Abstract
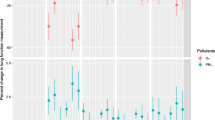
The occurrences of impaired lung function during childhood could substantially influence the health states of the respiratory system in adults. So, the effects of air pollution and green spaces on impaired lung function in children were investigated in this study. The lung function of each student was tested every year from 2015 to 2017 and the method of case-control study was applied. 2087 students aged from 9 to 11 years old of primary schools in Tianjin were ultimately included in this study. The method of propensity score matching (PSM) was performed to minimize the confounding bias and the conditional logistic regression model was carried out to evaluate the effects of indoor and outdoor environmental risk factors on the occurrences of impaired lung function in children. For every interquartile range (IQR) increase in the mixture of six air pollutants at the lag1, lag2, and lag3 periods, the risks of getting impaired lung function were increased by 53.4%, 34.7%, and 16.9%, respectively. The protective effect of greenness at lag2 period (odds ratios (OR)) = 0.022 (95% confidence interval (CI): 0.008–0.035)) was stronger than that at lag1and lag3 periods, respectively. Separate and combined effects of most air pollutants at different lag periods exerted hazardous effects on the lung function of students. Exposure to greenness had protective effects on the lung health of children.
Graphical abstract





Similar content being viewed by others
References
American Thoracic Society (1991) Lung function testing: selection of reference values and interpretative strategies. Am Rev Respir Dis 144:1202–1218. https://doi.org/10.1164/ajrccm/144.5.1202
Barbone F, Catelan D, Pistelli R, Accetta G, Grechi D, Rusconi F, Biggeri A (2019) A panel study on lung function and bronchial inflammation among children exposed to ambient SO2 from an oil refinery. Int J Environ Res Public Health 16:1057. https://doi.org/10.3390/ijerph16061057
Buccolieri R, Gromke C, Di Sabatino S, Ruck B (2009) Aerodynamic effects of trees on pollutant concentration in street canyons. Sci Total Environ 407:5247–5256. https://doi.org/10.1016/j.scitotenv.2009.06.016
Chao X, Yi L, Lan LL, Wei HY, Wei D (2020) Long-term PM(2.5) exposure increases the risk of non-small cell lung cancer (NSCLC) progression by enhancing interleukin-17a (IL-17a)-regulated proliferation and metastasis. Aging (Albany NY) 12:11579–11602. https://doi.org/10.18632/aging.103319
Chen N, Shi J, Huang J, Yu W, Liu R, Gu L, Yang R, Yu Z, Liu Q, Yang Y, Cui S, Wang Z (2020) Impact of air pollutants on pediatric admissions for Mycoplasma pneumonia: a cross-sectional study in Shanghai, China. BMC Public Health 20:447. https://doi.org/10.1186/s12889-020-8423-4
Dadvand P, Tischer C, Estarlich M, Llop S, Dalmau-Bueno A, López-Vicente M, Valentín A, de Keijzer C, Fernández-Somoano A, Lertxundi N, Rodriguez-Dehli C, Gascon M, Guxens M, Zugna D, Basagaña X, Nieuwenhuijsen MJ, Ibarluzea J, Ballester F, Sunyer J (2017) Lifelong residential exposure to green space and attention: a population-based prospective study. Environ Health Perspect 125:097016. https://doi.org/10.1289/ehp694
Dauchet L, Hulo S, Cherot-Kornobis N, Matran R, Amouyel P, Edmé JL, Giovannelli J (2018) Short-term exposure to air pollution: associations with lung function and inflammatory markers in non-smoking, healthy adults. Environ Int 121:610–619. https://doi.org/10.1016/j.envint.2018.09.036
Doiron D, de Hoogh K, Probst-Hensch N, Fortier I, Cai Y, De Matteis S, Hansell AL (2019) Air pollution, lung function and COPD: results from the population-based UK biobank study. Eur Respir J 54:1802140. https://doi.org/10.1183/13993003.02140-2018
Fuertes E, Markevych I, Thomas R, Boyd A, Granell R, Mahmoud O, Heinrich J, Garcia-Aymerich J, Roda C, Henderson J, Jarvis D (2020) Residential greenspace and lung function up to 24 years of age: the ALSPAC birth cohort. Environ Int 140:105749. https://doi.org/10.1016/j.envint.2020.105749
Gromke C, Ruck B (2007) Influence of trees on the dispersion of pollutants in an urban street canyon-experimental investigation of the flow and concentration field. Atmospheric Environ 41:3287–3302
Guo C, Hoek G, Chang LY, Bo Y, Lin C, Huang B, Chan TC, Tam T, Lau AKH, Lao XQ (2019) Long-term exposure to ambient fine particulate matter (PM2.5) and lung function in children, adolescents, and young adults: a longitudinal cohort study. Environ Health Perspect 127:127008. https://doi.org/10.1289/ehp5220
Joelsson JP, Kricker JA, Arason AJ, Sigurdsson S, Valdimarsdottir B, Gardarsson FR, Page CP, Lehmann F, Gudjonsson T, Ingthorsson S (2020) Azithromycin ameliorates sulfur dioxide-induced airway epithelial damage and inflammatory responses. Respir Res 21:233. https://doi.org/10.1186/s12931-020-01489-8
King KL, Johnson S, Kheirbek I, Lu JWT, Matte T (2014) Differences in magnitude and spatial distribution of urban forest pollution deposition rates, air pollution emissions, and ambient neighborhood air quality in New York City. Landsc Urban Plan 128:14–22. https://doi.org/10.1016/j.landurbplan.2014.04.009
Laborde A, Tomasina F, Bianchi F, Bruné M, Buka I, Comba P, Corra L, Cori L, Duffert CM, Harari RJEHP (2015) Children's health in Latin America: the influence of environmental exposures. Environ Health Perspect 123:201–209. https://doi.org/10.1289/ehp.1408292
Lee YS, Min D, Park SY, Lee J, Bae H (2020) Standardized herbal extract PM014 alleviates fine dust-induced lung inflammation in mice. BMC Complement Med Ther 20:270. https://doi.org/10.1186/s12906-020-03060-w
Lo VE, Chiu YC, Tu HH, Liu CW, Yu CY (2019) A pilot study of five types of maximum hand strength among manufacturing industry workers in Taiwan. Int J Environ Res Public Health 16:4742. https://doi.org/10.3390/ijerph16234742
Lovinsky-Desir S, Jung KH, Jezioro JR, Torrone DZ, de Planell-Saguer M, Yan B, Perera FP, Rundle AG, Perzanowski MS, Chillrud SN, Miller RL (2017) Physical activity, black carbon exposure, and DNA methylation in the FOXP3 promoter. Clin Epigenetics 9:65. https://doi.org/10.1186/s13148-017-0364-0
Markevych I, Schoierer J, Hartig T, Chudnovsky A, Hystad P, Dzhambov AM, de Vries S, Triguero-Mas M, Brauer M, Nieuwenhuijsen MJ, Lupp G, Richardson EA, Astell-Burt T, Dimitrova D, Feng X, Sadeh M, Standl M, Heinrich J, Fuertes E (2017) Exploring pathways linking greenspace to health: theoretical and methodological guidance. Environ Res 158:301–317. https://doi.org/10.1016/j.envres.2017.06.028
Miller MR, Hankinson J, Brusasco V, Burgos F, Casaburi R, Coates A, Crapo R, Enright P, van der Grinten CP, Gustafsson P, Jensen R, Johnson DC, MacIntyre N, McKay R, Navajas D, Pedersen OF, Pellegrino R, Viegi G, Wanger J (2005) Standardisation of spirometry. Eur Respir J 26:319–338. https://doi.org/10.1183/09031936.05.00034805
Nordeide Kuiper I, Svanes C, Markevych I, Accordini S, Bertelsen RJ, Bråbäck L, Heile Christensen J, Forsberg B, Halvorsen T, Heinrich J, Hertel O, Hoek G, Holm M, de Hoogh K, Janson C, Malinovschi A, Marcon A, Miodini Nilsen R, Sigsgaard T, Johannessen A (2021) Lifelong exposure to air pollution and greenness in relation to asthma, rhinitis and lung function in adulthood. Environ Int 146:106219. https://doi.org/10.1016/j.envint.2020.106219
Oerlemans AM, Wardenaar KJ, Raven D, Hartman CA, Ormel J (2020) The association of developmental trajectories of adolescent mental health with early-adult functioning. PLoS One 15:e0233648. https://doi.org/10.1371/journal.pone.0233648
Paciência I, Moreira A (2017) Human health: is it who you are or where you live? Lancet Planet Health 1:e263–e264. https://doi.org/10.1016/s2542-5196(17)30123-7
Quanjer PH, Stanojevic S, Cole TJ, Baur X, Hall GL, Culver BH, Enright PL, Hankinson JL, Ip MS, Zheng J, Stocks J (2012) Multi-ethnic reference values for spirometry for the 3-95-yr age range: the global lung function 2012 equations. Eur Respir J 40:1324–1343. https://doi.org/10.1183/09031936.00080312
Reiner RC Jr, Olsen HE, Ikeda CT et al (2019) Diseases, injuries, and risk factors in child and adolescent health, 1990 to 2017: findings from the Global Burden of Diseases, Injuries, and Risk Factors 2017 Study. JAMA Pediatr 173:e190337. https://doi.org/10.1001/jamapediatrics.2019.0337
Sly PD, Flack F (2008) Susceptibility of children to environmental pollutants. Ann N Y Acad Sci 1140:163–183. https://doi.org/10.1196/annals.1454.017
Terzaghi E, Wild E, Zacchello G, Cerabolini BEL, Jones KC, Di Guardo A (2013) Forest Filter Effect: Role of leaves in capturing/releasing air particulate matter and its associated PAHs. Atmospheric Environ 74:378–384. https://doi.org/10.1016/j.atmosenv.2013.04.013
Wang M, Aaron CP, Madrigano J, Hoffman EA, Angelini E, Yang J, Laine A, Vetterli TM, Kinney PL, Sampson PD, Sheppard LE, Szpiro AA, Adar SD, Kirwa K, Smith B, Lederer DJ, Diez-Roux AV, Vedal S, Kaufman JD, Barr RG (2019) Association between long-term exposure to ambient air pollution and change in quantitatively assessed emphysema and lung function. JAMA 322:546–556. https://doi.org/10.1001/jama.2019.10255
Wong SF, Yap PS, Mak JW, Chan WLE, Khor GL, Ambu S, Chu WL, Mohamad MS, Ibrahim Wong N, Ab Majid NL, Abd Hamid HA, Rodzlan Hasani WS, Mohd Yussoff MFB, Aris HTB, Ab Rahman EB, M Rashid ZB (2020) Association between long-term exposure to ambient air pollution and prevalence of diabetes mellitus among Malaysian adults. Environ Health 19:37. https://doi.org/10.1186/s12940-020-00579-w
Wu D, Meng Z (2003) Effect of sulfur dioxide inhalation on the glutathione redox system in mice and protective role of sea buckthorn seed oil. Arch Environ Contam Toxicol 45:423–428. https://doi.org/10.1007/s00244-003-2157-z
Wu QZ, Li S, Yang BY, Bloom M, Shi Z, Knibbs L, Dharmage S, Leskinen A, Jalaludin B, Jalava P, Roponen M, Lin S, Chen G, Guo Y, Xu SL, Yu HY, Zeeshan M, Hu LW, Yu Y et al (2020) Ambient airborne particulates of diameter ≤1 μm, a leading contributor to the association between ambient airborne particulates of diameter ≤2.5 μm and children's blood pressure. Hypertension 75:347–355. https://doi.org/10.1161/hypertensionaha.119.13504
Xing X, Hu L, Guo Y, Bloom MS, Li S, Chen G, Yim SHL, Gurram N, Yang M, Xiao X, Xu S, Wei Q, Yu H, Yang B, Zeng X, Chen W, Hu Q, Dong G (2020) Interactions between ambient air pollution and obesity on lung function in children: The Seven Northeastern Chinese Cities (SNEC) Study. Sci Total Environ 699:134397. https://doi.org/10.1016/j.scitotenv.2019.134397
Yang HB, Teng CG, Hu J, Zhu XY, Wang Y, Wu JZ, Xiao Q, Yang W, Shen H, Liu F (2019) Short-term effects of ambient particulate matter on blood pressure among children and adolescents: a cross-sectional study in a city of Yangtze River delta, China. Chemosphere 237:124510. https://doi.org/10.1016/j.chemosphere.2019.124510
Yu Y, Yu Z, Sun P, Lin B, Li L, Wang Z, Ma R, Xiang M, Li H, Guo S (2018) Effects of ambient air pollution from municipal solid waste landfill on children's non-specific immunity and respiratory health. Environ Pollut 236:382–390. https://doi.org/10.1016/j.envpol.2017.12.094
Yu F, Ye K, Hu Y, Li J, An Y, Qu D (2019) Exposure to polycyclic aromatic hydrocarbons derived from vehicle exhaust gas induces premature senescence in mouse lung fibroblast cells. Mol Med Rep 19:4326–4334. https://doi.org/10.3892/mmr.2019.10086
Yuchi W, Sbihi H, Davies H, Tamburic L, Brauer M (2020) Road proximity, air pollution, noise, green space and neurologic disease incidence: a population-based cohort study. Environ Health 19:8. https://doi.org/10.1186/s12940-020-0565-4
Zeka A, Sullivan JR, Vokonas PS, Sparrow D, Schwartz J (2006) Inflammatory markers and particulate air pollution: characterizing the pathway to disease. Int J Epidemiol 35:1347–1354. https://doi.org/10.1093/ije/dyl132
Zhang C, Guo Y, Xiao X, Bloom MS, Qian Z, Rolling CA, Xian H, Lin S, Li S, Chen G, Jalava P, Roponen M, Hirvonen MR, Komppula M, Leskinen A, Yim SHL, Chen DH, Ma H, Zeng XW et al (2019a) Association of breastfeeding and air pollution exposure with lung function in chinese children. JAMA Netw Open 2:e194186. https://doi.org/10.1001/jamanetworkopen.2019.4186
Zhang H, Pang Q, Long H, Zhu H, Gao X, Li X, Jiang X, Liu K (2019b) Local residents' perceptions for ecosystem services: a case study of fenghe river watershed. Int J Environ Res Public Health 16:3602. https://doi.org/10.3390/ijerph16193602
Zhang J, Feng L, Hou C, Gu Q (2020) How the constituents of fine particulate matter and ozone affect the lung function of children in Tianjin, China. Environ Geochem Health 42:3303–3316. https://doi.org/10.1007/s10653-020-00574-7
Zhu L, Ge X, Chen Y, Zeng X, Pan W, Zhang X, Ben S, Yuan Q, Xin J, Shao W, Ge Y, Wu D, Han Z, Zhang Z, Chu H, Wang M (2017) Short-term effects of ambient air pollution and childhood lower respiratory diseases. Sci Rep 7:4414. https://doi.org/10.1038/s41598-017-04310-7
Acknowledgements
We would also like to thank the language editing service provided by Xiaoyu Chen (Monash University, Australia).
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Author information
Authors and Affiliations
Contributions
Jingwei Zhang: conceptualization, methodology, software, and writing-original draft preparation; Yuming Wang: data curation; Lihong Feng: visualization and investigation; Changchun Hou: Supervision and software; Qing Gu: validation, writing-reviewing and editing.
Corresponding author
Ethics declarations
Ethics approval
We have verified consent from subjects participating in the study was received prior to conducting the study and provided written assurance that the study has been reviewed and approved by an accredited committee. The study was approved by the Committee on the Ethics of Tianjin Centers for Disease Control and Prevention (permit number: TJCDC0111).
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Responsible Editor: Lotfi Aleya
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhang, J., Wang, Y., Feng, L. et al. Effects of air pollution and green spaces on impaired lung function in children: a case-control study. Environ Sci Pollut Res 29, 11907–11919 (2022). https://doi.org/10.1007/s11356-021-16554-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-021-16554-y