKP2:
-
S-phase kinase-associated protein 2
- TNF-α:
-
Tumor necrosis factor-α
References
Greb JE, Goldminz AM, Elder JT, Lebwohl MG, Gladman DD, Wu JJ et al (2016) Psoriasis. Nat Rev Dis Primers 2:16082. https://doi.org/10.1038/nrdp.2016.82
Zhu Y, Wu Z, Yan W, Shao F, Ke B, Jiang X et al (2022) Allosteric inhibition of SHP2 uncovers aberrant TLR7 trafficking in aggravating psoriasis. EMBO Mol Med. https://doi.org/10.15252/emmm.202114455
Ding Y, Ouyang Z, Zhang C, Zhu Y, Xu Q, Sun H et al (2020) (2022) Tyrosine phosphatase SHP2 exacerbates psoriasis-like skin inflammation in mice via ERK5-dependent NETosis. MedComm. https://doi.org/10.1002/mco2.120
Lande R, Gregorio J, Facchinetti V, Chatterjee B, Wang YH, Homey B et al (2007) Plasmacytoid dendritic cells sense self-DNA coupled with antimicrobial peptide. Nature 449(7162):564–569. https://doi.org/10.1038/nature06116
Chiricozzi A, Guttman-Yassky E, Suarez-Farinas M, Nograles KE, Tian S, Cardinale I et al (2011) Integrative responses to IL-17 and TNF-alpha in human keratinocytes account for key inflammatory pathogenic circuits in psoriasis. J Invest Dermatol 131(3):677–687. https://doi.org/10.1038/jid.2010.340
Naik S, Larsen SB, Gomez NC, Alaverdyan K, Sendoel A, Yuan S et al (2017) Inflammatory memory sensitizes skin epithelial stem cells to tissue damage. Nature 550(7677):475–480. https://doi.org/10.1038/nature24271
Usha T, Goyal AK, Lubna S, Prashanth H, Mohan TM, Pande V et al (2014) Identification of anti-cancer targets of eco-friendly waste Punica granatum peel by dual reverse virtual screening and binding analysis. Asian Pac J Cancer Prev 15(23):10345–10350. https://doi.org/10.7314/apjcp.2014.15.23.10345
Manickam V, Dhawan UK, Singh D, Gupta M, Subramanian M (2022) Pomegranate peel extract decreases plaque necrosis and advanced atherosclerosis progression in Apoe (-/-) Mice. Front Pharmacol 13:888300. https://doi.org/10.3389/fphar.2022.888300
Chen B, Tuuli MG, Longtine MS, Shin JS, Lawrence R, Inder T et al (2012) Pomegranate juice and punicalagin attenuate oxidative stress and apoptosis in human placenta and in human placental trophoblasts. Am J Physiol Endocrinol Metab 302(9):E1142-1152. https://doi.org/10.1152/ajpendo.00003.2012
Venusova E, Kolesarova A, Horky P, Slama P (2021) Physiological and immune functions of punicalagin. Nutrients 13(7):2150. https://doi.org/10.3390/nu13072150
Luo J, Long Y, Ren G, Zhang Y, Chen J, Huang R et al (2019) Punicalagin reversed the hepatic injury of tetrachloromethane by antioxidation and enhancement of autophagy. J Med Food 22(12):1271–1279. https://doi.org/10.1089/jmf.2019.4411
Houston DMJ, Bugert JJ, Denyer SP, Heard CM (2017) Potentiated virucidal activity of pomegranate rind extract (PRE) and punicalagin against Herpes simplex virus (HSV) when co-administered with zinc (II) ions, and antiviral activity of PRE against HSV and aciclovir-resistant HSV. PLoS ONE 12(6):e0179291. https://doi.org/10.1371/journal.pone.0179291
Xu Y, Shi C, Wu Q, Zheng Z, Liu P, Li G et al (2017) Antimicrobial activity of punicalagin against staphylococcus aureus and its effect on biofilm formation. Foodborne Pathog Dis 14(5):282–287. https://doi.org/10.1089/fpd.2016.2226
Xu J, Cao K, Liu X, Zhao L, Feng Z, Liu J (2021) Punicalagin regulates signaling pathways in inflammation-associated chronic diseases. Antioxidants 11(1):29. https://doi.org/10.3390/antiox11010029
Tang L, Li T, Zhang B, Zhang Z, Sun X, Zhu Y et al (2022) Punicalagin alleviates psoriasis by inhibiting NF-kappaB-mediated IL-1beta transcription and caspase-1-regulated IL-1beta secretion. Front Pharmacol 13:817526. https://doi.org/10.3389/fphar.2022.817526
Huang H, Regan KM, Wang F, Wang D, Smith DI, van Deursen JM et al (2005) Skp2 inhibits FOXO1 in tumor suppression through ubiquitin-mediated degradation. Proc Natl Acad Sci U S A 102(5):1649–1654. https://doi.org/10.1073/pnas.0406789102
Wang G, Chan CH, Gao Y, Lin HK (2012) Novel roles of Skp2 E3 ligase in cellular senescence, cancer progression, and metastasis. Chin J Cancer 31(4):169–177. https://doi.org/10.5732/cjc.011.10319
Nakayama K, Nagahama H, Minamishima YA, Miyake S, Ishida N, Hatakeyama S et al (2004) Skp2-mediated degradation of p27 regulates progression into mitosis. Dev Cell. https://doi.org/10.1016/s1534-5807(04)00131-5
Bochis OV, Irimie A, Pichler M, Berindan-Neagoe I (2015) The role of Skp2 and its substrate CDKN1B (p27) in colorectal cancer. J Gastrointestin Liver Dis. https://doi.org/10.15403/jgld.2014.1121.242.skp2
Griffiths CEM, Armstrong AW, Gudjonsson JE, Barker JNWN (2021) Psoriasis. The Lancet 397(10281):1301–1315. https://doi.org/10.1016/s0140-6736(20)32549-6
Ji AL, Rubin AJ, Thrane K, Jiang S, Reynolds DL, Meyers RM et al (2020) Multimodal analysis of composition and spatial architecture in human squamous cell carcinoma. Cell 182(6):1661–1662. https://doi.org/10.1016/j.cell.2020.08.043
Pogorzelska-Antkowiak A (2022) Lichen planus-like keratosis: what do we know about it? Clin Exp Dermatol 47(11):1923–1927. https://doi.org/10.1111/ced.15318
Al-Khawalde AAA, Abukhalil MH, Jghef MM, Alfwuaires MA, Alaryani FS, Aladaileh SH et al (2022) Punicalagin protects against the development of methotrexate-induced hepatotoxicity in mice via activating Nrf2 signaling and decreasing oxidative stress inflammation, and cell death. Int J Mol Sci 23(20):12334. https://doi.org/10.3390/ijms232012334
Ge G, Bai J, Wang Q, Liang X, Tao H, Chen H et al (2022) Punicalagin ameliorates collagen-induced arthritis by downregulating M1 macrophage and pyroptosis via NF-kappaB signaling pathway. Sci China Life Sci 65(3):588–603. https://doi.org/10.1007/s11427-020-1939-1
Lo J, Liu CC, Li YS, Lee PY, Liu PL, Wu PC et al (2022) Punicalagin attenuates LPS-induced inflammation and ROS production in microglia by inhibiting the MAPK/NF-kappaB signaling pathway and NLRP3 inflammasome activation. J Inflamm Res 15:5347–5359. https://doi.org/10.2147/JIR.S372773
Cai Z, Moten A, Peng D, Hsu CC, Pan BS, Manne R et al (2020) The Skp2 pathway: a critical target for cancer therapy. Semin Cancer Biol 67(Pt 2):16–33. https://doi.org/10.1016/j.semcancer.2020.01.013
Bloom J, Pagano M (2003) Deregulated degradation of the cdk inhibitor p27 and malignant transformation. Semin Cancer Biol 13(1):41–47. https://doi.org/10.1016/s1044-579x(02)00098-6
Fujita T, Liu W, Doihara H, Date H, Wan Y (2008) Dissection of the APCCdh1-Skp2 cascade in breast cancer. Clin Cancer Res 14(7):1966–1975. https://doi.org/10.1158/1078-0432.CCR-07-1585
Ji P, Jiang H, Rekhtman K, Bloom J, Ichetovkin M, Pagano M et al (2004) An Rb-Skp2-p27 pathway mediates acute cell cycle inhibition by Rb and is retained in a partial-penetrance Rb mutant. Mol Cell 16(1):47–58. https://doi.org/10.1016/j.molcel.2004.09.029
Signoretti S, Di Marcotullio L, Richardson A, Ramaswamy S, Isaac B, Rue M et al (2016) Oncogenic role of the ubiquitin ligase subunit Skp2 in human breast cancer. J Clin Invest 126(11):4387. https://doi.org/10.1172/JCI90690
Xia X, Liu X, Chai R, Xu Q, Luo Z, Gu J et al (2021) USP10 exacerbates neointima formation by stabilizing Skp2 protein in vascular smooth muscle cells. J Biol Chem 297(5):101258. https://doi.org/10.1016/j.jbc.2021.101258
Xia B, Pang L, Zhuang ZX, Liu JJ (2016) Biotin-mediated epigenetic modifications: potential defense against the carcinogenicity of benzo[a]pyrene. Toxicol Lett 241:216–224. https://doi.org/10.1016/j.toxlet.2015.11.010
Li Z, Chen Q, Wang J, Pan X, Lu W (2021) Research progress and application of bioorthogonal reactions in biomolecular analysis and disease diagnosis. Top Curr Chem 379(6):39. https://doi.org/10.1007/s41061-021-00352-8
Das J (2011) Aliphatic diazirines as photoaffinity probes for proteins: recent developments. Chem Rev 111(8):4405–4417. https://doi.org/10.1021/cr1002722
Zhu Y, Ouyang Z, Du H, Wang M, Wang J, Sun H et al (2022) New opportunities and challenges of natural products research: when target identification meets single-cell multiomics. Acta Pharm Sin B 12(11):4011–4039. https://doi.org/10.1016/j.apsb.2022.08.022
Acknowledgements
This study was supported by the Joint Funding Project of Municipal Schools (Colleges) of Science and Technology Program of Guangzhou (No. 202102010192); The Specific Fund of State Key Laboratory of Dampness Syndrome of Chinese Medicine (SZ2021ZZ23); The Specific Fund of “Young Talents Program” of Guangdong College of Traditional Chinese Medicine (SZ2022QN10); The 2020 Guangdong Provincial Science and Technology Innovation Strategy Special Fund (Guangdong-Hong Kong-Macau Joint Lab) (2020B1212030006); The Specific Research Fund for TCM Science and Technology of Guangdong Provincial Hospital of Chinese Medicine (YN2018QJ03); The Specific Fund for the Administration of Traditional Chinese Medicine of Guangdong Province (20222066); Science and Technology Planning Project of Guangzhou (202102021001); The China-Dutch special projects of Guangdong Provincial Hospital of Chinese Medicine (YN2019HL01, YN2019HL02).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflicts of interest in this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tang, L., Zhang, B., Li, G. et al. Punicalagin alleviates the hyperproliferation of keratinocytes in psoriasis through inhibiting SKP2 expression. J Nat Med 77, 712–720 (2023). https://doi.org/10.1007/s11418-023-01711-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11418-023-01711-z