Abstract
Although the relationship between asthma and exposure to fine particulate matter (PM2.5) has been frequently measured, reported conclusions have not been consistent. As emergency department (ED) visits are an effective way to estimate health outcomes for people with asthma and short-term exposure to PM2.5, this review systematically searched five databases without language or geographical restrictions from inception to January 13, 2015 to study the impact of PM2.5 on asthma ED visits. A random-effects model was used to calculate the pooled risk ratio (RR) and 95 % confidence intervals (CI). With respect to short-term effects, asthma ED visits increased at higher PM2.5 concentrations (RR 1.5 % per 10 μg/m3; 95 % CI 1.2–1.7 %), and children were more susceptible (3.6 % per 10 μg/m3; 95 % CI 1.8, 5.3 %) than adults (1.7, 95 % CI 0.7 %, 2.8 %) to increased PM2.5; the ED visits increased during the warm season by 3.7 % (95 % CI 0.5, 6.9 %) per 10 μg/m3 increase in PM2.5, which was higher than the corresponding increase during the cold season (2.6, 95 % CI 0.7–4.6 %). This demonstrates that ambient PM2.5 has an adverse impact on asthma ED visits after short-term exposure and that children are a high-risk population when PM2.5 concentrations are high, particularly in warm seasons, during which measures should be taken to prevent PM2.5.

Similar content being viewed by others
References
Anderson HR, Favarato G, Atkinson RW (2013) Long-term exposure to air pollution and the incidence of asthma: meta-analysis of cohort studies. Air Qual, Atmos Health 6:47–56
Babin S, Burkom H, Holtry R, Tabernero N, Davies-Cole J, Stokes L, DeHaan K, Lee D (2008) Medicaid patient asthma-related acute care visits and their associations with ozone and particulates in Washington, DC, from 1994–2005. Int J Environ Health Res 18:209–221
Burnett RT, Smith-Doiron M, Stieb D, Cakmak S, Brook JR (1999) Effects of particulate and gaseous air pollution on cardiorespiratory hospitalizations. Arch Environ Health 54:130–139
Carracedo-Martinez E, Sanchez C, Taracido M, Saez M, Jato V, Figueiras A (2008) Effect of short-term exposure to air pollution and pollen on medical emergency calls: a case-crossover study in Spain. Allergy 63:347–353
Chen BY, Chen CH, Chen PC, Wang GS, Guo YL (2013) Air pollution, allergic co-morbidity, and emergency department visit for pediatric asthma in Taiwan. Aerosol Air Qual Res 13:1847–1852
de Pablo-Romero MPRR, Limón JMG, Praena-Crespo M (2015) Effects of fine particles on children’s hospital admissions for respiratory health in Seville, Spain. J Air Waste Manage Assoc 65:436–444
Delfino RJ, Wu J, Tjoa T, Gullesserian SK, Nickerson B, Gillen DL (2014) Asthma morbidity and ambient air pollution effect modification by residential traffic-related air pollution. Epidemiology 25:48–57
Eder W, Ege MJ, von Mutius E (2006) The asthma epidemic. N Engl J Med 355:2226–2235
EPA US (2014) Particulate matter (PM). 2014.5.6, Washington
Evans KA, Halterman JS, Hopke PK, Fagnano M, Rich DQ (2014) Increased ultrafine particles and carbon monoxide concentrations are associated with asthma exacerbation among urban children. Environ Res 129:11–19
Fan J, Wei W, Bai Z, Fan C, Li S, Liu Q, Yang K (2015) A systematic review and meta-analysis of dengue risk with temperature change. Int J Environ Res Public Health 12:1–15
Gasana J, Dillikar D, Mendy A, Forno E, Ramos Vieira E (2012) Motor vehicle air pollution and asthma in children: a meta-analysis. Environ Res 117:36–45
Glad JA, Brink LL, Talbott EO, Lee PC, Xu X, Saul M, Rager J (2012) The relationship of ambient ozone and PM(2.5) levels and asthma emergency department visits: possible influence of gender and ethnicity. Arch Environ Occupation Health 67:103–108
Gleason JA, Bielory L, Fagliano JA (2014) Associations between ozone, PM2.5, and four pollen types on emergency department pediatric asthma events during the warm season in New Jersey: a case-crossover study. Environ Res 132:421–429
Halonen JI, Lanki T, Yli-Tuomi T, Kulmala M, Tiittanen P, Pekkanen J (2008) Urban air pollution, and asthma and COPD hospital emergency room visits. Thorax 63:635–641
Jacquemin B et al. (2015) Ambient air pollution and adult asthma incidence in six European Cohorts (ESCAPE). Environmental health perspectives
Kim YK, Kim SH, Tak YJ, Jee YK, Lee BJ, Kim SH, Park HW, Jung JW, Bahn JW, Chang YS, Choi DC, Chang SI, Min KU, Kim YY, Cho SH (2002) High prevalence of current asthma and active smoking effect among the elderly. Clin Experiment Allerg : J British Soc Allerg Clin Immunol 32:1706–1712
Li S, Batterman S, Wasilevich E, Wahl R, Wirth J, Su FC, Mukherjee B (2011) Association of daily asthma emergency department visits and hospital admissions with ambient air pollutants among the pediatric Medicaid population in Detroit: time-series and time-stratified case-crossover analyses with threshold effects. Environ Res 111:1137–1147
Makra L, Puskas J, Matyasovszky I, Csepe Z, Lelovics E, Balint B, Tusnady G (2014) Weather elements, chemical air pollutants and airborne pollen influencing asthma emergency room visits in Szeged, Hungary: performance of two objective weather classifications. Int J Biometeorol
Mar TF, Koenig JQ (2009) Relationship between visits to emergency departments for asthma and ozone exposure in greater Seattle, Washington. Ann Allerg, Asthma Immunol : Off Public Am Coll Allerg, Asthma, Immunol 103:474–479
Mar TF, Jansen K, Shepherd K, Lumley T, Larson TV, Koenig JQ (2005) Exhaled nitric oxide in children with asthma and short-term PM2.5 exposure in Seattle. Environ Health Perspect 113:1791–1794
Mar TF, Koenig JQ, Primomo J (2010) Associations between asthma emergency visits and particulate matter sources, including diesel emissions from stationary generators in Tacoma, Washington. Inhal Toxicol 22:445–448
Meng YY, Rull RP, Wilhelm M, Lombardi C, Balmes J, Ritz B (2010) Outdoor air pollution and uncontrolled asthma in the San Joaquin Valley, California. J Epidemiol Community Health 64:142–147
Molter A et al (2015) A multicentre study of air pollution exposure and childhood asthma prevalence: the ESCAPE project. Europ Respirat J 45:610–624
Murray CJ et al (2012) Disability-adjusted life years (DALYs) for 291 diseases and injuries in 21 regions, 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 380:2197–2223
O’Connor GT, Neas L, Vaughn B, Kattan M, Mitchell H, Crain EF, Evans R 3rd, Gruchalla R, Morgan W, Stout J, Adams GK, Lippmann M (2008) Acute respiratory health effects of air pollution on children with asthma in US inner cities. J Allerg Clin Immunol 121:1133–1139, e1
Organization WH, Europe WHOROf (2006) Air quality guidelines: global update 2005: particulate matter, ozone, nitrogen dioxide, and sulfur dioxide. World Health Organization
Paulu C, Smith AE (2008) Tracking associations between ambient ozone and asthma-related emergency department visits using case-crossover analysis. J Public Health Manag Pract : JPHMP 14:581–591
Peel JL, Tolbert PE, Klein M, Metzger KB, Flanders WD, Todd K, Mulholland JA, Ryan PB, Frumkin H (2005) Ambient air pollution and respiratory emergency department visits. Epidemiology 16:164–174
Port A, Hein J, Wolff A, Bielory L (2006) Aeroallergen prevalence in the northern New Jersey-New York City metropolitan area: a 15-year summary. Ann Allerg, Asthma Immunol : Off Public Am Coll Allerg, Asthma, Immunol 96:687–691
Selgrade MK, Plopper CG, Gilmour MI, Conolly RB, Foos BS (2008) Assessing the health effects and risks associated with children’s inhalation exposures—asthma and allergy. J Toxic Environ Health A 71:196–207
Shah AS, Langrish JP, Nair H, McAllister DA, Hunter AL, Donaldson K, Newby DE, Mills NL (2013) Global association of air pollution and heart failure: a systematic review and meta-analysis. Lancet 382:1039–1048
Silverman RA, Ito K (2010) Age-related association of fine particles and ozone with severe acute asthma in New York City. J Allerg Clin Immunol 125:367–373, e5
Slaughter JC, Lumley T, Sheppard L, Koenig JQ, Shapiro GG (2003) Effects of ambient air pollution on symptom severity and medication use in children with asthma. Ann Allerg, Asthma Immunol : Off Public Am Coll Allerg, Asthma, Immunol 91:346–353
Slaughter JC, Kim E, Sheppard L, Sullivan JH, Larson TV, Claiborn C (2005) Association between particulate matter and emergency room visits, hospital admissions and mortality in Spokane, Washington. J Expo Anal Environ Epidemiol 15:153–159
Song C, Pei T, Yao L (2015) Analysis of the characteristics and evolution modes of PM2.5 pollution episodes in Beijing, China during 2013. Int J Environ Res Public Health 12:1099–1111
Stieb DM, Beveridge RC, Smith-Doiron M, Burnett RT, Judek S, Dales RE, Anis AH (2000) Beyond administrative data: characterizing cardiorespiratory disease episodes among patients visiting the emergency department. Can J Publ Health = Rev Canadienne de sante Publ 91:107–112
Stieb DM, Szyszkowicz M, Rowe BH, Leech JA (2009) Air pollution and emergency department visits for cardiac and respiratory conditions: a multi-city time-series analysis. Environ Health : Global Access Sci Source 8:25
Strickland MJ, Darrow LA, Klein M, Flanders WD, Sarnat JA, Waller LA, Sarnat SE, Mulholland JA, Tolbert PE (2010) Short-term associations between ambient air pollutants and pediatric asthma emergency department visits. Am J Respir Crit Care Med 182:307–316
Tecer LH, Alagha O, Karaca F, Tuncel G, Eldes N (2008) Particulate matter (PM(2.5), PM(10–2.5), and PM(10)) and children’s hospital admissions for asthma and respiratory diseases: a bidirectional case-crossover study. J Toxic Environ Health A 71:512–520
van Donkelaar A, Martin RV, Brauer M, Kahn R, Levy R, Verduzco C, Villeneuve PJ (2010) Global estimates of ambient fine particulate matter concentrations from satellite-based aerosol optical depth: development and application. Environ Health Perspect 118:847–855
Winquist A, Klein M, Tolbert P, Flanders WD, Hess J, Sarnat SE (2012) Comparison of emergency department and hospital admissions data for air pollution time-series studies. Environ Health : Global Access Sci Source 11:70
Yu O, Sheppard L, Lumley T, Koenig JQ, Shapiro GG (2000) Effects of ambient air pollution on symptoms of asthma in Seattle-area children enrolled in the CAMP study. Environ Health Perspect 108:1209–1214
Zora JE, Sarnat SE, Raysoni AU, Johnson BA, Li WW, Greenwald R, Holguin F, Stock TH, Sarnat JA (2013) Associations between urban air pollution and pediatric asthma control in El Paso, Texas. Sci Total Environ 448:56–65
Acknowledgments
Jinhui Tian from Evidence-Based Medicine Center, School of Basic Medical Sciences, Lanzhou University, is acknowledged for his valuable comments on the manuscript.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Responsible editor: Philippe Garrigues
Shulan Li contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Appendix S1
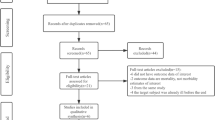
Flowchart of literature research and review process. (PDF 120 kb)
Appendix S2
Contextual details of studies included in the meta-analysis by publication year (PDF 172 kb)
Appendix S3
References list. (PDF 16 kb)
Appendix S4
Quality assessment of selected studies. (PDF 116 kb)
Rights and permissions
About this article
Cite this article
Fan, J., Li, S., Fan, C. et al. The impact of PM2.5 on asthma emergency department visits: a systematic review and meta-analysis. Environ Sci Pollut Res 23, 843–850 (2016). https://doi.org/10.1007/s11356-015-5321-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-015-5321-x