Abstract
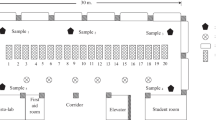
This study used a formaldehyde detector tube with a gas-piston hand pump to assess ceiling levels of student breathing zone and gross laboratory environment across the 2018 academic year. The room dimension was 28.6 × 55.48 × 5.5 m. It contained 90 cadavers, each placed on a hinged cover table. We measured before and during nine body region dissections. There was a significant difference (p < 0.01) between student exposure and laboratory environment levels. The highest level was student exposure during body wall dissection (2.7 ppm), the first laboratory; students may accidentally enter body cavities. The latter two were in abdominal (1.85 ppm) and lower limb dissections (1.49 ppm). The three highest environment levels were in different regions; spinal cord removal (1.13 ppm), lower limb (0.72 ppm), and thorax (0.71 ppm) dissection. Only the perineum environment level (0.09 ppm) was below the NIOSH ceiling level (0.1 ppm), which may result from the table covers that had been opened for 2 weeks before measurement. This study finding signified the importance of student personal exposure monitoring and encouraged the academic year measurement. Because each laboratory has unique factors, those affect formaldehyde levels; dissection steps, dissection table design, cadaver storage protocol, and heating-ventilation-air conditioning system performance, for instance.



Similar content being viewed by others
References
Azari MR, Asadi P, Jafari MJ, Soori H, Hosseini V (2012) Occupational exposure of a medical school staff to formaldehyde in Tehran. Tanaffos 11:36–41
Azuma M, Endo Y, Miyazaki T, Hikita Y, Ikeda H, Moriya Y, Hara I, Araki S (2003) Efficacy of a detector tube method in formaldehyde measurement. Ind Health 41:306–312
Durongphan (2019) A pilot study of measures enhancing local ventilation system to decrease formaldehyde level at Siriraj’s gross laboratory. Siriraj Med J 71:S33–S38
Hendricks W (1989) Acrolein and/or formaldehyde. Occupational Safety and Health Administration. www.osha.gov/dts/sltc/methods/organic/org052/org052.html. Accessed 24 July 2019
Hundy GF, Trott AR, Welch TC (2016) Refrigeration, air conditioning and heat pumps. Chapter 24 - Air Conditioning Methods and Applications. Butterworth-Heinemann
Kaden DA, Mandin C, Nielsen GD et al (2010) Formaldehyde, WHO guidelines for indoor air quality: selected pollutants. WHO Guidelines Approved by the Guidelines Review Committee, Geneva
Ku JC (1990) Formaldehyde in workplace atmospheres (3M model 3721 monitor). Occupational Safety and Health Administration wwwoshagov/dts/sltc/methods/inorganic/id205/id205html Accessed July 30
Kunugita N, Nakashima T, Kikuta A, Kawamoto T, Arashidani K (2004) Exposure to formaldehyde during an anatomy dissecting course. J UOEH 26:337–348
Lakchayapakorn K (2010) Formaldehyde exposure of medical students and instructors and clinical symptoms during gross anatomy laboratory in Thammasat University. J Med Assoc Thai 93(Suppl 7):S92–S98
MOI (1977) Notification of the Ministry of Internal Affairs No. 103, B.E. 2520. Re: Chemical standard values in establishment. . Government Gazette Ministry of Interior of the Kingdom of Thailand
Naoki S (2006) Levels of formaldehyde, phenol and ethanol in dissection room air and measures for reduction. Jpn J Occup Med Traumatol 54:1–10
NIOSH (2018) Formaldehyde. Centers for Disease Control and Prevention. https://www.cdc.gov/niosh/npg/npgd0293.html. Accessed 24 July 2019
Ohmichi K, Komiyama M, Matsuno Y, Takanashi Y, Miyamoto H, Kadota T, Maekawa M, Toyama Y, Tatsugi Y, Kohno T, Ohmichi M, Mori C (2006) Formaldehyde exposure in a gross anatomy laboratory--personal exposure level is higher than indoor concentration. Environ Sci Pollut Res Int 13:120–124
OSHA (2011) Formaldehyde fact sheet. Occupational Safety and Health Administration USA
OSHA (2013) Substance technical guidelines for formalin. Occupational Safety and Health Standards. www.osha.gov/pls/oshaweb/owadisp.show_document?p_table=STANDARDS&p_id=10076. Accessed 24 July 2019
OSHA (2014) OSHA technical Manualhttps://www.osha.gov/dts/osta/otm/otm_ii/otm_ii_1.html. Accessed 24 July 2019
OSHA (2018) FORMALIN (as FORMALDEHYDE)https://www.osha.gov/chemicaldata/chemResult.html?RecNo=378. Accessed 24 July 2019
Saowakon N, Ngernsoungnern P, Watcharavitoon P, Ngernsoungnern A, Kosanlavit R (2015) Formaldehyde exposure in gross anatomy laboratory of Suranaree University of Technology: a comparison of area and personal sampling. Environ Sci Pollut Res Int 22:19002–19012
SAVER (2014) Portable colorimetric tubes for chemical vapor detection market survey report. In: (DHS) DoHS (Hrsg.). System Assessment and Validation for Emergency Responders (SAVER)
Sugata Y, Miyaso H, Odaka Y, Komiyama M, Sakamoto N, Mori C, Matsuno Y (2016) Levels of formaldehyde vapor released from embalmed cadavers in each dissection stage. Environ Sci Pollut Res Int 23:16176–16182
Takahashi S, Tsuji K, Fujii K, Okazaki F, Takigawa T, Ohtsuka A, Iwatsuki K (2007) Prospective study of clinical symptoms and skin test reactions in medical students exposed to formaldehyde gas. J Dermatol 34:283–289
Takayanagi M, Sakai M, Ishikawa Y, Murakami K, Kimura A, Kakuta S, Sato F (2007) Formaldehyde concentrations in the breathing zone of medical students during gross anatomy laboratory in Toho University. Kaibogaku Zasshi 82:45–51
Vohra MS (2011) Personal formaldehyde exposure level in the gross anatomy dissecting room at College of Medicine King Saud University Riyadh. Int J Occup Med Environ Health 24:108–113
Wantke F, Focke M, Hemmer W, Bracun R, Wolf-Abdolvahab S, Gotz M, Jarisch R, Gotz M, Tschabitscher M, Gann M, Tappler P (2000) Exposure to formaldehyde and phenol during an anatomy dissecting course: sensitizing potency of formaldehyde in medical students. Allergy 55:84–87
Wei CN, Harada K, Ohmori S, Wei QJ, Minamoto K, Ueda A (2007) Subjective symptoms of medical students exposed to formaldehyde during a gross anatomy dissection course. Int J Immunopathol Pharmacol 20:23–25
Acknowledgments
The authors would like to thank Jantima Roongruangchai, Ph.D., and Mathee Ongsiriporn, M.D., for research permission. We appreciate Mr. Noppadol Piumpook for laboratory data support, Mr. Sutthipol Udompanturak for his assistance in the statistical analysis, and Jeerapa Kerdnoppakhun for the advice.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design.
Material preparation and data collection were performed by Anuch Durongphan, Nutchaya Amornmettajit, Jarun Rungruang, and Eakkapong Nitimanee.
The analysis was performed by Anuch Durongphan.
The first draft of the manuscript was written by Anuch Durongphan, and all authors commented on previous versions of the manuscript.
All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Responsible editor: Philippe Garrigues
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 114 kb)
Rights and permissions
About this article
Cite this article
Durongphan, A., Amornmettajit, N., Rungruang, J. et al. One academic year laboratory and student breathing zone formaldehyde level, measured by gas-piston hand pump at gross anatomy laboratory, Siriraj Hospital, Thailand. Environ Sci Pollut Res 27, 16521–16527 (2020). https://doi.org/10.1007/s11356-020-08199-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-020-08199-0