Abstract
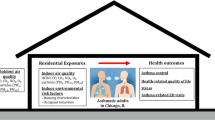
This investigation explored the association between indoor environmental factors and childhood asthma in Yancheng, China. Asthma case (201 children with recurrent asthma) and control cohorts (242 healthy subjects) were recruited from a Traditional Chinese Medical (TCM) Hospital in Yancheng city, based on the results of an ISAAC questionnaire. Questionnaires regarding environmental risk factors were completed by the child’s primary caregivers. To compare data on environmental VOCs and formaldehyde contents between asthma and control cohorts, we passively conducted a 10-day indoor and outdoor sampling. Breastfeeding was a major protective indoor environmental factor for recurrent asthma (adjusted odds ratio [aOR]: 0.368, 95% confidence interval [CI]: 0.216–0.627). Our analysis revealed that childhood recurrent asthma was intricately linked to a family history of asthma. Recurrent asthma was also associated with passive smoking [aOR2.115 (95%-CI 1.275–3.508)]. Analogous correlations were observed between household renovation or new furniture introduction and recurrent asthma [aOR3.129(95%-CI1.542–6.347)]. Benzene and formaldehyde were present in all examined homes. Enhanced benzene and formaldehyde concentrations were strongly evident among asthma versus control cohorts, and they were strongly correlated with augmented recurrent asthma risk. Home environment heavily regulates incidences of childhood recurrent asthma. Hence, actions against the indoor environmental risk factors described in this study may assist in the prevention of recurrent asthma among children.
Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article.
References
Abarca NE, Garro AC, Pearlman DN (2018) Relationship between breastfeeding and asthma prevalence in young children exposed to adverse childhood experiences. J Asthma 56(2):142–151. https://doi.org/10.1080/02770903.2018.1441869
Ambade B, Ghosh S (2013) Characterization of PM10 in the ambient air during Deepawali festival of Rajnandgaon district India. Natural Hazards 69(1):589–598. https://doi.org/10.1007/s11069-013-0725-8
Ambade B, Sethi SS, Kurwadkar S, Mishra P, Tripathee L (2022) Accumulation of polycyclic aromatic hydrocarbons (PAHs) in surface sediment residues of Mahanadi River Estuary: Abundance, source, and risk assessment. Mar Pollut Bull 183:114073. https://doi.org/10.1016/j.marpolbul.2022.114073
Annika Klopp LV, Becker AB, Subbarao P, Mandhane PJ, Stuart E, Diana L, Lefebvre Malcolm BA (2017) Modes of infant feeding and the risk of childhood asthma: a prospective birth cohort study. J Pediatr 190:192–199.e192. https://doi.org/10.1016/j.jpeds.2017.07.012
Arif AA (2018) The association of prenatal risk factors with childhood asthma. J Asthma 56(10):1056–1061. https://doi.org/10.1080/02770903.2018.1515224
Asher MI, Montefort S, Björkstén B, Lai CKW, Strachan DP, Weiland SK, Williams H (2006) Worldwide time trends in the prevalence of symptoms of asthma, allergic rhinoconjunctivitis, and eczema in childhood: ISAAC phases one and three repeat multicountry cross-sectional surveys. Lancet 368(9537):733–743. https://doi.org/10.1016/s0140-6736(06)69283-0
Athanasios K (2019) ‘Cocktails and dreams’: the indoor air quality that people are exposed to while sleeping. Curr Opin Environ Sci Health 8:6–9. https://doi.org/10.1016/j.coesh.2018.12.005
Chang T, Wang J, Lu J, Shen Z, Huang Y, Sun J, Xu H, Wang X, Ren D, Cao J (2019) Evaluation of indoor air pollution during decorating process and inhalation health risks in Xi’an, China: a case study. Aerosol and Air Quality Res 19(4):854–864. https://doi.org/10.4209/aaqr.2018.07.0261
Eassey D, Reddel HK, Foster JM, Kirkpatrick S, Locock L, Ryan K, Smith L (2018) “…I've said I wish I was dead, you'd be better off without me”: a systematic review of people's experiences of living with severe asthma. J Asthma 56(3):311–322. https://doi.org/10.1080/02770903.2018.1452034
El-Helaly M, Abdel-Elah K, Haussein A, Shalaby H (2011) Paternal occupational exposures and the risk of congenital malformations — a case-control study. Int J Occupat Med Environ Health 24(2). https://doi.org/10.2478/s13382-011-0019-x
Franck U, Weller A, Röder SW, Herberth G, Junge KM, Kohajda T, von Bergen M, Rolle-Kampczyk U, Diez U, Borte M, Lehmann I (2014) Prenatal VOC exposure and redecoration are related to wheezing in early infancy. Environ Int 73:393–401. https://doi.org/10.1016/j.envint.2014.08.013
Gilbert KC, Mirabelli MC, Ragan K, Gower EW, Ashburn NP, Gower WA (2015) Pediatric asthma deaths in North Carolina, 1999-2012. J Allerg Clin Immunol 135(2):AB86. https://doi.org/10.1016/j.jaci.2014.12.1212
Hallit S, Sacre H, Kheir N, Hallit R, Waked M, Salameh P (2021) Prevalence of asthma, its correlates, and validation of the Pre-School Asthma Risk Factors Scale (PS-ARFS) among preschool children in Lebanon. Allergologia et Immunopathologia 49(1):40–49. https://doi.org/10.15586/aei.v49i1.25
Harvey SM, Murphy VE, Gibson PG, Collison A, Robinson P, Sly PD, Mattes J, Jensen ME (2020) Maternal asthma, breastfeeding, and respiratory outcomes in the first year of life. Pediatr Pulmonol 55(7):1690–1696. https://doi.org/10.1002/ppul.24756
Hu Y, Chen Y, Liu S, Jiang F, Wu M, Yan C, Tan J, Yu G, Hu Y, Yin Y, Qu J, Li S, Tong S (2021) Breastfeeding duration modified the effects of neonatal and familial risk factors on childhood asthma and allergy: a population-based study. Respirator Res 22(1). https://doi.org/10.1186/s12931-021-01644-9
Huang L, Wei Y, Zhang L, Ma Z, Zhao W (2021) Estimates of emission strengths of 43 VOCs in wintertime residential indoor environments Beijing. Sci Total Environ 793:148623. https://doi.org/10.1016/j.scitotenv.2021.148623
Huang S, Wei W, Weschler LB, Salthammer T, Kan H, Bu Z, Zhang Y (2017) Indoor formaldehyde concentrations in urban China: preliminary study of some important influencing factors. Sci Total Environ 590-591:394–405. https://doi.org/10.1016/j.scitotenv.2017.02.187
Huang TP, Liu PH, Lien ASY, Yang SL, Chang HH, Yen HR (2013) Characteristics of traditional Chinese medicine use in children with asthma: a nationwide population-based study. Allergy 68(12):1610–1613. https://doi.org/10.1111/all.12273
Huo X, Chu S, Hua L, Bao Y, Du L, Xu J, Zhang J (2018) The effect of breastfeeding on the risk of asthma in high-risk children: a case-control study in Shanghai China. BMC Preg Childbirth 18(1). https://doi.org/10.1186/s12884-018-1936-5
Hwang G, Yoon C, Choi J (2011) A case-control study: exposure assessment of VOCs and formaldehyde for asthma in children. Aerosol and Air Quality Res 11(7):908–914. https://doi.org/10.4209/aaqr.2011.05.0072
Ibrahim NM, Almarzouqi FI, Al Melaih FA, Farouk H, MAL A, Jassim FM (2021) Prevalence of asthma and allergies among children in the United Arab Emirates: a cross-sectional study. World Allerg Org J 14(10):100588. https://doi.org/10.1016/j.waojou.2021.100588
Julia A, Santigao P, Ricardo B, Amat A, Ruiz I, Mora A, Escolano S, Chofre L (2020) Asthma prevalence and risk factors in school children: The RESPIR longitudinal study. Allergologia et Immunopathol 48(3):223–231. https://doi.org/10.1016/j.aller.2019.06.003
Kansen HM, Le TM, Uiterwaal C, van Ewijk BE, Balemans WAF, Gorissen DMW, de Vries E, van Velzen MF, Slabbers G, Meijer Y, Knulst AC, van der Ent CK, van Erp FC (2020) Prevalence and predictors of uncontrolled asthma in children referred for asthma and other atopic diseases. J Asthma Allerg 13:67–75. https://doi.org/10.2147/jaa.s231907
Kodate J, Marganwar R, Dhurvey V, Dhawas S, Urkude R (2016) Assessment of groundwater quality with special emphasison fluoride contamination in some villages of Chandrapur district of Maharashtra,India. IOSR J Environ Sci , Toxicol Food Technol 10(3):15–26. https://doi.org/10.9790/2402-10311526
Kuang H, Li Z, Lv X, Wu P, Tan J, Wu Q, Li Y, Jiang W, Pang Q, Wang Y, Fan R (2021) Exposure to volatile organic compounds may be associated with oxidative DNA damage-mediated childhood asthma. Ecotoxicol Environ Safety 210:111864. https://doi.org/10.1016/j.ecoenv.2020.111864
Kumar A, Ambade B, Sankar TK, Sethi SS, Kurwadkar S (2020) Source identification and health risk assessment of atmospheric PM2.5-bound polycyclic aromatic hydrocarbons in Jamshedpur, India. Sustain Cities Soc 52:101801. https://doi.org/10.1016/j.scs.2019.101801
Luo S, Sun Y, Hou J, Kong X, Wang P, Zhang Q, Sundell J (2018) Pet keeping in childhood and asthma and allergy among children in Tianjin area China. Plos One 13(5):e0197274. https://doi.org/10.1371/journal.pone.0197274
Madureira J, Paciência I, Ramos E, Barros H, Pereira C, Teixeira J P, Fernandes E d O,2015. Children’s health and indoor air quality in primary schools and homes in Portugal—study design. J Toxicol Environ Health, Part A 78(13-14), 915-930. https://doi.org/10.1080/15287394.2015.1048926
Mahon GM, Koppelman GH, Vonk JM (2021) Grandmaternal smoking, asthma and lung function in the offspring: the Lifelines cohort study. Thorax 76(5):441–447. https://doi.org/10.1136/thoraxjnl-2020-215232
Merianos AL, Jandarov RA, Mahabee-Gittens EM (2018) Association of secondhand smoke exposure with asthma symptoms, medication use, and healthcare utilization among asthmatic adolescents. J Asthma 56(4):369–379. https://doi.org/10.1080/02770903.2018.1463379
Mirzakhani H, Carey VJ, Zeiger R, Bacharier LB, O'Connor GT, Schatz MX, Laranjo N, Weiss ST, Litonjua AA (2019) Impact of parental asthma, prenatal maternal asthma control, and vitamin D status on risk of asthma and recurrent wheeze in 3-year-old children. Clin Exp Allergy 49(4):419–429. https://doi.org/10.1111/cea.13320
Morales E (2019) Genetics and gene-environment interactions in childhood and adult onset asthma. Front Pediatr 7. https://doi.org/10.3389/fped.2019.00499
Neophytou AM, Oh SS, Hu D, Huntsman S, Eng C, Rodríguez-Santana JR, Kumar R, Balmes JR, Eisen EA, Burchard EG (2019) In utero tobacco smoke exposure, DNA methylation, and asthma in Latino children. Environ Epidemiol 3(3):e048. https://doi.org/10.1097/ee9.0000000000000048
Peel AM, Wilkinson M, Sinha A, Loke YK, Fowler SJ, Wilson AM (2020) Volatile organic compounds associated with diagnosis and disease characteristics in asthma – a systematic review. Respiratory Medicine 169:105984. https://doi.org/10.1016/j.rmed.2020.105984
Pennington AF, Strickland MJ, Klein M, Zhai X, Bates JT, Drews-Botsch C, Hansen C, Russell AG, Tolbert PE, Darrow LA (2018) Exposure to mobile source air pollution in early-life and childhood asthma incidence. Epidemiology 29(1):22–30. https://doi.org/10.1097/ede.0000000000000754
Rodrigues dos Santos R, Gregório J, Castanheira L, Fernandes AS (2020) Exploring volatile organic compound exposure and its association with wheezing in children under 36 months: a cross-sectional study in South Lisbon, Portugal. Int J Environ Res Public Health 17(18):6929. https://doi.org/10.3390/ijerph17186929
Sankar TK, Kumar A, Mahto DK, Das KC, Narayan P, Fukate M, Awachat P, Padghan D, Mohammad F, Al-Lohedan HA, Soleiman AA, Ambade B (2023) The health risk and source assessment of polycyclic aromatic hydrocarbons (PAHs) in the soil of industrial cities in India. Toxics 11(6):515. https://doi.org/10.3390/toxics11060515
Shakerkhatibi M, Benis KZ, Asghari-Jafarabadi M, Sadeghi-Bazarghani H, Allahverdipour H, Oskouei DS, Fatehifar E, Farajzadeh M, Yadeghari A, Ansarin K, Jafari R, Zakeri A, Moshashaei P, Behnami A (2021) Air pollution-related asthma profiles among children/adolescents: a multi-group latent class analysis. Ecotoxicol Environ Safety 219:112344. https://doi.org/10.1016/j.ecoenv.2021.112344
Stanford RH, Buikema AR, Riedel AA, Camargo CA, Rey GG, Chapman KR (2012) Asthma controller delay and recurrence risk after an emergency department visit or hospitalization. Respirator Med 106(12):1631–1638. https://doi.org/10.1016/j.rmed.2012.08.017
Sun Y, Hou J, Sheng Y, Kong X, Weschler LB, Sundell J (2019) Modern life makes children allergic. A cross-sectional study: associations of home environment and lifestyles with asthma and allergy among children in Tianjin region, China. Int Arch Occupational Environ Health 92(4):587–598. https://doi.org/10.1007/s00420-018-1395-3
Wag J, Huang K, Feng G, Song J (2020) Analysis of winter formaldehyde and volatile organic compound pollution characteristics of residential kitchens in severe cold regions of northeast China. Indoor Built Environ 30(8):1226–1243. https://doi.org/10.1177/1420326x20937462
Wang J, Janson C, Jogi R, Forsberg B, Gislason T, Holm M, Torén K, Malinovschi A, Sigsgaard T, Schlünssen V, Svanes C, Johannessen A, Bertelsen RJ, Franklin KA, Norbäck D (2021a) A prospective study on the role of smoking, environmental tobacco smoke, indoor painting and living in old or new buildings on asthma, rhinitis and respiratory symptoms. Environ Res 192:110269. https://doi.org/10.1016/j.envres.2020.110269
Wang J, Zhang Y, Li B, Zhao Z, Huang C, Zhang X, Deng Q, Lu C, Qian H, Yang X, Sun Y, Sundell J, Norbäck D (2021b) Asthma and allergic rhinitis among young parents in China in relation to outdoor air pollution, climate and home environment. Sci Total Environ 751:141734. https://doi.org/10.1016/j.scitotenv.2020.141734
Yang S, Perret V, Hager Jörin C, Niculita-Hirzel H, Goyette Pernot J, Licina D (2020) Volatile organic compounds in 169 energy-efficient dwellings in Switzerland. Indoor Air 30(3):481–491. https://doi.org/10.1111/ina.12667
Zhang H-l, Wang B-y, Luo Y, Li Y, Cai C-s, Huang L-l, He B-h, Cai J, Li Z-y, Mai A-d, Guo Y (2020) Association of pet-keeping in home with self-reported asthma and asthma-related symptoms in 11611 school children from China. J Asthma 58(12):1555–1564. https://doi.org/10.1080/02770903.2020.1818772
Zhang J, Sun C, Liu W, Zou Z, Zhang Y, Li B, Zhao Z, Deng Q, Yang X, Zhang X, Qian H, Sun Y, Sundell J, Huang C (2018) Associations of household renovation materials and periods with childhood asthma, in China: a retrospective cohort study. Environ Int 113:240–248. https://doi.org/10.1016/j.envint.2018.02.001
Zhang Y, Li B, Huang C, Yang X, Qian H, Deng Q, Zhao Z, Li A, Zhao J, Zhang X, Qu F, Hu Y, Yang Q, Wang J, Zhang M, Wang F, Zheng X, Lu C, Liu Z et al (2013) Ten cities cross-sectional questionnaire survey of children asthma and other allergies in China. Chinese Sci Bull 58(34):4182–4189. https://doi.org/10.1007/s11434-013-5914-z
Zhang Z, Weichenthal S, Kwong JC, Burnett RT, Hatzopoulou M, Jerrett M, van Donkelaar A, Bai L, Martin RV, Copes R, Lu H, Lakey P, Shiraiwa M, Chen H (2021) A population-based cohort study of respiratory disease and long-term exposure to iron and copper in fine particulate air pollution and their combined impact on reactive oxygen species generation in human lungs. Environ Sci Technol 55(6):3807–3818. https://doi.org/10.1021/acs.est.0c05931
Acknowledgements
The authors would like to thank all the reviewers who participated in the review and MJEditor (http://www.mjeditor.com) for its linguistic assistance during the preparation of this manuscript.
Funding
This study was supported in part by grants from the Natural Science Foundation of the Jiangsu Higher Education Institutions of China [20KJA610002] and the “Qing Lan Project” of Colleges and Universities in JiangSu Province.
Author information
Authors and Affiliations
Contributions
Tianming Chen conceived and designed the studies. Baoping Zhang performed the studies and drafted the manuscript. Chuntao Yin, Yang Yuan, and Zhibin Xia contributed data collection. Xu Jiang contributed data analysis. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable
Consent for publication
Not applicable
Competing interests
The authors declare no competing interests.
Additional information
Responsible Editor: Lotfi Aleya
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, B., Xia, Z., Jiang, X. et al. Indoor environment in relation to recurrent childhood asthma in Yancheng, China: a hospital-based case-control study. Environ Sci Pollut Res 30, 102212–102221 (2023). https://doi.org/10.1007/s11356-023-29631-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-023-29631-1