Abstract
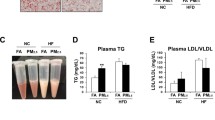
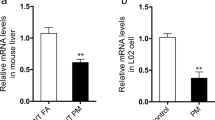
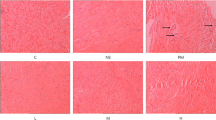
Both the epidemiological and animal experimental studies have reported the association between PM2.5 and respiratory, cardiovascular, and metabolic diseases. However, the study linking PM2.5 and hepatic injury is few, and the relative mechanism has not been fully elucidated. Thirty-two 6-week-old male C57BL/6 mice were exposed to filtered air (FA) or concentrated PM2.5 for 12 weeks using Shanghai Meteorological and Environmental Animal Exposure System (“Shanghai-METAS”), respectively. At week 11, the mice began to be treated with intraperitoneal injection of normal 0.9% saline or AMPK activator (AICAR). The mRNA levels of IL-6 and TNF-α, and protein expressions of AMPK, GLUT4, NF-κB, p38MAPK, ERK, and JNK in the liver and UCP-1 in brown adipose tissue (BAT) were measured. Meanwhile, histopathological examination both in the liver and BAT was performed to evaluate the histopathological changes. PM2.5 exposure induced steatosis, hepatocyte ballooning, lobular and portal inflammation in the liver, and the brown adipocyte swelling in BAT. The results found that PM mice displayed higher IL-6, TNF-α, NF-κB, and JNK expression and lower AMPK, GLUT4, and UCP-1 when compared with FA mice. The AICAR injection upregulated the expressions of GLUT4 in the liver of PM-AIC mice when compared with the PM mice. However, there were no significant effects of AICAR on histopathological condition. The current study showed that ambient PM2.5 exposure might induce the hepatic injury along with the lipid metabolism disorder in BAT. AMPK activation can ameliorate most of the harmful effects and might become the potential target for treating PM2.5-induced hepatic injury.





Similar content being viewed by others
References
Collaborators GBDRF (2018) Global, regional, and national comparative risk assessment of 84 behavioural, environmental and occupational, and metabolic risks or clusters of risks for 195 countries and territories, 1990-2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 392:1923–1994
Coulthard LR, White DE, Jones DL, McDermott MF, Burchill SA (2009) p38(MAPK): stress responses from molecular mechanisms to therapeutics. Trends Mol Med 15:369–379
Crane JD, Palanivel R, Mottillo EP, Bujak AL, Wang H, Ford RJ, Collins A, Blumer RM, Fullerton MD, Yabut JM, Kim JJ, Ghia JE, Hamza SM, Morrison KM, Schertzer JD, Dyck JR, Khan WI, Steinberg GR (2015) Inhibiting peripheral serotonin synthesis reduces obesity and metabolic dysfunction by promoting brown adipose tissue thermogenesis. Nat Med 21:166–172
Deng H, Eckel SP, Liu L, Lurmann FW, Cockburn MG, Gilliland FD (2017) Particulate matter air pollution and liver cancer survival. Int J Cancer 141:744–749
Du XH, Jiang S, Zeng XJ, Zhang J, Pan K, Zhou J, Xie YQ, Kan HD, Song WM, Sun QH, Zhao JZ (2018) Air pollution is associated with the development of atherosclerosis via the cooperation of CD36 and NLRP3 inflammasome in ApoE(−/−) mice. Toxicol Lett 290:123–132
Haberzettl P, O’Toole TE, Bhatnagar A, Conklin DJ (2016) Exposure to fine particulate air pollution causes vascular insulin resistance by inducing pulmonary oxidative stress. Environ Health Perspect 124:1830–1839
Hu X, Zhao Y, He X, Li J, Wang T, Zhou W, Wan D, Wang H, Gu J (2008) Ciliary neurotrophic factor receptor alpha subunit-modulated multiple downstream signaling pathways in hepatic cancer cell lines and their biological implications. Hepatology 47:1298–1308
Iglesias MA, Ye JM, Frangioudakis G, Saha AK, Tomas E, Ruderman NB, Cooney GJ, Kraegen EW (2002) AICAR administration causes an apparent enhancement of muscle and liver insulin action in insulin-resistant high-fat-fed rats. Diabetes 51:2886–2894
Jian T, Ding X, Wu Y, Ren B, Li W, Lv H, Chen J (2018) Hepatoprotective effect of loquat leaf flavonoids in PM2.5-induced non-alcoholic fatty liver disease via regulation of IRs-1/Akt and CYP2E1/JNK pathways. Int J Mol Sci 19:E3005
Jiang Z, Zhou J, Zhou D, Zhu Z, Sun L, Nanji AA (2015) The adiponectin-SIRT1-AMPK pathway in alcoholic fatty liver disease in the rat. Alcohol Clin Exp Res 39:424–433
Kang OH, Shon MY, Kong R, Seo YS, Zhou T, Kim DY, Kim YS, Kwon DY (2017) Anti-diabetic effect of black ginseng extract by augmentation of AMPK protein activity and upregulation of GLUT2 and GLUT4 expression in db/db mice. BMC Complement Altern Med 17:341
Kleiner DE, Brunt EM, Van Natta M, Behling C, Contos MJ, Cummings OW, Ferrell LD, Liu YC, Torbenson MS, Unalp-Arida A, Yeh M, McCullough AJ, Sanyal AJ, Nonalcoholic Steatohepatitis Clinical Research N (2005) Design and validation of a histological scoring system for nonalcoholic fatty liver disease. Hepatology 41:1313–1321
Lidell ME, Betz MJ, Enerback S (2014) Brown adipose tissue and its therapeutic potential. J Intern Med 276:364–377
Liu C, Bai Y, Xu X, Sun L, Wang A, Wang TY, Maurya SK, Periasamy M, Morishita M, Harkema J, Ying Z, Sun Q, Rajagopalan S (2014a) Exaggerated effects of particulate matter air pollution in genetic type II diabetes mellitus. Part Fibre Toxicol 11:27
Liu C, Xu X, Bai Y, Wang TY, Rao X, Wang A, Sun L, Ying Z, Gushchina L, Maiseyeu A, Morishita M, Sun Q, Harkema JR, Rajagopalan S (2014b) Air pollution-mediated susceptibility to inflammation and insulin resistance: influence of CCR2 pathways in mice. Environ Health Perspect 122:17–26
Mottillo EP, Desjardins EM, Crane JD, Smith BK, Green AE, Ducommun S, Henriksen TI, Rebalka IA, Razi A, Sakamoto K, Scheele C, Kemp BE, Hawke TJ, Ortega J, Granneman JG, Steinberg GR (2016) Lack of adipocyte AMPK exacerbates insulin resistance and hepatic steatosis through brown and beige adipose tissue function. Cell Metab 24:118–129
Pan K, Jiang S, Du X, Zeng X, Zhang J, Song L, Zhou J, Kan H, Sun Q, Xie Y, Zhao J (2019) AMPK activation attenuates inflammatory response to reduce ambient PM2.5-induced metabolic disorders in healthy and diabetic mice. Ecotoxicol Environ Saf 179:290–300
Pedersen M, Andersen ZJ, Stafoggia M, Weinmayr G, Galassi C, Sørensen M, Eriksen KT, Tjønneland A, Loft S, Jaensch A, Nagel G, Concin H, Tsai MY, Grioni S, Marcon A, Krogh V, Ricceri F, Sacerdote C, Ranzi A, Sokhi R, Vermeulen R, Hoogh K, Wang M, Beelen R, Vineis P, Brunekreef B, Hoek G, Raaschou-Nielsen O (2017) Ambient air pollution and primary liver cancer incidence in four European cohorts within the ESCAPE project. Environ Res 154:226–233
Shimizu I, Aprahamian T, Kikuchi R, Shimizu A, Papanicolaou KN, MacLauchlan S, Maruyama S, Walsh K (2014) Vascular rarefaction mediates whitening of brown fat in obesity. J Clin Invest 124:2099–2112
Sun L, Liu C, Xu X, Ying Z, Maiseyeu A, Wang A, Allen K, Lewandowski RP, Bramble LA, Morishita M, Wagner JG, Dvonch J, Sun Z, Yan X, Brook RD, Rajagopalan S, Harkema JR, Sun Q, Fan Z (2013) Ambient fine particulate matter and ozone exposures induce inflammation in epicardial and perirenal adipose tissues in rats fed a high fructose diet. Part Fibre Toxicol 10:43
Sun Q, Wang A, Jin X, Natanzon A, Duquaine D, Brook RD, Aguinaldo JG, Fayad ZA, Fuster V, Lippmann M, Chen LC, Rajagopalan S (2005) Long-term air pollution exposure and acceleration of atherosclerosis and vascular inflammation in an animal model. Jama 294:3003–3010
Sun Q, Yue P, Deiuliis JA, Lumeng CN, Kampfrath T, Mikolaj MB, Cai Y, Ostrowski MC, Lu B, Parthasarathy S, Brook RD, Moffatt-Bruce SD, Chen LC, Rajagopalan S (2009) Ambient air pollution exaggerates adipose inflammation and insulin resistance in a mouse model of diet-induced obesity. Circulation 119:538–546
van Dam AD, Kooijman S, Schilperoort M, Rensen PCN, Boon MR (2015) Regulation of brown fat by AMP-activated protein kinase. Trends Mol Med 21:571–579
Xu X, Liu C, Xu Z, Tzan K, Zhong M, Wang A, Lippmann M, Chen LC, Rajagopalan S, Sun Q (2011) Long-term exposure to ambient fine particulate pollution induces insulin resistance and mitochondrial alteration in adipose tissue. Toxicol Sci : an official journal of the Society of Toxicology 124:88–98
Yang G, Wang Y, Zeng Y, Gao GF, Liang X, Zhou M, Wan X, Yu S, Jiang Y, Naghavi M, Vos T, Wang H, Lopez AD, Murray CJ (2013) Rapid health transition in China, 1990-2010: findings from the Global Burden of Disease Study 2010. Lancet 381:1987–2015
Yuan H, Shyy JY, Martins-Green M (2009) Second-hand smoke stimulates lipid accumulation in the liver by modulating AMPK and SREBP-1. J Hepatol 51:535–547
Zheng Z, Xu X, Zhang X, Wang A, Zhang C, Huttemann M, Grossman LI, Chen LC, Rajagopalan S, Sun Q, Zhang K (2013) Exposure to ambient particulate matter induces a NASH-like phenotype and impairs hepatic glucose metabolism in an animal model. J Hepatol 58:148–154
Zheng Z, Zhang X, Wang J, Dandekar A, Kim H, Qiu Y, Xu X, Cui Y, Wang A, Chen LC, Rajagopalan S, Sun Q, Zhang K (2015) Exposure to fine airborne particulate matters induces hepatic fibrosis in murine models. J Hepatol 63:1397–1404
Funding
This study was financially supported by the National Key Research and Development Program of China (2017YFC0211602) and the National Natural Science Foundation of China (No. 81673125 and 91543119).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Responsible editor: Philippe Garrigues
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 49 kb)
Rights and permissions
About this article
Cite this article
Song, L., Jiang, S., Pan, K. et al. AMPK activation ameliorates fine particulate matter-induced hepatic injury. Environ Sci Pollut Res 27, 21311–21319 (2020). https://doi.org/10.1007/s11356-020-08624-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-020-08624-4