Abstract
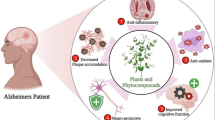
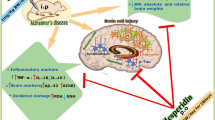
This study aims to clarify the bioactive constituents responsible for the anti-dementia effects of Ocimum sanctum Linn. ethanolic extract (OS) using olfactory bulbectomized (OBX) mice, an animal model of dementia. The effects of OS or its extract further fractionated with n-hexane (OS-H), ethyl acetate (OS-E), and n-butanol (OS-B) on the spatial cognitive deficits of OBX mice were elucidated by the modified Y-maze tests. The effects of the major constituents of the most active OS fraction were also elucidated using the reference drug donepezil. The administration of OS and OS-E ameliorated the spatial cognitive deficits caused by OBX, whereas OS-H or OS-B had no effect. Two major constituents, ursolic acid (URO) and oleanolic acid (OLE), and three minor constituents were isolated from OS-E. URO (6 and 12 mg/kg) and OLE (24 mg/kg) attenuated the OBX-induced cognitive deficits. URO (6 mg/kg) and donepezil reversed the OBX-induced down-regulation of vascular endothelial growth factor (VEGF) and choline acetyltransferase expression levels in the hippocampus. URO inhibited the ex vivo activity of acetylcholinesterase with similar efficacy to donepezil. URO inhibited the in vitro activity of acetylcholinesterase (IC50 = 106.5 μM), while the effects of OS, OS-E, and other isolated compounds were negligible. These findings suggest that URO and OLE are responsible for the anti-dementia action of OS extract, whereas URO possesses a more potent anti-dementia effect than its isomer OLE. The effects of URO are, at least in part, mediated by normalizing the function of central cholinergic systems and VEGF protein expression.
Graphical abstract










Similar content being viewed by others
References
Olivari BS, French ME, McGuire LC (2020) The public health road map to respond to the growing dementia crisis. Innov Aging 4:igz043
Cummings J, Lee G, Zhong K, Fonseca J, Taghva K (2021) Alzheimer’s disease drug development pipeline: 2021. Alzheimers Dement 7:e12179
Kovács T (2009) Therapy of Alzheimer disease. Neuropsychopharmacol Hung 11:27–33
Casey DA, Antimisiaris D, O’Brien J (2010) Drugs for Alzheimer’s disease: are they effective? Pharm Ther 35(4):208–211
Du X, Wang X, Geng M (2018) Alzheimer’s disease hypothesis and related therapies. Transl Neurodegener 7:2
Cohen MM (2014) Tulsi-Ocimum sanctum: a herb for all reasons. J Ayurveda Integr Med 5:251
Rege NN, Thatte UM, Dahanukar SA (1999) Adaptogenic properties of six rasayana herbs used in Ayurvedic medicine. Phytother Res 13:275–291
Pattanayak P, Behera P, Das D, Panda SK (2010) Ocimum sanctum Linn. A reservoir plant for therapeutic applications: an overview. Pharmacogn Rev 4:95
Le XT, Nguyen HT, Nguyen TV, Pham HTN, Nguyen PT, Nguyen KM et al (2021) Ocimum sanctum Linn. extract improves cognitive deficits in olfactory bulbectomized mice via the enhancement of central cholinergic systems and VEGF expression. Evid Based Complement Alternat Med 2021:6627648
Bobkova N, Vorobyov V, Medvinskaya N, Aleksandrova I, Nesterova I (2008) Interhemispheric EEG differences in olfactory bulbectomized rats with different cognitive abilities and brain beta-amyloid levels. Brain Res 1232:185–194
Avetisyan A, Samokhin A, Alexandrova I, Zinovkin R, Simonyan R, Bobkova N (2016) Mitochondrial dysfunction in neocortex and hippocampus of olfactory bulbectomized mice, a model of Alzheimer’s disease. Biochem Mosc 81:615–623
Hu J, Wang X, Liu D, Wang Q, Zhu LQ (2012) Olfactory deficits induce neurofilament hyperphosphorylation. Neurosci Lett 506:180–183
Hozumi S, Nakagawasai O, Tan-No K, Niijima F, Yamadera F, Murata A et al (2003) Characteristics of changes in cholinergic function and impairment of learning and memory-related behavior induced by olfactory bulbectomy. Behav Brain Res 138:9–15
Mizuki D, Qi Z, Tanaka K, Fujiwara H, Ishikawa T, Higuchi Y et al (2014) Butea superba–induced amelioration of cognitive and emotional deficits in olfactory bulbectomized mice and putative mechanisms underlying its actions. J Pharmacol Sci 124:457–467
Song C, Leonard BE (2005) The olfactory bulbectomised rat as a model of depression. Neurosci Biobehav Rev 29:627–647
Hohman TJ, Bell SP, Jefferson AL, AsDN I (2015) The role of vascular endothelial growth factor in neurodegeneration and cognitive decline: exploring interactions with biomarkers of Alzheimer disease. JAMA Neurol 72:520–529
Kimura K, Matsumoto K, Ohtake H, Oka J-I, Fujiwara H (2018) Endogenous acetylcholine regulates neuronal and astrocytic vascular endothelial growth factor expression levels via different acetylcholine receptor mechanisms. Neurochem Int 118:42–51
Inada C, Le XT, Tsuneyama K, Fujiwara H, Miyata T, Matsumoto K (2013) Endogenous acetylcholine rescues NMDA-induced long-lasting hippocampal cell damage via stimulation of muscarinic M1 receptors: Elucidation using organic hippocampal slice cultures. Eur J Pharmacol 699:150–159
Inada C, Niu Y, Matsumoto K, Le XT, Fujiwara H (2014) Possible involvement of VEGF signaling system in rescuing effect of endogenous acetylcholine on NMDA-induced long-lasting hippocampal cell damage in organotypic hippocampal slice cultures. Neurochem Int 75:39–47
Gupta P, Yadav DK, Siripurapu KB, Palit G, Maurya R (2007) Constituents of Ocimum sanctum with antistress activity. J Nat Prod 70:1410–1416
Sarkar D, Srimany A, Pradeep T (2012) Rapid identification of molecular changes in tulsi (Ocimum sanctum Linn) upon ageing using leaf spray ionization mass spectrometry. Analyst 137:4559–4563
Gupta S, Prakash J, Srivastava S (2002) Validation of traditional claim of Tulsi, Ocimum sanctum Linn. as a medicinal plant. Indian J Exp Biol 40(7):765–773
Baliga MS, Rao S, Rai MP, D’souza P (2016) Radio protective effects of the Ayurvedic medicinal plant Ocimum sanctum Linn. (Holy Basil): a memoir. J Cancer Res Ther 12:20
Nguyen HT, Le XT, Phung HN, Nguyen TV, Nguyen KM (2020) Putative constituents contributing to the antidepressant-like effects of Ocimum sanctum in olfactory bulbectomized-mice. J Med Materials 25:186–192
Liang W, Zhao X, Feng J, Song F, Pan Y (2016) Ursolic acid attenuates beta-amyloid-induced memory impairment in mice. Arq Neuropsiquiatr 74:482–488
Mirza FJ, Amber S, Hassan D, Ahmed T, Zahid S (2021) Rosmarinic acid and ursolic acid alleviate deficits in cognition, synaptic regulation and adult hippocampal neurogenesis in an Aβ1-42-induced mouse model of Alzheimer’s disease. Phytomedicine 83:153490
Wang K, Sun W, Zhang L, Guo W, Xu J, Liu S et al (2018) Oleanolic acid ameliorates Aβ25-35 injection-induced memory deficit in Alzheimer’s disease model rats by maintaining synaptic plasticity. CNS Neurol Disord Drug Targets 17:389–399
Zhao L, Wang J-L, Liu R, Li X-X, Li J-F, Zhang L (2013) Neuroprotective, anti-amyloidogenic and neurotrophic effects of apigenin in an Alzheimer’s disease mouse model. Molecules 18:9949–9965
Yoo DY, Choi JH, Kim W, Nam SM, Jung HY, Kim JH et al (2013) Effects of luteolin on spatial memory, cell proliferation, and neuroblast differentiation in the hippocampal dentate gyrus in a scopolamine-induced amnesia model. Neurol Res 35:813–820
Nguyen HT, Le XT, Nguyen TV, Pham HTN, Nguyen KM, Matsumoto K (2021) The antidepressant-like effects of an n-butanol fraction of Ocimum sanctum extract in unpredictable chronic mild stress-induced depression in mice. VJSTE 63(4):55–61
Le XT, Pham HTN, Do PT, Fujiwara H, Tanaka K, Li F et al (2013) Bacopa monnieri ameliorates memory deficits in olfactory bulbectomized mice: possible involvement of glutamatergic and cholinergic systems. Neurochem Res 38:2201–2215
Wang Y-J, Lu J, Wu D-m, Zheng Z-h, Zheng Y-L, Wang X-h et al (2011) Ursolic acid attenuates lipopolysaccharide-induced cognitive deficits in mouse brain through suppressing p38/NF-κB mediated inflammatory pathways. Neurobiol Learn Mem 96:156–165
Ma CM, Wu XH, Hattori M, Wang XJ, Kano Y (2009) HCV protease inhibitory, cytotoxic and apoptosis-inducing effects of oleanolic acid derivatives. J Pharm Pharm Sci 12:243–248
Yamada M, Hayashida M, Zhao Q, Shibahara N, Tanaka K, Miyata T et al (2011) Ameliorative effects of yokukansan on learning and memory deficits in olfactory bulbectomized mice. J Ethnopharmacol 135:737–746
Zhao Q, Yokozawa T, Tsuneyama K, Tanaka K, Miyata T, Shibahara N et al (2011) Chotosan (Diaoteng San)-induced improvement of cognitive deficits in senescence-accelerated mouse (SAMP8) involves the amelioration of angiogenic/neurotrophic factors and neuroplasticity systems in the brain. Chin Med 6:33
Ellman GL, Courtney KD, Andres V Jr, Featherstone RM (1961) A new and rapid colorimetric determination of acetylcholinesterase activity. Biochem Pharmacol 7:88–95
Kraeuter A-K, Guest PC, Sarnyai Z (2019) The Y-maze for assessment of spatial working and reference memory in mice. Methods Mol Biol 1916:105–111
Dellu F, Contarino A, Simon H, Koob G, Gold L (2000) Genetic differences in response to novelty and spatial memory using a two-trial recognition task in mice. Neurobiol Learn Mem 73:31–48
Seebacher W, Simic N, Weis R, Saf R, Kunert O (2003) Complete assignments of 1H and 13C NMR resonances of oleanolic acid, 18α-oleanolic acid, ursolic acid and their 11-oxo derivatives. Magn Reson Chem 41:636–638
Alwahsh MAA, Khairuddean M, Chong WK (2015) Chemical constituents and antioxidant activity of Teucrium barbeyanum Aschers. Rec Nat Prod 9:159–163
Hwang SH, Kim HY, Zuo G, Wang Z, Lee JY, Lim SS (2018) Anti-glycation, carbonyl trapping and anti-inflammatory activities of chrysin derivatives. Molecules 23:1752
Saunders NL, Summers MJ (2010) Attention and working memory deficits in mild cognitive impairment. J Clin Exp Neuropsychol 32:350–357
Yehuda S, Rabinovitz S (2014) Olfactory bulbectomy as a putative model for Alzheimer’: the protective role of essential fatty acids. PharmaNutrition 2:12–18
Masurkar AV, Devanand DP (2014) Olfactory dysfunction in the elderly: basic circuitry and alterations with normal aging and Alzheimer’s disease. Curr Geriatr Rep 3:91–100
Djordjevic J, Jones-Gotman M, De Sousa K, Chertkow H (2008) Olfaction in patients with mild cognitive impairment and Alzheimer’s disease. Neurobiol Aging 29:693–706
Klein J, Yan X, Johnson A, Tomljanovic Z, Zou J, Polly K et al (2021) Olfactory impairment is related to Tau pathology and neuroinflammation in Alzheimer’s disease. J Alzheimers Dis 80:1051–1065
Jeong DW, Kim YH, Kim HH, Ji HY, Yoo SD, Choi WR et al (2007) Dose-linear pharmacokinetics of oleanolic acid after intravenous and oral administration in rats. Biopharm Drug Disposition 28:51–57
Ren C, Kong D, Ning C, Xing H, Cheng Y, Zhang Y et al (2021) Improved pharmacokinetic characteristics of ursolic acid in rats following intratracheal instillation and nose-only inhalation exposure. J Pharm Sci 110:905–913
Chen Q, Luo S, Zhang Y, Chen Z (2011) Development of a liquid chromatography–mass spectrometry method for the determination of ursolic acid in rat plasma and tissue: application to the pharmacokinetic and tissue distribution study. Anal Bioanal Chem 399:2877–2884
Cao L, Jiao X, Zuzga DS, Liu Y, Fong DM, Young D et al (2004) VEGF links hippocampal activity with neurogenesis, learning and memory. Nat Genet 36:827–835
Simpson J, Yates C, Gordon A, St Clair D (1984) Olfactory tubercle choline acetyltransferase activity in Alzheimer-type dementia, Down’s syndrome and Huntington’s chorea. J Neurol Neurosurg Psychiatry 47:1138
Acknowledgements
This research is funded by the Vietnam National Foundation for Science and Technology Development (NAFOSTED) under Grant Number 106-YS.05-2016.22.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Nguyen, H.T., Le, X.T., Van Nguyen, T. et al. Ursolic acid and its isomer oleanolic acid are responsible for the anti-dementia effects of Ocimum sanctum in olfactory bulbectomized mice. J Nat Med 76, 621–633 (2022). https://doi.org/10.1007/s11418-022-01609-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11418-022-01609-2