Abstract
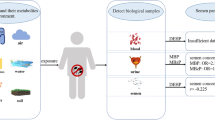
Previous studies have reported that exposure to phthalates and polycyclic aromatic hydrocarbons (PAHs) is individually associated with altered semen quality, but no human studies have evaluated their joint effects of exposure mixtures, a more real-world scenario. We aimed to explore urinary metabolite mixtures of phthalates and PAHs in associations with semen quality. Repeated spot-urine samples gathered from 695 men attending a fertility clinic were analyzed for urinary metabolites of eight phthalates and ten monohydroxylated-PAHs (OH-PAHs). Principal component analysis (PCA)-multivariable linear regression (MLR) model, quantile g-computation (qg-comp), and Bayesian kernel machine regression (BKMR) were applied to estimate the associations of urinary mixtures of phthalate and OH-PAH metabolites with semen quality. The overall effects of urinary mixtures of phthalate and PAH metabolites on semen quality were not statistically significant. However, hydroxynaphthalene (OHNa) factor identified from PCA was monotonically associated with decreased total sperm count and sperm concentration, whereas di(2-ethylhexyl) phthalate (DEHP) factor was non-monotonically related to increased progressive sperm motility and total sperm motility. Qg-comp and BKMR models confirmed these findings and identified 2-OHNa and 2-OHFlu as the primary negative contributors, whereas MEOHP and MEHP as the primary positive contributors. Our findings suggest that exposure to mixtures of naphthalene and DEHP is associated with altered semen quality. The finding is warranted to confirm in further well-designed epidemiological studies.


Similar content being viewed by others
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Al-Saleh I, Coskun S, Al-Doush I, Al-Rajudi T, Abduljabbar M, Al-Rouqi R, Palawan H, Al-Hassan S (2019) The relationships between urinary phthalate metabolites, reproductive hormones and semen parameters in men attending in vitro fertilization clinic. Sci Total Environ 658:982–995
Arzuaga X, Smith MT, Gibbons CF, Skakkebaek NE, Yost EE, Beverly B, Hotchkiss AK, Hauser R, Pagani RL, Schrader SM, Zeise L, Prins GS (2019) Proposed key characteristics of male reproductive toxicants as an approach for organizing and evaluating mechanistic evidence in human health hazard assessments. Environ Health Perspect 127(6):65001
Axelsson J, Rylander L, Rignell-Hydbom A, Jonsson BA, Lindh CH, Giwercman A (2015) Phthalate exposure and reproductive parameters in young men from the general Swedish population. Environ Int 85:54–60
Bhagat J, Nishimura N, Shimada Y (2021) Toxicological interactions of microplastics/nanoplastics and environmental contaminants: current knowledge and future perspectives. J Hazard Mater 405:123913
Bloom MS, Whitcomb BW, Chen Z, Ye A, Kannan K, Buck LG (2015) Associations between urinary phthalate concentrations and semen quality parameters in a general population. Hum Reprod 30(11):2645–2657
Bobb JF, Valeri L, Claus HB, Christiani DC, Wright RO, Mazumdar M, Godleski JJ, Coull BA (2015) Bayesian kernel machine regression for estimating the health effects of multi-pollutant mixtures. Biostatistics 16(3):493–508
Buck LG, Smarr MM, Sun L, Chen Z, Honda M, Wang W, Karthikraj R, Weck J, Kannan K (2018) Endocrine disrupting chemicals in seminal plasma and couple fecundity. Environ Res 163:64–70
Chang W, Wu M, Pan H, Guo P, Lee C (2017) Semen quality and insulin-like factor 3: associations with urinary and seminal levels of phthalate metabolites in adult males. Chemosphere 173:594–602
Chen Q, Garabrant DH, Hedgeman E, Little RJ, Elliott MR, Gillespie B, Hong B, Lee SY, Lepkowski JM, Franzblau A, Adriaens P, Demond AH, Patterson DG (2010) Estimation of background serum 2,3,7,8-TCDD concentrations by using quantile regression in the UMDES and NHANES populations. Epidemiology 21(Suppl 4):S51–S57
Chen X, An H, Ao L, Sun L, Liu W, Zhou Z, Wang Y, Cao J (2011) The combined toxicity of dibutyl phthalate and benzo(a)pyrene on the reproductive system of male Sprague Dawley rats in vivo. J Hazard Mater 186(1):835–841
Czarnota J, Gennings C, Wheeler DC (2015) Assessment of weighted quantile sum regression for modeling chemical mixtures and cancer risk. Cancer Inform 14(Suppl 2):159–171
Deng Y, Yan Z, Shen R, Huang Y, Ren H, Zhang Y (2021) Enhanced reproductive toxicities induced by phthalates contaminated microplastics in male mice (Mus musculus). J Hazard Mater 406:124644
Dutta S, Sengupta P, Muhamad S (2019) Male reproductive hormones and semen quality. Asian Pac J Reprod 8(5):189
Fix C, Jordan C, Cano P, Walker WH (2004) Testosterone activates mitogen-activated protein kinase and the cAMP response element binding protein transcription factor in Sertoli cells. Proc Natl Acad Sci U S A 101(30):10919–10924
Frederiksen H, Jensen TK, Jorgensen N, Kyhl HB, Husby S, Skakkebaek NE, Main KM, Juul A, Andersson AM (2014) Human urinary excretion of non-persistent environmental chemicals: an overview of Danish data collected between 2006 and 2012. Reproduction 147(4):555–565
Han X, Cui Z, Zhou N, Ma M, Li L, Li Y, Lin H, Ao L, Shu W, Liu J, Cao J (2014) Urinary phthalate metabolites and male reproductive function parameters in Chongqing general population. China Int J Hyg Environ Health 217(2–3):271–278
Hipwell AE, Kahn LG, Factor-Litvak P, Porucznik CA, Siegel EL, Fichorova RN, Hamman RF, Klein-Fedyshin M, Harley KG (2019) Exposure to non-persistent chemicals in consumer products and fecundability: a systematic review. Hum Reprod Update 25(1):51–71
Hou J, Yin W, Li P, Huang Y, Wan Y, Hu C, Xu T, Cheng J, Wang L, Yu Z, Yuan J (2019) Effect of exposure to phthalates on association of polycyclic aromatic hydrocarbons with 8-hydroxy-2′-deoxyguanosine. Sci Total Environ 691:378–392
Hou J, Yin W, Li P, Hu C, Xu T, Cheng J, Li T, Wang L, Yu Z, Yuan J (2020) Joint effect of polycyclic aromatic hydrocarbons and phthalates exposure on telomere length and lung function. J Hazard Mater 386:121663
Howdeshell KL, Rider CV, Wilson VS, Gray LJ (2008) Mechanisms of action of phthalate esters, individually and in combination, to induce abnormal reproductive development in male laboratory rats. Environ Res 108(2):168–176
Huang Q, Liu L, Wu Y, Wang X, Luo L, Nan B, Zhang J, Tian M, Shen H (2019) Seminal plasma metabolites mediate the associations of multiple environmental pollutants with semen quality in Chinese men. Environ Int 132:105066
Inyang F, Ramesh A, Kopsombut P, Niaz MS, Hood DB, Nyanda AM, Archibong AE (2003) Disruption of testicular steroidogenesis and epididymal function by inhaled benzo(a)pyrene. Reprod Toxicol 17(5):527–537
Joensen UN, Frederiksen H, Blomberg JM, Lauritsen MP, Olesen IA, Lassen TH, Andersson AM, Jorgensen N (2012) Phthalate excretion pattern and testicular function: a study of 881 healthy Danish men. Environ Health Perspect 120(10):1397–1403
Johnson KJ, Heger NE, Boekelheide K (2012) Of mice and men (and rats): phthalate-induced fetal testis endocrine disruption is species-dependent. Toxicol Sci 129(2):235–248
Jurewicz J, Radwan M, Sobala W, Ligocka D, Radwan P, Bochenek M, Hawula W, Jakubowski L, Hanke W (2013) Human urinary phthalate metabolites level and main semen parameters, sperm chromatin structure, sperm aneuploidy and reproductive hormones. Reprod Toxicol 42:232–241
Jurewicz J, Radwan M, Sobala W, Radwan P, Jakubowski L, Wielgomas B, Ligocka D, Brzeznicki S, Hanke W (2016) Exposure to widespread environmental endocrine disrupting chemicals and human sperm sex ratio. Environ Pollut 213:732–740
Keil AP, Buckley JP, O’Brien KM, Ferguson KK, Zhao S, White AJ (2020) A quantile-based g-computation approach to addressing the effects of exposure mixtures. Environ Health Perspect 128(4):47004
Keshavarzifard M, Moore F, Keshavarzi B, Sharifi R (2017) Polycyclic aromatic hydrocarbons (PAHs) in sediment and sea urchin (Echinometra mathaei) from the intertidal ecosystem of the northern Persian Gulf: Distribution, sources, and bioavailability. Mar Pollut Bull 123(1–2):373–380
Kranvogl R, Knez J, Miuc A, Voncina E, Voncina DB, Vlaisavljevic V (2014) Simultaneous determination of phthalates, their metabolites, alkylphenols and bisphenol A using GC-MS in urine of men with fertility problems. Acta Chim Slov 61(1):110–120
Laue HE, Moroishi Y, Jackson BP, Palys TJ, Madan JC, Karagas MR (2020) Nutrient-toxic element mixtures and the early postnatal gut microbiome in a United States longitudinal birth cohort. Environ Int 138:105613
Levine H, Jorgensen N, Martino-Andrade A, Mendiola J, Weksler-Derri D, Mindlis I, Pinotti R, Swan SH (2017) Temporal trends in sperm count: a systematic review and meta-regression analysis. Hum Reprod Update 23(6):646–659
Li Z, Romanoff LC, Lewin MD, Porter EN, Trinidad DA, Needham LL, Patterson DJ, Sjodin A (2010) Variability of urinary concentrations of polycyclic aromatic hydrocarbon metabolite in general population and comparison of spot, first-morning, and 24-h void sampling. J Expo Sci Environ Epidemiol 20(6):526–535
Liu L, Bao H, Liu F, Zhang J, Shen H (2012) Phthalates exposure of Chinese reproductive age couples and its effect on male semen quality, a primary study. Environ Int 42:78–83
Meek ME, Boobis AR, Crofton KM, Heinemeyer G, Raaij MV, Vickers C (2011) Risk assessment of combined exposure to multiple chemicals: a WHO/IPCS framework. Regul Toxicol Pharmacol 60(2):S1–S14
Meeker JD, Rossano MG, Protas B, Diamond MP, Puscheck E, Daly D, Paneth N, Wirth JJ (2008) Cadmium, lead, and other metals in relation to semen quality: human evidence for molybdenum as a male reproductive toxicant. Environ Health Perspect 116(11):1473–1479
Minguez-Alarcon L, Bellavia A, Gaskins AJ, Chavarro JE, Ford JB, Souter I, Calafat AM, Hauser R, Williams PL (2021) Paternal mixtures of urinary concentrations of phthalate metabolites, bisphenol A and parabens in relation to pregnancy outcomes among couples attending a fertility center. Environ Int 146:106171
Niehoff NM, Keil AP, O’Brien KM, Jackson BP, Karagas MR, Weinberg CR, White AJ (2020) Metals and trace elements in relation to body mass index in a prospective study of US women. Environ Res 184:109396
O’Rourke NHL (2013) A step-by-step approach to using SAS for factor analysis and structural equation modeling. Cary, NC: SAS Institute, Inc. 55(1):102–119
Ombelet W, Cooke I, Dyer S, Serour G, Devroey P (2008) Infertility and the provision of infertility medical services in developing countries. Hum Reprod Update 14(6):605–621
Oudir M, Chader H, Bouzid B, Bendisari K, Latreche B, Boudalia S, Iguer-Ouada M (2018) Male rat exposure to low dose of di(2-ethylhexyl) phthalate during pre-pubertal, pubertal and post-pubertal periods: impact on sperm count, gonad histology and testosterone secretion. Reprod Toxicol 75:33–39
Pallotti F, Pelloni M, Gianfrilli D, Lenzi A, Lombardo F, Paoli D (2020) Mechanisms of testicular disruption from exposure to bisphenol A and phtalates. J Clin Med 9(2):471
Pant N, Shukla M, Kumar Patel D, Shukla Y, Mathur N, Kumar Gupta Y, Saxena DK (2008) Correlation of phthalate exposures with semen quality. Toxicol Appl Pharmacol 231(1):112–116
Preau JJ, Wong LY, Silva MJ, Needham LL, Calafat AM (2010) Variability over 1 week in the urinary concentrations of metabolites of diethyl phthalate and di(2-ethylhexyl) phthalate among eight adults: an observational study. Environ Health Perspect 118(12):1748–1754
Puppel K, Kapusta A, Kuczynska B (2015) The etiology of oxidative stress in the various species of animals, a review. J Sci Food Agric 95(11):2179–2184
Radke EG, Braun JM, Meeker JD, Cooper GS (2018) Phthalate exposure and male reproductive outcomes: a systematic review of the human epidemiological evidence. Environ Int 121(Pt 1):764–793
Raychoudhury SS, Kubinski D (2003) Polycyclic aromatic hydrocarbon-induced cytotoxicity in cultured rat Sertoli cells involves differential apoptotic response. Environ Health Perspect 111(1):33–38
Sengupta P, Nwagha U, Dutta S, Krajewska-Kulak E, Izuka E (2017) Evidence for decreasing sperm count in African population from 1965 to 2015. Afr Health Sci 17(2):418–427
Sengupta P, Borges EJ, Dutta S, Krajewska-Kulak E (2018) Decline in sperm count in European men during the past 50 years. Hum Exp Toxicol 37(3):247–255
Shrier I, Platt RW (2008) Reducing bias through directed acyclic graphs. BMC Med Res Methodol 8:70
Sidorkiewicz I, Zareba K, Wolczynski S, Czerniecki J (2017) Endocrine-disrupting chemicals-mechanisms of action on male reproductive system. Toxicol Ind Health 33(7):601–609
Skakkebaek NE, Rajpert-De ME, Buck LG, Toppari J, Andersson AM, Eisenberg ML, Jensen TK, Jorgensen N, Swan SH, Sapra KJ, Ziebe S, Priskorn L, Juul A (2016) Male reproductive disorders and fertility trends: influences of environment and genetic susceptibility. Physiol Rev 96(1):55–97
Smits RM, Mackenzie-Proctor R, Fleischer K, Showell MG (2018) Antioxidants in fertility: Impact on male and female reproductive outcomes. Fertil Steril 110(4):578–580
Song XF, Chen ZY, Zang ZJ, Zhang YN, Zeng F, Peng YP, Yang C (2013) Investigation of polycyclic aromatic hydrocarbon level in blood and semen quality for residents in Pearl River Delta Region in China. Environ Int 60:97–105
Souter I, Bellavia A, Williams PL, Korevaar T, Meeker JD, Braun JM, de Poortere RA, Broeren MA, Ford JB, Calafat AM, Chavarro JE, Hauser R, Mínguez-Alarcón L (2020) Urinary concentrations of phthalate metabolite mixtures in relation to serum biomarkers of thyroid function and autoimmunity among women from a fertility center. Environ Health Perspect 128(6):67007
Vander BM, Wyns C (2018) Fertility and infertility: definition and epidemiology. Clin Biochem 62:2–10
Wang C, Swerdloff RS (2014) Limitations of semen analysis as a test of male fertility and anticipated needs from newer tests. Fertil Steril 102(6):1502–1507
Wang YX, You L, Zeng Q, Sun Y, Huang YH, Wang C, Wang P, Cao WC, Yang P, Li YF, Lu WQ (2015) Phthalate exposure and human semen quality: results from an infertility clinic in China. Environ Res 142:1–9
Wang YX, Zeng Q, Sun Y, Yang P, Wang P, Li J, Huang Z, You L, Huang YH, Wang C, Li YF, Lu WQ (2016) Semen phthalate metabolites, semen quality parameters and serum reproductive hormones: a cross-sectional study in China. Environ Pollut 211:173–182
White AJ, O Brien KM, Niehoff NM, Jackson BP, Karagas MR, Weinberg CR, Keil AP (2020) Toenail metal concentrations and age at menopause. Environ Epidemiol 4(4):e0104
WHO (2010) Who Laboratory Manual for the Examination and Processing of Human semen. 5th ed. Available: http://whqlibdoc.who.Int/publications/2010/9789241547789_eng.Pdf (accessed 11.05.14). 12(1):59–63
Xia Y, Han Y, Zhu P, Wang S, Gu A, Wang L, Lu C, Fu G, Song L, Wang X (2009) Relation between urinary metabolites of polycyclic aromatic hydrocarbons and human semen quality. Environ Sci Technol 43(12):4567–4573
Xia Y, Zhu P, Han Y, Lu C, Wang S, Gu A, Fu G, Zhao R, Song L, Wang X (2009) Urinary metabolites of polycyclic aromatic hydrocarbons in relation to idiopathic male infertility. Hum Reprod 24(5):1067–1074
Yang P, Wang Y, Sun L, Chen Y, Liu C, Huang L, Lu W, Zeng Q (2017) Urinary metabolites of polycyclic aromatic hydrocarbons, sperm DNA damage and spermatozoa apoptosis. J Hazard Mater 329:241–248
Yang P, Wang YX, Chen YJ, Sun L, Li J, Liu C, Huang Z, Lu WQ, Zeng Q (2017) Urinary polycyclic aromatic hydrocarbon metabolites and human semen quality in China. Environ Sci Technol 51(2):958–967
Zamkowska D, Karwacka A, Jurewicz J, Radwan M (2018) Environmental exposure to non-persistent endocrine disrupting chemicals and semen quality: an overview of the current epidemiological evidence. Int J Occup Med Environ Health 31(4):377–414
Zhang J, Yang JC, Wang RQ, Hou H, Du XM, Fan SK, Liu JS, Dai JL (2013) Effects of pollution sources and soil properties on distribution of polycyclic aromatic hydrocarbons and risk assessment. Sci Total Environ 463–464:1–10
Zhao Z, Gong X, Zhang L, Jin M, Cai Y, Wang X (2021) Riverine transport and water-sediment exchange of polycyclic aromatic hydrocarbons (PAHs) along the middle-lower Yangtze River. China J Hazard Mater 403:123973
Zheng SJ, Tian HJ, Cao J, Gao YQ (2010) Exposure to di(n-butyl)phthalate and benzo(a)pyrene alters IL-1beta secretion and subset expression of testicular macrophages, resulting in decreased testosterone production in rats. Toxicol Appl Pharmacol 248(1):28–37
Funding
This study was supported by the National Key Research and Development Plan of China (No. 2018YFC1004201) and the National Natural Science Foundation of China (No. 81872585).
Author information
Authors and Affiliations
Contributions
Yan-Ling Deng: conceptualization, formal analysis, methodology, software, visualization, data curation, writing—original draft, writing—review and editing. Pan Yang: methodology, supervision, writing—review and editing. Yi-Xin Wang: investigation, methodology, supervision, writing—review and editing; Chong Liu: supervision, writing—review and editing. Qiong Luo: investigation. Tian Shi: investigation. Jia-Yue Zeng: investigation. Ting-Ting Lu: investigation. Pan-Pan Chen: investigation. Yu Miao: investigation. Min Zhang: investigation. Fei-Peng Cui: investigation. Wen-Qing Lu: supervision, funding acquisition, resources. Qiang Zeng: project administration, conceptualization, methodology, supervision, writing—review and editing, funding acquisition.
Corresponding author
Ethics declarations
Ethical approval
The protocol was approved by The Ethics Committee of Tongji Medical College (number 2019/S004).
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Responsible Editor: Lotfi Aleya
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Deng, YL., Yang, P., Wang, YX. et al. Urinary concentrations of polycyclic aromatic hydrocarbon and phthalate metabolite mixtures in relation to semen quality among men attending an infertility clinic. Environ Sci Pollut Res 29, 81749–81759 (2022). https://doi.org/10.1007/s11356-022-21525-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-022-21525-y